© Borgis - New Medicine 4/2012, s. 125-128
*Agnieszka Ledniowska1, Grzegorz Ledniowski2, Jarosław Karoń1, Przemysław Karoń1
Implantation of the gynecare prolift system in lower pelvic organ prolapse correction in patients with co-occurring urological disorders
1Gynaecology-Maternity Ward, ZOZ Kędzierzyn-Koźle Public Hospital, Poland
Supervisor: Jarosław Karoń, MD
2Urology Ward, ZOZ Kędzierzyn-Koźle Public Hospital, Poland
Supervisor: Andrzej Trondowski
Summary
Aim. Assessment of the impact of correction of pelvic organ prolapse on co-occurring urological disorders in patients operated on with the use of the TVM Prolift system.
Material and methods. The TVM Prolift system was implanted in 22 patients with co-occurring pelvic organ prolapse in POPQ stages from II to IV and urological disorders such as: stress urinary incontinence, mixed urinary incontinence, overactive bladder, pollakiuria and difficulties with starting urination.
Results. In all of the patients, the surgery restored the correct anatomical conditions of the lower pelvic organs. In 77.3% of the patients operated on, the urological problems subsided or abated, in 4.5% of the patients the symptoms intensified and in 18.2% of the patients the symptoms in question remained unchanged.
Conclusions. It is justified to implant the TVM Prolift system in patients with co-occurring pelvic organ prolapse and urological disorders, because after the restoration of proper stability of lower pelvic organs the urological disorders subsided or abated in 77.3% of the patients operated on.
INTRODUCTION
Pelvic organ prolapse (POP) is defined as the descent of lower pelvic organs, which leads to the lowering of the vaginal walls and/or uterus. The final stage of this process is the prolapse of the genital organ. The condition in question can be seen while supine; it usually worsens with the increase of intra-abdominal pressure. This defect often intensifies with consecutive births and the woman’s age (1, 2). According to different authors, the incidence of pelvis organ descent in the female population between 20 and 70 is about 14%. In nulliparous women, POP occurs in 2-4% of the population in multiparous women the incidence of such disorders reaches 76% (3, 4). It is believed that the cause of POP occurrence is the weakening of the pelvic floor muscles, inadequate quality of the connective tissue and failure of the musculo-fibrous apparatus of lower pelvic organs (5).
POP patients often also suffer from urological disorders resulting from abnormal anatomical conditions in the pelvic floor area (6). In order to determine patients in whom genital organ prolapse co-occurs with urological disorders, before any corrective surgeries are conducted, apart from the case history, physical examination and ultrasonographic examination, urodynamic testing needs to be performed.
A number of various POP corrective surgery methods have been developed. It is estimated that the lifetime risk of a surgery due to POP is 7-14% (7). One of the methods of restoration of proper anatomical conditions of lower pelvic organs is vaginal implantation of synthetic meshes (Gynecare Prolift) which take over the role of a deficient suspensory system of lower pelvic organs. The application of synthetic materials significantly improves subsequent results of surgery, thus considerably increasing the comfort of patients’ lives (7). Implantation of the TVM Prolift system enables simultaneous improvement of anatomical conditions of lower pelvic organs as well as resolution of urological disorders in a large number of patients (8).
AIM
The evaluation of the results of surgery with the application of the Gynecare Prolift system in instances of urological disorders.
MATERIAL AND METHODS
The Gynecare Prolift system was implemented in 22 patients between 33 and 77 in whom pelvic organ prolapse had co-occurred with urological disorders. The patients were operated on at the Kędzierzyn-Koźle ZOZ Public Hospital between October of 2006 and December of 2008.
In the patients, pelvic organ prolapse disorders in stages from II to IV, according to POP-Q classification, co-occurred with urological disorders in the form of: stress urinary incontinence in10 patients, mixed urinary incontinence in 7 patients, in 2 patients overactive bladder was diagnosed, in 2 pollakiuria occurred, 1 patient reported problems with starting urination.
All of the patients were called in for check-ups consisting of physical examination and urodynamic testing. They also filled out anonymous questionnaires, subjectively evaluating their disorders. The patients answered the questions:
1. Did the surgery conducted affect preoperative urological disorders? (a. yes; b. no).
2. If the surgery did affect the disorders, what was the result? (a. resolution of the preoperative symptoms; b. reduction of the preoperative symptoms; c. intensification of the preoperative symptoms).
RESULTS
The application of the TVM Prolift system restored normal anatomical conditions of the genital tract in all of the patients.
