© Borgis - Nowa Pediatria 4/2014, s. 141-144
*Łukasz Szarpak1, Andrzej Kurowski2, Katarzyna Karczewska3, Togay Evrin4, Tomasz J. Merta5
Porównanie skuteczności trzech metod intubacji dzieci podczas resuscytacji – badanie pilotażowe
Comparison of the efficacy of three methods of child intubation during resuscitation – pilot study
1Department of Cardiosurgery and Transplantology, Institute of Cardiology, Warszawa, Poland
Head of Department: Mariusz Kuśmierczyk, PhD, MD
2Department of Anesthesiology, Institute of Cardiology, Warszawa, Poland
Head of Department: Ewa Sitkowska-Rysiak, PhD, MD
3Anesthesiology and Intensive Care Unit, Mazovian Regional Hospital, Radom, Poland
Head of Department: Krzysztof Sys, MD
4Emergency Department, Darica Farabi Public Hospital, Darica, Turkey
Head of Department: Togay Evrin, PhD, MD
5New York University Shanghai, Shanghai, China
Head of Department: Yu Lizong, PhD
Summary
Introduction. Securing the airway is one of the basic skills that paramedics should have. Obstruction of the airways is a major cause of cardiac arrest among children. Adequate airway management, oxygenation and ventilation are important goals of paediatric cardiopulmonary resuscitation.
Aim. The aim of this study is to compare the effectiveness of a paediatric patient intubation during simulated cardiopulmonary resuscitation performed by paramedic students.
Material and methods. Three intubation devices were compared in a simulated scenario of resuscitation: Miller Laryngoscope, GlideScope and ILMA. A group of 45 student paramedics intubated a pediatric manikin with uninterrupted chest compressions.
Results. The mean intubation time performed with these devices was 37.55 ± 12.84 s, 45.63 ± 21.63 s, 35.51 ± 5.87 s. The overall efficacy of intubation was 86.65% for Miller, 95.54% for GlideScope, and 91.12% for ILMA, respectively. Participants reported the ILMA to be easier to use in intubation method during chest compression scenario.
Conclusions. Video laryngoscopy and blind intubation using ILMA are a good alternative for the Miller laryngoscope for intubation during resuscitation without interruption of chest compressions.

Introduction
Adequate airway management is one of the main activities undertaken during emergency events. This procedure is all the more important in case of cardiac arrest in a child. Hypoxia arising from airway obstruction is a major cause of cardiac arrest in the paediatric population. It should be remembered that the patient’s oxygen reserves in the normothermia with cardiac arrest are sufficient only for 3-5 minutes (1). The most recommended method for airway management in both children and adults according to the guidelines of the European Resuscitation Council, as well as the American Heart Association, is endotracheal intubation (ETI) (2, 3). Securing the airway using an endotracheal tube carries many benefits. First, the placement of an ETI can accomplish stable ventilation support without additional pauses in chest compressions during CPR. Secondly, it is possible to use a positive end-expiratory pressure (PEEP) and to measure the concentration of carbon dioxide in exhaled air. However, using the laryngoscope with Miller blade (MIL) for tracheal intubation is sometimes a difficult skill even for medical emergency professionals, and securing the airway becomes even more difficult in an emergent situation (4). Through the development of medicine and the introduction of new patency devices, intubation is now possible with the use of electronic visualization or intubation blindly.
Aim
The aim of the study was to compare time and success rates of different intubation devices for the emergency intubation during resuscitation with chest compression in a standardized paediatric manikin model performed by student paramedics.
Material and methods
The study was approved by the Programme Council of the International Institute of Rescue Research and Education (Warsaw, Poland; Decision no. 2014/17). The study was conducted in May 2014. Forty-five paramedics (16 female and 29 male, age 31 ± 10) participated in this study. Participants were selected at random from among the students of medical universities in Masovian voivodeship. Participation in the study was voluntary. None of participants had previously used GlideScope or ILMA.
Prior to the trial, all participants were given a standard training session of two 45-min lectures on the anatomy of the airway and tracheal intubation with the laryngoscope with Miller blade no. 2 (Mercury Medical; Clearwater, FL, USA), GlideScope (Verathon, Bothell, WA, USA) and ILMA (Teleflex, Buckinghamshire, Great Britain). At the end of the training, instructors demonstrated the correct technique of intubation using a laryngoscope Miller, GlideScope and ILMA. After this part of the study, participants involved in the study practiced, under the supervision of instructors, endotracheal intubation using the above listed methods of intubation until they were comfortable with the devices. All intubations were performed using a Magill tracheal tube with 5.0 mm internal diameter (ID).
Intubation was performed on a training phantom MegaCode Kid (Laerdal, Norway). In order to standardize the difficulties associated with intubation during chest compression, a Lucas 2 device was used (Physio-Control, USA). During intubation attempts, only the person performing the intubation and instructors were present in the room – other people did not have the opportunity to observe the process of intubation.
A Research Randomizer program was used (www.randomizer.com) to divide the volunteers into 3 groups and to determine the order in which to apply the different ETI devices within each group. The first groups attempted ETI using the Miller, the second using the GlideScope and the third using the ILMA as a conduct for endotracheal tube. The detailed procedure of randomization is presented in figure 1. After completing the ETI procedure participants had a 15 minute break before performing another emergency procedure.
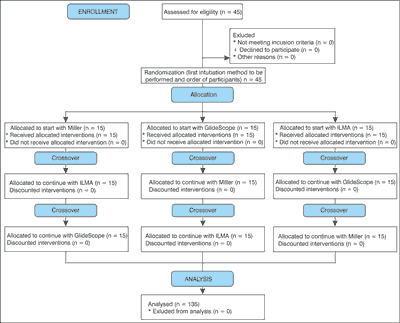
Fig. 1. Flow chart of design and recruitment of participants according to CONSORT statement.
