© Borgis - New Medicine 1/2011, s. 19-21
*Ewa Ogłodek, Aleksander Araszkiewicz
Stress as a mechanism of intermediary function in the onset of illness
Department of Clinical Psychiatry of the Nicolaus Copernicus University in Toruń, Collegium Medicum in Bydgoszcz
Head of Department: Aleksander Araszkiewicz
Summary
Living in the social milieu is a constant exposure to psycho-social stimuli, influencing an individual, and making it difficult to meet its substantial needs. It results from the differences between the requirements of the milieu and the abilities of a given individual to meet them. The force of impact of psycho-social factors depends on their significance for the person and the intensiveness and duration of stimuli. With substantial intensiveness and duration of the influence of stimuli, disturbing mechanisms (physiological, emotional and behavioral) may occur. It contributes to the manifestation of symptoms of an illness – the faulty physiological and psychological functioning of an individual. Prolonged prodromal symptoms turn, as time passes, into the illness picture - inefficiency and/or limiting individual’s functioning due to psychosomatic disorders. Frequent experience of stress as well as activation of physiological mechanisms of the organism’s reaction to stress, facilitates development of medical problems. There exists no unambiguous answer to the question, what determines which organs will be subject to the impact of distress.
Stress resulting from the pace of life, lack of stable family life or work qualities may increase the risk of cardiovascular diseases. The main representative of this group of medical problems is the ischemic heart disease, called coronary disease. In spite of a downward trend in mortality, number of its victims still makes it one of the major causes of death in Poland. The disease affects arteries, transporting blood to the cardiac muscle. It has, most frequently, three stages: angina pectoris, heart attack and sudden coronary death (1, 2, 3). Shemesh E et al. emphasize in their research an important connection between stress and cardiovascular diseases. They point out that a psycho-social stimuli increase the activity of the neuro-vegetative system, which results in elevated blood pressure and heart rate, ventricular fibrillation and lowered perfusion of heart muscle (4). Prolonged stress exacerbates the above-mentioned symptoms, accelerating the process of formation of an atherosclerotic plate and degenerative changes of the blood vessels of the cardiac muscle. In her research, Alonzo AA found out that frequent experience of stress in the working environment is a factor, increasing the risk of developing cardiovascular diseases (5). Banou E et al. showed that both daily duties, experienced life events and traumatic situations, contribute to the development of an illness (6). Many researchers emphasize that stress also contributes to the development of exacerbation of already started disease. Research conducted by Morrill EF et al. showed that traumas and traumatic experiences from childhood may constitute risk factors for coronary disease in adult life (7). In turn, another researcher, emphasizes that individuals more susceptible to heart diseases are those who have experienced a traumatic event/trauma, but choose not to talk about that and avoid expressing relevant emotions. Dobkin PL points up that having experienced a traumatic event may contribute to the increase in mortality of victims due to cardiovascular diseases (8).
Psycho-physiological Sternbach model emphasizes the importance of prolonged stress for a given organ. It finally results in the dysfunction and pathology of those organs. Sternbach psycho-physiological model draws our attention to three main predisposing elements, i.e.: response stereotypy (individual’s tendency to display similar patterns of psycho-physiological reacting to many different stress stimuli), frequent activation of psycho-physiological stress reaction and failure of homeostatic mechanisms (9, 10, 11).
The figure 1 shows that biological and environmental factors determine the risk factors in the aetiopathogenesis of diseases. As far as biological factors are concerned, one may refer to widely-studied ischemic heart disease, in case of which medicine differentiates the following known risk factors: elevated cholesterol level, arterial hypertension and insufficient physical activity. In turn, „contributing personality” in terms of illnesses development was popularized in the form of personality patterns: A, C and D (12, 13).
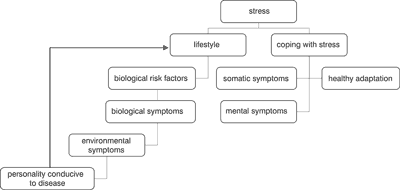
Fig 1. Model of the risk factor interaction and processes of intermediary function for health.
