© Borgis - New Medicine 3/2013, s. 91-96
*Zsuzsanna Kovács
A study assesing the efficiency of treating emotional distress in women with malignant breast tumour
Faculty of Health Sciences, Semmelweis University, Budapest
Head of Faculty: Prof. Dr. Nagy Zoltán Zsolt
Summary
Aim. The aim of the study is to examine the change of emotional distress and fatigue influenced by a psychosocial intervention programme in women with non metastatic breast cancer.
Material and methods. The research was carried out in Budapest at the Department of Radiodiagnostics of the National Institute of Oncology. The sample: n=173, (intervention group = 86, control = 87) (34 women have participated in the study), control = 87. The Shortened Beck Depression Inventory, the Spielberger’s State-Trait Anxiety Inventory and the EORTC QLQ C30 quality of life questionnaire have been used for the research.
Results. There was a significant improvement in patients in all three assessed outcome variables. Depression symptoms: F(1.72) = 4.347 p = 0.041; anxiety: F(1.65) = 6.021 p = 0.017; fatigue: F(1.78) = 15.060 p = 0.000.
Conclusions. The early recognition of the presence of anxiety and depression, and their medical and psychological support are crucial. The psychosocial intervention efficiently helped the reduction of emotional distress and fatigue.
INTRODUCTION
According to the 2008 statistics of the World Health Organization, there were 34 million people diagnosed with cancer. There are about 12.5 million registered new cases, and 7.6 million people die of cancer every year around the world. Caring for patients with malignant tumours is causing more and more difficulties for health services. According to John Seffrin, the chief executive officer of the American Cancer Society, cancerous diseases have to be treated as global epidemic (1). By 2030 the number of new cancer patients is estimated to rise to 26 million, and 11.5 million people will die of malignant tumours. In Hungary, during the last 60 years, the number of cancer cases has also gradually risen, and in this respect we are at the top of the statistics among the EU state members (1, 2). Breast cancer is the most common malignant disease in women worldwide. As a result of early recognition and treatment, in the developed countries, including Hungary, the relative 5-year-survival rate is about 80% (1, 3). The diagnosis of breast cancer usually comes as a shock, accompanied by feelings of a threat to life and uncertainty. The state of anxiety and hopelessness has been proved to cause a decline in the health-related quality of life (4). The most common symptoms, such as depression, anxiety and vital exhaustion, can persist for years after the diagnosis (5, 6).
The number of cases affected by clinical anxiety and depression is much smaller, but reserches suggest that the presence of symptoms of subclinical anxiety and depression adversely affects everyday life management and the experience of quality of life. Most authors suggest that the presence of psychological distress is 50%; these are mainly adjustment difficulties accompanied by anxiety and depression. Derogatis found psychological disorders in 47% of the cases (7). In a large sample research (4496 patients), the prevalence of depression showed 52% (8). Hopwood found close correlation between depression and anxiety; 35% of the patients were characterised by this score, and he did not register any significant improvement at the 5-year follow up either (9).
Concerning the subject, only a few studies have been conducted in Hungary.There has been a national representative study carried out by Hungarostudy 2002, surveying the physical and mental health of the adult population of Hungary, and the relationship between health indicators and the environmental, social and economic background. According to their research results, the incidence of clinically significant depression rate in women affected with cancer was 28.5%, while in men it was 27.4% (10). According to the results of a recent study (11), one tenth of women with breast cancer showed depression reaching the clinical border, and nearly two thirds of them had mild depression symptoms. The symptoms of anxiety were shown in one third of the patients, and 20% of these had severe state-trait anxiety. These results confirm the clinical experiences published by Riskó (12), and are also related to the sources of similar studies (13).
Beside distress, one of the most common side-effects of conventional oncology treatments is vital exhaustion, with its defining characteristics: feelings of excessive fatigue and lack of energy and increasing irritability. Normally, there is a strong correlation between these symptoms and depression (14, 6).
