© Borgis - New Medicine 3/2013, s. 71-77
*Urszula E. Ulmer1, Leszek Czerwosz2, Rafał Ł. Leszcz1, Michał Bielwaski1, Maria M. Grochowska1, Katarzyna Wilczyńska1, Paweł Białek1, Robert Proczka1, Paweł Nitkowski1, Jerzy A. Polański1
Influence of surgical endarterectomy in the femoral-popliteal segment on gait pattern in a patient with peripheral arterial disease
1II-nd Department of General, Vascular and Oncological Surgery of Medical University of Warsaw
Head of Department: prof. Jerzy A. Polański, MD, PhD
2Bioinformatics Laboratory, Mossakowski Research Medical Centre, Polish Academy of Sciences,
Warsaw
Head of Laboratory: prof. Bogdan Lesyng
Summary
Aim. The aim of this study was to determine if surgical endarterectomy of the arteries of the lower limb affects in any way the gait pattern in patients diagnosed with PAD and if in a remote postoperative day, can be established improvement of the patient’s gait parameters relative to the values obtained in the test before surgery. The third objective was the verification of the suitability of the measurement method by measuring the gait parameters in a relatively small stretch, with the aid of the measuring system Ultraflex Computer Dyno Graphy (CDG) from Infotronic Medical Engineering (12).
Material and methods. In the study participated PAD 20 patients and 17 controls. Each patient was subjected to a surgical endarterectomy. Measurements of gait were performed in each patient three times: I one day before the endarterectomy procedure, II 1-3 days after surgery, and III 6 weeks later.
Results. Gait speed was lower in patients than in the control group by more than 1 km/h. In PAD patients, gait speed in series III was higher then speed in series II and very similar to series I. Mean cycle and mean frequency did not differ among series I, II, and III in patients, but there were a significant differences from control values – in patients cycle was longer and frequency smaller. Comparative analysis of three series showed no severe changes of speed or single or double support duration. The results of comparisons of single and double support times, calculated as percentage with respect to the duration of gait cycle, indicate however, that patients avoid single support in favour of double support. Gait measured in series II manifested an increased heterogeneity (inequality of steps) in relation to the other two series in PAD patients.
Conclusions. The performed study demonstrates that surgical endarterectomy procedure in the femoro-popliteal segment affected the PAD patient’s gait pattern, especially in the early days after surgery.
INTRODUCTION
PAD epidemiology
Peripheral arterial disease (PAD) is the artherosclerotic process, especially the lower limb arteries.
Anatomically, only about 30% of atherosclerotic lesions in the lower extremities concern iliac arteries. But as many as 70% of lesions are found within the vessels of femoro-popliteal and tibial segments (1).
PAD is found in almost 10% of people around the world (2), and PAD patients have a high risk factors of death from cardiovascular causes (3).
As the risk factors of the occurrence of PAD are recognized:
– Tobacco smoking. Most of the PAD patients (85-95%) are the current or former smokers (4),
– Hyperlipidemia,
– Hypertension,
– Diabetes,
– Lack of physical activity,
– Age, gender, ethnicity.
Men aged: 33-44 years old – an average of 6 PAD cases per 10,000 examined persons, 65-74 years old 61/10,000. Women aged 33-44 years old – 3/10,000, in 65-74 – 54/10,000 (5). The incidence of PAD depending on gender corresponds to the ratio 2:1 (male:female), whereas the incidence of critical limb ischemia is the ratio 3:1 (male:female). The studies also demonstrate that in terms of ethnicity, a black race bears the highest risk of PAD occurrence (6).
PAD classification
Intermittent claudication, rest pain and ulceration of the skin are the set of the most common symptoms of PAD. Generally accepted PAD classifications are based on two scales: Fontaine and Rutherford (7) (tab. 1, 2).