Neoplasm diseases constitute the cause of the second largest number of deaths in Poland. Unfortunately, in recent years, the gradual increase of deaths caused by them has been observed (14, 15). The results of studies on the connection between stress and neoplasm diseases are ambiguous (16, 17). Most of these studies are of a cross-sectional character, which makes it impossible to determine the cause-and-effect relationship. Research conducted by Mehnert A, Koch U shows that stress has an influence on the growth of neoplastic cells depending on the type of neoplasm (18). Stress accelerated the development of a neoplasm, caused by a virus, whilst a neoplasm of a non-viral origin developed comparatively slower under the influence of stress. It should be added that an important role in the progression of neoplastic diseases is that of the immunity system, which participates in searching and destroying neoplasm cells. Stress has an important influence on the functioning of the immunity system, as it has an immunosuppressive effect, i.e. stops the ability of the immunity system to destroy neoplasm cells, making an individual more vulnerable to disease expansion. In his research on stress, Banerjee B et al. proved that the increase in cortisol and noradrenaline (stress hormones) in human organism results in lowering the activity of T and B cells, which are responsible for combating antigens (19). In turn, research of Pervanidou P, Chrousos GP proved that the risk of development of a neoplatic disease increases with the number of events in an individual’s life (20). Locke and his colleagues proved that stress contributes to a significant reduction of reactivity of the cytotoxic cells. Particularly low activity of these cells is observed in individuals, experiencing strong stress, being unable to cope with it effectively. Researchers point out depression, feeling of helplessness and hopelessness as mental states presenting the immunosuppressive impact. These states emerge particularly as a result of traumatic event. FitzGerald LZ et al. confirmed that in the organism of such an individual due to decrease in the level of catecholamines, and increase of endorphins level, blockage of pain perception (similarly to morphine) is ensured this way (21). Weakened cytotoxic cells may turn out to be too weak in order to destroy disease cells, in case of the onset of a disease. Studies by von Känel R et al. confirmed that people with high depression index died of cancer twice as frequently in comparison to people with lower indexes (22).
Experienced stress may also be related to the occurrence and intensification of skin problems, as it is subject to the influences of the vegetative and the internal-excretion systems. Common skins problems related to stress include, among others, eczemas, acne, hives, prurigo, leucoderma, psoriasis, atopic dermatitis, alopecia areata, lichen planus, excessive sweating and reoccurring herpes. Research of Ivanovski K et al. indicate that individuals experiencing stress and strong emotions are more susceptible to skin problems (23).
Research show that individuals with atopic dermatitis are excessively fearful. They are emotionally unstable and have visible problems with coping with stress. They most frequently display their emotions by excessive scratching their own body. In other epidemiologic studies, it was observed that psoriasis occurred in 1,5% participants, 37% of whom indicated stress as the cause of the exacerbation of the disease (24, 25).
In an individual’s lifestyle, risk factors are most clearly noticeable if they are related to the form of behavior, habits and routines, which are conditioned by the social-cultural and personality-related factors. It should, however, be emphasized that it is not stress that is the main cause of developing illnesses, but the way a human being copes with it.
