*Lidia Zawadzka-Głos, Krzysztof Ślączka
Effects of post-intubation laryngeal stenosis treatment depending on the grade of stenosis
Analiza efektów leczenia zwężeń pointubacyjnych krtani w zależności od stopnia zwężenia
Department of Pediatric Otolaryngology, Medical University of Warsaw, Poland
Head of Department: Associate Professor Lidia Zawadzka-Głos, MD, PhD
Streszczenie
Wstęp. Zwężenia krtani związane z przedłużoną intubacją w grupie dzieci przedwcześnie urodzonych, z uwagi na rosnącą populację tych dzieci, są aktualnym problemem laryngologii dziecięcej. Celem pracy było przeprowadzenie analizy przypadków pointubacyjnych zwężeń krtani pod względem częstości i stopnia nasilenia powikłań, jak również analiza wyników leczenia endoskopowego.
Materiał i metody. Do badania włączono grupę 92 dzieci leczonych z powodu powikłań pointubacyjnych krtani. W przeprowadzonej analizie porównano grupę dzieci pod względem stopnia zwężenia podgłośniowego krtani i jego wpływu na efekt leczenia. Zastosowano metodę endoskopową leczenia zwężeń pointubacyjnych krtani. Zabieg przeprowadzano w znieczuleniu ogólnym.
Wyniki. W grupie dzieci ze zwężeniem pointubacyjnym krtani stwierdzono zwężenie inne niż podgłośniowe u 9,78% dzieci, zwężenie podgłośniowe I stopnia u 10,87% dzieci, II stopnia – u 41,3% dzieci, III stopnia – u 18,48% dzieci, IV stopnia – u 19,57% dzieci. W badanej grupie 92 dzieci tylko 41 dzieci było urodzonych o czasie (44,57%), a 51 (55,43%) było urodzonych przedwcześnie. W grupie poddanej leczeniu uzyskano wyleczenie u 44 dzieci (48%), poprawę, czyli zmniejszenie stopnia zwężenia pointubacyjnego, uzyskano u 38 dzieci (41%), zaś niepowodzenie w leczeniu odnotowano u 10 pacjentów (11%). W grupie wcześniaków wyleczono 20 dzieci (39,22%), poprawę uzyskano u 22 dzieci (43,14%), niepowodzenie odnotowano u 9 dzieci (17,65%). W grupie dzieci urodzonych o czasie uzyskano pełne wyleczenie u 24 dzieci (58,54%), poprawę w 16 przypadkach (39,02%) oraz niepowodzenie w 1 przypadku (2,44%). Obserwowano również wzrost ryzyka niepowodzenia leczenia w zaawansowanych zwężeniach krtani stopnia III i IV według Cotton–Myer.
Wnioski. Zwężenia pointubacyjne krtani są problemem często występującym u wcześniaków. Leczenie endoskopowe zwężeń pointubacyjnych jest skuteczną metodą chirurgiczną. Niepowodzenie w leczeniu endoskopowym związane jest ze stopniem zwężenia. Zwężenia pointubacyjne krtani III i IV stopnia trudniej poddają się leczeniu.
Summary
Introduction. Laryngeal stenosis as a complication of prolonged endotracheal intubation is a current problem in paediatric laryngology because of the growing population of prematurely born children. The aim of our study was to analyse the cases of post-intubation laryngeal stenosis in terms of the frequency and severity of the complications, as well as to evaluate the effects of endoscopic treatment.
Material and methods. The study included 92 children treated for laryngeal stenosis. The analysis involved the comparison of the children in terms of the degree of subglottic stenosis and its effect on treatment. Laryngeal stenosis was treated with endoscopy, which was performed under general anaesthesia.
Results. In the group of children with laryngeal stenosis, supraglottic stenosis was found in 9.78% of children, grade I subglottic stenosis occurred in 10.87% of children, grade II in 41.3% of children, grade III in 18.48% of children, and grade IV in 19.57% of children. Of 92 patients, only 41 were full-term (44.57%) and 51 (55.43%) were premature. In the treated group, full recovery and a reduction of laryngeal stenosis were noted in 44 (48%) and 38 children (41%), respectively, while the failure of treatment was reported in 10 patients, representing 11% of the population. In the group of premature infants, 20 children (39.22%) were cured, the condition improved in 22 cases (43.14%) and treatment failed in 9 patients (17.65%). Of 41 full-term children, full recovery was observed in 24 (58.54%), improvement in 16 (39.02%) and failure in one case (2.44%). There was also an increase in the risk of treatment failure in advanced stenosis of grade III and IV according to Cotton–Myer.
Conclusions. Laryngeal stenosis is a common problem in premature infants. Endoscopic treatment is an effective surgical method. Failure of endoscopic treatment is related to the degree of stenosis. Grades III and IV are more difficult to treat.
