© Borgis - Postępy Nauk Medycznych 5/2013, s. 340-345
*Sabina Więcek1, Halina Woś1, Ewelina Stawicka-Ociepka2, Urszula Grzybowska-Chlebowczyk1
Obraz kliniczny zakażenia rotawirusowego u pacjentów hospitalizowanych w Klinice Pediatrii Śląskiego Uniwersytetu Medycznego w Katowicach w latach 2008-2009
Clinical picture of rotavirus infections in patients hospitalized in the Department of Pediatrics, Medical University of Silesia in Katowice, in the years 2008-2009
1Department of Pediatrics, Medical University of Silesia, Katowice
Head of Department: prof. Halina Woś, MD, PhD
2Student Research Club, Department of Pediatrics, Medical University of Silesia, Katowice
Head of Student Research Club: Sabina Więcek, MD, PhD
Streszczenie
Wstęp. Rotawirusy są najczęstszą przyczyną ostrej biegunki u niemowląt i dzieci do lat 4. Do zakażenia dochodzi głównie drogą pokarmową. Infekcje mogą mieć zróżnicowany przebieg – od łagodnego po ciężki, ze znacznym odwodnieniem i zaburzeniami gospodarki wodno-elektrolitowej i kwasowo-zasadowej.
Cel pracy. Celem pracy była analiza retrospektywna obrazu klinicznego zakażeń rotawirusowych u dzieci hospitalizowanych w Klinice Pediatrii SUM w latach 2008-2009.
Materiały i metody. Badaniem objęto 226 dzieci – 115 dziewczynek (51%) i 111 chłopców (49%), w wieku 0-18 lat, hospitalizowanych w Klinice Pediatrii SUM w Katowicach w latach 2008-2009 z powodu ostrych infekcji rotawirusowych. Zakażenie rotawirusowe rozpoznano na podstawie obrazu klinicznego oraz dodatniego wyniku testu immunoenzymatycznego stolca w kierunku zakażenia RV. W analizie uwzględniono: wiek, płeć pacjentów, objawy kliniczne, wyniki badań laboratoryjnych, choroby współistniejące. Otrzymane wyniki poddano analizie statystycznej.
Wyniki. Zakażenie rotawirusowe dotyczyło głównie niemowląt i małych dzieci (poniżej 3 roku życia) – 185/226 pacjentów (82%). Szczyt zachorowalności przypadał na miesiące od grudnia do marca. W obrazie klinicznym u niemowląt dominowała obfita, wodnista biegunka oraz wymioty. Z nieprawidłowości w badaniach laboratoryjnych najczęściej występowała hipertransaminazemia (84%) oraz podwyższone wykładniki stanu zapalnego (62%). U niemowląt częściej niż u dzieci starszych obserwowano zaburzenia gospodarki wodno-elektrolitowej i kwasowo-zasadowej. U 28/226 (12,4%) dzieci zakażenie RV współistniało z zakażeniem bakteryjnym przewodu pokarmowego (najczęściej enteropatogenna Escherichia coli, Campylobacter jejuni oraz Salmonella D-enteritidis).
Wnioski. Infekcje RV dotyczą głównie dzieci do lat 3. Przebieg choroby jest zróżnicowany, w dużym stopniu zależy od wieku pacjenta i chorób współistniejących.
Summary
Introduction. Rotavirus infections are the most common causes of acute diarrhoea in infants and children under 4 years of age. Such infections are mainly transmitted by the gastrointestinal route. They can vary in their course, which may be mild to severe with considerable dehydration and water, electrolyte and acid-base imbalance.
Aim. The aim of the study was a retrospective analysis of the clinical picture of rotavirus infections in children hospitalized in the Department of Pediatrics, Medical University of Silesia, in the years 2008-2009.
Patients and methods. The study involved 226 children: 115 girls (51%) and 111 boys (49%), aged 0-18 years, who were hospitalized in the Department of Pediatrics, Medical University of Silesia in Katowice, in the years 2008-2009 due to acute rotavirus infections. Rotavirus infections were diagnosed on the basis of the clinical picture and positive results of immunoenzymatic stool tests for RV infection. The analysis included: age, sex, clinical symptoms, results of laboratory tests and comorbidities. The obtained results were statistically analysed.
Results. Rotavirus infections mainly occurred in infants and young children (under 3 years of age), i.e. in 185/226 patients (82%). The highest incidence rate was observed from December to March. In infants, the clinical picture was dominated by abundant, watery diarrhoea and vomiting. Abnormalities in laboratory tests were accompanied by hypertransaminasemia (84%) and elevated levels of inflammatory markers (62%). Water, electrolyte and acid-base imbalance was observed more frequently in infants than in older children. In 28/226 (12.4%) children RV infection coexisted with a bacterial infection of the gastrointestinal tract (mostly enteropathogenic Escherichia coli, Campylobacter jejuni and Salmonella D-enteritidis).
Conclusions. RV infections mainly affect children under 3 years of age. The course of disease is varied and, to a large extent, depends on patient’s age and comorbidities.

