*Dorota Olczak-Kowalczyk1, Grażyna Marczuk-Kolada2, Lidia Postek-Stefańska3, Barbara Bartosiak-Drosio1, Renata Filipińska4, Dariusz Gozdowski5, Elżbieta Łuczaj-Cepowicz2, Paulina Modzelewska-Chiniewicz1, Małgorzata Daszkowska4, Anna Jurczak6, Joanna Szczepańska4
Avulsion of permanent teeth in children – a retrospective analysis of the causes, management strategy and treatment outcomes
Całkowite zwichnięcia zębów stałych u dzieci – analiza retrospektywna przyczyn, metod postępowania i wyników leczenia
1Department of Paediatric Dentistry, Medical University of Warsaw
Head of Department: Professor Dorota Olczak-Kowalczyk, MD, PhD
2Department of Paediatric Dentistry, Medical University of Białystok
Head of Department: Grażyna Marczuk-Kolada, MD, PhD
3Department of Developmental Age Dentistry, Medical University of Silesia in Katowice
Head of Department: Lidia Postek-Stefańska, MD, PhD
4Department of Paediatric Dentistry, Medical University of Łódź
Head of Department: Professor Joanna Szczepańska, MD, PhD
5Department of Experimental Design and Bioinformatics, Department of Agriculture and Biology, Warsaw University of Life Sciences
Head of Department: Professor Wiesław Mądry, PhD
6Department of Paediatric Dentistry, Institute of Dentistry, Jagiellonian University Medical College
Head of Department: Anna Jurczak, MD, PhD
Streszczenie
Wstęp. Całkowite zwichnięcie zęba powoduje jednoczesne uszkodzenie wielu tkanek – dziąsła, więzadła przyzębnego, miazgi, kości wyrostka zębodołowego, cementu i zębiny korzenia. Właściwe postępowanie po urazie zęba, już w miejscu wypadku, istotnie wpływa na pomyślność rokowania.
Cel pracy. Celem pracy było określenie związku płci i wieku pacjentów z miejscem i przyczyną zwichnięcia całkowitego zęba, rodzaju powikłań po replantacji zębów i czynników wpływających na ich występowanie.
Materiał i metody. Przeprowadzono analizę retrospektywną całkowicie zwichniętych 102 zębów stałych u 67 pacjentów. W grupie pacjentów po wykonanej replantacji odnotowywano informacje na temat: wieku, płci, czasu i przyczyny urazu, liczby zębów dotkniętych urazem, stadium rozwoju korzenia (dojrzały/niedojrzały), żywotności zębów, stanu tkanek okołokorzeniowych, czasu przebywania zęba poza jamą, medium, w jakim był przechowywany ząb, czasu, jaki upłynął od momentu wybicia zęba do replantacji, rodzaju i czasu szynowania oraz procesu gojenia.
Wyniki. Najczęściej wybiciu ulegały przyśrodkowe zęby sieczne szczęki. Do urazu zwykle dochodziło na ulicy lub podwórku, a większość urazów związana była z aktywnością sportową. Nie replantowano 10% zębów. Czas, jaki upłynął od urazu do udzielenia pierwszej pomocy, wahał się od 2 minut do 4 dni. Zęby przechowywano najczęściej na sucho. Obserwowano niewłaściwy sposób lub zbyt długie unieruchamiania związane z nieterminowym zgłaszaniem się pacjentów. Najczęściej obserwowanym powikłaniem była ankyloza. Ryzyko powikłań zmniejszały: brak współistniejących uszkodzeń pourazowych, replantacja < 60 minut od urazu, przechowywanie zęba w ślinie, prawidłowy sposób unieruchamiania oraz antybiotykoterapia.
Wnioski. Nieudzielenie pomocy na miejscu wypadku, niewłaściwe przechowywanie zęba całkowicie zwichniętego, błędy postępowania lekarskiego i niezgłaszanie się pacjentów na wyznaczone wizyty będące przyczynami powikłań gojenia wskazują na konieczność powszechnej edukacji dotyczącej postępowania w przypadku całkowitego zwichnięcia zęba.