Key words: which was performed under general anaesthesia. Results. In the group of children with laryngeal stenosis,
supraglottic stenosis was found in 9.78% of children,
grade I subglottic stenosis occurred in 10.87% of children,
grade II in 41.3% of children,
grade III in 18.48% of children,
and grade IV in 19.57% of children. Of 92 patients,
only 41 were full-term (44.57%) and 51 (55.43%) were premature. In the treated group,
full recovery and a reduction of laryngeal stenosis were noted in 44 (48%) and 38 children (41%),
respectively,
while the failure of treatment was reported in 10 patients,
representing 11% of the population. In the group of premature infants,
20 children (39.22%) were cured,
the condition improved in 22 cases (43.14%) and treatment failed in 9 patients (17.65%). Of 41 full-term children,
full recovery was observed in 24 (58.54%),
Introduction
Intubation is currently commonly used to maintain patency of the airways during surgeries, in unconscious patients and in intensive care units. It can cause local laryngeal complications. Lindholm, in 1969, was the first to describe posttraumatic tracheal and laryngeal changes after intubation for anaesthetic purposes (1). His studies demonstrated that the size of a tracheal tube and its unfavourable shape are responsible for complications after prolonged intubation. At that time, they were evaluated by physicians of various specialties with no uniform classification system. That is why their prevalence ranged from 0.5% to 61% (2, 3).
Cotton, Myer, Holinger and Montgomery claim that the subglottic region is a predisposing site to post-intubation complications (4-6). Changes in the posterior subglottis are not well diagnosed, but occur both in adults and children with equal frequency (7, 8).
The pathogenesis of such complications involves the fact that pressure that a tube exerts on the laryngeal wall causes blood flow disorders in mucosal capillaries. This leads to mucosal ischaemia, inflammation and oedema as soon as a few hours after intubation. Capillary flow disorders cause epithelial damage and ulceration, which are the basis for subsequent post-intubation complications. Deepening ulcerations result in mucosal necrosis and perichondritis even after 96 hours. Perichondritis may develop into laryngeal chondritis, which leads to necrosis (9, 10).
When a tracheal tube is removed, minor epithelial lesions undergo regeneration and reepithelialisation. If the healing process is incomplete, the histopathological examination will reveal squamous metaplasia and the lack of cilia (10). More advanced lesions heal through granulation or hard scar formation, leading to cicatricial narrowing within the subglottis.
Irrespective of the route of insertion, whether nasal or oral, a tracheal tube always compresses the posterior laryngeal wall. According to Lindholm and Weymuller, the larynx has three sites that are particularly exposed to compression (1, 11). These are: the medial surface of the arytenoids with the cricoarytenoid articulation and vocal process, the posterior part of the glottis in the interarytenoid region and the subglottal area, particularly the anterior surface of the posterior part of the cricoid cartilage.
Post-intubation lesions may affect one or several of these laryngeal sites. They mainly cause respiratory problems, but may also lead to phonation disorders. Cicatricial laryngeal stenosis requires surgical treatment.
Aim
The aim of the paper was to assess the effects of post-intubation laryngeal stenosis treatment depending on the grade of stenosis.
Material and methods
The analysis involved 92 patients treated for post-intubation laryngeal stenosis in the Department of Paediatric Otolaryngology of the Medical University of Warsaw. The grade of subglottic stenosis was assessed based on the Cotton–Myer classification, where grade I means obstruction of up to 50% of the lumen, grade II: 51-70% obstruction, grade III: 71-99% obstruction, and grade IV: 99-100% obstruction.
All patients were treated endoscopically using argon plasma coagulation (APC), and outcomes were assessed with respect to the grade of stenosis. Argon plasma coagulation is a contact-free method of monopolar electrosurgical coagulation based on a thermal effect in tissues exerted by high-frequency (HF) currents. The application of high-frequency current to tissue leads to its rapid dehydration and collagen shrinkage, thereby reducing its volume. The procedures were conducted under general anaesthesia with an APC ERBOTROM ICC 350 device. Spray coagulation of 30-50 W and argon flow of 0.3-1.4 l/min were applied.
Results
In the group of children with laryngeal stenosis, supraglottic stenosis was found in 9.78% of children, grade I subglottic stenosis occurred in 10.87% of children, grade II in 41.3% of children, grade III in 18.48% of children, and grade IV in 19.57% of children (fig. 1). Of 92 children, only 41 were full-term (44.57%) and 51 (55.43%) were premature. In the treated group, full recovery and a reduction of laryngeal stenosis were noted in 44 (48%) and 38 children (41%), respectively, while failure of treatment was reported in 10 patients, representing 11% (fig. 2). In the group of premature infants, 20 children (39.22%) were cured, the condition improved in 22 cases (43.14%) and treatment failed in 9 patients (17.65%). Of 41 full-term children, full recovery was observed in 24 (58.54%), improvement in 16 (39.02%) and failure in one case (2.44%).