Nowadays it is more and more important that the patients are provided with psychological and emotional support, and there is more emphasis put on promoting the ability for spiritual and emotional adjustment, encouraging coping, and improving psychosocial quality of life. During this process, psychosocial interventions have outstanding significance; in complex therapies for cancerous afflictions, the role of onco-psychology and integrated psychosocial care has become increasingly important (15).
The majority of the studies assesing patients with breast-cancer confirms the beneficial effects of psychosocial interventions in reducing emotional distress and also in impoving quality of life (16-20).
MATERIAL AND METHODS
In 2009-2010, a comprehensive psycho-oncology research was conducted, intending to develop a complex, complementary rehabilitation programme in addition to the conventional medical cancer treatment, in order to improve health and quality of life, strengthen coping abilities, and increase the life expectancy of patients suffering from cancer. As first steps of this research, cross-sectional studies were carried out, then a randomized sample was introduced to a complex, psychosocial intervention programme.
Our present study explores the variation of three commonly characteristicsymptoms of breast cancer following a psychosocial intervention programme:
1. Variation of depression and anxiety affected by the programme.
2. Variation of vital exhaustion, fatigue affected by the programme.
The assessed sample and methodologies
173 women agreed to participate in our research, all suffering from malignant breast cancer (C50) and who were currently undergoing medical treatment because of their illness. The research was carried out in Budapest at the Department of Radiodiagnostics of the National Institute of Oncology, with the permission of the Institute’s Ethical Committee. During the assessments an eight-page self-assessment form was used that took 50 minutes to be completed. The sample (n = 173) was randomly divided into treatment (n = 86) and control group (n = 87).Patients assigned to the experimental group were sent a letter of information, followed by telephone contact. 36 patients agreed to participate in the programme. All participants attended the first interview. The 36 patients were divided into two groups; between September and December 2009 (group 1) and between February and June 2010 (group 2). Two patients left the intervention; hence the final number of the participants was 34. Two measurements were carried out: one before the programme (1st measurement – T1) and one after the programme (2nd measurement – T2). The first questionnaires were completed during mammographic investigation, and then the participants received the other packages by post. 51 participants of the control-group (out of 87) returned the questionnaire. Social-demographic characteristics of the sample are shown in table 1.
Table 1. Demographic characteristics of study sample by groups at T1.
| | Treatment group (N = 36) | Control group (N = 87) | p |
| Age (mean and SD) | 53.17 (7.66) | 52.09 (9.15) | t = 0.61 ns. |
| Duration of the disease (mean and SD) | 2.47 (0.47) | 2.55 (0.86) | t = 0.45 ns. |
| Time spent since surgery (mean and SD) | 2.30 (0.74) | 2.30 (0.79) | t = 0.04 ns. |
Education: N (%)
primary or vocational school
secondary school or higher |
1 (2.8%)
35 (97.2%) |
19 (22.1%)
67 (77%) |
p = 0.007* |
Marital status: N (%)
lack of stable relationship
stable relationship |
14 (38.9%)
22 (61.1%) |
21 (24.1%)
66 (75.9%) |
χ2 = 2.72
ns. |
Having Children: N (%)
no
yes |
6 (16.7%)
30 (83.3%) |
6 (6.9%)
81 (93.1%) |
χ2 = 2.76
ns. |
Economic activity: N (%)
active
inactive |
17 (47.2%)
19 (52.8%) |
42 (48.3%)
45 (51.7%) |
χ2 = 0.01
ns. |
History of family cancer N (%)
no cancer
had cancer |
8 (22.2%)
28 (77.8%) |
42 (68.3%)
45 (51.7%) |
χ2 = 7.16
p < 0.01 |
SD – Standard Deviation; ns.= non-significant; *Fisher’s exact test
Concerning the demographic characteristics of the treatment and the control group, there were differences in education (the treatment group had more patients with at least secondary school); concerning the family medical history, there was a difference in the occurrence of cancerous affections (the control group had higher number of family members affected by tumours) (tab. 1).