Summary
Introduction. Avulsion of the tooth results in a simultaneous damage of many tissues – gingiva, periodontal ligament, pulp, alveolar bone, cement and dentin of the root. Proper management after tooth injury, already at the site of the accident, has a significant impact on successful prognosis.
Aim. The aim of the study was to determine the relationship between patient gender/age and the place/cause of tooth avulsion, the type of complications after tooth replantation as well as factors influencing their occurrence.
Material and methods. A retrospective analysis of 102 avulsed permanent teeth was performed in 67 patients. The following data was recorded in the group of patients after replantation: age, gender, time and cause of the injury, number of affected teeth, the stage of root maturation (mature/immature), vitality of the affected teeth, condition of supporting tissues, extra-oral time of avulsed teeth, storage media, time elapsed between injury and replantation, type and duration of splinting, and the healing process.
Results. Maxillary central incisors were most frequently avulsed. Dental trauma usually occurred in the street or courtyard, and most of the injuries were associated with sports activities. A total of 10% of teeth were not replanted. The time elapsed between the injury and first-aid ranged from 2 minutes to 4 days. Most teeth were stored dry. Improper or prolonged splinting due to untimely reporting on dental visits was observed. Ankylosis was the most common complication. The risk of complications was reduced due to: the lack of concomitant traumatic lesions, replantation < 60 minutes post-injury, tooth storage in saliva, correct splinting and antibiotic therapy.
Conclusions. Lack of first-aid at the accident site, improper storage of the avulsed tooth, medical errors and patients’ missing scheduled visits, all of which cause healing complications, indicate the need for public education on the management in tooth avulsion.

Introduction
A sudden tooth injury causing dental avulsion results in a simultaneous damage of many tissues – gingiva, periodontal ligament (PDL), pulp, alveolar bone, cement and dentin of the root. Children aged 7-9 years are at increased risk of injury-related dental avulsion due to immature periodontal fibres and reduced resistance of periodontal ligament (PDL) to extrusion.
Avulsion of permanent teeth is one of the most serious dental injuries. Proper management after tooth injury, already at the scene of the accident, has a significant influence on successful prognosis. Although replantation is a treatment of choice in most cases, it may be impossible immediately after the injury (1-3).
There are a number of factors affecting the periodontal healing process in replanted teeth. Complications most often occur due to the lack of properly performed first-aid at the site of accident, patient’s reporting to the dentist a few hours after the accident and the use of inappropriate storage medium to ensure periodontal cell viability. Furthermore, despite appropriate treatment, pathological resorption (replacement, inflammatory) often occurs in these teeth, leading to progressive tooth mobility and loss (1, 4). First-aid procedures depend on the circumstances of the injury (site, cause), the age and general condition of the child with avulsed tooth and, most of all, the knowledge and skills of accident witnesses.
Aim
The aim of the study was to determine the relationship between patient gender/age and the place/cause of tooth avulsion, the type of complications after tooth replantation as well as factors influencing their occurrence.
Material and methods
A retrospective analysis of medical records from 67 patients with avulsion of at least one permanent tooth, presenting at paediatric dentistry clinics of four medical universities between 2006 and 2015, was performed. Patients who did not report for a follow-up visit after receiving first medical aid were excluded from the study. Qualification criteria were as follows: replantation and at least 2 months of follow-up.
Data on gender and age at injury, the cause and place of injury, the type and the number of avulsed teeth, the time elapsed between the injury and replantation, tooth storage conditions, person performing replantation, the methods of medical management and complications was obtained from medical records.
The obtained results were analysed statistically using Chi-square test and Kendall’s tau correlation. Statistica 12 and SPSS 22 were used for statistical analysis; a p-value of 0.05 was accepted as statistically significant.
Results
Dental avulsion of 102 teeth occurred in 67 patients (mean 1.48 ± 1.04). Replantation was not performed in 10 avulsed teeth in 6 patients, including 2 teeth lost in a traffic accident (first medical aid was provided in the department of surgery), 6 teeth that were not found and 2 teeth due to unknown reasons. Injuries occurred at the age between 5.2 and 17.9 years, with a mean age of 10.29 ± 3.28 years (41.3% of patients aged between 5.2 and 10 years). Tooth avulsion was statistically significantly more common in girls and at a younger age compared to boys (9.29 years vs. 11.77 years; p = 0.005).