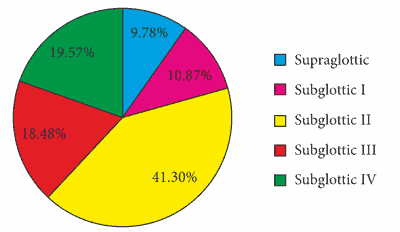
Fig. 1. Grade of laryngeal stenosis

Fig. 2. Treatment outcome
Subglottic stenosis was graded according to the Cotton–Myer classification, from grade I to grade IV. Laryngeal stenosis other than subglottic was marked with 0. The correlation between the stenosis grade and therapeutic effect was analysed (tab. 1), and it was found that the best outcomes after endoscopic treatment were achieved for grades I and II in the Cotton–Myer classification. Grades III and IV were more difficult to treat, with grade IV resulting in much worse treatment outcomes. Of 10 patients with no improvement, the number of failed treatment cases was 1 for grade II subglottic stenosis, 2 for grade III and 7 for grade IV. Among 44 cured patients, only 3 had grade IV subglottic stenosis. The grade of stenosis correlated with the treatment outcome in a statistically significant way. A high grade of subglottic stenosis was more frequently identified in patients with no improvement after treatment.
Tab. 1. Efekt leczenia a stopień zwężenia
| | | Stopień 0 | Stopień I | Stopień II | Stopień III | Stopień IV | Wiersz | % |
| Liczba | Wyleczonych | 2 | 8 | 21 | 10 | 3 | 44 | 47,83% |
| % z kolumny | | 22,22% | 80,00% | 55,26% | 58,82% | 16,67% | | |
| % z wiersza | | 4,55% | 18,18% | 47,73% | 22,73% | 6,82% | | |
| Liczba | Poprawa | 7 | 2 | 16 | 5 | 8 | 38 | 41,30% |
| % z kolumny | | 77,78% | 20,00% | 42,11% | 29,41% | 44,44% | | |
| % z wiersza | | 18,42% | 5,26% | 42,11% | 13,16% | 21,05% | | |
| Liczba | Brak poprawy | 0 | 0 | 1 | 2 | 7 | 10 | 10,87% |
| % z kolumny | | 0,00% | 0,00% | 2,63% | 11,76% | 38,89% | | |
| % z wiersza | | 0,00% | 0,00% | 10,00% | 20,00% | 70,00% | | |
| Kolumna | | 9 | 10 | 38 | 17 | 18 | 92 | |
| % | | 9,78% | 10,87% | 41,30% | 18,48% | 19,57% | | 100,00% |
Discussion
Endoscopy for subglottic stenosis in children has been used in the Department of Paediatric Otolaryngology for many years. Up to 1999, the Danielewicz method was employed. It consists of intralaryngeal incisions and insertion of a laryngeal separator. The method of endoscopic laryngeal dilation with argon plasma coagulation has been used since 1999. The treatment of post-intubation laryngeal stenosis in children is difficult and involves several stages. There are no age restrictions for the initiation of treatment. In most cases, children with post-intubation stenosis require tracheotomy to obtain airway patency. Tracheotomy is a factor that reduces normal development in the period of speech development. Such children require individual care, and a parent frequently resigns from work. That is why treatment of these conditions is so important, not only for medical, but also psychological and economic reasons. There are many ways of managing post-intubation laryngeal stenosis, including endoscopic argon plasma coagulation. Treatment outcomes observed in our Department are comparable with those reported in the literature. The application of the new endoscopic method using argon plasma coagulation has led to a high rate of full recovery. Within a decade of our experience based on 92 patients with subglottic stenosis managed with endoscopic argon plasma coagulation, we have obtained the following outcomes: the treatment result was positive in 82 patients: decannulation was possible in 44 cases whereas 38 children improved and were deemed candidates for decannulation. Positive treatment effects were not obtained in only 10 cases, which constitutes 10.87% of the whole group. This rate of treatment failure in endoscopy is not different from those reported in the global literature (12). Based on our own results, it can be stated that, among many endoscopic methods, argon plasma coagulation can be a valuable and safe strategy for the treatment of post-intubation laryngeal stenosis.
This study also involved the analysis of the relationship between stenosis grade and treatment outcomes as well as evaluation of children with post-intubation stenosis in order to determine risk factors of post-intubation complications. Cases in which a satisfactory effect was not obtained after endoscopy received particular emphasis. Treatment effects were found to be significantly correlated with the grade of post-intubation subglottic stenosis.
