© Borgis - New Medicine 2/2012, s. 52-62
*József Rácz1,2, Ferenc Márványkövi1, Zsolt Petke2,3, Katalin Melles1, Anna Légmán1, István Vingender4
The barriers to obtaining treatment for Roma and non-Roma intravenous drug users in Budapest, Hungary: a group comparison
1Institute of Psychology, Eotvos University Budapest, Hungary
Director of the Institute: Dr. Zsolt Demetrovics, PhD
2Department of Addiction Medicine, Faculty of Health Sciences, Semmelweis University Budapest, Hungary
Dean of the Faculty: Dr. Judit Mészáros, PhD
Doctoral School of Pathology, Semmelweis University, Budapest, Hungary
Program coordinator Prof. István Szabolcs, DSc
4Department of Social Studies, Faculty of Health Sciences, Semmelweis University Budapest, Hungary
Dean of the Faculty: Dr. Judit Mészáros, PhD
Summary
Introduction. The authors analysed the social exclusion of intravenous Roma and non-Roma drug users who are outside the treatment system. The goal of the study was to explore the barriers to treatment of the two groups and to see if the Roma group had a lower access rate to drug treatment.
Methods. Subjects: There were 70 Roma and 70 non-Roma subjects from clients of needle exchange services and their friends. The subjects were recruited by snowball techniques in Budapest (capital of Hungary). The two group members were selected to be similar in terms of their major socio-demographic characteristics. A questionnaire was developed regarding barriers to treatment and the need for treatment as well as regarding their drug use and risky behavior.
Results. Indicators of social exclusion suggest a less favourable situation for the Roma subjects (education, employment, source of income, criminality). On the basis of their drug use and high-risk behavior, the Roma are not a higher risk group (injecting drug use, frequency of drug use, sharing behavior, hepatitis testing, hepatitis C infection, participation in needle exchange service). The probability of obtaining treatment can not be explained by ethnic background.
Conclusions. Roma drug users are at a greater risk from a social standpoint, while in relation to health and drug behavior, they are at a lower risk. The results do not fit in with earlier studies on Roma populations with high risk drug using profiles. Regarding the study’s results, some limitations can be considered: low number of subjects studied, the special populations from needle exchange services.
INTRODUCTION
According to the Council of Europe, there are approximately 10 million Roma in Europe (estimates vary from 8 to 15 million; “approximately 10 million” seems to us to be the best estimate). They are mainly found in the Balkans and in Central and Eastern Europe (2). According to the Council of Europe’s data on the Roma population in Hungary, the official number of Roma people (according to the 2001 census) is 190,046. The estimated numbers are between 400,000 and 800,000 (2). In Hungary, most of the Roma people do not speak a Roma language (3). The total population of Hungary is 10 million inhabitants.
“The 1993 Hungarian Act on the Rights of National and Ethnic Minorities (Minorities Act) clearly made ethnic classification the exclusive right of the individual. Self-identification has thus become the sole legal ground for defining ethnicity” (3 p. 14). This is why we asked study persons to identify their own ethnicity. We also note that “The words Roma (Roma) and cigány (Gypsy) are used as synonyms in Hungary, although there is no consensus on the correct, un-stigmatised name” (3 p. 16).
With regard to the characteristics of Roma groups in terms of drug use, we must first note that both the international and domestic data are either insufficient or inconsistent. One reason for this is that during the course of data collection it is not permitted to ask about ethnic origins in the examination of a large, representative sample, and on the other hand the existing research does not completely satisfy numerous methodological criteria. In the latter case, we believe that it is primarily the lack of a representative sample (in many cases, the studies in question are local studies) and the reliability of the sources of information (experts’ estimates) which can significantly influence the ability to interpret and make generalizations from the data. We are attempting to provide an overview of the barriers preventing Roma individuals from obtaining treatment through a review of international (European) and domestic literature.
International studies: Roma drug users not undergoing treatment
The study by Grund, Öfner and Verbraeck (4) states that Roma drug users in the central European region are less willing to seek out assistance with social or healthcare issues, including low-threshold services. This increases their marginalized status, while marginalization contributes to their unwillingness to seek aid. The discrimination and stigmatization of Roma drug users can also be felt in the treatment facilities, as well as in the wider realm of society. The study performed by the United Nations Development Programme (5) highlights the fact that one of the impediments to obtaining basic healthcare and social assistance – in addition to geographic distance – is the lack of information, which represents a barrier for both Roma drug users and non-users.
British and Dutch researchers (6-9) – also basing their studies primarily on the opinions of experts – examined the factors which keep members of ethnic minorities, including Roma drug users, away from the various treatment programs available. On the basis of these studies, they identified the following factors which make it more difficult to receive treatment for drug addiction:
– The lack of cultural sensitivity: the treatment centers do not take into account the family’s primary role in Roma groups, or ignore the opportunity to bring family members into the treatment programs;
– Fearing stigmatization, the Roma users do not dare to resort to seeking treatment;
– The differing backgrounds of the treatment workers and the users: the non-Roma professionals do not show sufficient cultural sensitivity and empathy;
– Mistrust of the treatment centers;
– Language difficulties.