The psychosocial intervention programme consisted of three main parts: a five-day residential life-style camp, where the patients received theoretical and a practical training related to healthy living, the incorporation of the acquired knowledge into everyday life-management, and finally a 14-week group psychotherapy, 5 hours a week.
Measures
Shortened Beck Depression Inventory BDI
The Shortened Beck Depression Inventory BDI was used to determine severity, and explore and follow up depression (21). The shortened version has nine items, that are related to social withdrawal, indecisiveness, change of sleep pattern, fatigue, hypochondria, inability towork, pessimism, lack of contentment and joy, and feelings of self-reproach. They can be scored by the patient between 1 and 4 (from ‘not at all characteristic’ to ‘totally characteristic’). High correlation (r = 0.92) between the total scores of the Shortened and the Full version confirms the reliability and applicability of the Shortened version. Concerning the severity of the depression, the Shortened Beck Inventory has the following categories: 0-9: not depressed,
10-18: mild depression, 19-25: moderate depression, above 26 points: severe depression. According to clinical validity, the borderline for clinical depression is 19 points. The reliability of the questionnaire on the sample proved adequate (Cronbach-alpha = 0.86) (22).
Spielberger’s State-Trait Anxiety Inventory (STAI-T)
The Spielberger’s State-Trait Anxiety Inventory STAI-T measures the levels of trait-anxiety and shows the level of predisposition to anxiety. The questionnaire consists of 20 questions. Answers can be recorded on a four-point Likert Scale. The choice of answers is as follows: 1 – not at all, 2 – somewhat, 3 – quite, 4 – very much). Minimum 20, maximum 80 points are achievable. Standard scores in female population: mean: 45.37; std. deviation: 7.97. In the sample, the Cronbach-alpha coefficient is 0.84 (23, 24).
Quality of Life Questionnaire
(EORTC QLQ C30 BR23)
For measuring quality of life, the EORTC QLQ C30 questionnaire was used that was developed by the Quality of Life Team of the European Organisation for Research and Treatment of Cancer (EORTC) (25). It consists of 30 items, andis divided into 3 scales. These are: 1) Global quality of life, 2) Functional quality of life and 3) Symptom-related quality of life. Global quality of life is assessed by two questions: „How would you rate the overall state of your health last week?” and „How would you rate the general quality of life last week?” The answers have to be indicated on a 1 to 7 scale, 1 = very bad, 7=excellent. Functional quality of life scales assess: physical functioning, role functioning, emotional functioning, cognitive functioning and social functioning. Symptom-related quality of life scales measure: fatigue, nausea, pain, dyspnoea, change in sleep pattern, loss of appetite, constipation, diarrhoea, and financial difficulties. Answers are recorded in a four-point Likert-scale: 1 – not at all characteristic, 2 – somewhatcharacteristic, 3 – characteristic, 4 – very much characteristic. The Cronbach-alpha coefficient for this questionnaire is between 0.62 and 0.89. The European Organisation for the Research and Treatment of Cancer (EORTC) has made the Hungarian translation of the test available. These tests have previously been used only a few times in Hungary; therefore, their validation on a national sample is also one of the objectives of our study. Out of the symptom scales, the present study assesses the results of the fatigue scale. The Cronbach-alpha coefficients of the tests appliedon our sample are shown in table 2.
Table 2. Reliability of scales at T1 and at T2.
| Scale | Number
of items | Cronbach-α
at T1 | Cronbach-α
at T2 |
| Anxiety (STAI) | 20 | 0.889 | 0.904 |
Depression
(BDI-Short) | 9 | 0.847 | 0.884 |
| EORTC-fatigue | 3 | 0.810 | 0.789 |
HYPOTHESES
1. We hypothesise that, following the intervention, the mood-related outcome measurements (anxiety, depression) in the assessed experimental group will show improvement, while the control group will show no change (to be verified by using the Repeated Measures Analysis of Variance assessing Time X Group Interaction).
