*Dominika Szczepanek1, Katarzyna Emerich1, 2
Treatment methods for selected complications of dentin dysplasia type I – a report of five cases
Metody leczenia wybranych powikłań dysplazji zębiny typu I – opis pięciu przypadków
1Pediatric and Family Dental Clinic, University Dental Center, Medical University of Gdańsk
Head of Clinic: Professor Katarzyna Emerich, BDS, PhD, DSc
2Chair and Department of Paediatric Dentistry, Medical University of Gdańsk
Head of Chair and Department: Professor Katarzyna Emerich, BDS, PhD, DSc
Streszczenie
Dysplazja zębiny typu I jest chorobą genetyczną, dziedziczoną autosomalnie dominująco, występującą 1/100 000 urodzeń. Charakteryzuje się nieprawidłową morfologią koron oraz zmianami w budowie korzeni zębów: skróceniem, nieprawidłowym kształtem, częściowym lub całkowitym brakiem komór miazgi, obecnością torbieli oraz rozchwianiem zębów. Wiąże się to z utrudnionym lub niemożliwym do wykonania leczeniem endodontycznym oraz szybką utratą ruchomych zębów. Praca pokazuje wybrane metody leczenia powikłań dysplazji zębiny oraz zasady profilaktyki pozwalające utrzymać zęby jak najdłużej w jamie ustnej. Najważniejsze dla prawidłowego leczenia jest trafne postawienie diagnozy. O ile na podstawie badania zewnątrzustnego bardzo trudno jest postawić diagnozę, to po wykonaniu zdjęcia ortopantomograficznego nie powinno być wątpliwości. Lecząc pacjenta z dysplazją zębiny, należy przede wszystkim zadbać o profilaktykę przedwczesnej utraty zębów. Należy regularnie wykonywać skaling pozwalający uniknąć stanów zapalnych oraz eliminować wszystkie węzły urazowe i przedwczesne kontakty.
Wobec konieczności leczenia endodontycznego związanego z bólem lub zmianami okołowierzchołkowymi należy zastosować kiretaż otwarty lub zamknięty. Leczenie ortodontyczne oraz protetyczne jest dość ryzykowne ze względu na obciążenie zębów dodatkowymi siłami. Należy dążyć do poprawy warunków w jamie ustnej oraz jak najdłuższego utrzymania własnych zębów pacjenta, nawet rozważając często niestandardowe metody leczenia.
Summary
Dentin dysplasia, type I, is a genetic disorder inherited as an autosomal dominant trait. The incidence has been estimated at 1/100,000 births. DDI is characterized by the presence of teeth with abnormal crown morphology without rudimentary root development: shortened root length, abnormal shape, partial or total obliteration of the pulp chamber, periapical radiolucent areas or cysts and loosening of the teeth. This results in more complex or impossible endodontic treatment and a rapid loss of loose teeth.
This paper describes methods for the treatment of selected complications of type I dentin dysplasia as well as prevention strategies aimed at preserving the teeth for the longest possible time. A correct diagnosis is essential for proper treatment planning.
It is very difficult to make a diagnosis based only on intraoral examination but with OPG there should be no doubts. The most important aspect in the treatment of dentin dysplasia type I is to prevent premature loss of teeth. Scaling should be performed regularly to avoid inflammatory conditions. Moreover occlusal trauma and premature occlusal contacts should be eliminated. If endodontic treatment associated with pain or periapical changes is necessary, open or closed curettage should be performed. Orthodontic and prosthetic treatment methods are quite risky due to additional forces applied on the teeth. Therefore, we should strive to improve dental condition in the oral cavity and preserve the patient’s own teeth for as long as possible, even if non-standard methods of treatment are needed.

Introduction
Dentin dysplasia is a genetic disorder of teeth occurring in 1 per 100,000 births. It is often observed throughout several generations of family members. The disorder exhibits sex-unlinked, autosomal dominant inheritance. It is probably related to gene mutation on chromosome 4q 13-21. This location corresponds to locus dentinogenesis imperfecta, therefore the symptoms of dentin dysplasia type I and II are similar. It is believed that an abnormal migration of Hertwig’s epithelial root sheath cells into the dental papilla contributes to the development of dentin dysplasia. These cells induce abnormal osteoblasts differentiation, leading to excessive dentin deposition and pulp chamber obliteration (1-4).
Three types of dysplasia have been distinguished based on clinical and radiological symptoms. Type I dentin dysplasia, also known as radicular dysplasia, will be discussed in more detail below.