During an Irish study in 2005 of itinerant Roma groups, (10) identified the following factors which make it more difficult for these people to receive healthcare treatment:
– The lack or low degree of knowledge about treatment types;
– The low level of schooling and education in itinerant Roma groups, and the illiteracy that arises from this;
– Discrimination and stigmatization of the Roma in healthcare at the individual and institutional levels;
– The concealment from professionals of problems arising from drug use;
– The lack of treatment programs specific to the culture and target group;
– The lack of cultural sensitivity in the relevant institutions.
Data was collected from primary sources in Bulgaria (11), providing more information about Roma drug users in Sofia. The workers at the Sofia needle exchange center identified the lack of healthcare provision for Roma intravenous drug users as the most commonly experienced difficulty (81%). They named the low level of education and the state of their health as being secondary concerns, and poor living conditions, the closed nature of the Roma community and discrimination as further barriers. Research performed on a sample from a Spanish treatment center that deals with drug users studied the likelihood that Roma and non-Roma drug addicts would remain in treatment (12). The results showed that remaining in treatment is more likely in the case of non-Roma addicts, although the result was not statistically significant. An important component of the analysis was that a history of treatment has an impact on whether or not users remain in treatment, and this impact is significant in the case of Roma drug users. The importance of this is that in the case of the Roma, the socializing effect of a history of treatment is significant as regards the success of their continuing course of treatment. In conclusion, it is worth mentioning Subata’s (1997) (13) research, who observed at a methadone maintenance center in Vilnius that the Roma drug users did not make use of the services, due on the one hand to geographic distance, and on the other to a lack of trust in the workers there. In Spain, due to similar difficulties, the criteria for receiving methadone maintenance treatment were relaxed (14).
Hungarian studies: Roma drug users not undergoing treatment
In practice, no focused study has been conducted in Hungary that has made a comprehensive attempt to uncover the drug use characteristics and patterns of the Roma, or to explore the barriers they meet in obtaining treatment. Although certain researchers have dealt with the topic in a secondary manner (15, 16), the only comprehensive and focused study was conducted by Ritter (2005) (17), who – even if only to a minor degree – studied the barriers to obtaining treatment. Of the drug users questioned, 4.5% indicated that they had taken part in a treatment program for their drug problem. This meant primarily in-patient hospital treatment or an out-patient drug clinic. Of these, a total of only two people stated that they underwent treatment because they needed it; it was far more typical that they sought out an aid center due to advice or pressure from their immediate environment (family members or friends). The researchers did not examine the possible reasons for such a low percentage of Roma drug users who had participated in a treatment program. At the same time, it is an interesting fact that more than three-quarters of those questioned (76.7%) knew a Roma youth who, according to their opinion, was in need of treatment, but had not entered into a program. They saw the primary reason for this as being that the person in question did not want to quit, or did not feel the need for treatment.
The limitation of this research was that there was no opportunity for a comparison with non-Roma drug users in terms of either the frequency of drug use or enrollment in treatment programs, or in connection with the reasons for the barriers and difficulties in obtaining treatment.
From the synopsis above of the literature, it is therefore easy to see that numerous factors influence the entrance into, the need for and the seeking out of treatment by problematic drug users, including users of intravenous drugs. The research and studies outlined above suggest that numerous factors are not specific to culture or background; they may be found equally in groups of both Roma and non-Roma intravenous drug users. At the same time, we repeatedly met with explanations relating to discrimination due to the subjects’ Roma ethnic origins and the shortage of information, as well as factors arising from the Roma culture and way of life, such as the closed nature of the Roma community and the differing attitudes of the Roma to their health and physical condition.
There are several methodological problems with Roma drug users, it is also a problem that who many are in treatment and what the main barriers are to get treatment. A speacial geographical region (the 8th district of Budapest) was chosen, wher Roma snd non- Roma drug users live together. Here a needle exchange program is run so we can study the clients of this program.
The objectives of the research were to:
– Explore the characteristics of socially excluded (and at the same time those not undergoing treatment) intravenous drug users, as regards their drug use, and furthermore the types of service they obtain (or do not obtain);
– Discover what knowledge Roma and non-Roma intravenous drug users have about the various treatment programs, identify their reasons for not entering into treatment and uncover their relationship with and attitudes towards the treatment system;
– Explore the differences in drug use patterns between Roma and non-Roma users, and the high-risk or preventative behaviors related to their drug use;
– Identify the characteristics of the intravenous drug users who classify themselves as Roma and non-Roma, assuming that the drug users who classify themselves as Roma do not represent a homogenous group.
Methods
Sample
Intravenous drug users can be considered as a hidden target population, with whom the traditional random sampling and data acquisition procedures cannot be employed, or can only be employed in a limited fashion (24).
