*Éva Zitás1, Judit Mèszáros2
Prevention possibilities of the most common childhood skin disorders
1PhD student, Doctoral School, Semmelweis University, Budapest, Hungary
Head of Department: Gyula Domján, PhD
2Department of Nursing Faculty of Health Sciences, Semmelweis University, Budapest, Hungary
Head of Faculty: prof. Zoltán Zsolt Nagy, MD, PhD
Summary
Introduction. This paper reviews the basic principles of childhood skin disease treatment and prevention as well as the most common factors affecting recovery and recurrences.
Aim. The symptoms, the frequency of occurrence and the possibilities for prevention of the disorders are examined, while the most important factors affecting recovery are also reviewed.
Material and methods. In this paper we examine the data of 230 children, all treated for skin disease, and all under the age of two. The applied method is the evaluation of answers collected from questionnaires. The questions are related to the skin symptoms (type, time and place of appearance, whether it is a primary symptom or a recurrence, etc.) and also to the circumstances (family anamnesis, housing conditions, diet, skincare practices, materials in direct contact with the skin, clothing, toys, etc.), which could be brought into connection with the skin symptoms.
Results. The results of the examination are shown on charts. Based on the evaluation of the results, it can be concluded that diaper dermatitis (D.D.) and atopic dermatitis (A.D.) are the two most commonly occurring skin diseases among children under the age of two. For the development of A.D., hereditary disposition is required. Both are prone to recurrence, however, the recurrence of D.D. is irrespective of seasons, while the recurrence of A.D. is mainly expected in the heating period. No connection with dietary habits was found.
Conclusions. From the results it can be concluded, that in the recovery process of all the skin diseases, proper skin care plays an important part. In the case of both D.D. and A.D., avoiding all drying effects (bathing frequently in warm soapy water) is highly recommended. Using washing cream, bathing oil, and greasy body milk is advisable. In order to prevent recurrences, it is important to make sure that the degree of humidity in the air is adequate. Sunshine and spending time in the fresh air also prove beneficial. It is favourable to wear clothing which is made of light, soft and natural materials. The condition of the skin is worsened by toys (plasticine) made from materials which cause irritation, as is by playing in the sand. Keeping pets is inadvisable only in case the child also suffers from a chronic respiratory disease (asthma, hay-fever).
INTRODUCTION
In infancy and babyhood there is a very high incidence rate of skin disease. Recovery time and any possible recurrences are dependent upon proper skin care, as well as upon treatment, but it is also influenced by diet, the degree of humidity in the air, and the materials which come into direct contact with the skin (clothing, toys, animals). This paper is going to give a detailed account of the basic principles of skin care and treatment, as well as the possibilities for prevention.
AIM
In our research we examined the ever increasing skin symptoms in children, the frequency of occurrence of the phenomenon as well as the possibilities for prevention.
The objective of the study is to research how the recovery of the health of the skin may be influenced by skin care, dietary habits, the degree of humidity in the air and the materials in direct contact with the skin (clothing, toys, animals).
MATERIAL AND METHODS
The survey was conducted in Budapest in the autumn of 2015, by evaluating the data collected from questionnaire made by ourselves, detected 230 children out of 405 cases. The data appearing in the survey are those of children under the age of 2. The calculation results were set in percentage to the nearest whole number. The questions were divided into nine main categories: 1. skin symptoms, 2. family anamnesis, 3. housing conditions, 4. dietary habits, 5. leisure time, 6. skin care practices, 7. clothing, 8. the material of the toys, 9. keeping pets.
RESULTS
1. Skin symptoms: type; at what age; in which season; in which localization it started; first symptom, or recurrence (fig. 1-6).
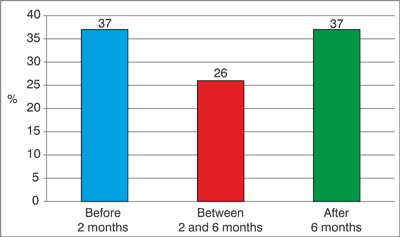
Fig. 1. The time of appearance of the skin symptoms
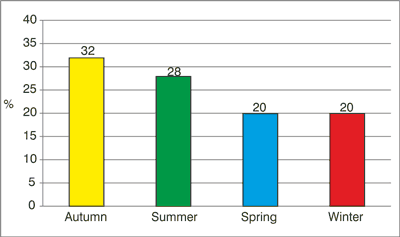
Fig. 2. The season of appearance of the skin symptoms
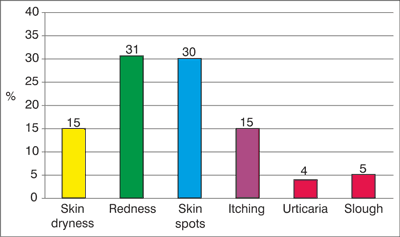
Fig. 3. The type of appearance of the skin symptoms
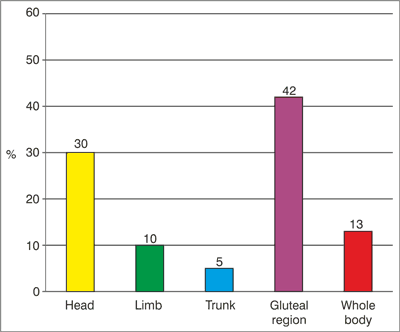
Fig. 4. Localization of the skin symptoms
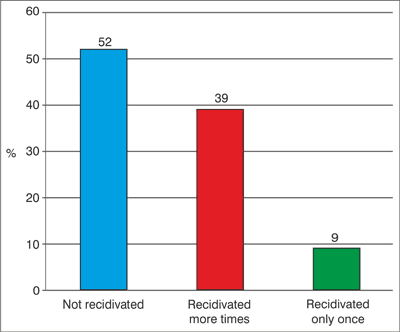
Fig. 5. Frequency of recurrences
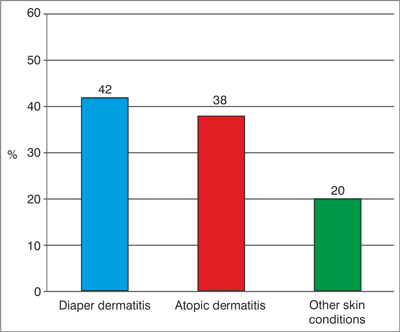
Fig. 6. Diagnosis
2. Family anamnesis: 59% of the family anamnesis proved negative. In the families there was a 24% occurrence of eczema, a 4% occurrence of asthma, and a 13% occurrence of hay-fever.