Table 1. Rutherford scale.
| Rutherford |
| Degree | Category | Clinical symptoms |
| 0 | 0 | No symptoms |
| I | 1 | Mild claudication |
| I | 2 | Moderate claudication |
| I | 3 | Severe claudication |
| II | 4 | Ischaemic rest pain |
| III | 5 | Small tissue defects |
| III | 6 | Large tissue defects |
Table 2. Fontaine scale.
| Fontaine |
| Stage | Clinical symptoms |
| I | No symptoms |
| IIa | Mild claudication |
| IIb | Moderate claudication |
| III | Ischaemic rest pain |
| IV | Ulceration/gangrene |
The types of surgical methods for endarterectomy of the femoral-popliteal segment
The primary purpose of each treatment of PAD is to minimize the risk of limb loss and reduce the symptoms associated with the presence of the disease, significantly impairing the quality of patient’s life (1).
Surgical treatments of peripheral ischemia, have long been the gold standard of treatment when symptoms cannot be controlled by diminishing the risk factors, physical therapy, or pharmacotherapy.
In the femoro-popliteal segment, the following treatment’s methods are used:
– PTA (percutaneous balloon angioplasty),
– atherectomy,
– stent implantation,
– laser endarterectomy.
A combination of these methods for the purposes of one procedure is also possible.
Another type of providing of the occlusion of the femoro-popliteal area is the procedure of implantation of femoro-popliteal bypass; from native vein, as well as artificial (7).
Intermittent claudication as the main symptom of PAD
Intermittent claudication as the primary symptom of peripheral arterial disease, is described as discomfort or pain in the lower extremities, thighs or buttocks, emerging during walking or other physical activity, and decreasing during the rest (2).
Statistically, the most common location of pain resulting from claudication caused by occlusion of superficial femoral artery are calf muscles.
Disorders of flow within the iliac, common femoral, tibial or peroneal artery result in pain around the buttocks, thighs, or feet.
The presence of symptoms of pain in both extremities, may indicate a disturbance in the flow within the aorta, iliac arteries on both sides or the non-vascular nature of the disease (8).
The majority of patients with intermittent claudication presents a stable course of PAD throughout life and in these patients is found ailments reduction as a result of the elimination of risk factors for PAD. 20-30% of patients are subjected to surgical treatment of arterial endarterectomy due to the deterioration of symptoms (9).
Intermittent claudication as a factor affecting the quality of gait
Intermittent claudication, defined as lower limbs pain emerging during gait and forcing the patient to stop and rest, is considered a classic symptom of peripheral arterial disease (10).
Quality of life in PAD patients who have intermittent claudication is deteriorating in many aspects. The pain resulting from claudication significantly effects on the degree of their independence – PAD patients have a higher susceptibility to fatigue as a result of reduced locomotion, they have difficulty in performing activities of daily living (11).
Purpose of the pilot study
To the II-nd Department of General, Vascular and Oncological Surgry of Medical University of Warsaw, per year are admitted about 400 patients with diagnosed peripheral arterial disease, in order to carry the procedure of endarterectomy of arteries of the lower limb. On average, 250 of the patients in this group are subjected to endarterectomy procedure in the femoro-popliteal region.
The objectives of this study is to determine:
1. If surgical endarterectomy of the arteries of the lower limb affects in any way the gait pattern in patients diagnosed with PAD.
2. If in a remote postoperative day, i.e. min 6 weeks after treatment, can be established improvement of the patient’s gait parameters relative to the values obtained in the test before surgery and thus recognize that the endarterectomy surgical procedure may significantly affect the quality improvement of the PAD patient’s gait
3. Verification of the suitability of the measurement method by measuring the gait parameters in a relatively small stretch, with the aid of the measuring system Ultraflex Computer Dyno Graphy (CDG) from Infotronic Medical Engineering (12).
MATERIAL AND METHODS
The research material
In the study participated 20 patients with diagnosed peripheral arterial disease (5 women, 15 men) and 17 healthy people as a control group. The average age of PAD patients participating in the study is 70 years old, the age range was 56-85 y.o. Each participating in the experiment patient was subjected to a surgical endarterectomy in the femoro-popliteal segment, of which nine treatments were related to endarterectomy in the right lower limb, and 11 in the left lower limb. PAD patients were admitted to the ward of II Department of General, Vascular and Oncological Surgery of Medical University in Warsaw in the period from VII.2011 to II.2012, in order to perform the endarterectomy procedure in the femoral-popliteal segment.
