*Przemysław Ciesielski1, 2, Agnieszka Kucharczyk1, Paweł Dutkiewicz2
The place of alternative treatment methods for haemorrhoidal disease in the modern therapeutic algorithm
Miejsce alternatywnych metod leczenia choroby hemoroidalnej we współczesnym algorytmie terapeutycznym
1Warsaw Proctology Centre, Saint Elizabeth’s Hospital, Mokotów Medical Centre
Head of Centre: Associate Professor Małgorzata Kołodziejczak, PhD
2Department of General Surgery, County Hospital in Wołomin
Head of Department: Krzysztof Górnicki, MD, PhD
Streszczenie
Według szacunkowych danych dolegliwości związane z chorobą hemoroidalną dotyczą ponad połowy populacji po 50. roku życia. Do głównych objawów choroby hemoroidalnej należą: krwawienia, wypadanie hemoroidów, dyskomfort, pieczenie i swędzenie oraz uczucie niepełnego wypróżnienia. Różnorodne nasilenie objawów zależne jest od wielu czynników. Celem leczenia choroby hemoroidalnej jest przede wszystkim ograniczenie dolegliwości, co można uzyskać leczeniem zachowawczym, zabiegowym lub operacyjnym. Wskazaniem do leczenia zabiegowego jest choroba hemoroidalna w stopniu II i III, objawowa, w której leczenie zachowawcze nie przynosi oczekiwanego efektu lub gdy efekt leczenia zachowawczego jest jedynie krótkotrwały. Poszukiwania alternatywnych metod leczenia guzków krwawniczych przynoszą nowe rozwiązania lub kolejne modyfikacje już istniejących sposobów leczenia mające na celu poprawę wyników i indywidualizację leczenia. Do alternatywnych metod leczenia guzków krwawniczych należą: metoda Barrona, skleroterapia, DGHAL, krioterapia, diatermia jednobiegunowa i niskonapięciowa (met. Hemoron), elektrokoagulacja bipolarna, laser CO2, diodowy oraz neodymowo-yagowy. W artykule przedstawiono aktualne dane dotyczące skuteczności poszczególnych metod w oparciu o najnowsze piśmiennictwo i wyniki publikowanych badań. Autorzy zwracają również uwagę na ograniczenia i specyficzne dla poszczególnych metod powikłania.
Summary
It is estimated that haemorrhoids affect more than half of the population over 50 years of age. The main symptoms of haemorrhoidal disease include bleeding, haemorrhoidal prolapse, discomfort, burning, itching and a feeling of incomplete evacuation. The severity of symptoms depends on many factors. The treatment of haemorrhoidal disease is primarily aimed to limit the symptoms, which can be achieved via conservative, interventional or surgical treatment. Indications for interventional treatment include symptomatic stage II and III haemorrhoidal disease when conservative therapy does not bring the desired effect, or the effect is only temporary. The search for alternative methods for the treatment of haemorrhoids results in new solutions as well as further modifications of the existing treatments, which is aimed at therapeutic outcome improvement and treatment individualisation. Alternative interventional therapies include Barron’s method, Sclerotherapy, DGHAL, cryotherapy, unipolar and low-voltage diathermy (Hemoron), bipolar electrocautery, CO2, diode and Nd:YAG laser. The article presents current data on the effectiveness of these methods based on the latest literature and published studies. The authors also point to limitations and complications associated with the described methods.

Introduction
It is estimated that haemorrhoids affect more than half of the population over 50 years of age. The main symptoms of haemorrhoidal disease include bleeding, discomfort, burning, itching and a feeling of incomplete evacuation. Pain and haemorrhoidal prolapse can occur in later stages of the disease. The varying severity of the symptoms depends on many factors, such as, primarily, the stage of the disease, but also diet, age, sports activity, type of work and genetic predispositions. The treatment of haemorrhoidal disease is mainly aimed to limit the symptoms. In most cases, conservative or interventional treatment is sufficient. At present, only 10% of patients require surgical treatment. Indications for alternative interventional treatment include symptomatic stage II and III haemorrhoidal disease when conservative therapy does not bring the desired effect, or the effect is only temporary. In exceptional cases, interventional treatment is used in patients with stage IV haemorrhoidal disease, particularly in patients not qualified for surgical treatment due to age or multiple comorbidities. The lack of patient’s consent for surgical treatment, which often results from the fear of potential postoperative pain and complications, sphincter dysfunction in particular, is another indication for interventional treatment. For centuries, the search for alternative methods for the treatment of haemorrhoids have brought new solutions or further modifications of the existing treatments (1). The aim of these measures is to improve treatment outcomes and allow for tailoring therapy for individual patients. Efficacy assessments for a given technique found in the literature are based on the rate of recurrence as well as the incidence and the type of complications. Methods for interventional treatment of haemorrhoidal disease are presented in table 1.