For the remaining 61 patients (21 girls and 40 boys), a total of 92 teeth were replanted (between 1 and 7 teeth in one patient; mean 1.43 ± 1.04; 1 tooth in 73.8%). Avulsion was more common in maxillary (79) rather than mandibular teeth (13). These were mostly maxillary central incisors (60), followed by maxillary lateral incisors (15), mandibular central incisors (7) mandibular lateral incisors (5), maxillary canines (3), mandibular canines (1), and the first maxillary premolar (1) (fig. 1).
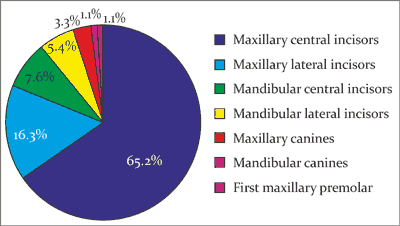
Fig. 1. Types of avulsed teeth
Place and cause of injury
The place of injury remains unknown in 5 patients, and the cause of injury is unclear in 8 patients. Injuries most often occurred in the street or courtyard, less frequently at home, school or swimming pool (tab. 1). Most injuries (n = 20) were related to sports activities (32.2%), including cycling, team sports (e.g. colliding with another player during a football match, teeth stuck in a volleyball net), swimming pool activities (e.g. hitting with the teeth against the pipe or the knee) or other (e.g. a fall from the trampoline). A total of 8.19% of patients lost their teeth as a result of a fight (peer conflicts), while 3.27% due to a traffic accident. In one case, the dentist removed the wrong tooth.
Tab. 1. Place and cause of dental injury
| Injury circumstances | Patients |
| n/% |
| Place | street/courtyard | 26/34.3 |
| school | 14/22.95 |
| home | 12/19.6 |
| swimming pool | 3/4.91 |
| other | 1/1.63 |
| unknown | 5/8.19 |
| Cause | fall | 14/22.95 |
| hitting an object | 9/14.75 |
| bicycle | 11/18.03 |
| team sports | 5/8.19 |
| fight | 5/8.19 |
| other sport-related | 4/6.55 |
| collision with another person | 2/3.27 |
| traffic accident | 2/3.27 |
| other | 1/1.64 |
| unknown | 8/13.11 |
The analysis of Kendall rank correlation showed a significant relationship between age and injuries occurring at school and cycling-related injuries as well as gender and falls from a bicycle. The incidence of school accidents increased with age (correlation coefficient 0.192, p < 0.05). Bicycle accidents were significantly more common in girls (correlation coefficient 0.199, p < 0.05) and younger children (-0.182, p < 0.05).
The time of first medical aid and the storage of avulsed teeth
Medical records of 2 patients (3.27%) lacked data on the time elapsed between injury and first aid in relation to 3 avulsed teeth (3.26%). For the remaining 59 patients, the time of replantation of 89 teeth ranged from 2 minutes to 4 days (mean 6.39 ± 13.92 hours). One tooth was replanted after 4 days; the remaining 88 teeth were replanted within 48 hrs, an average of 5.13 ± 7.19 hours. A total of 22 teeth (22.82%) were replanted within 60 minutes of injury, including 2 teeth replanted immediately after avulsion and 67 teeth replanted more than 60 minutes (tab. 2) after the injury. Uncompleted root development was reported in 21 teeth.
Tab. 2. Time elapsed between the injury and the replantation of teeth with formed/unformed apices
| The time from injury to replantation | Number of teeth | Total | The time from injury to replantation |
| open apex | closed apex | mean ± SD |
| after < 60 minutes of injury | 7 | 15 | 22 | 43.90 ± 19.71 minutes |
| after > 60 minutes of injury | 14 | 53 | 67 | 7.97 ± 13.37 hrs |
| no data | 0 | 3 | 3 | – |
| total | 21 | 71 | 92 | 6.39 ± 13.92 hrs |
Powyżej zamieściliśmy fragment artykułu, do którego możesz uzyskać pełny dostęp.
Mam kod dostępu
- Aby uzyskać płatny dostęp do pełnej treści powyższego artykułu albo wszystkich artykułów (w zależności od wybranej opcji), należy wprowadzić kod.
