© Borgis - New Medicine 2/2008, s. 45-47
*Eryk Chrapowicki, Marek Kruk, Grzegorz Krasowski, Andrzej Płoński
A case of recurrent bleeding from the upper gastrointestinal tract in the course of acute pancreatitis
Department of General Surgery, Wolski Gostyńska Memorial Hospital, Warsaw
Summary
We present a rare case of coincidence of severe and life-threatening complications of pancreatitis: abscess and bleeding due to rupture of pseudoaneurysm. CT angiography is usually recommended to establish the diagnosis. Aspiration or surgery with drainage of the abscess are the common methods of treatment. Endovascular embolisation of the feeding artery seems to be the method of choice, but surgery is reserved for patients with haemodynamic instability and haemorrhagic shock or with recurrent bleeding.
Introduction
The acute pancreatitis morbidity rate is estimated at 240/1 million habitants, i.e. about 9 000 patients per year. According to the Atlanta classification, severe and benign forms of pancreatitis may be distinguished. In the severe form, which concerns about 15% of patients, many systemic and local complications may occur. Both abscess and, leading to pseudoaneurysm formation, vascular erosion are generally known local complications of severe pancreatitis. Each of them is associated with a high death risk (12% and 57%, respectively). Among many publications regarding diagnostics and treatment conducted in similar cases that we have found while reviewing world-wide literature, we did not come across an article describing coincidence of both above-mentioned complications. Thus, we believe that diagnostics and treatment procedures may be very difficult to establish.
Case report
A sixty-three-year-old male patient, with long-term alcohol abuse and a history of alcohol-induced chronic pancreatitis, was admitted to the internal ward due to exacerbation of epigastric pain. A physical examination of his abdomen did not reveal any abnormal findings; no peritoneal symptoms were found. BP 130/80, HR 88. Except for high levels of serum amylase (948), with normal range not exceeding 250, all the other biochemical blood parameters were in the normal ranges.
A computer tomography scan of the abdomen revealed a pseudocyst (83x94x93 mm size) which was localized in the head of the pancreas, moulding to the duodenum, and abutting the distal part of the stomach.
Conservative treatment was initiated: intraintestinal (enteral) nutrition, analgesics and relaxants were applied and endoscopic drainage of the pseudocyst was planned.
On the 20th day of hospitalization the patient presented symptoms of bleeding from the upper gastrointestinal tract in the form of blood vomiting, melaena and blood pressure decrease. He was given some fluids i.v., omeprasol, a group-compatible transfusion, three units of erythrocytic mass, and 2 units of plasma, and it enabled stabilization of his state to be achieved. An emergency gastroscopy revealed massive duodenal ulceration covered with a clot, which included about 1/3 of the duodenal circumference. The patient was classified for surgical treatment; he was transferred to the surgical ward, and the Whipple operation was planned.
Due to poor nutritional status, confirmed by laboratory test results, parenteral nutrition was instituted.
On the 3rd day after the patient´s transfer, he had massive bleeding into the gastrointestinal lumen. He underwent an emergency operation.
After performing a gastrostomy and duodenotomy, the operating surgeons found out that the pancreatic abscess had perforated into the duodenal lumen. A bleeding vessel was visible in the abscess cavity and it was underpinned with nonabsorbable sutures. In regard of ischaemic lesions observed in the initial 1/3 of the duodenal wall, the pylorus and the duodenal stump were sutured, and necrotic tissues were removed after checking the patency of the biliary tracts and localization of the papilla of Vater. Precolic gastroduodenostomy with Brown´s fistula was subsequently carried out. A jejunostomy was performed in order to conduct parenteral alimentation in the postoperative period. The abscess cavity was drained using a Petzer´s drain placed in the area of the duodenal chimney (edge) as well as in rectovesical excavation.
The patient stayed in the intensive care ward for 8 days. When his state was better, he was moved to the general surgery ward. From day 11 after the operation enteral alimentation was introduced and intensive physical rehabilitation was carried out. Oral alimentation was introduced on day 15. Further hospitalization proceeded with no complications. The patient was discharged from the hospital on day 25. Control CT scan of his abdominal cavity was planned after 1 month.
Eight days after discharge, the patient was once again admitted to the surgical ward due to symptoms of bleeding from the upper gastrointestinal tract which initially were stopped using conservative therapy. Gastroscopy performed on the next day revealed the sources of bleeding and, thus, a CT examination was carried out, which revealed the existence of an anomalous cistern of clotted blood, which was probably a residue of aneurysm of the gastro-duodenal artery, located between the pancreas and the duodenum.
Observing no symptoms of bleeding, and radiological presentation suggesting clotting of the aneurysm, the surgeons decided not to operate on the patient.
The patient´s state was stable for the next 5 days. On day 6 massive bleeding from the upper gastrointestinal tract accompanied by signs of shock took place.
The patient was transferred to the operating suite and operated on, following an unsuccessful attempt of endovascular vessel obliteration.
During the operation a laparotomy and, subsequently, a duodenotomy were performed. Clots localized in the duodenal lumen were evacuated and an aperture of the fistula to the false aneurysm of the gastro-duodenal artery was found. Ligating the artery just above the aneurysm, the cavity of which was additionally sutured, enabled the bleeding to be arrested. Introduction of Silastic, releasing the drain into the duodenal lumen, produced its closure. Then haemostasis and closure of the patient´s integument were performed. Four units of group-compatible red blood cell concentrate and four units of group compatible plasma were transfused during the operation.
The patient stayed in the intensive care unit for 4 days following the operation. When his general state improved, he was transferred to the surgical ward in order to continue alimentation treatment and rehabilitation. The patient was discharged from the hospital in a generally good state after 20 days.
