*Małgorzata Borowska, Katarzyna Szadkowska
Analysis of dental clearance conducted under general anaesthesia in disabled patients aged 2 to 18 from the Dental Clinic of the Little Prince Hospice for Children in Lublin
Analiza zabiegów sanacji jamy ustnej w znieczuleniu ogólnym u niepełnosprawnych pacjentów w wieku 2-18 lat z poradni stomatologicznej Lubelskiego Hospicjum dla Dzieci im. Małego Księcia
Dental Clinic, Little Prince Hospice for Children in Lublin
Head of Clinic: Małgorzata Borowska, MD, PhD
Streszczenie
Wstęp. Dzieci i młodzież z różnymi rodzajami niepełnosprawności rzadko objęte są planowym leczeniem stomatologicznymi oraz profilaktyką próchnicy. Integralność w opiece stomatologicznej w stosunku do opieki ogólnomedycznej i specjalistycznej w tej grupie pacjentów jest niedostateczna.
Cel pracy. Ocena stomatologicznych potrzeb leczniczych u dzieci z orzeczoną niepełnosprawnością leczonych w znieczuleniu ogólnym.
Materiał i metody. Przeprowadzono analizę ilościową 542 kart zabiegowych u 439 niepełnosprawnych pacjentów w wieku 2-18 lat leczonych stomatologicznie w znieczuleniu ogólnym. Oceniono: zaawansowanie próchnicy w poszczególnych grupach wiekowych, liczbę pacjentów z daną chorobą ogólną, wiek pacjenta, gdy został wykonany pierwszy zabieg sanacji jamy ustnej w znieczuleniu ogólnym oraz źródło informacji o możliwości leczenia w pełnym znieczuleniu przy braku współpracy z pacjentem.
Wyniki. W grupie pacjentów z uzębieniem mlecznym z powodu zaawansowania próchnicy usunięto średnio 6,48 zęba (w przeliczeniu na jednego pacjenta), podczas gdy wyleczono średnio 3,45 zęba. U pacjentów z uzębieniem stałym średnia liczba zębów wyleczonych wynosiła 8,35, natomiast usuniętych 1,35. Najwięcej pacjentów zakwalifikowanych do sanacji jamy ustnej w znieczuleniu ogólnym to pacjenci z mózgowym porażeniem dziecięcym (18,45%). Najczęściej pacjenci zgłaszali się po raz pierwszy na leczenie w wieku 7 lat (12,75%). Jedynie 4,56% pacjentów zostało skierowanych do naszej poradni na zabieg sanacji w znieczuleniu ogólnym przez lekarza pediatrę lub lekarza stomatologa. W pozostałych przypadkach rodzice szukali możliwości leczenia na własną rękę.
Wnioski. Leczenie stomatologiczne dzieci niepełnosprawnych wymaga zaangażowania nie tylko lekarzy dentystów, ale również współpracy z lekarzami specjalistami – szczególnie w kwestii wczesnego podjęcia leczenia i profilaktyki chorób jamy ustnej.
Summary
Introduction. Children and youths with various kinds of disabilities are rarely covered by scheduled dental treatment and dental caries prevention. The integrity of dental care as compared to general medical care in this patient group is insufficient.
Aim. The assessment of dental treatment needs in children with certificates of disability, treated under general anaesthesia.
Material and methods. A quantitative analysis of 542 procedure charts from 439 children with disabilities, aged 2 to 18 years old, who were administered dental treatment under general anaesthesia, was performed. The following factors have been evaluated: dental caries progression in different age groups, the number of patients with a given primary disease, age at which the patient underwent their initial dental clearance treatment performed in general anaesthesia, and the sources of information concerning the possibility of receiving treatment under general anaesthesia for patients unable to collaborate with the dentist.
