© Borgis - New Medicine 3/2012, s. 66-67
Alicja Sapała-Smoczyńska1, *Teresa Jackowska1,2
Accordance of clinical symptoms of OSAS (obstructive sleep apnea syndrome) with polisomnography results
1Department of Pediatrics, Bielanski Hospital, Warsaw
Head of Department: prof. Teresa Jackowska, MD, PhD
2Department of Pediatrics, The Medical Centre of Postgraduate Education, Warsaw
Head of Department: prof. Teresa Jackowska, MD, PhD
Summary
Introduction. OSAS is characterized by symptoms that occur during the day and night, such as snoring, sleep apnea, tiredness, drowsiness and behavioral disorders. A gold standard in diagnosing OSAS is polysomnography.
Aim. This study aims to compare the accordance of suspicion of OSAS posed by primary care physicians based on an interview and a physical examination with polysomnography results.
Material and methods. 66 children (43 males and 23 females), aged from 5 months to 16 years were hospitalized at the Department of Pediatrics (September 2009 to August 2011). Polysomnography was performed in Sleep Lab with the Elmico EEG DiGi Track device, with software extended for PSG.
Results. 24 patients (36%) met the criteria of OSAS. Among the children studied, in 8 (12%) cases we diagnosed a clinically significant central apnea, and in 13 patients (19.6%), the syndrome of an increased airway resistance was found. Altogether, in 45 children (68.2%) abnormalities in the PSG were observed, and in 21 children (31.8%) the examination showed no abnormalities.
Conclusions. A diagnosis of OSAS enables its treatment, and thereby prevents the related diseases and disorders such as hypertension, nocturia, obesity or behavioral disorders. Based on the results, where the compatibility of the symptoms with the results of PSG was observed in 36% cases, we are certain that the benefits of performing PSG for patients are rational, despite the occasional unjustifiable referrals for the test.
INTRODUCTION
Breathing disorders during sleep among children (1), (2), are primarily a problem of snoring children, dominated by patients with hypertrophy of lymphatic tissue of throat. The narrowing of the upper airways associated with hypertrophy may be the cause of snoring as well as pauses in breathing (Obstructive Sleep Apnea, OSA), whose presence in many cases allows the diagnosis of Obstructive Sleep Apnea Syndrome (OSAS).
An untreated OSAS may lead to disturbances in the child’s development and, as in adults, the development of a systemic hypertension and pulmonary hypertension (4), somnolence (5, 6), nocturnal enuresis (7, 8), obesity and the metabolic syndrome related to it (9, 10).
From a clinical perspective, the OSAS is characterized by the presence of day and night symptoms, such as the above mentioned snoring, apnea during sleep, sleepiness, behavioral disorders, hyperactivity and problems with concentration. Depending on the age of the patient, these symptoms may be noticed by the child itself, by the parents or by doctors of the Primary Health Care. In order to clearly explain the cause of the distressing symptoms, General Practitioners (GPs) have the option to refer for polysomnography (PSG), which is the gold standard in the diagnosis of OSAS and other breathing problems during sleep (SBD, Sleep Disorders of Breathing) (11).
The aim of this study was to assess how often the OSAS was diagnosed using PSG among children referred by GPs on the basis of the observed clinical symptoms.
MATERIAL AND METHODS
Polisomnographic studies of 66 patients aged 5 months to 16 years were analyzed (43 boys and 23 girls). Every PSG was performed at the Department of Pediatrics, Bielanski Hospital, Warsaw, in the period between September 2009 to August 2011 (2 years). Every patient was referred for PSG by a GP because of day or night symptoms.
Before the PSG was performed, parents and children were asked to fill a specially prepared questionnaire about the occurrence of night- and daytime symptoms of the OSAS. Questions covered both nocturnal symptoms, such as snoring, waking up, restless sleep, and daytime symptoms, such as learning problems, hyperactivity, inability to focus attention.
Polysomnography lasted all night (on average, 7.2 hours). It was performed at the Sleep Lab with the ELMICO EEG DiGi Track device, with extended software for PSG testing. The diagnosis of the OSAS was made based on the AHI value – apnea/hipopnea index (slightly severe OSAS 1-4, 5-9 medium severe OSAS, ≥ 10 severe OSAS). A detailed analysis of the of the polysomnographic examination results was performed, which confirmed both OSAS and other irregularities. In addition, when children met the criteria for OSAS, we took into account their comorbid conditions and obesity (body mass equal to or greater than the 95th BMI percentile).