The study was carried out in the capital (Budapest: 2 million inhabitans), in the 8th district of Budapest (82.000 inhabitans). Here, the Blue Point Drug Counselling and Outpatient Centre runs a needle exhange service. The clients of this service were the points of snowball samples of the study groups.
During the course of the research, 70 Roma intravenous drug users who were not in treatment programs were questioned, as well as a further 70 non-Roma as a comparison group (total: 140 persons). For the purpose of comparability, the major socio-demographic and drug use characteristics of the group being examined and the control group were similar. The formation of the comparison sample occurred continuously during the course of the data collection process, at the same time as the Roma sampling, using a so-called quota sample. This method of sampling required the continuous registration of quotas based on major socio-demographic characteristics, and the continuous supervision of the data collection process (12).
Data collection
During the course of the research, in addition to the utilization of questions that could be adapted from international surveys (regarding the socio-demographic background, treatment history, health and social status, drug use habits, perception of risks relating to infection and barriers to obtaining treatment of the drug users), there were also operationalization questions regarding the attitudes of the intravenous drug users towards the people providing the services.
The assessment methods that we took into account during the development of the questionnaire and that we wanted to use in order to measure the barriers to obtaining healthcare and social welfare treatment, as well as for measuring social exclusion, were adapted from the following:
1. The barriers to obtaining treatment for intravenous drug users on the street in New York (18);
2. Barriers to obtaining treatment for illegal drug users in Australia (19);
3. The need for medical and psychosocial treatment amongst intravenous drug users in a treatment sample (20);
4. The previously validated Hungarian version of the questionnaire examining the habits of intravenous drug users developed by the National Institute on Drug Abuse (NIDA) (21);
5. A questionnaire which we produced ourselves that was utilized during the course of research performed amongst problematic drug users in Budapest who were not in treatment programs (22);
The Heroin Severity Dependence Scale that has been used in international research and has also been validated in Hungary was included in the questionnaire (21, 23).
Following a period of instruction regarding the pre-prepared, partially structured interviews, they were conducted in the street by social workers participating in the research and who were employed by low-threshold service providers.
Procedure
The data sampling occurred between December 2007 and March 2008.
During the course of the study, we creat a sample of 70 non-Roma drug users who were not undergoing treatment to the snowball sample consisting of 70 Roma (total: 140 persons). During this alignment process, we took into account two considerations in addition to the appropriate drug use history: the sex and age of the subjects. The configuration of the two samples occurred continuously, with the basis being the Roma sample, and the interviewers had to constantly align the “non-Roma” sub-sample in order to agree with the other group. We determined that the difference in age could be +/- two years. During the snowball sampling of the “Roma” sample, our objective was for the questioning to be initiated from as many points as possible, and that the chain should be as long as possible. The drug users received a 1,000 Hungarian Forint shopping voucher in exchange for taking part in the interview.
We entered the interview data into the Statistical Package for the Social Sciences (SPSS) database, and the processing of the data also occurred with the help of this statistical software package.
Considerations for research ethics
The Scientific Research Ethics Board of the Hungarian Academy of Sciences’ Psychological Research Institute issued the required ethics permit for the research. We also consulted the Office of the Parliamentary Commissioner for Data Protection.
Results
Univariate analysis methods
Socio-demographic indicators
The majority of the drug users in the samples were male, 18-35 years old and single but living with someone. Most people in the sample did not complete either elementary or secondary school. The number of homeless people was insignificant. The proportion of those raising a child/children was relatively high (39%). Nowhere did a significant difference develop between the two sub-groups in terms of their socio-demographic data.
Table 1. The presentation of the sample according to socio-demographic characteristics.
