*Konrad Wroński1, Zbigniew Masłowski2, Leszek Frąckowiak1, Przemysław Stefaniak2
Treatment subungual melanoma in foot – case report
1Department of Oncology, Faculty of Medicine, University of Warmia and Mazury, Olsztyn, Poland
Head of Department: prof. Sergiusz Nawrocki, MD, PhD
2Department of Surgical Oncology, Hospital Ministry of Internal Affairs with Warmia and Mazury Oncology Centre, Olsztyn, Poland
Head of Department: Andrzej Lachowski, MD
Summary
Subungual melanoma is rare disease and has worse prognosis than cutaneous melanoma in other places. This type of melanoma is observed accounting for 1 to 3% of all cutaneous melanoma in Caucasians. It is estimated that 1 of every 39 people in the western countries will be diagnosed melanoma of the skin during lifetime. The number of patients with skin melanoma is increasing and cause a growing economic problem for health care. Dermoscopy or videos dermoscopy is the basis for the initial diagnosis of melanoma of the skin. Sensitivity dermoscopy is up to 96.3% and the specificity up to 94.2%. The literature on dermoscopic examination of the nails is limited to very few published observations. Large number of information is available on dermoscopy of pigmented lesions elsewhere on the body skin. Dermoscopy can help clinicians accurately decide if a biopsy of the nail apparatus is necessary in cases of melanoma suspicious. Surgical biopsy of the lesion is the gold standard for diagnosis subungual melanoma. The „gold standard” of treatment is surgical amputation and sentinel lymph node biopsy. In this article the authors presented a case of a woman who was admitted to the hospital because of subungual melanoma in foot. The patient underwent amputation of toe with sentinel lymph node biopsy and in the second day after surgery was discharged home.
INTRODUCTION
Subungual melanoma is rare disease and has worse prognosis than cutaneous melanoma in other places (1). This type of melanoma is observed accounting for 1 to 3% of all cutaneous melanoma in Caucasians (1). It is estimated that 1 of every 39 people in the western countries will be diagnosed melanoma of the skin during lifetime (2). The number of patients with skin melanoma is increasing and cause a growing economic problem for health care.
CASE REPORT
A 71-year-old woman, Caucasian race, was admitted to the Department of Surgical Oncology because of diagnosed subungual melanoma of the right feet. In an interview with the patient, she informed us that the black spot under the nail was observed three months earlier and gradually expanded. The patient reported no pain in the area of melanoma. Surgical biopsy showed subungual melanoma.
She had no any other symptoms, there was no history of weight loss and loss of appetite. The patient was treated chronically with hypertension and ischemic heart disease. She had no surgeries before and there was no history of carcinoma (especially skin melanoma) in patient family. Blood test and other routine hematological examinations and biochemical tests were within normal limits.
On physical examination, the right great toe nail plate was changed by the a fungal infection with a prominent black spot with a diameter of about 5 mm under the nail (fig. 1). There were not enlarged inguinal lymph nodes. Also ultrasound examination of the inguinal lymph nodes did not show pathologically enlarged lymph nodes.
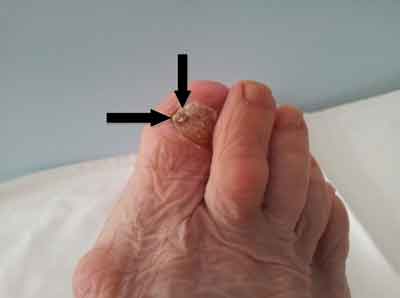
Fig. 1. Subungual melanoma in right foot.
The patient was qualified for surgery, she underwent amputation of the right toe with sentinel lymph node biopsy. Pathological examination revealed subungual melanoma and there was no melanoma cells in sentinel lymph node. The duration of surgery was 50 minutes. Patient after surgery felt good and did not complain of pain. The postoperative period was uncomplicated and the patient left the ward in the second day after operation. The patient is in the care of outpatient surgical oncology.