Into the study were enrolled PAD patients who have:
– A history of the occurrence of intermittent claudication;
– Ankle-brachial index did not exceed the value of 0.6;
– Occlusion of the carotid arteries on ultrasound did not exceed 4%;
– Occlusion of the lower limbs has been confirmed in angioTK study.
Measurement tools
Measurement of the walking pattern and the gait analysis of each patient was performed by means of the CDG measurement system. Values and distribution of ground reaction forces were measured by means of eight tensometers embedded in each sole of measurement shoes.
Gait structure
The gait analysis was performed according to the method described in the Whittle’s book (13) „Gait Analysis: an Introduction” Whittle Michael, 2007, Butterworth-Heinemann. The author gives the gait structure in form of gait phases, which detection and the measurement provide parameters for gait evaluation Thus, main parameters are: duration of the support, including single and double support. The schedule is demonstrated on the figure 1 according to that described by Whittle.
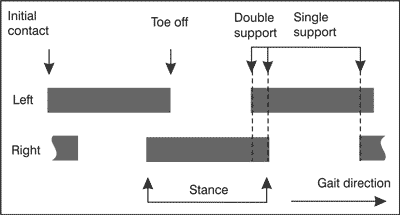
Fig. 1. Gait phases (adapted from 13).
Method of measurement
In each patient qualified for the study three-fold measurement of gait were performed. All measurements were carried out within specified periods of time:
– I series – the day before the endarterectomy procedure,
– II series – 1-3 days after the endarterectomy procedure,
– III series – 6 weeks after the endarterectomy procedure.
In the control group only one measurement of gait was performed.
Each person taking part in the study walked distance of 24 meters, at a rate appropriate for his daily walk. Such a short distance was established for purpose for this study, so that no intermittent claudication in the patients occurred during the measurement , which could result in significant impairment of gait or stopping.
The essence of this study was in fact to determine, not a direct effect of claudication on patients’ gait, but the indirect effects in the form of gait adaptation to the current state of the disease and developing particular gait pattern, designed to minimize the risk of claudication during walking.
The following parameters of gait were subjected to the analysis of each measurement:
– walking speed (in km/h), the duration of the gait cycle (full cycle with both legs),
– the frequency of walking (in min-1),
– average time of single support and its standard deviation – heterogeneity (in seconds),average time of double-support and its standard deviation – heterogeneity (in seconds).
To avoid the ambiguity of application of the term standard deviation, two parameters require a comment: the standard deviation of times of a single and a double support.
An average value of single – or double-support time was calculated for each individual measurement within a set of steps that patient performed in while measuring. Within this set the standard deviation of a single or double-support time was also calculated. Average values represent approximately the typical times for a given set of steps, and standard deviations express their distribution, that is the heterogeneity of steps.
The standard deviation of a single-or double-support times calculated within a set of steps was then, as well as other parameters, averaged for group of patients. In the calculation appears therefore the standard deviation (within a set of measurements) of the standard deviation (within a set of steps for each measurement). For convenience, the standard deviation of times of a single/double support within a set of steps is referred to as, for the purposes of this study, the heterogeneity of time of a single/double support.
RESULTS
Velocity, cycle and frequency
As you can see from the table 3, gait speed was lower in patients than in the control group by more than 1 km/h, which is about 25%. All differences between measurements in patients (series: I, II, and III) and the measurements in the control group were statistically significant (p < 0.0001). If taking into account the comparison of successive series I, II and III in PAD patients, the gait speed in the III series differed from the speed obtained in the II series statistically significant (p < 0.01). Series I exhibited velocity similar to III, and yet, difference between series I and II was not statistically significant. Scattering the measurements of series I was, however, greater than of series III.