Results. In the group of patients with primary teeth, an average of 6.48 teeth (per patient) were extracted due to the progression of dental caries, while an average of 3.45 teeth were successfully treated. In the patients with permanent teeth, the average number of the treated teeth equaled 8.35, while the average number of the removed teeth was 1.35. Most patients enrolled for dental clearance under general anaesthesia suffered from cerebral palsy (18.45). The most common age of the initial treatment was 7 years old (12.75%). Only 4.56% of the patients were referred to our clinic by a paediatrician or a dentist. In the remaining cases, parents sought treatment opportunities on their own.
Conclusions. Dental care in children with disabilities requires not only commitment from care professionals, but also their cooperation with other specialists, particularly regarding the early initiation of treatment and the prevention of oral cavity diseases.

Introduction
Children and youths with various disabilities are rarely covered by scheduled dental treatment and prevention of dental caries. This is due not merely to the existing indisputable difficulties in obtaining patient-dentist collaboration during a dental appointment, but also due to the lack of comprehensive dental care as compared with general health care (1). There is an urgent need to raise the oral health awareness of the disabled children’s parents and caregivers, as well as of relevant medical staff, and to improve the availability of medical institutions offering dental treatment under general anaesthesia (2).
The Dental Clinic of the Little Prince Hospice for Children in Lublin has for the past 7 years been involved in administering dental care and treatment to patients of different ages with a certificate of disability. The offered care covers both outpatient visits and dental clearance procedures performed under anaesthesia, followed by regular follow-up appointments (every 3-6 months, as relevant), all under the free National Health Fund (Narodowy Fundusz Zdrowia) treatment plan. From the total of over 2000 disabled patients treated at our clinic, a group of children and youths aged 2-18 were selected for this study. The results of the analysis of the procedures they received under general anaesthesia have been presented in this study, and their oral health and treatment needs have been assessed.
Aim
The purpose of this study is to evaluate dental treatment needs in children and youths with a certificate of disability, treated under general anaesthesia.
Material and methods
A quantitative analysis of 542 procedure charts of 439 disabled patients who received dental treatment under general anaesthesia at the Dental Clinic of the Little Prince Hospice for Children in Lublin. The patients’ age was 2-18 years. The number of patients according to the cause of their disability certificate has been presented in figure 1.
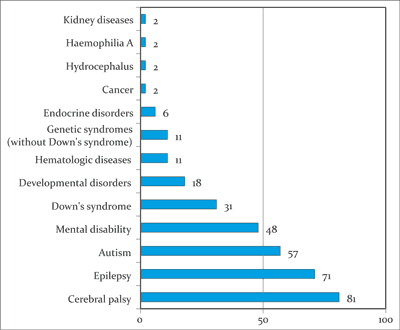
Fig. 1. The number of patients according to the cause of their certificate of disability
Patients with the need for the removal of an infection source within the oral cavity for the existing risk of an focal infection have been identified. They have been classified into three groups according to their dental development stage: primary dentition, mixed (primary and permanent) dentition, and permanent dentition.
According to the dental development stage, the studied group was comprised by:
– 120 patients with primary dentition (aged 2-8 years old) – 27.34%,
– 255 patients with mixed dentition (aged 5-15 years old) – 58.09%,
– 62 patients with permanent dentition (aged 9-18 years old) – 14.12%.
The advancement of the carious process (related to the number of teeth treated and removed in the course of the administered procedures, and the ratio of the restored to the removed teeth) in given age groups, the patient’s age at the time of the initial dental clearance procedure received under general anaesthesia, and the source of information of the possibility to receive treatment under general anaesthesia when the patient is unable to collaborate (referrals from other physicians) have all been analysed.
Results
The analysis of the type of the primary disease affecting the patients revealed the largest percentage to be children suffering from cerebral palsy (18.45%), epilepsy (16%), and autism (12.9%) (fig. 1).
In 21.64% of the patients, there were absolute indications for the removal of the infection focus from the oral cavity for the existing risk of complications in the form of an odontogenic disease. In this group, 79 of the patients were children with a heart defect (83.16%) and 12 (12.63%) were patients treated for hemato-oncological diseases (fig. 2, 3). In 4% of the patients, renal diseases and rheumatoid arthritis were found.