Type II dentin dysplasia, also known as coronal dentin dysplasia (2-4), is often confused with amelogenesis imperfecta. Both, permanent and deciduous teeth are affected. Normal shape of the crown, characteristic amber or blue colour and a rapid enamel abrasion are observed in deciduous teeth. The roots are of normal length and shape (1-3). The crowns of the permanent teeth have slightly altered colour and the enamel susceptibility to abrasion is lower compared to deciduous teeth. The teeth exhibit lower susceptibility to caries and lower responsiveness to thermal stimuli. No pathological mobility or marginal periodontal lesions are observed (4). The roots of the teeth affected by dysplasia type II show normal morphology. However, an X-ray reveals characteristic shell-like appearance. The pulp chamber in molars may be crescent-shaped, while single-rooted teeth may be thistle-tube shaped. Pulp stones, which rarely develop in dental canals, may be found in the chamber (2-4).
Dentin dysplasia type III, i.e. fibrous dysplasia, is a combination of type I and II dysplasia. The disorder is very rare. Both the chamber and the root are of normal structure. Normal appearance of the enamel and the presence of dental chamber give rise to many difficulties in the diagnosis of the disease. Fibrous dentin in the pulp chamber as well as rearrangement of collagen, which is only present in the predentin, are the only characteristic features (2-4). Dentin dysplasia type I, also known as radicular dysplasia, often remains undetected in clinical practice due to normal coronal morphology as well as resistance to caries and abrasion (2-5). Patients attend to the dentist due to cervical exposure or teeth mobility. Dentin dysplasia is usually diagnosed accidentally, based on OPG. X-ray images show shortened tooth roots, partially or completely obliterated pulp chamber and pulp stones in the 1/3 of the periapical chamber. Pathological lesions also affect the parodontium, manifesting in horizontal bone atrophy, thinning of the bone structure around the roots as well as the presence of cysts (5, 6). Furthermore, patients with the above-described radiographic image may sometimes experience throbbing pain increasing with temperature and in the horizontal position, i.e. symptoms typical of gangrene (2, 3). The observed clinical symptoms include fistulas in the region of the affected teeth despite obliterated pulp and the absence of canal lumens (5).
Four subtypes of type I dentin dysplasia have been distinguished: Ia, Ib, Ic, Id. Subtype Ia corresponds to the most advanced disease – the teeth have no roots, while only residual roots are present in subtype Ib. Subtype Ic is characterised by shortened roots, while normal root length and the presence of pulp stones in the pulp chamber are observed in subtype Id (2). Patients often do not realize for many years that they suffer from dentin dysplasia. Symptoms such as exposed cervical dentin or tooth mobility are attributed to periodontitis. Currently, the wide use of panoramic radiographs allows for an accidental detection of the disease (5). However, this usually happens at the stage of permanent, often residual, dentition. Currently, the increasing number of patients deciding for orthodontic treatment have a panoramic radiograph performed, which allows to detect dentin dysplasia already at the stage of mixed dentition (7, 8). Radiological image of dentin dysplasia in deciduous dentition is extremely rarely encountered by a dentist.
Aim
The aim of this paper was to familiarize the reader with the clinical manifestations of dentin dysplasia based on the description of two families affected by this disorder. In the first case, type I dentin dysplasia was observed in siblings (brother and sister); in the second case, the disease affected two sisters and a daughter of one of them.
Case reports
A 12-year boy was reported to the Paediatric and Family Dental Clinic of the University Dental Center, Medical University of Gdańsk, referred by his orthodontist for dental treatment. The orthodontist began treatment with removable dental braces. However, he discontinued treatment and referred the patient to a specialist pedodontic center after performing a panoramic radiograph. The boy’s parents reported no systemic diseases, allergies or chronic use of medications. Intraoral examination revealed no abnormalities, but a typical picture of mixed dentition, which is usually found in a 12-year-old child. Dental crowns were of normal shape, size and structure (fig. 1), covered with properly developed, hard, shiny and smooth enamel. Permanent teeth, except for 2nd and 3rd molars and 36, 43, 44 and 45 as well as persistent deciduous teeth 53 and 63 were found in the oral cavity. The teeth 32, 31, 41 and 42 had second-degree mobility. Caries was present in the fissures of teeth 16, 26 and 46. The patient delivered a panoramic radiograph (fig. 2) taken a few months earlier, showing a different status of dentition compared to that of the day of examination. The OPG showed root shortening in all permanent teeth and complete pulp chamber obliteration in teeth 25, 26, 36, 32, 31, 41 and 42. A crescent-shaped brighter area could be seen in the coronal portion of the chamber in the remaining permanent teeth, indicating partial chamber obliteration. Periapical lesions and bone thinning were identified in teeth 36, 32, 41 and 46. Based on dental examination and a characteristic radiological image, type I dentin dysplasia was diagnosed. Treatment plan was presented: thorough hygiene instructions and non-traumatic tooth brushing training, treatment of teeth affected by caries, extraction of persistent and worn deciduous teeth as well as orthodontic consultation with a specialist in the treatment of patients with dentin dysplasia. Medical history collected from the patient and his parents provided important information on the loss of tooth 36, which was extracted a few months earlier. The patient reported to the endodontist due to idiopathic pain persisting for a few days. The pain neither resolved when consuming cold beverages, nor was increased by warm stimuli. After X-ray examination, the dentist began endodontic treatment. An attempt to localize dental chamber or the root canal ortifice failed. As the pain persisted, extraction was performed. Deciduous teeth were extracted under infiltration anaesthesia with 4% articaine during several subsequent visits. In the first permanent molars, medium carious lesions were removed and cavities filled with composite material. Fluoride varnish was applied after treatment completion. The patient reported for a follow up every 3 months; no new carious lesions were observed and a very good hygiene was maintained. The boy does not report pain or gingival bleeding. Fluoride preventive treatment is regularly performed during visits. Since dentin dysplasia is inherited as an autosomal dominant trait and occurs among family members, particular emphasis was put on the search for other cases of the disorder among the family members when collecting medical history. It was found that a very rapid loss of previously mobile teeth was experienced by the father and the grandmother of the patient.