Table 3. Average values of parameters together with respective standard deviations of velocity, cycle time and frequency of gait in three consecutive measurements in the PAD patients, and the results for the same parameters acquired by control group.
| | Velocity
(m/s) | Cycle
(sec) | Frequency (min-1) |
| Series I | 3.5 ± 0.90 | 1.21 ± 0.20 | 101.2 ± 15.6 |
| Series II | 3.18 ± 0.86 | 1.26 ± 0.21 | 97.6 ± 15.1 |
| Series III | 3.63 ± 0.71 | 1.20 ± 0.17 | 101.4 ± 12.6 |
| Control Group | 5.13 ± 0.50 | 1.06 ± 0.07 | 114.4 ± 7.6 |
Gait cycle is called the time of the two full steps, once with the left and the right foot. Frequency is an ordinary reciprocal of gait cycle time, expressed in min-1. Both the cycle and the frequency does not differ in a statistically significant way, while comparing outcomes of series I, II and III in patients, but there was a significant difference from control values. The longest cycle and the lowest rate was observed in patients in the II series.
Next results relate to gait characteristics of the left and right legs separately and then to the extremities identified as sick and healthy, and finally to the combined results in groups of left and right legs. Any differences in the results calculated for different extremities may arise from lateralization and dysfunction or just limb pain resulting from a PAD, but also as result of surgery (in particular in series II).
Single support time (ssup)
Observation of the single support times (ssup) for the pair of limbs: left and right and for the pair: disabled and healthy (tab. 4) shows that these times are for both limbs in the pair very similar (within separately I, II, III series in patients and in controls). The differences do not exceed 5%. However, statistical analysis showed a significantly shorter time of single support related to the left leg than to the right (p < 0.01) in series I. Comparison of ssup time of the left and the right leg in healthy individuals did not reveal any differences.
Table 4. Average values of single support times with their standard deviations, separately for the left and right and healthy and the diseased limb in three series in patients and in the control group.
| Ssup (sec) | Left | Right | Disabled | Healthy |
| Series I | 0.41 ± 0.06 | 0.43 ± 0.05 | 0.41 ± 0.05 | 0.42 ± 0.06 |
| Series II | 0.43 ± 0.08 | 0.43 ± 0.06 | 0.42 ± 0.05 | 0.44 ± 0.05 |
| Series III | 0.42 ± 0.04 | 0.43 ± 0.04 | 0.42 ± 0.05 | 0.42 ± 0.04 |
| Control Group | 0.39 ± 0.03 | 0.40 ± 0.03 | 0.39 ± 0.03 | 0.39 ± 0.03 |
To test the potential cause of these differences ssup times were determined for healthy and diseased limbs instead of left and right. In our PAD cohort there were 11 left and 9 right legs disabled.
Statistical analysis did not show any significant difference in the duration of ssup related to diseased and healthy legs in any series: I, II, III (separately), although a trend of increased time related to healthy leg can be observed for series II.
Checking consistent results on the left and right legs was intended to determine the feasibility of combining the results of two limbs. It turns out that in the case of ssup time, the results were ambiguous. In this situation, we decided to combine the results of measurements obtained from both legs. The same procedure was carried out for the other measurement parameters.
The statistical analysis of ssup time for the combined groups of left and right limbs showed no statistically significant differences between the series I, II and III. Comparison of results of patients and controls showed that only series III differed significantly with controls, and it’s not because the duration of the single support was in series III of the largest (ssup was the longest in series II) but because the dispersion of results in series III was the least. Such results are generally in pilot studies. Although ssup time tends to increase in series II,
and simultaneously in all series it is slightly longer than in the control group, it should be noted that the as a percentage of the duration of gait cycle, ssup time is shorter in PAD compared to healthy subjects. Percentages of ssup in gait cycle are shown in graph 2 – for the combined results of both limbs. Statistically, series III differs significantly from the series I (p < 0.03). As you can see, these differences are not large. In all three series in patients the percentage of single support was statistically significantly shorter than in the control group (p < 0.01).