| | Non-Roma drug users | Roma drug users | Full sample |
| Sex | | | |
| Male | 67.1 | 80.0 | 73.6 |
| Female | 32.9 | 20.0 | 26.4 |
| Age group | | | |
| 18-25 years old | 28.6 | 37.1 | 32.9 |
| 26-30 years old | 32.9 | 38.6 | 35.7 |
| 31-35 years old | 21.4 | 14.3 | 17.9 |
| 36 years old or above | 17.1 | 10.0 | 13.6 |
| Size of household | | | |
| 1 person | 14.3 | 7.1 | 10.7 |
| 2 people | 28.6 | 17.1 | 22.9 |
| 3 people | 24.3 | 27.1 | 25.7 |
| 4 people | 20.0 | 21.4 | 20.7 |
| 5 people or more | 12.9 | 27.1 | 20.0 |
| Number of children in the household | | | |
| No children | 71.4* | 50.0* | 60.7 |
| 1 child | 18.6* | 27.1* | 22.9 |
| 2 or more children | 10.0* | 22.9* | 16.4 |
| Marital status | | | |
| Single | 57.1 | 48.6 | 52.9 |
| Married | 7.1 | 8.6 | 7.9 |
| Cohabiting | 25.7* | 37.1* | 31.4 |
| Divorced | 7.1 | 5.7 | 6.4 |
| Widow/widower | 2.9 | | 1.4 |
| Who are you living with? | | | |
| No-one/alone | 12.9 | 10.0 | 11.4 |
| Spouse | 2.9 | 11.4 | 7.1 |
| Partner | 30.0 | 30.0 | 30.0 |
| Parent(s) | 48.6 | 44.3 | 46.4 |
| Friends | 8.6 | 5.7 | 7.1 |
| A child under 18 years of age | 14.3 | 35.7 | 25.0 |
| Other family | 24.3 | 25.7 | 25.0 |
| Other adults | 2.9 | 10.0 | 6.4 |
| Level of education | | | |
| Lower than 8th grade | 7.1 | 20.0 | 13.6 |
| 8th grade | 20.0 | 38.6 | 29.3 |
| Incomplete vocational secondary school education | 17.1 | 22.9 | 20.0 |
| Incomplete high school education | 5.7 | 1.4 | 3.6 |
| Vocational secondary school diploma | 28.6 | 14.3 | 21.4 |
| High school diploma | 12.9 | | 6.4 |
| National Instruction Registry training | 4.3 | 2.9 | 3.6 |
| Incomplete college or university education | 2.9 | | 1.4 |
| College or university diploma | 1.4 | | 0.7 |
| Living conditions | | | |
| Self-owned residence | 17.1 | 15.7 | 16.4 |
| Other residence | 42.9 | 32.9 | 37.9 |
| Tennant | 11.4 | 12.9 | 12.1 |
| Homeless shelter | 1.4 | | 0.7 |
| Street | 4.3 | 2.9 | 3.6 |
| Squat | 8.6 | 2.9 | 5.7 |
| Municipal housing | 11.4 | 32.9 | 22.1 |
| Other | 1.4 | | 0.7 |
| No response | 1.4 | | 0.7 |
*p < 0.05
Drug use characteristics
On the basis of a survey of the life prevalence values of particular illegal drugs, we can see that the value for amphetamines is the highest in both sub-samples, and this is followed by marihuana. Significant differences between the Roma and the non-Roma participants can be observed in two areas: in the case of non-prescribed methadone (purchased on the street), and for hypnotics and sedatives.
As regards the participants’ drug use in the past 30 days, we can see that the use of amphetamine derivatives was the most common practice, particularly amongst Roma drug users, amongst whom the proportion who had used these kinds of drugs was 83%. Over half of the sample also used marihuana on a regular basis, and nearly a third of the sample took sedatives and hypnotics not in accordance with doctor’s recommendations. The use of amphetamines and ecstasy was more typical of the Roma population, while the use of heroin as well as hypnotics and sedatives was characteristic of the non-Roma population.
With regard to initial use, we observed that in the cases of both the Roma and non-Roma drug users, the initial regular use of marihuana occurred earliest, while the use of non-prescribed methadone occurred last. There was no significant difference between the two sub-samples for any drug.
On the basis of the international scale for measuring drug dependence (fig. 1), in which the larger values indicate greater levels of dependence, all of those questioned received a score between four and 16. The entire sample studied had an average dependence value of 9.52, which includes an average value of 10.2 for the Roma sample and 8.8 for the non-Roma sample. The difference between the two samples proved to be significant (t = 3.8; p<0.001).
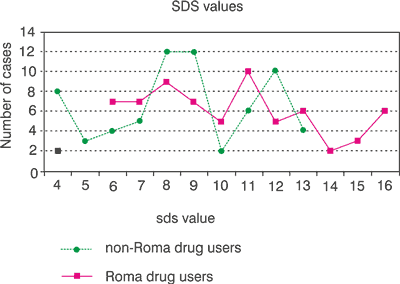
Fig. 1. Severity dependence scale (min: 4, max: 16).
Table 2. Prevalence values for illegal and legal drugs (lifetime prevalence, %).
| | Non-Roma drug users | Roma drug users | Full sample |
| Injecting heroin | 64.3 | 62.9 | 63.6 |
| Injecting amphetamines | 97.1 | 95.7 | 96.4 |
| Non-prescribed methadone | 37.1* | 23.2* | 30.2 |
| Marijuana | 88.6 | 928 | 90.6 |
| Ecstasy | 74.3 | 79.7 | 77.0 |
| Hypnotics and sedatives | 62.9* | 42.0* | 52.5 |
*p < 0.01
Forms of high-risk behavior
Although the incidence rate of the sharing of needles in the last 30 days was low for the total sample, as well as for both the Roma and non-Roma populations, the values for the other forms of risky behavior were high. Amongst the differences examined, there was a significant disparity between the Roma and non-Roma populations relating to the incidence of sharing paraphernalia in the last 30 days.
Infections and participation in screening
In connection with inquiries about HIV and hepatitis, it can be stated that there was a disparity between the Roma and the non-Roma as regards their participation in screening, but that this difference was not significant. While 80.0% of the Roma had been screened for HIV, 71.4% of the non-Roma had, and 84.3% of the Roma and 73.0% of the non-Roma had been screened for hepatitis at some point in their lives.
