Female physicians´ and nurses´ self-rated general and psychosocial health status and health behaviour in Hungary
1Department of Public Health, Faculty of Health Sciences, Semmelweis University, Budapest, Hungary;
Head of Department: Balázs Péter Ph.D.
2Department of Health and Social Care, Széchenyi István University, Györ, Hungary
Summary
Summary
Aim. This study analyses the self-rated general and psychosocial health of female physicians and nurses in Hungary related to healthy lifestyle habits and individual behavioural patterns.
Material and method. cross-sectional data were taken by a questionnaire survey among Hungarian female health care staff members (N=409) selected representatively in 2005 (responding rate 45.5%).
Results. Six out of ten staff members mentioned at least one health problem. Strongly related to self-rated health (SRH) were role conflicts (p<0.001), pessimistic future expectations (p<0.001), perceived difficulties in maintaining the actual partnership (p=0.001), and satisfaction with one´s life and career (p<0.001). About 40% said that they did some sports once a week or even more frequently. Smokers represented 24.4%.
Conclusion. The results obtained suggest that health is not a highly appreciated value among female staff members in Hungarian health care. Moreover, their health-related behaviour is at a substandard level. Improving this situation should be a priority aim of any intervention.
Introduction
Medical and nursing professions are stressful due to a number of major problems: high work-related expectations, complex workplace organization, ethical dilemmas, difficult patients and multiple roles (concerning physicians and nurses as mothers with young children). All these factors may lead to psychic and somatic symptoms as a result of these difficulties [1-8]. Despite recent fundamental political changes (since 1989) there remain many inherited problems in the Hungarian health care system, such as heavy workloads, inadequate workplace conditions, lack of proper tools and equipment, inflexible work schedules, irregular daylight and night shift changing, very low incomes and considerable psychological burden imposed by the nature of the job itself. Hungarian literature suggests high prevalence of mortality and morbidity of female physicians [9], and on the other hand poor health status [8, 11-14], high prevalence of using hazardous substances and low motivation for healthy behaviour [11] of all female staff members.
Aim of the study
To our knowledge, there are only a few studies comparing health determinants and health-related behavioural patterns of female physicians and nurses. Therefore, the aim of this study was to gain an objective evaluation of female physicians´ and nurses´ (1) SRH-status according to their workloads, role conflicts, and life and career satisfaction, (2) psychosocial health, and (3) health-related behaviours.
Material and method
Cross-sectional quantitative surveys were conducted in May 2005 among female physicians and college-educated nurses. 898 female physicians and nurses were invited to participate. They were selected randomly out of six hospitals (five in county capitals and one in Budapest, the capital of the country). Questionnaires were completed on a strictly voluntary and anonymous basis, and were collected and returned by the hospital administration (489 persons refused; response rate 45.54%). Questionnaires included questions about basic demographic and work-related data of respondents, as well as items related to their health status, psychosocial health and health-related behaviour. Work-related data concerned department, position, workload and job satisfaction. SRH was used as a reliable health indicator, since it is widely accepted as a valid source of the actual health status [15, 16]. The scale of psychosomatic symptoms included eight self-reported items (Figure 1). It was used to measure the frequency of these symptoms. Health-related behaviours were mapped by questions about smoking, alcohol and coffee consumption, use of tranquilizers, sleeping pills, painkillers and narcotic drugs, physical activity, dietary habits, and average sleep duration. Statistical analyses were conducted by the program package SPSS 13.0. In addition to distribution tests, Pearson´s chi-squared test was applied to measure bivariate relationships between categorical variables. Odds ratios (OR) and 95% confidence intervals (CI) were also displayed.
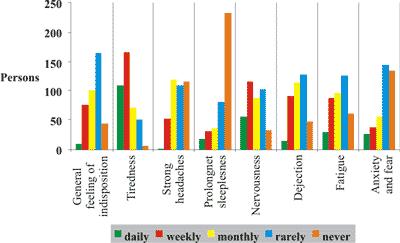
Fig. 1. Prevalence of psychosomatic symptoms (N=404)
Results
The respondents´ average age was 39.7 years (SD=10.8). Average age of female college-educated nurses was lower than that of female physicians (p<0.001). The majority of respondents were married (58.3%), an additional 19.6% were living with a partner, 28.7% were unmarried, and 13.0% were divorced or widowed.
There was no statistical evidence of a correlation between respondents´ type of job and their SRH status (p=0.725). 62.9% of college-educated nurses and 67.6% of physicians gave a positive ("excellent” or "good”) SRH evaluation. Negative evaluation ("bad” or "very bad”) was given only by 4.2% of the entire sample. Within this proportion, nurses outnumbered physicians. On the other hand, there was no correlation with the respondents´ position and type of hospital department. Despite our expectations, SRH status was not influenced by the number of on-duty shifts worked, the number of overtime hours or activity in secondary employment.