Double support time (dsup)
Despite the fact that a person being tested is based on both legs during the dual support, this phase is assigned once to the left and once to the right leg. This is because the double support phase follows alternately single support on the left and the right leg.
The following table (tab. 5) shows the times of double support (dsup), average values with their standard deviations for both lower limbs are given, then dsup is assigned to disabled and to healthy limb in I, II, III series in patients and in controls.
Table 5. Average values of double support times with their standard deviations, separately for the left and right and healthy and the diseased limb in three series in patients and in the control group.
| Dsup (sec) | Left | Right | Disabled | Healthy |
| Series I | 0.19 ± 0.05 | 0.18 ± 0.05 | 0.19 ± 0.05 | 0.18 ± 0.05 |
| Series II | 0.20 ± 0.06 | 0.20 ± 0.05 | 0.20 ± 0.06 | 0.20 ± 0.06 |
| Series III | 0.18 ± 0.05 | 0.17 ± 0.04 | 0.18 ± 0.04 | 0.18 ± 0.05 |
| Control Group | 0.13 ± 0.03 | 0.14 ± 0.02 | 0.13 ± 0.02 | 0.13 ± 0.02 |
Dsup times for the pair of legs: left and right and for the pair: disabled and healthy) are very similar (within separately I, II, III series in patients and in controls). The differences do not exceed 5%. There are small differences between left and right dsup time in series III (p < 0.04). The results of dsup measurements from both legs have been combined.
Statistical analysis of dsup time (for the combined groups of left and right limbs) showed no statistically significant differences between the series I, II and III, despite indications to series II – dsup time was longest – see the figure 2.

Fig. 2. Average times of single and double supports with their standard deviations in three series in PAD patients and in the control group.
Comparison of results of patients and controls, however, indicate statistically significant differences in duration of double support (p < 0.001). Double support times expressed as percentages of gait cycle were similar among series I, II and III, there was no statistically significant difference. Figure 3 shows dsup% together with ssup%. In all three series in patients double-support times as a percentage were statistically significantly less than in controls (p < 0.0001).
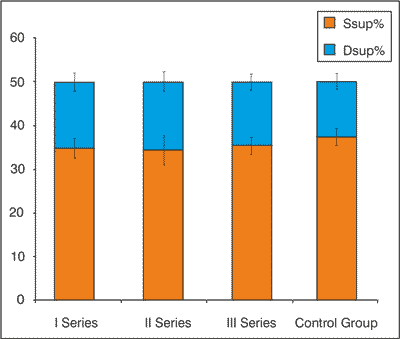
Fig. 3. Average percentage times of single and double supports with their standard deviations in three series in PAD patients and in the control group. The percentage was calculated in relation to the duration of the cycle.
Gait heterogeneity
Because, as we have shown in Section 3.4, the standard deviation of single support time and standard deviation of the double-support time, based on a set of steps of any single measurement, have equal rights to be called parameters (named heterogeneities), comparisons of average values of these heterogeneities have been performed.
Figure 4 summarizes the average heterogeneity of single and double support times in I, II and III series in patients and in healthy controls.
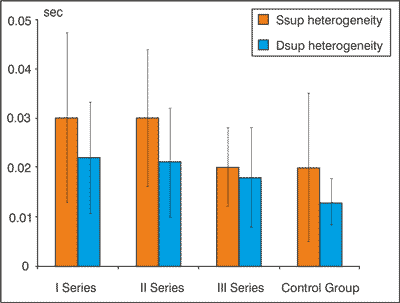
Fig. 4. Average times of heterogeneities of single and double supports with their standard deviations in three series in PAD patients and in the control group.
The graph shows that the heterogeneities of single support time in series I and II were almost the same, and higher than the heterogeneity in series III and in the control group. Heterogeneity difference between series II and III was statistically significant (p < 0.03), similarly the difference between series II and control group (p < 0.03). Heterogeneity in series I was slightly smaller than in series II, and it does not differ significantly from the control group.
Double-support time heterogeneity have slightly different character, heterogeneity in I series I, II and III were significantly different from the control group (p < 0.00001, p < 0.005, and p < 0.04, respectively), but did not differ from each other.