Tab. 1. Interventional methods for the treatment of haemorrhoidal disease
| Barron’s method (RBL) |
| Sclerotherapy |
| DGHAL |
| Cryotherapy |
| Infrared coagulation |
| Unipolar and low-voltage diathermy |
| Bipolar electrocoagulation |
Laser therapy:
– CO2 laser
– diode laser
– Nd:YAG laser |
Although the Barron’s method (rubber band ligation – RBL) was first described in 1963, it is still one of the most popular non-surgical procedures for the treatment of haemorrhoids (2). This popularity is due to the low costs, acceptable efficacy and low complication rate. The technique involves placing a rubber-band around the base of the haemorrhoid using a special cylindrical ligator. The haemorrhoidal tissue is pulled into a cylinder to allow the placement of rubber bands around the base of the haemorrhoid. As a result, ischemia develops, leading to haemorrhoid fibrosis, necrosis and spontaneous amputation (3). Patients with stage II and III haemorrhoids, particularly those complaining of bleeding or haemorrhoidal prolapse, are qualified for the procedure. Providing the patient with detailed information about the course of the procedure as well as symptoms that may occur during the procedure is an important element of this type of treatment. Moderate pain, minor bleeding after several days or tenesmus are expected symptoms that usually resolve after 1 or 2 days and should not cause anxiety. Prolonged symptoms, lack of response to pharmacotherapy or increased temperature should be alarming for patients, who should contact their doctor. The need to repeat the procedure several times in order to achieve the desired effect is an inconvenience of this technique. Usually, one rubber band is placed on a single haemorrhoid. Once the wound has healed, another rubber band is placed on another haemorrhoid (fig. 1).

Fig. 1. A haemorrhoid after rubber band ligation (Barron’s method)
Sclerotherapy is also one of the most commonly used methods in the treatment of haemorrhoids. Haemorrhoid fibrosis occurs as a result of inflammatory response to the injected obliterating agent into the submucosal layer at the base of the haemorrhoid. A simple anoscope or an anoscope featuring special canal for the injection needle is used in the procedure (4). Obliterating preparations have changed over the years. The name of the procedure was determined by the type of obliterating preparation – Blanchard’s method used 5% phenol in almond oil, while an injection of quinine urethane was used in the Blond method (5, 6). Presently, 3% polidocanol is the most popular preparation. Obliterating preparation is administered in the form of fluid or foam. A simultaneous injection of all haemorrhoids, which allows for a quick effect and limits the need for repeated medical appointments, is an advantage of the method. Proper administration of the agent into the submucosal layer is an important technical aspect of this method. Deeper injection can lead to complications, such as inflammation and even local necrosis (fig. 2).
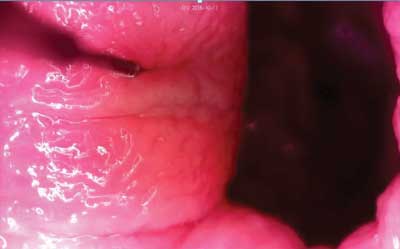
Fig. 2. Sclerotherapy
DGHAL requires local, peripheral or general anaesthesia and involves ligation of the vessels that supply haemorrhoids using a special Doppler-equipped anoscope (7). Limitation of indications to early stage disease is a disadvantage of the method. Patients with stage II non-prolapsed haemorrhoids are qualified for this treatment. The technique is additionally limited by high costs. In patients with prolapsing haemorrhoids, DGHAL can be combined with recto-anal-repair (RAR), which involves lifting and fixing the prolapsing mucosa into its correct position, which reduces the prolapse.
Powyżej zamieściliśmy fragment artykułu, do którego możesz uzyskać pełny dostęp.
Mam kod dostępu
- Aby uzyskać płatny dostęp do pełnej treści powyższego artykułu albo wszystkich artykułów (w zależności od wybranej opcji), należy wprowadzić kod.
- Wprowadzając kod, akceptują Państwo treść Regulaminu oraz potwierdzają zapoznanie się z nim.
- Aby kupić kod proszę skorzystać z jednej z poniższych opcji.