Nevertheless, SHR was clearly related to age (p<0.001), frequency of psychosomatic symptoms (p=0.000–0.027), and the quantity of recreational physical activity they did (p=0.004). Respondents with a rather negative SRH indicated more likely conflicts between their work and family roles (p<0.001), negative future expectations (p<0.001), problems with their partners (p=0.001), and less satisfaction with their lives (p<0.001) and their professional careers (p=0.013).
Despite a rather positive SRH, 62.1% of the sample indicated at least one health problem. The source of concern was more or less exactly determined in 54.5%, as (1) frequent headaches, (2) general locomotion disorders, (3) spinal complaints, and (4) being overweight.
Among the eight psychosomatic symptoms (Figure 1) tiredness was most frequently mentioned. Different types of jobs had no statistically relevant impact on the prevalence of psychosomatic symptoms. Since the average age of college-educated female nurses was significantly lower than that of physicians, their age-related prevalence must be assumed to be relatively worse then that of physicians.
Respondents sleep 6 ˝ hours on average on weekdays, and almost 8 hours on free weekends, 15.2% woke up without having had a good rest, and only 12.5% indicated that they always felt relaxed after sleep. More than half of respondents had only 6 hours of sleep or even less on weekdays, and more than 80% slept less than 8 hours even at weekends. There was no difference between the two professional groups in time span of sleep, but they differed in quality of sleep (p=0.002). Fewer college-educated nurses than physicians indicated that "waking up I feel almost always relaxed”, and "I never wake up with the feeling of having had a good rest”.
Based on the results in Table 1, female physicians less frequently access general health screening tests and gynaecological screening than nurses; yet physicians are more protected against hazardous habits and they take holidays more frequently in a year. Figure 2 shows the data of physical activity with very small (less than 20%) regular participation in recreational events. Nearly 70% of college-educated nurses do not do any sports at all. There is a clear correlation between the type of profession and frequency of doing physical activity (p=0.024).
Table 1. Correlations between health-related behaviours and types of profession (N=409)
| | Yes (%) | Correlation with profession | Odds ratio of nurses compared to physicians |
| CN | P |
| Goes to annual gynaecological screening test | 76.5 | 62.7 | p=0.002 | OR: 1.908
95%CI:1.237-2.942 |
| Goes to annual general health screening test | 59.5 | 45.4 | p=0.004 | OR: 1.936
95%CI:1.234-3.036 |
| Abstains from health-damaging habits | 73.5 | 86.1 | p=0.001 | OR: 0.530
95%CI:0.297-0.944 |
| Eats healthy food | 63.5 | 74.1 | p=0.020 | - |
| Takes several holiday trips a year for recreation | 21.0 | 47.9 | p<0.001 | OR: 0.277
95%CI:0.169-0.455 |
| Has breakfast regularly | 53.5 | 58.4 | p=0.321 | - |
| Has several light meals a day | 53.5 | 61.8 | p=0.092 | - |
| Goes to the dentist on an annual basis | 61.5 | 68.4 | p=0.142 | - |
CN = college-educated nurses, P = physicians
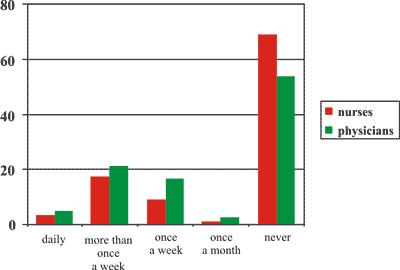
Fig. 2. Frequency of doing sports, by type of profession (%) (N=409)
Table 2, broken down by types of profession, overviews the frequency of using hazardous substances. Differences are statistically significant for smoking (p=0.035), coffee consumption (p=0.004) and alcohol consumption (p<0.001).
Table 2. Use of substances detrimental to health, by type of profession (%) (N=403)
| | Daily user | Several times a week | Several times a month | Once a month | Does not use them |
| CN | P | CN | P | CN | P | CN | P | CN | P |
| Tranquilizers | 2.5 | 0 | 3.0 | 3.0 | 2.5 | 2.5 | 5.0 | 9.4 | 86.8 | 85.15 |
| Sleeping pills | 0.5 | 0 | 0.5 | 0.5 | 0.5 | 2.0 | 2.5 | 1.5 | 96.0 | 96.0 |
| Smoking | 22.2 | 11.3 | 3.5 | 3.9 | 0 | 0 | 2.5 | 2.5 | 71.7 | 82.2 |
| Coffee | 59.6 | 72.7 | 5.0 | 8.3 | 3.5 | 1.5 | 1.5 | 2.0 | 30.3 | 15.6 |
| Alcohol | 0 | 0 | 5.0 | 3.2 | 19.4 | 13.1 | 33.3 | 29.7 | 42.3 | 53.9 |
| Painkillers | 0 | 0 | 6.2 | 5.5 | 17.5 | 19.5 | 36.6 | 31.0 | 39.7 | 44.0 |
| Narcotic drugs | 0.5 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 99.5 | 100 |
CN = college-educated nurses, P = physicians
Discussion
Comparing our results with relevant Hungarian data taken from a survey carried out in 15 European countries in 2003, it can be concluded that respondents of the present survey indicated a better overall health status [17]. Previous SRH surveys used samples out of the entire population above 15 and 18 years respectively. With growing age, the higher people´s education level, the higher are the odds of giving a positive SRH evaluation [17]. Based on this tendency, college-educated female nurses, being younger, would indicate a poorer health status than physicians. As a consequence, some psychosomatic symptoms in the present study (linked strongly with SRH) should have been mentioned more frequently by the nurses. Therefore it is necessary that subsequent surveys specifically address this problem and explain background causes of these differences. It was alarming that neither of the professional groups had a relaxing sleep. Despite older age, female physicians less frequently accessed general medical and gynaecological screenings, which may partly be traced back to self-examinations, although we did not survey this particular issue. Physical activity levels proved to be quite poor, even though it has been demonstrated by many researchers in the past few decades that there is a close correlation between levels of physical activity and health status, as well as rates of morbidity and mortality [18, 19].