Only one individual in the sample was found to be HIV positive. In contrast with the rate of HIV infection, one-fifth of the total sample was positive for hepatitis, while 39.9% of them thought they were not. While the Roma and the non-Roma had an HCV infection rate of 27.1% and 11.4%, (on the basis of the screening results; p<0.05), the proportion of those who were not infected was nearly the same for the Roma (38.6%) and the non-Roma (40.0%) on the basis of their own admission. It is an interesting fact that one-fifth of the sample could not say, or did not respond to the question (Roma: 18.6%; non-Roma: 21.4%), and that 21.4% of the entire sample had not been screened for hepatitis. With regard to hepatitis, 27.1% of the non-Roma and 15.7% of the Roma had not been tested. These disparities were statistically significant, although barely so (10.71; p<0.05).
The relationship with the treatment system for drug users who were not undergoing treatment
Participation in low-threshold services (needle exchange)
The data relating to needle exchanges shows that a significant portion of those in the sample (92.8%) had utilized these kinds of services in some form during their lives. Amongst the Roma, this was true of everyone, and 85.7% of the non-Roma admitted to using needle exchanges. This disparity is significant. Of the entire sample, 84.3% had participated in needle exchanges in the last 30 days. This included an overwhelming majority of the Roma (94.3%), and three-quarters (74.3%) of the non-Roma (18.65; p<0.001).
Treatment history
Taking into account the participants’ treatment histories, we can see that 20% of the sample had been in one of the types of treatment studied during the course of this research, with the proportion being slightly higher for the Roma drug users than the non-Roma, although this disparity was not significant. Amongst those with a history of treatment, the majority (n=25) had participated in only one form of treatment, and only three respondents had participated in two different forms of treatment.
Attempts and experiences relating to obtaining treatment
We also explored any unsuccessful attempts at enrolling in programs in relation to the subjects’ history of obtaining treatment. Of the entire sample, 19% (27 individuals) had attempted to enroll in some kind of treatment program, but were not successful. There was a significant disparity between the two sub-samples as regards these unsuccessful attempts (p<0.05). In the case of the Roma drug users, the percentage who did not receive treatment despite trying to enroll was 24%, while for the non-Roma drug users this was 14%.
Unsuccessful attempts at enrolling in methadone treatment were the most common, while smaller proportions of the participants had made unsuccessful attempts at obtaining out-patient or hospital in-patient care. The reasons given for failing to gain admittance were most often a lack of space, or in other words they were put on the waiting list but did not obtain the services.
Multivariate analysis methods
In connection with assessing the participants’ treatment histories or what treatment they had obtained, we performed a logistic regression where we entered the variables that showed deviation into a single-variable statistical proof. These variables were: age; sex; level of education; ethnic background (Roma/non-Roma); drug addiction (on the basis of the Severity Dependence Scale); the length of drug use and whether the participants had drug users who had received treatment amongst their friends and family members (yes or no).
On the basis of the analysis of the logistic regression, we can state that amongst the numerous factors that we examined, only the level of drug dependence had an independently significant impact on the participants’ treatment histories, or in other words, the chance of entering into treatment increased with an increase in drug dependence (OR = 0.41; p<0.001).
Assessment of treatment obtained
We assessed the drug users who were not undergoing treatment with the aid of a five-tiered scale, as to how difficult or easy they considered it to enroll in particular types of treatment programs. In connection with assessing the difficulty of enrolling in treatment programs, we can see that both sub-samples considered obtaining methadone treatment to be the most difficult, while out-patient treatment proved to be the easiest to receive, although hospital in-patient treatment had a similar value. No significant disparity developed between the two sub-samples.
In connection with admittance to the particular treatment centers, we also examined which factors influenced the assessment process, or, in other words, we examined the background factors which the drug users thought made it harder to enter certain treatment centers. We performed this examination using a multi-variable linear regression analysis. We examined the four different types of treatment separately, utilizing the same independent variables in each case. The dependent variables employed during the analysis were the assessment of admittance to the particular types of treatment (on a scale of 1-5).
The independent variables employed during the analysis were: sex; age; ethnicity; length of drug use; level of drug dependence; treatment history and number of attempts to enroll for treatment.
We found that amongst the background factors which we included, the level of drug dependence and the history of treatment within the family both had an independent impact on the assessment of admittance to methadone treatment. This means that the more dependent the drug users were, the more difficult they considered it to be to enroll in a methadone program (R = 0.18; p<0.001). Furthermore, the drug users who did not have any drug users who had previously received treatment in their family considered admittance into treatment to be more difficult (R = 0.9; p<0.001). The other independent variables did not have any significant individual impact.
Regarding the assessment of out-patient treatment, the results indicated that, amongst the background factors which we included, the treatment history of those questioned and their family members had an impact. Therefore, we can state that if the individuals questioned had themselves been in some form of treatment, then they considered the chance of receiving out-patient treatment to be more likely (R = 0.76; p<0.05). In contrast to this, if the individuals questioned had a family member who had received some form of treatment, then they considered admittance to be more difficult (R = 0.76; p<0.05).