RESULTS
Out of 66 children tested, 45 (68.2%) (27 boys and 18 girls) had a clinically significant change in the PSG examination. OSAS was diagnosed in 24 (36.4%) patients (13 boys and 11 girls). Eight patients (12.1%) did not meet the criteria for the OSAS, but in their cases the central sleep apnea syndrome (CSAS, Central Sleep Apnea Syndrome) was diagnosed, whereas thirteen patients (19.7%) had a syndrome of increased resistance in the upper airways (UARS, Upper Airway Resistance Syndrome). In 21 (31.8%) patients no change in the PSG test was observed. Eight (33.3 %) out of the 24 children with OSAS were obese (7 boys and 1 girl) (fig. 1).
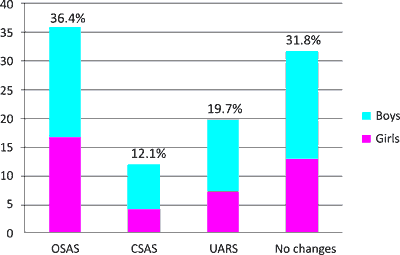
Fig. 1. PSG results in total and by gender.
OSAS – Obturative Sleep Apnea Syndrome
CSAS – Central Sleep Apnea Syndrome
UARS – Upper Airway Resistance Syndrome
According to the surveys, children with the OSAS have more trouble focusing their attention at school (62%), and they subjectively feel much more tired in the morning than children without the OSAS (46%). Other symptoms, such as hyperactive behavior, bedwetting and learning difficulties, were at similar levels in both groups (with and without the OSAS).
DISCUSSION
The OSAS may lead to the development of many disorders and diseases among children and adults. The detection and treatment of the OSAS at the early stages gives the possibility of preventing such diseases as systemic or even pulmonary hypertension.
Our study shows that 1/3 of children with day or night symptoms had actual changes observed in the polysomnography examination that confirmed the OSAS or gave basis for the diagnosis of the CSAS or the UARS. The results confirm the benefits of the PSG examination, even if in 31.8% of cases, no PSG changes were found.
This work also pointed out that among children with a diagnosed OSAS, 33.3% (8/24) were obese. Our results showed that primary care physicians in 68.2% of the children correctly suspected that the symptoms reported by the children or their parents suggest an occurrence of the OSAS or other breathing disorders during sleep.
CONCLUSIONS
1. Accordance of clinical symptoms of the OSAS and the results of the PSG is high enough to recommend all-night polysomnography more frequently to children with the symptoms mentioned above .
2. An early diagnosis of the OSAS and other breathing disorders during sleep gives you more opportunity to treat severe cases, which may significantly affect the child’s development.
3. Polysomnography remains the gold standard in the diagnosis of the OSAS and other breathing disorders during sleep in children.
Piśmiennictwo
1. Gozal D, Capdevila O, Gozal L, Dayyat E: Obstructive Sleep Apnea in Children- Relative Contributions of Body Mass Index and Adenotonsillar Hypertrophy. Chest 2009; 1: 136-137. 2. Leung S, Chung-hong C, Wong J: Ambulatory Blood Pressure Before and After Adenottonsilledectomy in Children with Obstructive Sleep Apnea. Sleep Medicine 2010; 11: 721-725. 3. Leung S, Chung-hong C, Wong J: The Correlation Among Obesity, Apnea-hypopnea Index, and Tonsil Size in Children. Chest 2006; 12: 130-132. 4. Sajkov D, McEvoy RD. Obstructive Sleep Apnea and Pulmonary Hypertension. Progress in Cardiovas Dis 2009; 51: 363-370. 5. Melenders MC, Lutz JM, Rubin ED et al.: Daytime sleeplessness and hyperactivity in children with suspected sleep-disorder breathing. Pediatrics 2004; 114: 768-775. 6. Gozal D, Wang M, Pope DW Jr: Objective sleepiness measures in pediatric obstructive sleep apnea. Pediatrics 2001; 108: 693-697. 7. Brooks LG, Topol HI: Enuresis in children with sleep apnea. J Pediatr 2003; 142: 515-518. 8. Guven A, Giramonti K, Kogan BA: The effect of obesity on treatment efficacy in children with nocturnal enuresis and voiding dysfunction. J Urol. 2007; 178: 1458-1462. 9. Tauman R, O’Brien LM, Ivanenko A et al. : Obesity rather than severity of sleep disordered breathing as the major determinant of insulin resistance and altered lipidemia in snoring children. Pediatrics 2005; 116: e66-e73. 10. Tatsumi K, Saibara T: Effects of obstructive sleep apnea syndrome on hepatic steatosis and nonalcoholic steatohepatitis. Hepatol Res 2005; 33: 100-104. 11. The AASM Manual for the Scoring of Sleep and Associated Events; Rules, Terminology and Technical Specification. American Academy of Sleep Medicine 2007.