This study also investigated treatment outcomes achieved with argon plasma coagulation relative to the grade of subglottic stenosis. The best therapeutic effects were observed in children with grade I and II stenosis in the Cotton scale. Grades III and IV were more difficult to treat, with grade IV resulting in much worse treatment outcomes. The literature offers a lot of publications on treatment effects in patients with post-intubation laryngeal stenosis after implementation of various endoscopic techniques and open surgeries in relation to the grade of stenosis (13-16). The higher the grade, the lower the decannulation percentage and the longer the treatment duration. Endoscopy used in severe grades III and IV leads to much worse outcomes when compared with open surgery. That is why a number of authors believe that grades III and IV should be managed with open surgery only (13, 16). Endoscopy proves effective for grade I and II as well as slight grade III stenosis, and is recommended as first-choice treatment, with open surgery used only in the case of first-line treatment failure (13, 17, 18). The results obtained in this study are in line with foreign authors’ reports. Argon plasma coagulation can be used with good effects in endoscopic treatment of post-intubation laryngeal stenosis with grades I, II and III in the Cotton classification. Of 10 patients with no improvement, the number of failed treatment cases was 1 for grade II, 2 for grade III and 7 for grade IV subglottic stenosis.
Conclusions
Laryngeal stenosis is a common problem in premature infants. Endoscopic treatment is an effective surgical method. The grade of stenosis correlates with the treatment outcome in a statistically significant way. A high grade of subglottic stenosis carries worse prognosis concerning full recovery after the application of endoscopic argon plasma coagulation.
Piśmiennictwo
1. Lindholm CE: Prolonged endotracheal intubation (a clinical investigation with specific reference to its consequences for larynx and trachea) and its place as an alternative to tracheostomy. Acta Anaesthes Scan (Suppl) 1969; 33: 1-131.
2. Aberdeen EA, Downes JJ: Artificial airways in children. Surg Clin North Am 1974; 54: 1155-1170.
3. Walner DL, Loewen MS, Kimura RE: Neonatal subglottic stenosis- incidence and trends. Laryngoscope 2001; 111(1): 48-51.
4. Holinger LD: Treatment of severe subglottic stenosis without tracheotomy- a preliminary report. Ann Otol Rhinol Laryngol 1982; 91: 407-410.
5. Cotton RT, Myer CM: Contemporary surgical management of laryngeal stenosis in children. Am J Otolaryngol Head Neck Surg 1984; 5: 360-368.
6. Montgomery WW: Chronic subglottic stenosis. Otolaryngol Clin North Am 1984; 17: 107-113.
7. Carron JD, Derkay CS, Strope GL et al: Pediatric tracheotomies: Changing Indications and Outcomes. Laryngoscope 2000; 110: 1099-1103.
8. Cohen SR: Pseudolaryngeal paralysis: a postintubation complication. Ann Otol Rhinol Laryngol 1981; 90: 483-488.
9. Jorgensen J, Weil JL, Sykes KJ et al: Incidence of and risk factors for airway complications following endotracheal intubation for bronchiolitis. Otolaryngol Head Neck Surg 2007; 137(3): 394-399.
10. Sato K, Nakashima T: Histopathologic changes in laryngeal mucosa of extremely low-birth weight infants after endotracheal intubation. Ann Otol Rhinol Laryngol 2006; 115(11): 816-823.
11. Weymuller EA: Laryngeal injury from prolonged endotracheal intubation. Laryngoscope 1988; 98(Suppl 45): 1-15.
12. Bakthavachlam S, McClay JE: Endoscopic management of subglottic stenosis. Otolaryngol Head Neck Surg 2008; 139(4): 551-559.
13. Alvarez-Neri H, Penchyna-Grub J, Porras-Hernandez JD et al: Primary cricotracheal resection with thyrotracheal anastomosis for the treatment of severe subglottic stenosis in children and adolescents. Ann Otol Rhinol Laryngol 2005; 114: 2-6.
14. Bailey M, Hoeve H, Monnier P: Paediatric laryngotracheal stenosis: a consensus paper from three European centres. Eur Arch Otorhinolaryngol 2003; 260: 118-123.
15. Hartley BE, Rutter MJ, Cotton RT: Cricotracheal resection as a primary procedure for laryngotracheal stenosis in children. Int J Pediatr Otorhinolaryngol 2000; 54(2-3): 133-136.
16. Hartley BE, Cotton RT: Paediatric airway stenosis: laryngotracheal reconstruction or cricotracheal resection? Clin Otolaryngol Allied Sci 2000; 25(5): 342-349.
17. Maksoud-Filho JG, Goncalves ME, Cardoso SR et al: Early diagnostic and endoscopic dilatation for the treatment of acquired upper airway stenosis after intubation in children. J Pediatr Surg 2008; 43(7): 1254-1258.
18. Matute JA, Villafruela MA, Delgado MD et al: Surgery of subglottic stenosis in neonates and children. Eur J Pediatr Surg 2000; 10(5): 286-290.