Among 22 patients reporting urological problems prior to the surgery, the operation caused:
1. In 15 patients (68.2% of the population) resolution of the symptoms.
2. In 2 patients (9.1% of the population) reduction of the symptoms.
3. In 4 patients (18.2% of the population) the symptoms remained unchanged.
4. In 1 patient (4.5% of the population) the symptoms intensified.
After analysing the population with respect to urological disorders, it was found:
A. In the group of patients with stress urinary incontinence (10 patients):
1. The surgery did not affect urinary continence: 3 patients (30%).
2. The surgery caused intensification of the symptoms: 1 patient (10%).
3. The surgery caused reduction of the symptoms: 2 patients (20%).
4. The surgery caused resolution of the symptoms: 4 patients (40%).
B. In the group of patients with mixed urinary incontinence (7 patients):
1. The surgery did not affect urinary continence: 1 patient (14.3%).
2. The surgery caused resolution of the symptoms: 6 patients (85.7%).
C. In the group of patients with an overactive bladder (2 patients):
a. The surgery caused resolution of the symptoms: 2 patients (100%).
D. In the remaining patients (3 patients) :
a. Pollakiuria (2 patients) – in all of the patients the symptoms subsided – 100% treatment.
b. Difficulties with starting urination (1 patient) – the problems subsided – 100% treatment.
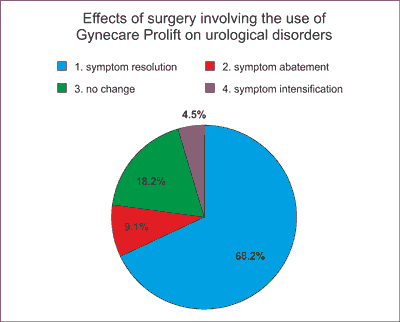
Fig. 1. The diagram below shows the effects of surgery involving the use of Gynecare Prolift on urological disorders. In 68.2% of the patients the symptoms subsided, in 9.1% they abated, in 18.2% they remained unchanged, in 4.5% of the patients the symptoms intensified.
DISCUSSION
The commonly occurring in women problem of pelvic organ prolapse has led to the development of multiple methods of treatment (9). Some patients are treated non-surgically with pelvis floor muscle exercises or with various vaginal inserts, so-called pessars (10-12). However, most patients undergo different kinds of corrective surgeries (13). There was discussed the role of surgery access (vaginal, abdominal, laparoscopic), various reducing surgeries were tested and involved the excision of excess vaginal mucosa with or without removal of the genital tract, attempts were made at using the patient’s own tissues or foreign biological materials. None of the surgeries described in the literature met all expectations. The high percentage of relapses of disorders after surgery forced doctors to modify operating techniques. Only the application of synthetic materials in the correction of pelvic organ prolapse brought a breakthrough. In light of the latest findings, the application of monofilament, macroporous, propylene meshes seems justified.
Doctors dealing with pelvic organ prolapse issues are often met with the problem of co-occurrence of urinary continence disorders. The spectrum of these disorders is broad, they often co-occur. No singular treatment strategy in such cases has been determined. Our practice and the findings of other authors suggest that correction of existing pelvic organ prolapse often leads to spontaneous resolution of urological disorders (14). However, this view is not without opponents, who in their papers argue for the need of simultaneous surgical treatment of POP and urological disorders, e.g., with suburethral slings (15). In our practice, we have assumed that POP correction alone is a sufficient procedure in the majority of patients. We based this proceeding on the observation that only a small number of patients would require supplementary treatment after properly conducted POP correction.
In the available literature there is little information on the influence of implantation of the Gynecare Prolift system on the resolution of urological disorders. Our observations suggest that properly conducted POP surgery causes resolution of urological disorders in 68% of patients and in 9% of patients it significantly reduces these disorders.
It seems unjustified to perform an implantation of the Gynecare Prolift system with the simultaneous implantation of a suburethral sling.
Analysing the studied population, we found that in the group of patients with stress urinary incontinence POP correction leads to resolution or reduction of the disorder in 60% of patients.
Similar conclusions were reached by Sergent F et al. (16) while investigating a group of 106 patients in which stress urinary incontinence co-occurred with pelvic organ prolapse. The authors observed that, after prolapse correction with polypropylene mesh, in 72 patients (69%) stress urinary incontinence symptoms had subsided, in 13 patients (12%) the disorders had abated.
Shek KL et al. used Gynecare Prolift meshes in a group of 24 patients in whom POP co-occurred with stress urinary incontinence. In 21 patients (87.5%), stress urinary incontinence symptoms subsided or abated, in 2 patients (8.3%) they remained at the same stage, in 1 patient (4.3%) the symptoms intensified (17).
There is no information in the literature on the application of meshes in POP correction in patients with mixed urinary incontinence. Our research shows that in 85.7% patients operated on symptoms subside and in the rest of cases surgery has no effect on the disorders in question.
De Boer TA et al. (18) performed surgeries using Gynecare Prolift in 505 patients in whom POP co-occurred with OAB. They observed that in 94% of the patients operated on OAB symptoms had abated, in 6% of the patients they had intensified. Similar conclusions were published by Long CY et al. They performed repair surgeries in 80 patients in whom POP co-occurred with OAB. In 78.8% of the patients operated on, resolution of problems related to OAB was observed, in 21.2% of the patients operated on the problems remained unchanged or intensified (19). Similar conclusions were reached by Ek M et al. (20).