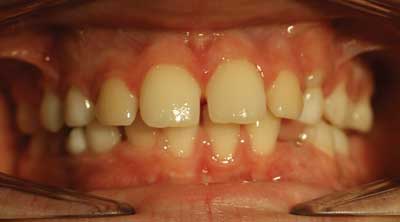
Fig. 1. The intraoral conditions presented by patient 1 (a 12-year-old boy)
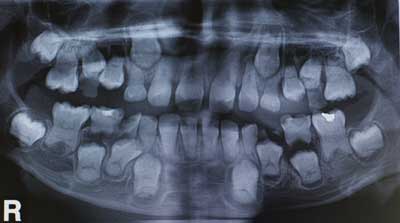
Fig. 2. A panoramic view of patient 1 (a 12-year-old boy)
Powyżej zamieściliśmy fragment artykułu, do którego możesz uzyskać pełny dostęp.
Mam kod dostępu
- Aby uzyskać płatny dostęp do pełnej treści powyższego artykułu albo wszystkich artykułów (w zależności od wybranej opcji), należy wprowadzić kod.
- Wprowadzając kod, akceptują Państwo treść Regulaminu oraz potwierdzają zapoznanie się z nim.
- Aby kupić kod proszę skorzystać z jednej z poniższych opcji.
Opcja #1
24 zł
Wybieram
- dostęp do tego artykułu
- dostęp na 7 dni
uzyskany kod musi być wprowadzony na stronie artykułu, do którego został wykupiony
Opcja #2
59 zł
Wybieram
- dostęp do tego i pozostałych ponad 7000 artykułów
- dostęp na 30 dni
- najpopularniejsza opcja
Opcja #3
119 zł
Wybieram
- dostęp do tego i pozostałych ponad 7000 artykułów
- dostęp na 90 dni
- oszczędzasz 28 zł
Piśmiennictwo
1. Cameron AC, Widmer RP (red. wyd. pol. U. Kaczmarek): Stomatologia dziecięca. Elsevier Urban & Partner, Wrocław 2013. 2. Syryńska M, Janiszewska-Olszowska J: Dziedziczna dysplazja zębiny typu Ic – opis 3 przypadków. Czas. Stomat 2005; 7: 520-524. 3. Tkacz I, Mielnik-Błaszczak M, Pels E, Borowicz J: Dysplazja zębiny – opis przypadku. Nowa Stomatol 2012; 2: 58-63. 4. Boguszewska-Gutenbaum H, Grzybowska A, Janicha J, Valipour Kolti F: Dysplazja zębiny – opis jednostki chorobowej. Nowa Stomatol 2009; 14: 82-89. 5. Ozer S, Ozden B, Ozden FO, Gunduz K: Dentinal dysplasia type I: A case report with a 6-year follow up. Case Rep Dent 2013, 659084: 1-3. 6. Toomarian L, Mashhadiabbas F, Mirkarimi M, Mehrdad L: Dentin displasia type I: a case report and review of the literature. J Med Case Reports 2010; 4: 1-6. 7. Bespalez-Filho R, De Azambuja Berti Couto S, Souza PHC et al.: Ortodontic treatment of a patient with dentin dysplasia type I. Am J Orthood Dentofacial Orthop 2013; 143: 421-425. 8. Fulari SG, Tambake DP: Rootless teeth: Dentin dysplasia type I. Contemp Clin Dent 2013; 4: 527-530. 9. Nettem S, Nettemu SK, Basha K, Venkatachalapathi S: Implant – based oral rehabilitation of a variant model of type I dentinal dysplasia: A rare case report. Dent Res J 2014; 11: 513-517. 10. Depprich RA, Ommerborn MA, Handschel JGK et al.: Dentin displasia type I: a challenge for treatment with dental implant. Head & Face Medicine 2007; 3(31): 1-5.