Opcja #1
29 zł
Wybieram
- dostęp do tego artykułu
- dostęp na 7 dni
uzyskany kod musi być wprowadzony na stronie artykułu, do którego został wykupiony
Opcja #2
69 zł
Wybieram
- dostęp do tego i pozostałych ponad 7000 artykułów
- dostęp na 30 dni
- najpopularniejsza opcja
Opcja #3
129 zł
Wybieram
- dostęp do tego i pozostałych ponad 7000 artykułów
- dostęp na 90 dni
- oszczędzasz 78 zł
Piśmiennictwo
1. Winkler R: Schorzenia splotów hemoroidalnych. [W:] Winkler R (red. pol. wyd. Dziki A): Proktologia praktyczna. Elsevier Urban & Partner, Wrocław 2013: 92-114. 2. Barron J: Office ligation of internal hemorrhoids. Am J Surg 1963; 105: 563-570. 3. Albuquerque A: Rubber band ligation of hemorrhoids: A guide for complications. World J Gastrointest Surg 2016 Sep 27; 8(9): 614-620. 4. Kucharczyk A, Kołodziejczak M: Czy skleroterapia guzków krwawniczych jest tylko metodą historyczną? Nowa Med 2015; 2: 63-66. 5. Blond K, Hoff H: Das Hamorrhoidalleiden. Deuticke, Leipzig Wien 1936. 6. Blanchard CE: Textbook of ambulant proctology. Medical Success Press, Youngtown, Ohio 1928: 134. 7. Chowdri NA, Parray FQ (eds.): Benign Anorectal Disorders A Guide to Diagnosis and Management. Springer, New Delhi 2016. 8. Crawshaw BP, Russ AJ, Ermlich BO et al.: Prospective Case Series of a Novel Minimally Invasive Bipolar Coagulation System in the Treatment of Grade I and II Internal Hemorrhoids. Surg Innov 2016 Dec; 23(6): 581-585. 9. Ahmad A, Kant R, Gupta A: Comparative Analysis of Doppler Guided Hemorrhoidal Artery Ligation (DG-HAL) & Infrared Coagulation (IRC) in Management of Hemorrhoids. Indian J Surg 2013 Aug; 75(4): 274-277. 10. Maloku H, Gashi Z, Lazovic R et al.: Laser Hemorrhoidoplasty Procedure vs Open Surgical Hemorrhoidectomy: a Trial Comparing 2 Treatments for Hemorrhoids of Third and Fourth Degree. Acta Inform Med 2014 Dec; 22(6): 365-367. 11. Crea N, Pata G, Lippa M et al.: Hemorrhoidal laser procedure: short- and long-term results from a prospective study. Am J Surg 2014 Jul; 208(1): 21-25. 12. Naderan M, Shoar S, Nazari M et al.: A Randomized Controlled Trial Comparing Laser Intra-Hemorrhoidal Coagulation and Milligan-Morgan Hemorrhoidectomy. J Invest Surg 2016 Nov 2: 1-7. 13. Aram F: Rubber Band Ligation for Hemorrhoids: an Office Experience. Indian J Surg 2016 Aug; 78(4): 271-274. DOI: 10.1007/s12262-015-1353-1. Epub 2015 Oct 22. 14. Misauno MA, Usman BD, Nnadozie UU, Obiano SK: Experience with rubber band ligation of hemorrhoids in northern Nigeria. Niger Med J 2013 Jul-Aug; 54(4): 258-260. 15. Brown SR, Tiernan JP, Watson AJ et al.: Haemorrhoidal artery ligation versus rubber band ligation for the management of symptomatic second-degree and third-degree haemorrhoids (HubBLe): a multicentre, open-label, randomised controlled trial. Lancet 2016 Jul 23; 388(10042): 356-364. 16. Giamundo P: Adventages and limits of hemorrhoidal dearterialization in the treatment of symptomatic hemorrhoids. World J Gastrointest Surg 2016; 8(1): 1-4. 17. Zinberg SS, Stern DH, Furman DS, Wittles JM: A personal experience in comparing three nonoperative techniques for treating internal hemorrhoids. Am J Gastroenterol 1989 May; 84(5): 488-492. 18. Kaidar-Person O, Person B, Wexner SD: Hemorrhoidal disease: A comprehensive review. J Am Coll Surg 2007; 204: 102-117. 19. Weyand G: CHAZ 14, Vol. 6. Book. 20. Crea N, Pata G, Lippa M et al.: Hemorrhoidal laser procedure: short and long term results from a prospective study. The American Journal of Surgery 2014. 21. Guindic LC: Treatment of uncomplicated hemorrhoids with a Hemor-Rite® cryotherapy device: a randomized, prospective, comparative study. Journal List J Pain Resv 2014; 7: 57-63.