DISCUSSION
The study showed that surgical endarterectomy in the femoro-popliteal segment affects some of the gait parameters.
The reduced walking speed is found in patients with symptoms of intermittent claudication – it is described in one published so far research work (14). It is due to the fact that the stance phase lasts longer in these patients than transfer phase relative to the control group at similar age. Speed reduction in PAD patients is demostrated by other reserchers (15), (16). According to them, support phase is extended in PAD patients, the time required to perform a step (cycle duration) is longer and the step length is reduced (15). A slower gait, shortened step and impaired gait rhythm in PAD patients has also been reported by Scherer et al. (17). Our results fully confirm the slowing of the gait and the extension of the gait cycle time in PAD patients if compared to healthy subjects.
Two independent research groups Scott et al. and Myers et al. conclude also that the disturbance of gait parameters occurs before the onset of intermittent claudication, at a time while the patient does not feel any discomfort yet (18), (19). Our results confirm the above statements, although the differences are not great.
Comparative analysis of series I, II and III showed no severe changes of speed or single or double support duration.
The results of percentage comparisons of single and double support times, calculated with respect to the duration of the gait cycle indicate however, that patients avoid single support. Single support time calculated as a percentage was shorter in patients, in contrast to the absolute numbers. Percentage of double support time was longer in a group of patients compared to healthy subjects. It was also longer in absolute numbers.
Average double-support time in series II was about 0.065 seconds longer than in controls, single support time was about 0.038 sec longer. For comparison, the average duration of the gait cycle in series II was about 0.208 sec longer than in controls. It can be explained by the fact that series II was performed at post-operative day, the still pain has accompanied the patient resulting from the existence of a fresh wound.
Walking speed in the distant postoperative day increased relative to the speed obtained in the early days after surgery. This may be due to the fact that it is managed to obtain by a surgical procedure an intended effect of arterial endarterectomy and surgical wound has healed, the patient no longer reported pain during walking a 24 m distance. In this study, in series II not only reduced walking speed was observed if compared to series I, but also the greatest inequality of gait in relation to the other two series. This was manifested by increased heterogeneity of single support times within sets of steps in many patients (therefore the average value of heterogeneity was increased).
Exactly the same factors, that cause a decrease in velocity, can affect on the result of the greatest inequalities of gait in the early postoperative day. Pain and load reduction on the operated limb may be the cause of this phenomenon. Similarly, there was a consequence of the improvement of the patient’s condition in the remote postoperative day, no pain complaints, postoperative wound healing, lack of claudication or pronounced elongation of claudication distance cause that the steps heterogeneity observed in the early postoperative day (series III) has decreased in a statistically significant manner.
Results obtained by us partially confirm those, which are reported in the publications. Decreased walking speed in patients with symptoms of intermittent claudication (14, 15, 16) relative to the control group, the variability and heterogeneity of steps, inequality of gait higher in PAD patients compared with the control group (17, 20) – these are conclusions, that also arise from our study.
So far, none of the research teams has assessed gait in PAD patients in correlation with endarterectomy procedure in the femoro-popliteal segment. We were unable to find the publication that evaluated the gait of PAD patients using a CDG system as well. Andrew W. Gardner and his team at MVAHCS in Baltimore performed relatively similar study concerning gait of PAD patients (14). The study was carried out on a shorter distance 7.3 m and pressure sensors mats were used.
CONCLUSIONs
The performed study demonstrates that surgical endarterectomy in the femoro-popliteal segment affected significantly the PAD patient’s gait pattern, especially in the early days after surgery. We believe that endarterectomy within other arteries of lower extremities, at different levels, will effect on the gait quality in PAD patient.
CDG method has been already used by one of the authors of this study (21, 22) for purposes of evaluation of current state of patient. We consider, it can be successfully used to assess of lower limb arterial occlusion and any subsequent rehabilitation of these patients.