Discussion
Pancreatic abscess is a severe complication of acute pancreatitis. Prognosis in such cases is very serious but new therapeutic methods such as drainage under USG control and wide spectrum antimicrobial therapy have enabled the mortality in this group of patients to be decreased – by up to 10% (7).
Interestingly, in the reported case typical symptoms suggesting pancreatic abscess formation were lacking. This is probably related to its spontaneous drainage into the lumen of the gastrointestinal tract. Unfortunately, it did not protect the patient from bleeding, which was a consequence of the focal inflammation process.
False aneurysm formation can be one of the complications of pancreatitis (1, 9). It is caused by both pancreatic enzyme activity and high pressure which accompanies cyst or abscess formation. It is most frequently related to the lienal artery (65%), next to the gastro-duodenal artery (up to 25%), rarely to the pancreatico-duodenal artery (up to 15%), and only exceptionally to the left gastric artery.
In the diagnostic procedures CT angiography is definitely recommended (5). It enables simultaneous assessment of lesions in the pancreatic parenchyma as well as aneurysmal location and size.
One of the consequences of aneurysm rupture may be bleeding into the abdominal cavity or rarely into the gastrointestinal lumen, or sometimes into the retroperitoneum. Bleeding into Wirsung´s duct (hemosuccus, Wirsungorrhea) may be an extremely rare complication of the disease (6). In the described case, the rupture was into the duodenal chimney formed during the initial operation.
In cases of haemodynamically stable patients initially an attempt of intravascular aneurysm embolization is generally recommended (1). In cases of patients presenting symptoms of shock an emergency laparotomy is recommended. The intravascular procedure mentioned above is successful in nearly 70-100% of cases, but recurrence of bleeding is possible in about 30% of cases (1, 2, 3, 4).
In the reported case an initial attempt of intravascular intervention was made but it was stopped due to sudden deterioration of haemodynamic parameters of the patient.
Surgical procedures include simple vessel ligation or excision of the false aneurysm (3). It depends on both the patient´s state and anatomical location of the lesion.
However, such a procedure has a high, up to 25%, risk of death.
Occurrence of the described complication reminds us that in cases of recurrent bleeding from the upper gastrointestinal tract in patients with pancreatic diseases it is necessary to keep in mind the possibility of aneurysm formation and its rupture.

Fig. 1. Legend. L – liver; V – stomach; HC – common hepatic artery; HP – hepatic artery proper; the arrow points to the aneurysm of the gastroduodenal artery.
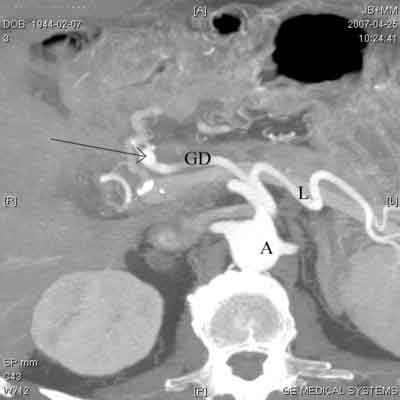
Fig. 2. A – abdominal aorta; L – splenic artery; GD – gastroduodenal artery; the arrow points to the aneurysm.
Piśmiennictwo
1. Pillay W, Lalloo S, Thomson S, et al.: Embolisation of metachronous pseudoaneurysms complicating chronic pancreatitis. HPB (Oxford). 2003; 5 (4): 251-253. 2. Chong WW, Tan SG, Htoo MM: Endovascular treatment of gastroduodenal artery aneurysm. Asian Cardiovasc Thorac Ann. 2008 Jan; 16 (1): 68-72. 3. Sun JB, Wang YJ, Li A: [The management of bleeding pseudoaneurysms in patients with severe acute pancreatitis]. Zhonghua Wai Ke Za Zhi. 2007 Jun 1; 45 (11): 730-2. Chinese. 4. Chen HL, Chang WH, Shih SC, et al.: Ruptured pancreaticoduodenal artery pseudoaneurysm with chronic pancreatitis presenting as recurrent upper gastrointestinal bleeding. Dig Dis Sci. 2007 Nov; 52 (11): 3149-53. Epub 2007 Apr 3. 5. Hyare H, Desigan S, Nicholl H, et al.: Multi-section CT angiography compared with digital subtraction angiography in diagnosing major arterial hemorrhage in inflammatory pancreatic disease. Eur J Radiol. 2006 Aug; 59 (2): 295-300. Epub 2006 Mar 20. 6. Etienne S, Pessaux P, Tuech JJ, et al.: Hemosuccus pancreaticus: a rare cause of gastrointestinal bleeding. Gastroenterol Clin Biol. 2005 Mar; 29 (3): 237-42. 7. Srikanth G, Sikora SS, Baijal SS, et al.: Department of Surgical Gastroenterology, Sanjay Gandhi Post Graduate Institute of Medical Sciences, Lucknow, India. Pancreatic abscess: 10 years experience. ANZ J Surg. 2002 Dec; 72 (12): 881-6. 8. Kune GA, Brough W: Department of Surgery, University of Melbourne, Repatriation General Hospital, Heidelberg, Victoria, Australia. Surgical intervention in severe acute pancreatitis: 476 cases in 20 years. Ann R Coll Surg Engl. 1989 Sep; 71 (5): 338. 9. Ghekiere O, Lesnik A, Hoa D, et al.: Department of Radiology, Centre Hospitalier Universitaire Lapeyronie, Montpellier, France. Value of computed tomography in the diagnosis of the cause of nontraumatic gastrointestinal tract perforation. Chirurgia (Bucur). 2006 Sep-Oct; 101 (5): 523-4.