INTRODUCTION
Acute infectious diarrhoea is the most common cause of morbidity and mortality among children all over the world. Improved living conditions, easier access to health care, early fluid therapy and prophylactic vaccination led to a considerable improvement of the epidemiologic situation.
At present, the most common causes of acute infectious diarrhoea in Polish children are viral infections, especially those caused by rotaviruses. More than 140 million rotavirus infections are reported yearly worldwide. Generally, 25 million children are outpatients, whereas 2 million require hospitalization, and approximately 600 000 children die, mostly those in developing countries. Infections usually affect children under 4 years of age, mainly infants. Characteristic symptoms of rotavirus infection include: watery diarrhoea, often accompanied by vomiting, fever and abdominal pain. Symptoms usually persist for up to 5-7 days (1-5).
AIM OF STUDY
Aim of study was a retrospective analysis of the clinical picture of rotavirus infections in children hospitalized in the Department of Pediatrics, Medical University of Silesia, in the years 2008-2009.
PATIENTS AND METHODS
The study involved 226 children: 115 girls (51%) and 111 boys (49%), aged 0-18 years (mean 2.3 years), who were hospitalized in the Department of Pediatrics, Medical University of Silesia in Katowice, in the years 2008-2009 due to acute rotavirus infections. Rotavirus infections were diagnosed on the basis of positive results of immunoenzymatic stool tests (ELISA method) for RV infection. The analysis included: age, sex, seasonal nature of infections (month of hospitalization), clinical symptoms on admission, results of laboratory tests (inflammatory markers – blood count and C-reactive protein, aminotransferase levels, parameters of water-electrolyte and acid-base balance).
In all our patients bacteriological stool tests were performed. Moreover, comorbidities were analysed in the group of subjects. The obtained results were statistically analysed.
Statistical analysis was performed according to procedures available for the MedCalc software. Quantitative variables were presented in the form of arithmetic mean and standard deviation. Qualitative variables were presented as absolute values and percentages. Intergroup differences were verified by means of the Chi-Square Test for qualitative variables. The assumed statistical significance level was p < 0.05.
RESULTS
The analysed group of patients was divided into 3 age subgroups: group 1 included infants – 27/226 (12%), group 2 (the largest) included children aged 1-3 years – 158/226 (70%), and group 3 including children over 3 years of age, which only constituted 18% (41/226) of the whole study population. The differences were statistically significant.
Over 3/4 of the analysed patients were children under 3 years of age (82% – 185/226) (fig. 1).
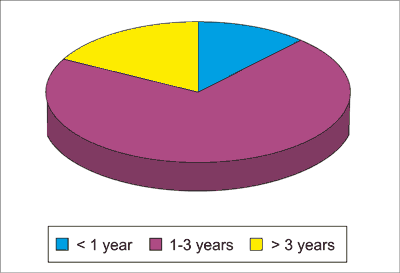
Fig. 1. Age analysis of the subjects with rotavirus infections.
| AGE | Number of patients | Percentage of analysed group |
| < 1 yr | 27 | 12.0% |
| 1-3 yrs | 158 | 70.0% |
| > 3 yrs | 41 | 18.0% |
| Total number of patients | 226 | 100.0% |
| Chi2 test | 24.885 |
| Significance level | p < 0.0001 |
Among the analysed patients, rotavirus infections were slightly more frequent among girls than boys; girls constituted 51% (115/226 patients), whereas boys 49% (111/226 patients). In the group of infants, boys fell ill more frequently (18/27 – 67%) than girls (9/27 – 33%). In the other age subgroups, no significant statistical differences were observed in the distribution.
Hospitalizations due to rotavirus infections were the most common in winter and in early spring, i.e. from December to March, whereas the least common – from May to August. The difference was statistically significant (p < 0.05) (fig. 2).
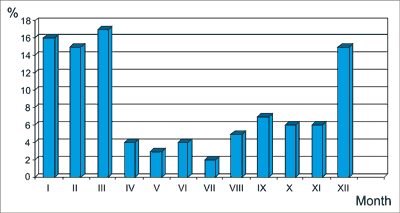
Fig. 2. Seasonal nature of rotavirus infections in the analysed population.
The clinical picture of rotavirus infections was varied. All examined children suffered from acute diarrhoea. Additionally, vomiting (120/226 – 53%), fever (44/226 – 19.4%), and abdominal pain (38/226 – 16.8%) were observed.
Neurological symptoms, usually in the form of apathy or agitation, anxiety and headache were observed in 99/226 children (43.8%) (tab. 1).