- Wprowadzając kod, akceptują Państwo treść Regulaminu oraz potwierdzają zapoznanie się z nim.
- Aby kupić kod proszę skorzystać z jednej z poniższych opcji.
Opcja #1
29 zł
Wybieram
- dostęp do tego artykułu
- dostęp na 7 dni
uzyskany kod musi być wprowadzony na stronie artykułu, do którego został wykupiony
Opcja #2
69 zł
Wybieram
- dostęp do tego i pozostałych ponad 7000 artykułów
- dostęp na 30 dni
- najpopularniejsza opcja
Opcja #3
129 zł
Wybieram
- dostęp do tego i pozostałych ponad 7000 artykułów
- dostęp na 90 dni
- oszczędzasz 78 zł
Piśmiennictwo
1. Andersson L, Andreasen JO, Day P et al.: International Association of Dental Traumatology guidelines for the management of traumatic dental injuries: 2. Avulsion of permanent teeth. Dent Traumatol 2012; 28: 88-96. 2. Andreasen JO, Lauridsen E, Andreasen RM: Contradictions in the treatment of traumatic dental injuries and ways to proceed in dental trauma research. Dent Traumatol 2010; 26: 16-22. 3. Andreasen JO, Andreasen FM, Bakland LK, Flores MT: Pourazowe uszkodzenia zębów. Elsevier Urban & Partner, Wrocław 2012. 4. Flores MT, Andersson L, Andreasen JO et al.: Guidelines for the management of traumatic dental injuries. II. Avulsion of permanent teeth. Dent Traumatol 2007; 23: 130-136. 5. Karayilmaz H, Kirzioglu Z, Gungor OE: Aetiology, treatment patterns and long-term outcomes of tooth avulsion in children and adolescents. Pak J Med Sci 2013; 29(2): 464-468. 6. Tzigkounakis V, Merglova V, Hecová H, Netolický J: Retrospective clinical study of 90 avulsed permanent teeth in 58 children. Dent Traumatol 2008; 24(6): 598-602. 7. Soares Ade J, Gomes BP, Zaia AA et al.: Relationship between clinical-radiographic evaluation and outcome of teeth replantation. Dent Traumatol 2008; 24: 183-188. 8. Andreasen JO, Borum MK, Jacobsen HL, Andreasen FM: Replantation of 400 avulsed permanent incisors: 2. Factors related to pulpal healing. Endod Dent Traumatol 1995; 11(2): 59-68. 9. Fortuniak A, Szczepańska J: Późna replantacja zęba siecznego stałego – opis przypadku. Poradnik Stom 2008; 3: 69-72. 10. Petrovic B, Marković D, Peric T, Blagojevic D: Factors related to the treatment and outcomes of avulsed teeth. Dent Traumatol 2010; 26: 52-59. 11. Kinoshita S, Kojima R, Taguchi Y, Noda T: Tooth replantation after traumatic avulsion: a report of 10 cases. Dent Traumatol 2002; 18: 153-156. 12. Andreasen JO, Lauridsen E, Gerds TA, Ahrensburg SS: Dental Trauma Guide: a source of evidence-based treatment guidelines for dental trauma. Dent Traumatol 2012; 28(2): 142-147. 13. Guideline on Management of Acute Dental Trauma. Council on Clinical Affairs 2011. 14. Tolentino LS, Tolentino ES, Dias-Ribeiro E et al.: Avulsed permanent incisor-Replantation after two days of the trauma: Report of a case. Revista de odontologia da UNICID 2010; 22: 70-77. 15. Prociów A, Wójcicka-Rubin A, Żęcin A: Urazy zębów u dzieci – stan świadomości nauczycieli szkół podstawowych w Łodzi. Czas Stomatol 2006; LIX(4): 257-265. 16. Guidelines for the Management of Traumatic Dental Injuries. International Association of Dental Traumatology 2007. 17. Jurczak A, Kołodziej I, Kościelniak D et al.: Resorpcja zewnętrzna zamienna korzenia zęba jako późne powikłanie pourazowe u pacjentów w wieku rozwojowym. Implantoprotetyka 2009; X, 4(37): 41-43.