3. Housing condition: 100% of the families use piped (hard) water. 52% of the families do not use evaporator units. 42% use units to be fitted on the radiators, and 7% use electric devices. 54% of the families use district heating, 41% gas convector and 3-2% use electric and traditional heating.
4. Dietary habits: animal protein (cow’s milk and eggs) was introduced to 9% of the children under the age of 1 year; the majority of the children were given animal protein after the age of 1 or 1 and a half years (fig. 7, 8).
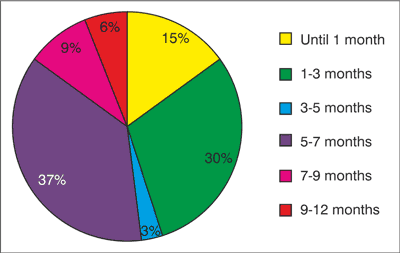
Fig. 7. Distribution of breastfeeding
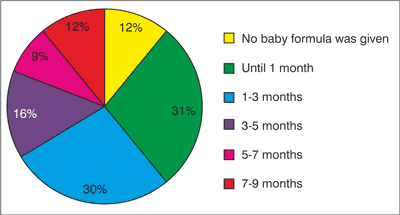
Fig. 8. Distribution of feeding with baby formula
5. Leisure time (time spent in the open air): according to the survey, all the children spend time in the fresh air every day.
6. Skin care practices: the children are generally given a bath every day, bathing time in most cases lasts for 10-15 minutes. Baby care products are used for hair wash and bathing. All the families use disposable nappies.
7. Clothing: in 88% of the cases, underwear was made from cotton, in 12% of the cases, from blended fabric. 78% of the outerwear was made from cotton, 17% from wool, and 5% from blended fabric.
8. Toys: all the children’s furry toys were made from synthetic fibre.
9. Keeping pets: 28% of the families have small mammal pets (hamsters, guinea pigs, cats), 72% of the families have no pets.
DISCUSSION
Based on the data gained from the survey questionnaire, as well as the personal conversations with the children’s parents, it can be proved that 57% of the children, under the age of two, who took part in the study, demonstrated skin symptoms. In the case of infants, the two most common conditions were D.D. and later, A.D.
The occurrence of diaper dermatitis is irrespective of season, while atopic dermatitis produces symptoms in the late autumn, winter and early spring months (72%), when the degree of humidity in the air in the houses is significantly reduced, due to heating. A.D. is a genetically determined condition, with a more frequent occurrence in families with a history of eczema, asthma, and hay-fever (41%). The results of examining dietary habits are shown in figures 7 and 8. As can be seen from the pie chart, 85% of the studied infants were breastfed at least up to the age of 7 months. According to the survey data, all infants spend time regularly in the fresh air.
An important connection is indicated between skin care practices and the course of the skin conditions. The survey data show that skin care products to clean and protect the skin are used regularly in the care of infants and babies. Products with great publicity are given preference, although results depend rather on the method of application than on the make of the used product. In most cases, the skin care products are not applied properly, which results in a significant decrease in effectiveness. Disposable nappies were used with all the studied infants, thus preventing irritation caused by detergent and fabric conditioner residue, resulting in a lower frequency and severity of D.D.
Wearing tight clothes from synthetic fabric increases sweating, and prevents the evaporation of perspiration, and by so doing, slows down the healing process and promotes recurrences. As can be seen from the survey data, the parents are well aware of this fact, and tend to buy clothes which are made from natural materials.
Irritation of the respiratory tract and allergy may be caused by the children’s furry toys, the fur of the pets, the dust and the dust mites the fur gathers, as well as hairs falling out (1). Extreme care must be taken in the case of A.D., especially if the family anamnesis proved positive. All the children’s furry toys were made from synthetic fabric, which washes well.