The other independent variables did not play a significant role in how difficult it was considered to be to obtain out-patient treatment.
In terms of the assessment of rehabilitation treatment, the results indicated that, amongst the independent factors included in the analysis, the only one with a significant individual impact was Roma ethnicity. According to this research, the Roma drug users considered admittance to be more easily obtained than the non-Roma drug users did (R = 0.79; p<0.05).
In connection with the assessment of hospital in-patient treatment, we saw that only the variable relating to drug dependence had an independent impact. In other words, those questioned who had a greater level of dependence on drugs considered it to be easier to obtain hospital in-patient treatment (R = 0.1; p<0.05).
Table 3. Drug use in the last 30 days (%).
| | Non-Roma drug users | Roma drug users | Full sample |
| Injecting heroin | 57.1* | 40.0* | 48.6 |
| Injecting amphetamines | 61.4* | 82.9* | 72.1 |
| Non-prescribed methadone | 17.1 | 5.7 | 11.4 |
| Marihuana | 51.4 | 54.3 | 52.9 |
| Ecstasy | 12.9* | 21.4* | 17.1 |
| Hypnotics and sedatives | 40.0* | 24.3* | 32.1 |
*p < 0.01
Table 4. Incidence of forms of high-risk behavior at any time and in the last 30 days (%).
| | Non-Roma drug users | Roma drug users | Full sample |
| Sharing of needles at any time | 60.0 | 51.4 | 55.7 |
| Sharing of needles in the last 30 days | 7.1 | 11.4 | 9.3 |
| Sharing of paraphernalia (filters, strainers etc.) at any time | 70.0 | 80.0 | 75.0 |
| Sharing of paraphernalia (filters, strainers etc.) in the last 30 days | 44.3* | 60.0* | 52.1 |
*p < 0.01
Discussion
On the basis of the results of this research, we were provided with a relatively diverse picture of Roma and non-Roma drug users who were not undergoing treatment. In the various dimensions of the study, we observed that while there was a fairly significant disparity between the two groups regarding certain questions, they had very similar characteristics in other aspects. This also meant that neither the Roma drug users nor the non-Roma drug users constituted in themselves a homogenous group.
During this research, a study was performed on 70 Roma and 70 non-Roma subjects who were not undergoing treatment, but were clients of two low-threshold needle exchange programs in Budapest. As well as the fact that the subjects were not undergoing treatment, it was important that the sample also included those who had never been in any kind of treatment program (this was true in the majority of cases), and also those who had at least a three year history of regular drug use, as the healthcare and social problems that would indicate the need for treatment would be most likely to arise in this period of time.
The indicators of social exclusion suggested a less favorable situation for the Roma drug users, as on average they had a lower level of education, had less favorable indicators as regards employment status, were in a somewhat more uncertain situation regarding the sources of income and were more likely to have a criminal record. All of these show a great similarity to the results of earlier research on itinerant Roma groups performed by Fountain (10). It seems that the Roma who were part of the sample also bear the marks of social exclusion that are characteristic of a significant portion of Hungarian Roma groups (25).
On the basis of other characteristics of drug use, forms of high-risk behavior and health characteristics, we can state that the Roma drug users cannot be considered to be at a higher risk as a group in terms of their frequency of drug use, drug use history or sharing of needles. Moreover, it can be established regarding their state of health and certain health-related behaviors that there is not a significant difference between the Roma and non-Roma people. This relates on the one hand to chronic illnesses, or those which occur due to drug use, as well as permanent damage to their health, and on the other hand to their participation in screening programs. A greater percentage of Roma drug users had taken part in the various screening programs, particularly in the last one to two years, and took advantage of the needle exchange service to a significantly greater degree, typically at the participating local organization.
In addition to all of this, it is important to mention that ethnic background did not have an impact in connection with the probability of obtaining treatment, or, in other words, Roma ethnicity did not make it more probable that someone would not receive treatment. As was observed, it was only the level of drug dependence that had a significant independent impact in relation to treatment history. This result is even more interesting in light of the fact that the Roma were more likely to attempt to obtain treatment, even if they were unsuccessful. In connection with this, during the course of our earlier research performed in Budapest amongst intravenous drug users who were not receiving treatment (22), we observed that two factors influenced whether or not treatment was obtained to a significant degree: the length of the subject’s history of drug use, and their level of education. Those with a longer history of drug use and with a higher level of education were more likely to enter into some kind of treatment. However, during the course of the present research, this connection could not be established. Only ethnic origin had an independent impact on the assessment of rehabilitation treatment; the Roma drug users considered enrollment to be easier than the non-Roma drug users. Our primary hypothesis in connection with this is that it could be that the Roma intravenous drug users were unfamiliar, or were less familiar, with this form of treatment, a fact which has been highlighted in other research relating to Roma drug users being less well informed (5, 10). At the same time, it may also be postulated that the intravenous use of amphetamines (which is more characteristic of the Roma) does not produce a need for that kind of treatment, or the consequences which would require rehabilitation treatment. This would explain why their knowledge of this form of treatment is lacking, because the Roma people do not know about it, even indirectly.