2. We hypothesise that, in the intervention group, the EORTC fatigue measurement (one of the quality of life measurements) will improve following the intervention, while the control group will show no change (to be verified by using the Repeated Measures Analysis of Variance assessing Time X Group Interaction).
Applied Statistical Methods
As the first step, we compared the experimental group with the control group at the initial data collection (T1). Secondly, at the second data collection (T2), we assessed the control group to measure any differences between those who returned the questionnaires and those who did not. As the third step, we compared the changes occurred since the first data collection in both the experimental and the control group. For the analysis of categorical variables, we used the Chi-square test or Fisher-exact test,and Analysis of Variance was used for comparing variables for statistical significance.
RESULTS
1. Comparison of the experimental and the control group at the initial data collection: According to the results of the variance analysis when looking at the questionnaires completed at T1, the only difference between the two groups appeared in the EORTC fatigue symptom scale. F(1.119) = 4.298 (Mexperimental: 39.20, SD: 18.30; Mcontrol: 30.46, SD: 22.30). Members of the experimental group started off with higher scores in the fatigue scales.
2. Comparison of the scores within the control group, between patients who returned the questionnaires and who did not: We assessed whether there were any significant differences concerning the psychological scales of the questionnaires within the control group between the patients who returned the tests (N = 51) and the patients who did not (N = 36). According to the analysis, there were no differences between the scores of the two groups, and neither was a difference concerning the demographic characteristics.
3. Changes occurring in the experimental and the control group between T1 and T2 (levels of anxiety and depression, fatigue). We applied repeated measures analysis of variance, where in the within-subjects design we assessed along the data collection date (time) the group affiliation (experimental vs. control) X time interaction (tab. 3). As an extra factor the education aspect was brought into the analysis, as the two groups showed major differences at T1.
Table 3. Mean scores (Standard Deviations) of scales at T1, T2 by group (intervention vs. control).
| | Before treatment (T1) | After treatment (T2) |
| Intervention group | Control group | Intervention group | Control group |
| Anxiety | 44.50 (9.04) | 43.23 (10.53) | 39.37 (9.13) | 42.58 (11.34) |
| Depression | 12.34 (3.56) | 12.37 (3.88) | 11.44 (2.27) | 12.63 (4.96) |
| EORTC-fatigue | 39.39 (18.65) | 31.25 (22.42) | 23.90 (15.57) | 31.37 (24.48) |
The repeated measures analysis of variance showed significant changes in all three assessed dimensions:
Anxiety F(1.65) = 6.021, p = 0.017 (fig. 1)
Depression F(1.72) = 4.347, p = 0.041 (fig. 2)
EORTC Fatigue F(1.78) = 15.060, p = 0.000 (fig. 3)
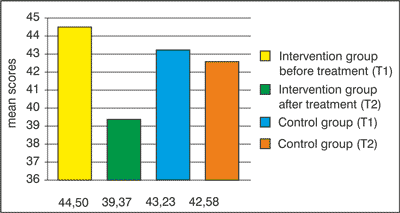
Fig. 1. Anxiety before treatment and after treatment.

Fig. 2. Depression before treatment and after treatment.
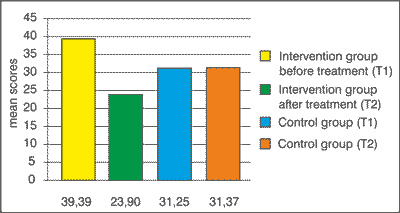
Fig. 3. Fatigue before treatment and after treatment.
These results show that the affiliation of the members had an important influence on the positive changes of the listed measurements (tab. 3), namely patients who achieved favourable scores at T2 in comparison with T1 were those who participated the intervention programme. We assessed the education factor too, but it had no influence on the analysed variables of the present study.