Piśmiennictwo
1. Higgins RO et al.: Emotional and adjustment issues faced by cardiac patients seen in clinical practice: a qualitative survey of experienced clinicians. J Cardiopulm Rehabil Prev 2007; 27(5): 291-297. 2. Dao TK et al.: Clinical depression, posttraumatic stress disorder, and comorbid depression and posttraumatic stress disorder as risk factors for in-hospital mortality after coronary artery bypass grafting surgery. J Thorac Cardiovasc Surg 2010; 140(3): 606-610. 3. Tapernoux D et al.: Myocardial infarction during attempted suicide. Dtsch Med Wochenschr 2009; 134(8): 339-342. 4. Shemesh E et al.: Posttraumatic stress, nonadherence, and adverse outcome in survivors of a myocardial infarction. Psychosom Med 2004; 66(4): 521-526. 5. Alonzo AA: Acute myocardial infarction and posttraumatic stress disorder: the consequences of cumulative adversity. J Cardiovasc Nurs 1999; 13(3): 33-45. 6. Banou E, Hobfoll SE, Trochelman RD: Loss of resources as mediators between interpersonal trauma and traumatic and depressive symptoms among women with cancer. J Health Psychol 2009; 14(2): 200-214. 7. Morrill EF et al.: The interaction of post-traumatic growth and post-traumatic stress symptoms in predicting depressive symptoms and quality of life. Psycho-oncology. 2008; 17(9): 948-953. 8. Dobkin PL: Mindfulness-based stress reduction: what processes are at work? Complement Ther Clin Pract 2008; 14(1): 8-16. 9. Oh SH et al.: Association of stress with symptoms of atopic dermatitis. Acta Derm Venereol 2010; 90(6): 582-528. 10. Reich A, Hrehorów E, Szepietowski JC: Pruritus is an important factor negatively influencing the well-being of psoriatic patients.Acta Derm Venereol 2010; 90(3): 257-263. 11. Biljan D et al.: Psoriasis, mental disorders and stress.Coll Antropol 2009; 33(3): 889-892. 12. Boehncke WH, Buerger C, Boehncke S: Co-morbidities in psoriasis vulgaris. Hautarzt 2009; 60(2): 116-121. 13. Willemsen R, Roseeuw D, Vanderlinden J: Alexithymia and dermatology: the state of the art. Int J Dermatol 2008; 47(9): 903-10. 14. Shah B, Ashok L, Sujatha GP: Evaluation of salivary cortisol and psychological factors in patients with oral lichen planus. Indian J Dent Res 2009; 20(3): 288-292. 15. Thornton LM, Andersen BL, Blakely WP: The pain, depression, and fatigue symptom cluster in advanced breast cancer: covariation with the hypothalamic-pituitary-adrenal axis and the sympathetic nervous system.Health Psychol 2010; 29(3): 333-337. 16. Pokupec JS, Gruden V, Gruden V Jr: Lichen ruber planus as a psychiatric problem. Psychiatr Danub 2009; 21(4): 514-516. 17. Banerjee B et al.: Effects of an integrated yoga program in modulating psychological stress and radiation-induced genotoxic stress in breast cancer patients undergoing radiotherapy. Integr Cancer Ther 2007; 6(3): 242-250. 18. Mehnert A, Koch U: Prevalence of acute and post-traumatic stress disorder and comorbid mental disorders in breast cancer patients during primary cancer care: a prospective study. Psychooncology 2007; 16(3): 181-188. 19. Banerjee B et al.: Effects of an integrated yoga program in modulating psychological stress and radiation-induced genotoxic stress in breast cancer patients undergoing radiotherapy. Integr Cancer Ther 2007; 6(3): 242-250. 20. Pervanidou P, Chrousos GP: Neuroendocrinology of post-traumatic stress disorder. Prog Brain Res. 2010; 182: 149-60. 21. FitzGerald LZ, Kehoe P, Sinha K: Hypothalamic-pituitary-adrenal axis dysregulation in women with irritable bowel syndrome in response to acute physical stress. West J Nurs Res 2009; 31(7): 818-836. 22. von Känel R et al.: Stress hormones in patients with posttraumatic stress disorder caused by myocardial infarction and role of comorbid depression. J Affect Disord 2010; 121(1-2): 73-79. 23. Ivanovski K et al.: Psychological profile in oral lichen planus. J Clin Periodontol. 2005; 32(10): 1034-1040. 24. Field T, Diego M: Cortisol: the culprit prenatal stress variable. Int J Neurosci 2008; 118(8): 1181. 25. Thornton LM, Andersen BL, Carson WE 3rd: Immune, endocrine, and behavioral precursors to breast cancer recurrence: a case-control analysis. Cancer Immunol Immunother 2008; 57(10): 1471-1481.