Families, taking part in the study and having an atopic history, do not keep pets in general.
CONCLUSIONS
The survey data suggest that almost all babies and young children will develop some kind of abnormal skin lesions before the age of two years. Most of these are D.D. and A.D.
The course of the skin conditions, recovery, and any possible recurrences are greatly influenced by skin care. It is of utmost importance therefore to establish proper skin care practices. A.D. is a dry-skin based disorder, therefore all drying effects must be avoided. First in line is bathing the children frequently in warm soapy water. Warm water in itself has degreasing properties, with hard tap water increasing the skin’s proneness to inflammation. It dissolves the lipoprotein layer on the surface of the skin. Dry, scaly and possibly chapped skin is prone to inflammation. The Ca++ ions of the epidermis are bound by soap, resulting in a prevalence of Na+ ions, which will further deteriorate the condition of the skin. Antigens are more easily bound by dry, scaly and inflamed skin, therefore any ingredients that aromatize or colour the soap, as well as any other additives, might cause allergic oversensitivity (2). That is why applying the so called ‘washing-cream’ (ung. Hydrophilicum non-ionicum Fo.No.) is so important, and can be recommended in the case of all skin conditions. When there is proneness to atopy, we should apply this when bathing our children even when they are symptom-free! It is important to note that first the cream has to be spread on the skin (for an easier application, we might wish to prepare a 1:1 solution with water), so as to eliminate irritation by tap water. The cream will cover the dirt on the skin, and makes it washable with water. For bathing purposes, do not use water which is too hot!
The washing cream does not need to be washed off completely, as after a gentle drying, it will be absorbed in the corneum and will make it smooth. Should the child wish to stay in the bath for a longer time, it might be advisable to add some bath oil to the water. After bath, it will be necessary to apply oily body emulsion.
For many types of childhood skin disorders, fresh air and sunshine prove to be beneficial, and can be recommended primarily in the case of A.D. The survey data also demonstrate a much lower rate of recurrences in the summer months. Care must be taken, however, and especially in the case of children with pale skin, blue eyes, or red hair, we should use sunscreen emulsions. In the autumn and winter months, skin dryness is worsened by the low degree of humidity in the air due to heating. It will result in the recurrence of the skin disorders. For prevention purposes, therefore, the use of proper evaporator units is essential.
From the results of the dietary habits survey, no essential conclusions could be drawn, neither is there a uniform attitude on the part of medical professionals in this regard. However, doctors all have a common stand in that infants should be breastfed as long as possible. In 85% of the surveyed cases, babies were breastfed at least up to the age of 7 months.
Due to its unsaturated sebacic acid content, the oil of evening primrose has beneficial effects, if given from early childhood (one teaspoonful a day). It would be essential that all clothing that comes into direct contact with the children’s skin should be made of natural materials, however, parents do not always pay enough attention to this. The material of the toys also plays a part in triggering possible recurrences. Playing with plasticine and playing in the sand frequently cause typical scaling skin symptoms on the hands of children prone to atopy. It is the responsibility of the health visitor to draw attention to this!
Piśmiennictwo
1. Flade S: Az ekcèmás bőr-neurodermatitis-gyógyítása termèszetes úton, Budapest, Új Gondolatok Kiadó 1994. 2. Ricci G, Neri I, Ricci L et al.: Silk fabrics in the management of atopic dermatitis. Skin Therapy Lett 2012; 17: 5-7. 3. Temesvári E: Ekzèmák; in: Bőrgyógyászat ès venerológia (Ed.: Kárpáti S), Medicina Könyvkiadó Zrt, Budapest 2013. 4. Lyons JJ, Milner, JD, Stone KD: Atopic Dermatitis in Children: Clinical Features, Pathophysiology and Treatment. Immunol Allergy Clin North Am 2015; 35: 161-183. 5. Varothai S, Nitayavardhana S, Kulthanan K. Moisturizers for patients with atopic dermatitis. Asian Pac J Allergy Immunol 2013; 31: 91-98. 6. Cseplák Gy: Gyakorlati bőrgyógyászat. Medicina Könyvkiadó Zrt, Budapest 2011. 7. Jakab É: A kozmetika alapjai; in: Kozmetikai kèzikönyv (Ed.: Hajdú, I), Műszaki Könyvkiadó, Budapest 1994. 8. Rajka G: Atopic dermatitis; in: Textbook of Cosmetic Dermatology (Ed.: Baran R), Martin Dunitz Ltd, London 1998. 9. Vestita M, Filoni A, Congedo M, et al.: Vitamin D and Atopic Dermatitis in Childhood. J Immunol Res 2015; 2015: 257879. 10. Lien TY, Goldman RD: Breastfeeding and maternal diet in atopic dermatitis. Can Fam Physician 2011; 57: 1403-1405. 11. Eigenmann PA: Breast-feeding and atopic eczema dermatitis syndrome: protective or harmful? Allergy 2004; 59 Suppl 78: 42-44. 12. Rácz I, Török I, Horváth A: Gyakorlati bőrgyógyászat. Medicina, Budapest 1991.