DISCUSSION
Our research aimed to assess the effectiveness of a complex, comprehensive, psychosocial interventional programme, affecting different levels of attitudes to health, life management and spiritual function in women with breast cancer. In order to enhance synergic effects, we tried to integrate numerous methods into the programme that according to the data of related literature can facilitate the spiritual growth and the physical healing of the patients. Our general aim was to strengthen the coping ability, to improve the quality of life, to facilitate cognitive emotional process, and to reduce the chances of remission. Our present study is focused on the changes of the disease characteristic symptoms: emotional distress, and vital exhaustion, fatigue in the light of the influence of the programme.
Depression and anxiety has been proved to cause a decline in health and deterioration of quality of life. A depressed, hopeless state, that full of anxiety is known to influence the patients’ quality of life. The psychological distress influences the physical comfort, the sense of well-being and the physical symptom perception (4, 13). The intervention proved to be effective, as all three symptoms of the patients have been significantly reduced. The programme successfully helped reducing anxiety and depression; the intervention group showed a significant improvement in their moods in comparison of the control group. An important measurement of the quality of life, the vital exhaustion, the general fatigue syndrome has also significantly improved. Just as the results of other researchers, these findings prove the effectiveness of psychosocial interventions, and psychotherapeutic procedures (16-18, 20).
According to the results we find it very important and suggest a regular and routine screening of psychological distress in patients with cancer. Beside the risk of clinical distress, the subclinical group also has to be monitored. The early recognition of anxiety and depression, and an appropriate support and treatment are crucial. They fundamentally influence the patients’ quality of life; they can encourage the patients’ co-operation, and evoke their fighting spirit.
Our study and the related similar researches also bear an important health care policy message: psychosocial interventions are largely cost-effective – for a small investment we can achieve a marked improvement in health and quality of life. Nowadays in the field of oncology the specialised onco-psychological services are underrepresented; most of the patients cannot access these kind of support (26, 27). High standard oncology services fulfilling the high expectations of our modern era cannot lack the knowledge of related sciences, the integrated psychosocial interventions (15).
ACKNOWLEDGEMENT
We would like to thank the co-workers of the Department of Radiodiagnostics (National Institute of Oncology, Budapest) for distributing the questionnaires to the patients.
Special thanks to Judit Kovacs and Prof. Dr Sándor Eckhardt for supervision and professional advises.
Piśmiennictwo
1. Tompa A: Daganatos betegségek előfordulása, a hazai és nemzetközi helyzet ismertetése, Global and Hungarian Burden of Cancer. Magyar Tudomány 2011; 11: 1333-1345. 2. WHO 2008. The global burden of disease: 2004 update Geneva: World Health Organization. 3. Coleman MP, Quaresma M, Berrino F et al.: Cancer survival in five continents: a worldwide population-based study (CONCORD). The Lancet Oncology 2008: 9(8): 730-756. doi: 10.1016/s1470-2045(08)70179-7. 4. Fann J: Major depression after breast cancer: a review of epidemiology and treatment. General Hospital Psychiatry 2008;30 (2):112-26. 