Among various risk behaviours we examined, the most frequent were coffee consumption and smoking. Papers published on these issues determined the prevalence of smoking nurses at between 17.7% and 46.0% [20]. Compared to the relevant international and Hungarian surveys this study indicated lower incidence of smoking for the entire sample. Nevertheless, the proportion of smoking nurses exactly mirrored that in the entire Hungarian female population above the age of 18.
Conclusions
1. According to international and Hungarian studies, the present SRH values of hospital-based female physicians and college-educated female nurses are clearly below the optimum levels.
2. Respondents – despite their specialized medical knowledge and their gender-based roles – demonstrated inadequate health behaviour, which is an obvious disadvantage when proposing a healthy lifestyle to patients and to their own families.
3. Especially college-educated female nurses are at a disadvantage in respect of health-related issues; therefore they must be provided with a very intensive health development strategy soon in the near future.
Piśmiennictwo
1. Stewart DE, et al.: Women physicians and stress. J. Womens Health Gend Based Med. 2000; 9: 185-189. 2.McGrath A, et al.: Occupational stress in nursing. Int. J. Nurs. Stud., 2003; 40: 555-565. 3.Firth-Cozens J: Doctors, their well-being, and their stress. BMJ, 2003; 326: 670-671. 4.Demir A, et al.: Investigation of factors influencing burnout levels in the professional and private lives of nurses. Int. J. Nurs. Stud., 2003; 40: 807-827. 5.Heiligers PJM, Hingstman L: Career preferences and the work-family balance in medicine: gender differences among medical specialists. Soc. Sci. Med., 2000; 50: 1235-1246. 6.Artazcoz L, et al.: Gender inequalities in health among workers: the relation with family demands. J. Epidemiol. Community Health 2001; 55: 639-647. 7.Pikó B: Work-related stress among nurses: challenge for health care institutions. The J. R. Soc. Health 1999; 119: 156-162. 8.Pikó B: Burnout, role conflict, job satisfaction and psychosocial health among Hungarian health care staff. Int. J. Nurs. Stud., 2006; 43: 311-318. 9.Molnár L, Mezey M: Az orvosok megbetegedéséről és halandóságáról. LAM 1991; 8-11: 524-528, 640-644, 966-970. 10. Molnár R, Feith H: Szerepkonfliktusok megnyilvánulásai orvosnők körében. LAM 2000; 10: 810-815. 11.Pikó B: A nővéri munka magatartástudományi vizsgálata. Pszichoszomatikus tünetek, munkahelyi stressz, társas támogatás. LAM 2001; 11: 318-325. 12.Győrffy Zs, Ádám Sz: Az egészségi állapot, a munkastressz és a kiégés alakulása az orvosi hivatásban. Szociológia Szemle 2004; 3: 107-127. 13.Hegedűs K, et al.: A súlyos betegekkel foglalkozó egészségügyi dolgozók testi és lelkiállapota. LAM 2004; 14: 786-793. 14. Győrffy Zs, et al.: A magyarországi orvostársadalom egészségi állapota - országos reprezentatív minta alapján. Orv. Hetil., 2005; (26): 1383-1391. 15.Idler E, Benyamini: Self-rated health and mortality: A review of twenty-seven community studies. J. of Health and Social Behaviour 1997; 38: 21-37. 16.Benjamins MR, et al.: Self-reported health and adult mortality risk: An analysis of cause-specific mortality. Soc. Sci. Med., 2004; 59: 1297-1306. 17.Knesebeck O, et al.: Education and health in 22 European countries. Soc. Sci. Med., 2006; 63: 1344-1351. 18.Blair SN, McCloy CH Research lecture: Physical activity, psychical fitness and health. Res. Q. Exerc. Sport., 1993; 64: 365-376. 19.Nowak M: Factors determining physical fitness, self-evaluation and health self-evaluation in physically active women. New Medicine 2006; 9: 19-25. 20.Rowe, Macleod Clark J: The incidence of smoking amongst nurses: a review of the literature. J. Adv. Nurs., 2000; 31: 1046-1053.