Our research shows that pelvic organ prolapse correction with the use of the Gynecare Prolift system leads to the resolution of OAB symptoms and pollakiuria in all patients operated on.
CONCLUSIONS
The application of the Gynecare Prolift system as a singular therapeutic procedure during primary surgery in patients in whom POP co-occurs with urological disorders seems a valid approach, as such procedure leads to successful treatment of the majority of patients.
Piśmiennictwo
1. Sola V, Pardo J, Ricci P et al.: Tension free monofilament macroporous polypropylene mesh (Gynemesh PS) in female genital prolapse repair. Int Braz J Urol 2006; 32(4): 410-415. 2. Rechberger T, Miotła P, Futyma K et al.: Risk factors of pelvic organ prolapse in women qualified to reconstructive surgery-in Polish multicenter study. Ginekol Pol 2010; 81(11). 3. Swift SE, Tate SB, Nicholas J: Correlation of symptoms with degree of pelvic organ support in a general population of women: what is pelvic organ prolapse? Am J Obstet Gynecol 2003; 189(2): 372-377. 4. Tunn R, Petri E: Introital and transvaginal ultrasound as the main tool in the assessment of urogenital and pelvic floor dysfunction: an imaging panel and practical approach. Ultrasound Obstet Gynecol 2003; 22(2): 205-213. 5. DeLancey JO: Anatomy and biomechanics of genital prolapsed. Clin Obstet Gynecol 1993; 36(4): 897-909. 6. Aukee P, Usenius JP, Kirkinen P: An evaluation of pelvic floor anatomy and function by MRI. Eur J Obstet Gynecol Reprod Biol 2004; 112(1): 84-88. 7. Surkont G, Wlaźlak E, Suzin J: Operacyjne leczenie zaburzeń statyki narządu płciowego u kobiet – gdzie jesteśmy, dokąd zmierzamy, Przegląd Urologiczny 2006; 7/4(38). 8. Sergent F, Sentilhes L, Resch B et al.: Treatment of concomitant prolapse and stress urinary incontinence via a transobturator subvesical mesh without independent suburethral tape. Acta Obstet Gynecol Scand 2010; 89(2): 223-229. 9. Bader G, Fauconnier A, Buyot B et al.: Use of prosthetic materials in reconstructive pelvic floor surgery. An evidence-based analysis. Gynecol Obst Fertil 2006; 34(4): 292-297. 10. South M, Amundsen CL: Pelvic organ prolapse: a review of the current literature. Minerva Ginecol 2007; 59(6): 601-612. 11. Br?kken IH, Majida M, Engh ME, Bø K: Can pelvic floor muscle training reverse pelvic organ prolapse and reduce prolapse symptoms? An assessor-blinded, randomized, controlled trial. Am J Obstet Gynecol 2010; 203(2): 170.e1-7. 12. Hagen S, Stark D, Glazener C et al.: A randomized controlled trial of pelvic floor muscle training for stages I and II pelvic organ prolapse. Int Urogynecol J Pelvic Floor Dysfunct 2009; 20(1): 45-51. 13. Patel M, Mellen C, O’Sullivan DM et al.: Impact of pessary use on prolapse symptoms, quality of life, and body image. Am J Obstet Gynecol 2010; 202(5): 499.e1-4. 14. Maher C, Feiner B, Baessler K et al.: Surgical management of pelvic organ prolapse in women. Cochrane Database Syst Rev 2010; 14, 4: CD004014. 15. 15. Yuan Z, Dai Y, Cen Y: Clinical study on concomitant surgery for stress urinary incontinence and pelvic organ prolapsed. Zhonghua Wai Ke Za Hi 2008; 46(20): 1533-1535. 16. Sergent F, Sentilhes L, Resch B et al.: Treatment of concomitant prolapse and stress urinary incontinence via a transobturator subvesical mesh without independent suburethral tape. Acta Obstet Gynecol Scand 2010; 89(2): 223-229. 17. Shek KL, Rane A, Goh J et al.: Stress urinary incontinence after transobturator mesh for cystocele repair. Int Urogynecol J Pelvic Floor Dysfunct 2009; 20(4): 421-425. 18. De Boer TA, Kluivers KB, Withagen MI et al.: Predictive factors for overactive bladder symptoms after pelvic organ prolapse surgery. Int Urogynecol J Pelvic Floor Dysfunct 2010; 21(9): 1143-1149. 19. Long CY, Hsu CS, Wu MP et al.: Predictors of improved overactive bladder symptoms after transvaginal mesh repair for the treatment of pelvic organ prolapse: Predictors of Improved OAB after POP Repair. Int Urogynecol J 2010; 22(5): 535-642. 20. Ek M, Altman D, Falconer C et al.: Effects of anterior trocar guided transvaginal mesh surgery on lower urinary tract symptoms. Neurourol Urodyn 2010; 29(8): 1419-1423.