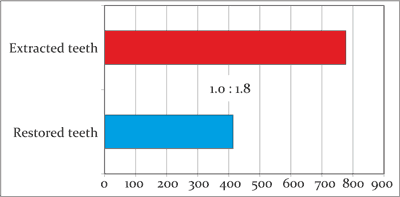
Fig. 2. The average number of the restored and the extracted teeth and the ratio of the average number of the restored teeth to the extracted teeth in the group of patients with primary dentition
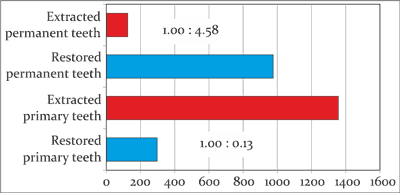
Fig. 3. The average number of the primary and permanent teeth restored and extracted, and the ratio of the average number of the restored teeth and the extracted teeth in the group of patients with mixed dentition
In the group of children with primary dentition, 414 teeth were conservatively treated (average 3.45 primary teeth per patient), whereas 777 teeth were extracted (average 6.48 teeth). The ratio of the average number of the restored teeth to the removed teeth was 1.0:1.8 (fig. 2).
In the mixed dentition group, the average number of the restored primary teeth decreased to 1.16, whereas the number of the extracted teeth was 5.32, with a ratio of 1.0:4.58. In this group, on average 3.83 permanent teeth required conservative treatment, whereas 0.49 had to be removed owing to the advancement of the carious process. Thus, the ratio for the permanent teeth was 1.0:0.13 (fig. 3).
In the 9-18 years old group (with permanent teeth), the average number of restored teeth was 8.35, and the removed ones – 1.35, with a ratio of 1.0:0.16 (fig. 4).
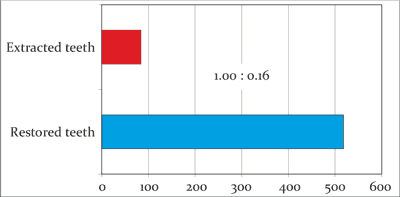
Fig. 4. The average number of the restored teeth and the extracted teeth and the ratio of the average number of the restored teeth and the extracted teeth in the group of patients with permanent dentition
For the patients’ permanent teeth, the assessment of the condition of the first permanent molars both for the mixed dentition group and the permanent dentition group was performed. This reflects, to some degree, the effectiveness of the education of parents and caregivers in respect to the children’s oral hygiene, and of the conducted preventive treatment (fissure sealing, fluoride varnish treatment).
In the group of children with mixed dentition, an average of 3.01 teeth were restored, and 0.43 teeth per patient were removed (fig. 5). In the older children (with permanent teeth), the values were 2.16 and 1.5 respectively (fig. 6). It is worth remembering that endodontic treatment of molars or multi-stage treatment of immature teeth is not performed under general anaesthesia, due to the risk of possible complications and the necessity for repeat general anaesthesia. Hence the importance of an early diagnosis and a prompt initiation of adequate treatment in non-collaborating paediatric patients.

Fig. 5. The number of the restored and the extracted first permanent molars in total, according to the type of dentition

Fig. 6. The number of the restored and the extracted first permanent molars according to the type of dentition, per patient
Powyżej zamieściliśmy fragment artykułu, do którego możesz uzyskać pełny dostęp.
Mam kod dostępu
- Aby uzyskać płatny dostęp do pełnej treści powyższego artykułu albo wszystkich artykułów (w zależności od wybranej opcji), należy wprowadzić kod.
- Wprowadzając kod, akceptują Państwo treść Regulaminu oraz potwierdzają zapoznanie się z nim.
- Aby kupić kod proszę skorzystać z jednej z poniższych opcji.