The primary endpoint of the study was the success rate of intubation. The secondary endpoint was defined as the time from insertion of the blade between the teeth to the first manual ventilation of the mannequin’s lungs. If the examinee failed at all attempts, the case was excluded from the time calculations. Finally, students were asked to rate the ease of intubation using each device using a Likert scale from 1 (extremely easy) to 5 (extremely difficult). Quantitative data are presented as mean and standard deviation or percentage.
Powyżej zamieściliśmy fragment artykułu, do którego możesz uzyskać pełny dostęp.
Mam kod dostępu
- Aby uzyskać płatny dostęp do pełnej treści powyższego artykułu albo wszystkich artykułów (w zależności od wybranej opcji), należy wprowadzić kod.
- Wprowadzając kod, akceptują Państwo treść Regulaminu oraz potwierdzają zapoznanie się z nim.
- Aby kupić kod proszę skorzystać z jednej z poniższych opcji.
Opcja #1
29 zł
Wybieram
- dostęp do tego artykułu
- dostęp na 7 dni
uzyskany kod musi być wprowadzony na stronie artykułu, do którego został wykupiony
Opcja #2
69 zł
Wybieram
- dostęp do tego i pozostałych ponad 7000 artykułów
- dostęp na 30 dni
- najpopularniejsza opcja
Opcja #3
129 zł
Wybieram
- dostęp do tego i pozostałych ponad 7000 artykułów
- dostęp na 90 dni
- oszczędzasz 78 zł
Piśmiennictwo
1. Gerritse BM, Schalkwijk A, Pelzer BJ et al.: Advanced medical life support procedures in vitally compromised children by a helicopter emergency medical service. BMC Emerg Med 2010; 10: 6. doi: 10.1186/1471-227X-10-6. 2. Deakin CD, Nolan JP, Soar J et al.: European Resuscitation Council Guidelines for Resuscitation 2010 Section 4. Adult advanced life support. Resuscitation 2010 Oct; 81(10): 1305-1352. doi: 10.1016/j.resuscitation.2010.08.017. 3. McCall MJ, Reeves M, Skinner M et al.: Paramedic tracheal intubation using the intubating laryngeal mask airway. Prehosp Emerg Care 2008; 12(1): 30-34. 4. Gerritse BM, Draaisma JM, Schalkwijk A et al.: Should EMS-paramedics perform paediatric tracheal intubation in the field? Resuscitation 2008; 79(2): 225-229. doi: 10.1016/j.resuscitation.2008.05.016. 5. Timmermann A, Russo SG, Crozier TA et al.: Laryngoscopic versus intubating LMA guided tracheal intubation by novice users – a manikin study. Resuscitation 2007; 73(3): 412-416. 6. Badia M, Montserrat N, Serviá L et al.: Severe complications of orotracheal intubation in the Intensive Care Unit: An observational study and analysis of risk factors. Med Intensiva 2014 Mar 4 (Epub ahead of print). 7. Sakles JC, Mosier JM, Chiu S, Keim SM: Tracheal intubation in the emergency department: a comparison of GlideScope® video laryngoscopy to direct laryngoscopy in 822 intubations. J Emerg Med 2012 Apr; 42(4): 400-405. doi: 10.1016/j.jemermed.2011.05.019. 8. Mosier JM, Stolz U, Chiu S, Sakles JC: Difficult airway management in the emergency department: GlideScope videolaryngoscopy compared to direct laryngoscopy. J Emerg Med 2012 Jun; 42(6): 629-634. doi: 10.1016/j.jemermed.2011.06.007. 9. Tung A, Griesdale DE: Comparing the novel GlideScope Groove videolaryngoscope with conventional videolaryngoscopy: a randomized mannequin study of novice providers. J Clin Anesth 2013 Dec; 25(8): 644-650. doi: 10.1016/j.jclinane.2013.07.005. 10. Rodríguez-Núñez A, Moure-González J, Rodríguez-Blanco S et al.: Tracheal intubation of pediatric manikins during ongoing chest compressions. Does Glidescope® videolaryngoscope improve pediatric residents’ performance? Eur J Pediatr 2014 Oct; 173(10): 1387-1390. doi: 10.1007/s00431-014-2329-z. 11. Moreira A, Koele-Schmidt L, Leland M et al.: Neonatal intubation with direct laryngoscopy vs videolaryngoscopy: an extremely premature baboon model. Paediatr Anaesth 2014 Jun 10. doi: 10.1111/pan.12435 (Epub ahead of print). 12. Melissopoulou T, Stroumpoulis K, Sampanis MA et al.: Comparison of blind intubation through the I-gel and ILMA Fastrach by nurses during cardiopulmonary resuscitation: a manikin study. Heart Lung 2014 Mar-Apr; 43(2): 112-116. doi: 10.1016/j.hrtlng.2013.12.004. 13. Shah VR, Bhosale GP, Mehta T, Parikh GPL: A comparison of conventional endotracheal tube with silicone wire-reinforced tracheal tube for intubation through intubating laryngeal mask airway. Saudi J Anaesth 2014 Apr; 8(2): 183-187. doi: 10.4103/1658-354X.130702. 14. Rabiner JE, Auerbach M, Avner JR et al.: Comparison of GlideScope Videolaryngoscopy to Direct Laryngoscopy for Intubation of a Pediatric Simulator by Novice Physicians. Emerg Med Int 2013; 2013: 407547. doi: 10.1155/2013/407547.