Table 1. Evaluation of the frequency of clinical symptoms in children with rotavirus infections.
| Clinical symptoms | Frequency | AGE | Statistical significance |
| < 1 yr | 1-3 yrs | > 3 yrs |
| Vomiting | 120/226
(53%) | 7/27
(26%) | 98/158 (62%) | 15/41
(37%) | p = 0.0014 |
| Abdominal pain | 38/226
(16.8%) | 2/27
(7.4%) | 12/158
(7.6%) | 24/41
(58.5%) | p < 0.001 |
| Fever | 44/226
(19.4%) | 4/27
(15%) | 33/158
(21%) | 7/41
(17%) | NS |
| Neurological symptoms | 99/226
(43.8%) | 5/27
(19%) | 77/158 (49%) | 17/41
(41%) | NS |
| Dehydration symptoms | 102/226
(45.1%) | 22/27
(81.5%) | 70/158
(44%) | 10/41
(25%) | p = 0.003 |
In the youngest patients, the clinical picture was dominated (apart from diarrhoea) by the symptoms of dehydration (22/27 – 81.5%). The incidence of severe dehydration decreased with age, reaching 25% in the group of older children (10/41).
Powyżej zamieściliśmy fragment artykułu, do którego możesz uzyskać pełny dostęp.
Mam kod dostępu
- Aby uzyskać płatny dostęp do pełnej treści powyższego artykułu albo wszystkich artykułów (w zależności od wybranej opcji), należy wprowadzić kod.
- Wprowadzając kod, akceptują Państwo treść Regulaminu oraz potwierdzają zapoznanie się z nim.
- Aby kupić kod proszę skorzystać z jednej z poniższych opcji.
Opcja #1
24 zł
Wybieram
- dostęp do tego artykułu
- dostęp na 7 dni
uzyskany kod musi być wprowadzony na stronie artykułu, do którego został wykupiony
Opcja #2
59 zł
Wybieram
- dostęp do tego i pozostałych ponad 7000 artykułów
- dostęp na 30 dni
- najpopularniejsza opcja
Opcja #3
119 zł
Wybieram
- dostęp do tego i pozostałych ponad 7000 artykułów
- dostęp na 90 dni
- oszczędzasz 28 zł
Piśmiennictwo
1. Benerjee I, Ramani S, Primrose B et al.: Comparative study of the epidemiology of rotavirus in children from a community-based birth cohort and hospital in South India. J Clin Microbiol 2006; 44: 2468-2474.
2. Desai R, Esposito D, Lees C et al.: Rotawirus – coded deaths in children United States 1999-2007. Pediatr Infect Dis J 2011; 30: 986-988.
3. Bruijning-Verhagen P, Sankatsing V, Kunst A et al.: Rotavirus – related hospitalizations are responsible for high seasonal peaks in all – cause pediatric hospitalizations. Pediatr Infect Dis J 2012; 31: 244-249.
4. Kuchar E, Nitsch-Osuch A, Szenborn L, Ołdak E: Rotawirusy jako czynnik etiologiczny zakażeń szpitalnych w Polsce – przegląd systematyczny z metaanalizą 11 badań. Przegl Epidemiol 2012; 66: 409-415.
5. Lopez-de-Andres A, Jiminez-Garcia R, Carrasco-Garrido P et al.: Hospitalizations associated with rotavirus gastroenterocolitis in Spain 2001-2005. BMC Public Health 2008; 8: 109-116.
6. Begue R, Perrin K: Reduction in gastroenterocolitis with the use of pentavalent rotavirus vaccine in a primary practice. Pediatrics 2010; 126: 40-46.
7. Albrecht P, Albrecht-Stanisławska A: Nadeszła era szczepień przeciwrotawirusowych. Ped Współ Gastroenterol Hep Żyw Dziecka 2006; 8: 215-219.
8. Munos M, Walker C, Black R: The effect of rotavirus vaccine on diarrhea mortality. Int J Epidemiol 2010; 39 (suppl. 1): i56-i62.
9. Perl S, Goldman M, Berkovitch M et al.: Characteristics of rotavirus gastroenteritis in hospitalized children in Israel. IMAJ 2011; 13: 274-277.
10. Szajewska H, Chmielewska A: Powikłania zakażenia rotawirusowego – przegląd piśmiennictwa. Ped Współ Gastroenterol Hep Żyw Dziecka 2008; 1: 7-11.
11. Hagbom M, Sharma S, Lundgren O, Svensson L: Towards a human rotavirus disease model. Curr Opin Virol 2012; 2: 408-418.
12. De Villiers FP, Driessen M: Clinical neonatal rotavirus infection: association with necrotizing enterocolitis. S Afr Med 2012; 6: 620-624.
13. Teitelbaum J, Daghistani R: Rotavirus causes hepatic transaminase elevation. Dig Dis Sci 2007; 52: 3396-3398.
14. Kacerka A, Wójcik K, Kuydowicz J et al.: An evaluation of the relationship between rotavirus diarrhoea and bacterial infection and acute hepatitis in children. Gastroenterol Pol 2009; 16: 446-448.
15. Hung T, Liu M, Hsu C, Lin Y: Rotavirus infection increases the risk of bacteremia in children with nontyphoid Salmonella gastroenteritis. Eur J Clin Microbiol Infect Dis 2009; 28(4): 425-428.
16. Kawashima H, Ishii H, Ioi H et al.: Transaminase in rotavirus gastroenteritis. Pediatrics International 2012; 54: 86-88.