At the same time, there was no difference between the Roma and non-Roma in connection with their opinions about obtaining hospital, out-patient or methadone maintenance treatment. The first two are uniformly considered to be moderately difficult, regardless of the subject’s ethnic background, while obtaining methadone treatment was judged to be difficult. All of this seems to underscore that prejudice against the Roma did not factor in amongst the reasons stated either for being unsuccessful in entering treatment or for not seeking it out.
Therefore, some of the results from this research do not support certain results and hypotheses from earlier research. The conclusion reached by Grund, Öfner and Verbraeck (4), who stated that Roma drug users are not as willing to seek out social or healthcare assistance, can be refuted, including for low-threshold services. Discrimination or stigma could not be observed in connection with the Roma intravenous drug users who took part in the research, at least in terms of their chances of being admitted for treatment, as well as in their assessment of unsuccessful attempts at obtaining treatment or enrollment in the various forms of treatment. This is in contrast with the results of other research (6-10).
The lack of cultural sensitivity towards the Roma by organizations (10) may be called into question by our research results, according to which participation in screening and needle exchanges is more characteristic of Roma drug users than others. Furthermore, a greater proportion of Roma than non-Roma drug users take part in street needle exchange programs, which are still underdeveloped in Hungary.
Regarding the situation in Hungary in terms of groups of intravenous drug users, we must also greet with skepticism the conclusion of Grund, Öfner and Verbraeck (4), according to whom Roma drug users represent a special group within drug users: they start their drug use earlier and exhibit more high-risk behaviors, the result of which is that they have a higher occurrence of various infectious diseases (HIV and hepatitis B and C). It seems that this conclusion was perfunctory, or that it at least bore the limitation that it was for the most part based on consultations with experts and chief spokespeople.
Our study indicated that the use of amphetamines and ecstasy is more typical in the Roma population, while the use of heroin, hypnotics and sedatives are characteristic of non-Roma intravenous drug users. Taking into account that the risk of overdosing is more likely in the case of sedatives, the non-Roma intravenous drug users in the sample are potentially at greater risk.
Nor can the Roma intravenous drug users in the sample be characterized as a homogenous group, as Ritter (17) had previously suggested, which was another factor used by Grund, Öfner and Verbraeck (4) in their determination of homogeneity.
Table 5. Assessment of the difficulty of enrolling in particular types of treatment programs.
| | Methadone treatment | Out-patient treatment | Rehabilitation | Hospital in-patient treatment |
| Non-Roma drug users | 3.60 | 2.47 | 3.16 | 2.58 |
| Roma drug users | 3.49 | 2.51 | 2.68 | 2.43 |
| Full sample | 3.54 | 2.49 | 2.92 | 2.51 |
Conclusions
In relation to the marginalization of Roma and non-Roma intravenous drug users from Budapest who are not undergoing treatment, the results of this research in its entirety indicate that Roma drug users seem to be at higher risk from a social perspective, while in connection with health issues linked to drug use their level of exclusion is no so significant or in certain respects not excluded at all. In order to answer all of these questions in more depth, more precise research is needed.
Limitations
One limitation of this research was that the study only extended to intravenous drug users from Budapest who were not receiving treatment, but they participated in needle exchange services. Second, during the sampling process, we did not have the opportunity to take into account all of the districts of Budapest (e.g. Újpest and Csepel) where intravenous drug use is also present. It was primarily drug users who were contacted by workers at the Kék Pont Drug Clinic or the Drug Prevention Foundation that became part of the sample. In order to counterbalance this, we employed sampling methods which helped to reduce or minimize the aberrations arising from the data acquisition during the research process.
Acknowledgements
We would like to express our thanks to employees of the Kék Pont Drug Consultation Center and Drug Clinic Foundation and the Drug Prevention Foundation. This research was supported by the Ministry of Social Affairs and Labor (KAB).