Piśmiennictwo
1. Zeller T: Current state of endovascular treatment of femoro-popliteal artery disesase. Vasc Med 2007; 12: 223-234. 2. Norgren L, Hiatt WR, Dormandy JA et al.: Inter-Society Consensus for the Management of Peripheral Arterial Disease (TASC II). J Vasc Surg 2007; 45(Suppl S): 5-67. 3. Criqui MH, Langer RD, Fronek A et al.: Mortality over a period of 10 years in patients with peripheral arterial disease. N Engl J Med 1992; 326(6): 381-386. 4. Daskalopoulou SS, Mikhailidis DP: Medical management of risk factors for vascular disease. Vasc Surg 2004; 22: 10. 5. Bradberry JC: Peripheral Arterial Disease: Pathophysiology, Risk Factors and Role of Antithrombotic Therapy. J Am Pharm Assoc 2004; 44(2), Suppl. 1. 6. Selvin E, Erlinger TP: Prevalence of and risk factors for peripheral arterial disease in the United States: results from the National Health and Nutrition Examination Survey. Vasc Med 2004; 110: 738-743. 7. Allaqaband S, Solis J, Kazemi S, Bajwa T: Endovascular Treatment of Peripheral Vascular Disease. Curr Probl Cardiol 2006; 31: 711-760. 8. Peach G, Griffin M, Jones KG et al.: Diagnosis and management of peripheral arterial disease. BMJ 2012; 345: e5208. 9. Menard MT, Belkin M: Infrapopliteal Intervention for the Treatment of the Claudicant. Semin Vasc Surg.2007; 20: 42-53. 10. Celis R, Pipinos II, Scott-Pandorf MM et al.: Peripheral arterial disease affects kinematics during walking. J Vasc Surg 2009; 49:127-132. 11. Breek JC, Hamming JF, De Vries J et al.: Quality of Life in Patients with Intermittent Claudication Using The World Health Organisation Questionnaire. Eur J Vasc Endovasc Surg 2001; 21: 118-122. 12. Infotronic Datatech (Internet). Available from: http://www.infotronic.nl. 13. Whittle M.Gait Analysis: an Introduction. 4th Ed. Oxford: Butterworth-Heinemann; 2007. 14. Gardner AW, Forrester L, Smith GV: Altered gait profile in subjects with peripheral arterial disease. Vasc Med 2001; 6: 31-34. 15. Crowther RG, Spinks WL, Leicht AS et al.: Relationship between temporal-spatial gait paramteres, gait kinematics, walking performance, exercise capacity, and physical activity level in peripheral arterial disease. J Vasc Surg. 2007; 45: 1172-1178. 16. Mc Cully K, Leiper C, Sanders T, Griffin E: The Effects of Peripheral Vascular Disease on Gait. J Gerontol Biol Sci.1999; 54A: 8291-294. 17. Scherer SA, Bainbridge JS, Hiatt WR: Gait characteristics of patients with claudication. Arch Phys Med Rehab 1998; 79(5): 529-531. 18. Scott-Pandorf MM, Stergiou N, Johanning JM et al.: Peripheral arterial disease affects ground reaction forces during walking. J Vasc Surg 2007; 46: 491-499. 19. Myers SA, Pipinos II, Johanning JM, Stergiou N: Gait variability of patients with intermittent claudication is similar before and after the onset of claudication pain. Clin Biomech 2011; 26:729-734. 20. Crowther RG, Spinks WL, Leicht AS et al.: Lower limb movement variability in patients with peripheral arterial disease. Clin Biomech 2008; 23: 1080-1085. 21. Czerwosz L, Szczepek E, Sokołowska B et al.: Recognition of Posture and Gait Disturbances in Patients with Normal Pressure Hydrocephalus Using a Posturography and Computer Dynography Systems. Hydrocephalus. InTech February; 2012. 22. Czerwosz L, Szczepek E, Sokołowska B et al.: Recognition of gait disturbances in patients with normal pressure hydrocephalus using a computer dynography system. J Physiol Pharmacol 2008; 59(Suppl. 6): 201-207.