5. Montazeri A: Health-related quality of life in breast cancer patients: a bibliographic review of the literature from 1974 to 2007. J Experim Clinical Cancer Research 2008, 27: 32. doi: 10.1186/1756-9966-27-32 6. Reddick BK, Nanda JP, Campbell L et al.: Examining the influence of coping with pain on depression, anxiety, and fatigue among women with breast cancer. J Psychosocial Oncology 2005; 23(2-3): 137–57. 7. Derogatis LR, Morrow GR, Fetting J et al.: The prevalence of psychiatric disorders among cancer patients. Journal of the American Medical Association 1983; 249: 751-757. 8. Zabora J, Brintzenhofe K, Curbow B et al.: The prevalence of psychological distress by cancer site. Psycho-oncology 2001; 10(1): 19-28. 9. Hopwood P, Sumo G, Mills J et al.: The course of anxiety and depression over 5 years of follow up and risk factors in women with early breast cancer: Results from the UK Standardisation of Radiotherapy Trials (START). Breast 2010; 19(2): 84-91. 10. Dégi L, Csaba: Pszichoszociális kockázati tényezők szerepe a daganatos megbetegedésekben 2008. [In:] Kopp M, Magyar lelkiállapot; Semmelweis Kiadó, Budapest, 557-568. 11. Kovács Zs, Pigniczkiné Rigó A, Hoyer M et al.: The prevalence of depression and anxiety in patients with malignant breast tumour. New Medicine 2011; 15(2): 61-66. 12. Riskó Á: Bevezetés az onkopszichológiába. Animula, Budapest 1999. 13. Reich M, Lesur A, Perdrizet-Chevallier C: Depression, quality of life and breast cancer: a review of the literature. Breast Cancer Research and Treatment 2008; 110(1): 9-17. 14. Silver JK: Rehabilitation in women with breast cancer. Physical Medicine and Rehabilitation Clinics of North America 2007; 18(3): 521-537, doi: 10.1016/j.pmr.2007.05.003. 15. Jacobsen PB, Holland JC, Steensma DP: Caring for the whole patient: the science of psychosocial care. J Clin Oncol 2012; 30: 1151-1153. 16. Fors EA, Bertheussen GF, Thune I et al.: Psychosocial interventions as part of breast cancer rehabilitation programs? Results from a systematic review. Psycho-oncology 2011; 20(9): 909-918, doi: 10.1002/pon.1844. 17. Kissane D: Beyond the psychotherapy and survival debate: the challenge of social disparity, depression and treatment adherence in psychosocial cancer care. Psycho-oncology 2009; 18(1): 1-5, doi: 10.1002/pon.1493. 18. Naaman SC, Radwan K, Fergusson D, Johnson S: Status of psychological trials in breast cancer patients: a report of three meta-analyses. Psychiatry 2009; 72(1): 50-69, doi: 10.1521/psyc.2009.72.1.50. 19. Osborn RL, Demoncada AC, Feuerstein M: Psychosocial interventions for depression, anxiety, and quality of life in cancer survivors: meta-analyses. Int J Psychiatr Med 2006; 36: 13-34. 20. Dewey A: Psychosocial interventions for reducing fatigue during cancer treatment in adults. Int J Evid Based Health 2010; 8: 106-107. 21. Beck AT, Beck RW: Screening depressed patient in family practice. A rapid technic. Postgrad Med 1972; 52: 81-85. 22. Rózsa S, Szádóczky E, Füredi J: A Beck Depresszió Kérdôív rövidített változatának jellemzôi hazai mintán. Psychiatria Hungarica 2001; 16: 384-402. 23. Spielberger CD, Gorsuch RL, Lushene RE: Manual for the State-Trait Anxiety Inventory. Consulting Psychologists Press 1970, Palo Alto, CA. 24. Sipos K, Sipos M, Spielberger CD: A State-Trait Anxiety Inventory (STAI) magyar változata. [In:] Mérei F, Szakács F (red.): Pszichodiagnosztikai vademecum I/2. Nemzeti Tankönyvkiadó, Budapest 1994, 123-148. 25. Aaronson NK, Ahmedzai S, Bergman B et al.: The European Organisation for Research and Treatment of Cancer QLQ-C30: a quality of life instrument for use in international clinical trials in oncology. Journal of National Cancer Institute 1993; 85: 365-367. 26. Dégi LC: Onkopszichológiai beavatkozások hatékonyságvizsgálata a daganatos betegek életminősége és túlélési esélye szempontjából. Psychiatr Hung 2006; 21: 138-146. 27. Greer S: Psychological intervention. The gap between research and practice. Acta Oncol 2002; 41: 238-243.


