© Borgis - New Medicine 1/2011, s. 17-18
*Ewa Ogłodek
Dermatitis Artefacta as a Spectrum of Borderline Personality Disorder – case report
Department of Clinical Psychiatry, Nicolaus Copernicus University Toruń, Medical University Bydgoszcz, Poland
Head of Department: prof. Aleksander Araszkiewicz, MD, PhD
Summary
Dermatitis artefacta refers to conditions in which patient self-inflicts excoriations with their own nails, sharp instruments, burning cigarettes or chemicals. There are instances in which recognition of this disorder is difficult. Histological findings are not characteristic and diagnosis depends on the clinical presentation. The differential diagnosis of cutaneous lesions is extensive, depending on the lesion type. Diagnosis of dermatitis arteficialis was based on clinical grounds, including bizarre-looking lesions, sites accessible to the patients and absence of other dermatologic diseases to explain the dermatosis. Knowledge of the psycho-dermatological diseases can contribute to more profitable therapy in both dermatology and psychiatry.
Dermatitis artefacta means self-inflicted lesions of the skin. Various psychosocial conflicts and unconscious motivating factors have been held responsible for this self-destructive activity (1). Dermatitis artefacta may represent one of Borderline Personality Disorders (BPD). Borderline personality disorder is a serious mental illness characterized by pervasive instability in moods, interpersonal relationships, self-image, and deregulated behaviors, such as non-suicidal self-injury and binge-eating (2). The development and exacerbation of Borderline Personality Disorders spectrum are associated with deregulation of the hypothalamic pituitary adrenal (HPA) axis, which is measured by aberrant levels of cortisol secretion (3). These symptoms are related to dysfunction of fronto-limbic circuits. Among subcortical limbic structures, the amygdala mediates the most extensive range of social and emotional processes (4). Patients suffering from BPD exhibit exaggerated amygdala responses to social and emotional stimuli. Biological basis of BPD has focused primarily on the relationships between dysfunctional behaviors and serotonin (5-HT) deregulation (5).
Emotional problems as the cause of skin lesions have been described in specialist literature over the last few years (6). Various types and methods of producing the skin lesions depend on the patient’s background and education. Clinical manifestation of self-inflicted dermatitis may be difficult to diagnose (7). Histological findings are not characteristic and diagnosis depends on the clinical presentation. Differential diagnosis of cutaneous lesions is extensive, depending on the lesion type. Below there is presented a case of dermatitis artefacta in a man who was diagnosed with a Borderline Personality Disorders (8).
Case Report
A 46-year-old male patient, single, with an 8-month history of the skin lesions was referred to the dermatology clinic by his family doctor. In clinical examination, numerous erosions, excoriations, post-inflammatory discolorations with straight edges were observed. The lesions were located on the patient’s hands and legs (fig. 1). A skin biopsy did not reveal any features characteristic for inflammation, but only supported the clinical diagnosis of erosion. The general examination did not reveal any other abnormalities: histopathologic study of biopsy taken from the lesion revealed fibroconnective tissue with loss of epithelial lining, sparse inflammatory cell infiltration, and capillary proliferation with no evidence of malignancy. These clinical features are typically observed in dermatitis artefacta. The results of bacteriological culture examination of the skin erosions showed the presence of Acinetobacter. The patient hasn’t been treated psychiatrically so far. While the patient was staying in the dermatological hospital, a follow-up visit to the psychiatrist was arranged, which confirmed the diagnosis of BPD with depression syndrome. Subsequently, systemic treatment with psychotropic drugs (100 mg of sertraline daily, 300 mg of lamotrigine per day) was introduced. Systemic treatment with antibiotics and antihistamines as well as topical treatment with mild steroids and emollients were also administered. After ten days of treatment, there was considerable improvement of the patient’s skin lesions and mental health. Currently, the patient is under psychiatric and dermatological care.
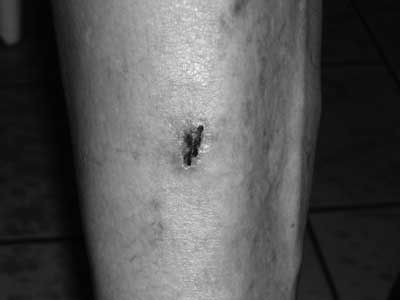
Fig. 1. Dermatitis Artefacta.
The clinical presentation of self-inflicted dermatitis varies widely in morphology and distribution, and may be difficult to recognize. Individual lesions are often bizarre, with irregular rectilinear outlines and geographical patterning not conforming to any spontaneous pathological process (9). In the presented case the cutaneous lesions accompanied BPD, which is characterized by affective instability, anger, and impulsivity. This study indicates that variety of models of anxiety and depression as well as their intensity are connected with changes in neuronal number and morphological complexity of neurons (10). These changes can be expected to have effect on both measures of the gross structure and the function of particular brain regions in adults who suffer from anxiety and depression. This study showed that dermatitis artefacta is a factitious disorder and may represent depression symptoms.
Piśmiennictwo
1. Gregurek-Novak T, Novak-Bilić G, Vucić M:. Dermatitis artefacta: unusual appearance in an older woman. J Eur Acad Dermatol Venereol. 2005; 19(2): 223-225. 2. Ebner-Priemer UW et al.: Emotional learning during dissociative states in borderline personality disorder. J Psychiatry Neurosci 2009; 34(3): 214-222. 3. Harth W, Mayer K, Linse R: The borderline syndrome in psychosomatic dermatology. Overview and case report. J Eur Acad Dermatol Venereol 2004; 18(4): 503-507. 4. Herpertz SC et al.: Emotional responses in patients with borderline as compared with avoidant personality disorder. J Pers Disord 2000; 14(4): 339-351. 5. Sansone RA et al.: Disability and borderline personality symptoms. Psychosomatics. 2003; 44(5): 442. 6. Gattu S, Rashid RM, Khachemoune A: Self-induced skin lesions: a review of dermatitis artefacta. Cutis. 2009, 84(5): 247-251. 7. Harman M, Akdeniz S, Bayram Y: Dermatitis artefacta. J Eur Acad Dermatol Venereol 2001; 15(4): 368-370. 8. Kwon EJ et al.: Dermatitis artefacta. J Cutan Med Surg 2006; 10(2): 108-113. 9. Koblenzer CS: Dermatitis artefacta. Clinical features and approaches to treatment. Am J Clin Dermatol 2000; 1(1): 47-55. 10. Minzenberg MJ et al.: Frontolimbic structural changes in borderline personality disorder. J Psychiatr Res 2008; 42(9): 727-733.