DISCUSSION
Subungual melanoma is uncommon disease but prognosis in this disease are worse than in skin melanoma in other sites (3). The 5-year survival rate is from 16 to 87% (3, 4). Ultraviolet radiation exposure is the main factor which penetrate the nail plate cause subungual melanoma (5).
Subungual melanoma is observed more in men than women and mean age is 55.5 years old (6). The most often, this type of melanoma is observed between 50-70 years old. This disease is diagnosed more often in Asian and African than in Caucasian. It is presented as a discoloration of nail, a mass, bleeding tumor and a non-healing wound (7). Subungual melanoma is observed more often in the hands than in the feet with ratio 3:2 (6).
Dermoscopy or videos dermoscopy is the basis for the initial diagnosis of melanoma of the skin. The simplest dermoscopy technique, called the „three-point dermoscopy scale”, is based on clinical suspicion of melanoma for two things meet the following three criteria: 1) asymmetric distribution structures in the lesion, 2) atypical grid pigmentosa, 3) blue-white veil. Sensitivity dermoscopy is up to 96.3% and the specificity up to 94.2%. The literature on dermoscopic examination of the nails is limited to very few published observations. Large number of information is available on dermoscopy of pigmented lesions elsewhere on the body skin. Dermoscopy can help clinicians accurately decide if a biopsy of the nail apparatus is necessary in cases of melanoma suspicious. Surgical biopsy of the lesion is the gold standard for diagnosis subungual melanoma. The „gold standard” of treatment is surgical amputation. Randomized controlled showed that sentinel lymph node biopsy should be done, but there are observed some implications for melanoma with intermediate thickness (1.2 to 3.5 mm) (8). Lymphadenectomy is necessary in case of positive sentinel lymph node biopsy. Elective lymph node dissection does not affect patient survival (9, 10).
The authors of this article recommend wild surgical amputation due to subungual melanoma with uninvolved margins and sentinel lymph node biopsy. Treatment of this disease should be done in highly specialized oncological surgery wards with experience in such operations.
Piśmiennictwo
1. Blessing K, Kernohan NM, Park KGM: Subungual malignant melanoma: clinicopathological features of 100 cases. Histopathology 1991; 19(5): 425-429. 2. Riker AI, Zea N, Trinh T: The epidemiology, prevention and detection of melanoma. The Ochsner Journal 2010; 10: 56-65. 3. Thai KE, Young R, Rd S: Nail apparatus melanoma. Austral J Dermatol 2001; 42: 71-83. 4. Banfield CC, Dawber RPR: Nail melanoma: a review of the literature with recommendations to improve patient management. Br J Dermatol 1999; 141: 628-632. 5. Bruls WAG, Slaper H, van der Leun JC, Berrens L: Transmission of human epidermis and stratum corneum as a function of thickness in the ultraviolet and visible wavelengths. Photochemistry and Photobiology 1984; 40(4): 485-494. 6. O’Leary JA, Berend KR, Johnson JL et al.: Subungual melanoma. A review of 93 cases with identification of prognostic variables. Clinical Orthopedics and Related Research 2000; 378: 206-212. 7. Cohen T, Busam KJ, Patel A, Brady MS: Subungual melanoma: management considerations. Am J Surg 2008; 195: 244-248. 8. Morton DL, Thompson JF, Cochran AJ et al.: Sentinel node biopsy or nodal observation in melanoma. New Engl J Med 2006; 355: 1307-1317. 9. Sim FH, Taylor WF, Pritchard DJ, Eh S: Lymphadenectomy in the management of stage I malignant melanoma: a prospective randomized study. Mayo Clinic Proceedings 1986; 61: 697-705. 10. Cascinelli N, Morabito A, Santinami M et al.: Immediate or delayed dissection of regional nodes in patients with melanoma of the trunk: a randomized trial. Lancet 1998; 351: 793-796.