Opcja #1
24 zł
Wybieram
- dostęp do tego artykułu
- dostęp na 7 dni
uzyskany kod musi być wprowadzony na stronie artykułu, do którego został wykupiony
Opcja #2
59 zł
Wybieram
- dostęp do tego i pozostałych ponad 7000 artykułów
- dostęp na 30 dni
- najpopularniejsza opcja
Opcja #3
119 zł
Wybieram
- dostęp do tego i pozostałych ponad 7000 artykułów
- dostęp na 90 dni
- oszczędzasz 28 zł
Piśmiennictwo
1. Proc P, Daszkowska M, Hilt A et al.: Ocena stomatologicznych zachowań zdrowotnych dzieci niepełnosprawnych – badania ankietowe rodziców. Czas Stomatol 2008; 61: 767-774. 2. Paszyńska E, Jurga J, Dyszkiewicz-Konwińska M, Mehr K: Ocena programu profilaktycznego zdrowia jamy ustnej u pacjentów niepełnosprawnych intelektualnie. Pediatr Med Rodz 2009; 5: 271-275. 3. Borysewicz-Lewicka M, Gerreth K, Wiśniewska K, Wysocki J: Leczenie stomatologiczne jako część wymaganej opieki medycznej nad dziećmi niepełnosprawnymi – opinia rodziców. Dent Med Probl 2011; 48: 45-53. 4. Elszyn B, Lewalska M, Rychlewska M et al.: Dostępność usług stomatologicznych dla niepełnosprawnych wychowanków ośrodków szkolno-wychowawczych w Polsce. Dental Forum 2009; 37: 69-74. 5. Rusyan E, Dubielecka M: Opieka stomatologiczna u osób chorych przewlekle i niepełnosprawnych. Asystentka i Higienistka 2006; 1: 29-30. 6. Gerreth K, Lewicka A: Problemy opieki stomatologicznej nad dziećmi niepełnosprawnymi. Polska Medycyna Rodzinna 2004; 6 (supl. 1): 172-176. 7. Gerreth K: Leczenie stomatologiczne pacjentów niepełnosprawnych i przewlekle chorych – diagnostyka i terapia. Nowa Stomatol 2015; 20(2): 59-64. 8. Adamczyk Ł, Olczak-Kowalczyk D: Leczenie stomatologiczne w znieczuleniu ogólnym dzieci przewlekle chorych. Dent Med Probl 2010; 47: 61-68. 9. Gerreth K, Cieślińska K: Zabiegi stomatologiczne w znieczuleniu ogólnym u dzieci niepełnosprawnych. Family Medicine & Primary Care Review 2005; 7: 63-67. 10. Gołębiowska M, Hreczecha M, Rawa-Kołodziejska J, Mikliński P: Leczenie stomatologiczne dzieci specjalnej troski w znieczuleniu ogólnym. Mag Stomatol 1995; 2: 52-54. 11. Hilt A, Daszkowska M, Filipińska-Skąpska R et al.: Stan uzębienia i potrzeby lecznicze dzieci z zaburzeniami rozwoju somatycznego i psychicznego z województwa łódzkiego. Czas Stomatol 2009; 62(4): 262-270. 12. Borysewicz-Lewicka M, Wochna-Sobańska M, Mielnik-Błaszczak M et al.: Wyniki ekspertyzy oceniającej stan jamy ustnej, potrzeby lecznicze, a także dostępność do stomatologa dzieci oraz młodzieży niepełnosprawnej i przwlekle chorej. Czas Stomatol 2010; 63(2): 90-101. 13. Herman K, Wrzyszcz-Kowalczyk A, Jankowska K: Ocena stanu zdrowia jamy ustnej u dzieci z zespołem Downa lub z mózgowym porażeniem dziecięcym. Dent Med Probl 2012; 2(48): 30-36. 14. Borowska M, Skorzyński W, Rahnama M et al.: Aspekty leczenia stomatologicznego dzieci specjalnej troski i pacjentów niepełnosprawnych. Cz. 2. Mag Stomatol 2013; 23(10): 90-94.