Piśmiennictwo
1. Project on ethnic relations: Roma and statistics. Princeton, New Jersey 2000. 2. Pedotti C, Guet M: Roma and travelers glossary. Compiled by Pedotti C (French translation department) and Guet M (DGIII Roma and travelers division) in consultation with the English and French translation departments and Aurora AILINCAI (DGIV Project “Schooling for Roma Children in Europe”). Kindly translated into English by Nash V (English translation department). Strasbourg: Council of Europe; 2006. [http://www.coe.int/t/dg3/romatravellers/Default_en.asp] accessed September 18 2009. 3. Babusik F: Legitimacy, statistics and research methodology: who is Romani in Hungary today and what are we (not) allowed to know about Roma. Roma Rights Quarterly 2004; 1: 1418 [www.ceeol.com]. 4. Grund JPC, Öfner PJ, Verbraeck HT: Marel o Del, kas kamel, le Romes duvar (God hits whom he chooses; the Roma gets hit twice). An exploration of drug use and HIV risks among the Roma of Central and Eastern Europe. New York: Open Society Institute; 2007. In Hungarian: Droghasználat is HIV kockázat a romák körében (Drug use and HIV risks among the Roma). Budapest: L’Harmattan 2000. 5. United Nations Development Programme (UNDP): Social assessment of Roma and HIV/AIDS in Central East Europe. UNDP Romania 2003. 6. Fountain J, Bashford J, Winters M, Patel K: Black and minority ethnic communities in England: a review of the literature on drug use and related service provision. London: National Treatment Agency (NTA) 2002. 7. Sangster D, Shiner M, Sheikh N, Patel K: Delivering drug services to Black and minority ethnic communities. DPAS/P16. London: Home Office Drug Prevention and Advisory Service (DPAS) 2002. 8. Broers E, Eland A: Verslaafd, allochtoon en drop-out. Vroegtijdig vertrek van allochtone verslaafden uit de intramurale verslavingszorg. Utrecht: Trimbos-instituut; 2000. 9. Van Wamel A, Eland A: Buiten bereik. Allochtone drugsgebruikers buiten dehulpverlening. Utrecht: Trimbos-instituut; 2001. 10. Fountain J: An overview of the nature and extent of illicit drug use amongst the traveler community: an exploratory study. National Advisory Committee on Drugs (NACD), Dublin: Stationery Office 2006. 11. Rusev A: Harm reduction interventions among Roma drug users in Sofia. Conference presentation 2007, Bratislava 2007. 12. Iraurgi Castillo I, Jiménez-Lermab JM, Landabasoc MA, Arrazolab X, Gutiérrez-Fraile M: Gypsies and drug addictions. European Addiction Research 2000; 6: 34-41. 13. Subata E: Methadone and the gypsy community in Vilnius. Euromethwork 1997; 12: 11-12. 14. European Monitoring Centre for Drugs and Drug Addiction (EMCDDA): Classifications of drug treatment and social reintegration and their availability in EU member states plus Norway. Final Report. Programme 2: monitoring of responses. Luxembourg 2002. 15. Paksi B: A drogfogyasztás populációs prevalenciájának becslése – Az iskolából kimaradók vizsgálata (An estimation of drug use prevalence in the population – a study of drop-outs from school): Kutatási beszámoló (Research Report).Corvinus University, Budapest 2000. 16. Ritter I: A kábítószer megvásárlásához szükséges pénz megszerzésére irányuló bűnözés és a bűnelkövetők jellemzői a fiatalkorúak büntetés-végrehajtási intézetében és a javító intézetekben lévő fogvatartottak körében (Characteristics of criminals and crimes aimed at obtaining the money needed to buy drugs among juveniles incarcerated in penal institutions and correctional facilities). Kutatási beszámoló (Research Report). Országos Kriminológiai Intézet (National Criminological Institute), Budapest 2002. 17. Ritter I: Roma fiatalok és kábítószerek (Roma youths and drugs). Kutatási beszámoló (Research Report). Budapest: Egészséges Ifjúságért Alapítvány – Országos Kriminológiai Intézet (Foundation for Healthy Youth – National Criminological Institute) 2005. 18. Appel PW, Ellison AA, Jansky HK, Oldak R: Barriers to enrollment in drug abuse treatment and suggestions for reducing them: opinions of drug injecting street outreach clients and other system stakeholders. The American Journal of Drug and Alcohol Abuse 2004; 30(1): 129-153. 19. Treloar C, Abelson J, Cao W et al.: Barriers and incentives to treatment for illicit drug users. Monograph Series 2004; 53. 20. Stein MD, Friedmann P: Need for medical and psychosocial services among injection drug users: a comparative study of needle exchange and methadone maintenance. The American Journal on Addictions 2002; 11: 262-270. 21. Rácz J, Máthé-Árvay N, Fehér B: Kezelésre jelentkező és “utcai” injekciós droghasználók kockázati magatartásainak és kockázatészlelésének jellemzői. Előzetes eredmények (Characteristics of high risk behaviors and perception of risk for intravenous drug users on the street and applying for treatment. Preliminary results). Addiktológia (Addictologia Hungarica) 2003; 3-4: 370-388. 22. Márványkövi F, Melles K, Rácz J: A kezelésbe és tűcserébe jutás akadályai problémás droghasználók körében Budapesten (The barriers to participation in treatment and needle exchange programs among problematic drug users in Budapest). Addiktológia 2006; 4: 319-341. 23. Gossop M, Darke S, Griffith P et al.: The Severity of Dependence Scale (SDS): psychometric properties of the SDS in English and Australian samples of heroin, cocaine and amphetamine users. Addiction 1995; 90: 607-614. 24. Magnani R, Sabinb K, Saidela T, Heckathorn D: Review of sampling hard-to-reach and hidden populations for HIV surveillance. AIDS 2005, 19(Suppl 2): S67-S72. 25. Babusik F: Az esélyegyenlőség korlátai Magyarországon (The Limits of Equal Opportunity in Hungary). Budapest: L’Harmattan 2005.
