© Borgis - New Medicine 2/2014, s. 63-66
*Tímea Tóth1, Erzsèbet Mák1, Szilvia Molnár1, Magdolna Sinka2, Fruzsina Tóth1, István Szabolcs1
Nutrition status of adult patients with cystic fibrosis
1Department of Dietetics and Nutrition Sciences, Institute of Applied Health Sciences, Faculty of Health Sciences, Semmelweis University, Budapest, Hungary
Head of Department: Katalin Tátrai-Nèmeth, PhD
2Department for Epidemiology, Institute of Health Promotion and Clinical Methodology, Faculty of Health Sciences, Semmelweis University, Budapest, Hungary
Head of Department: István Barcs, PhD
Summary
Introduction. The number of adults with cystic fibrosis (CF) is gradually increasing. The nutritional status has an important role in the progression of the disease.
Aim. To investigate the malnutrition risk and the nutritional status of adults with CF, and to analyse the obtained data according to gender, transplantation, dominantly affected system organ class, comorbidity, bacterial infection and sports habits.
Material and methods. The nutritional status was assessed by a bioelectrical impedance machine, and the malnutrition risk screening was measured by NRS2002.
Results. Forty-four patients participated (20 males, 24 females). Mean BMI in males was significantly higher compared with females (p = 0.01). The mean muscle percentage of patients doing sport regularly was significantly higher than those who do not do sport (p = 0.0126). Between mean body fat percentages there was no significant difference. There was no significant difference in mean BMI and body fat percentage between patients with and without transplantation, patients who live with one dominantly affected system organ class and patients who live with more dominantly affected system organ classes, patients who have concomitant illness and patients who do not, or patients who have one concomitant illness and patients who have more concomitant illnesses. Moreover, there was no significant difference in mean BMI and body fat percentage between patients who suffer from a bacterial infection and who do not, or patients who suffer from one bacterial infection and patients who have several bacterial infections. The majority of those patients who participated in the malnutrition risk screening were malnourished (77.3%).
Conclusions. The research can prove high prevalence of malnutrition among adult patients with CF, which needs nutrition intervention to recover from.
INTRODUCTION
Cystic fibrosis is one of the most common autosomal recessive metabolic disease. The disorder itself occurred by genetic alteration and shows chronic progression with respiratory aberrations, gastrointestinal symptoms as well as reproductive and endocrine system dysfunctions, and leads to early death (1). This genetic disorder inflicts alterations in the functions of exocrine glands, therefore thick, viscous secretions occurred, which can cause obstructive malformations in the concerned organs (2). In Hungary, incidence of CF is about 1:3500 from the data obtained local screenings. In 2012 the mean age of the 579 registered patients was 16.54 years, and 42.8% (248 men) of them were adults (3, 4). Number of patients shows increasing tendency as well as the mean age owing to the improvement of medical treatment and dietotherapy (5). Nutritional status has got crucial role in the progression of CF, thus dietotherapy is the vital part of the treatment (7, 8). Patients with good nutritional status possess better chances to maintain or improve of good health (9), while bad nutritional status decrease the survival chances (10, 11), hence detection of malnutrition, and evolving of an appropriate nutritional status are essential in the optimal therapy (9). Pulmonary infections evoke intensified resting metabolic rate and lack of appetite, but then again serve pulmonary disease can be found more frequently among patients with malnutrition (10). In contrast, patients with higher body mass index possess better lung condition (12). Furthermore it is proved that body weight and BMI correlate positively with Forced Expiratory Volume (FEV1) and Forced Vital Capacity (FVC) (13).
Malnutrition defined as BMI value lower than 18,5 kg/m2, and body fat% < 10% in men, or < 20% in women (8).
BMI and body fat% are accurate indicators of nutritional status of CF patients. BMI can be applied routinely, because of its easy feasibility and accurate results. Body fat% value determinated by measurements of skinfold thickness and BMI often differ lot from the verity, because in the case of thin people it is unreliable, thus in the case of CF, it isn’t a reliable method. Instead of the classical determination, body fat% can be determinated with bioimpedancy based methods at the highest accuracy (1, 5, 8). Laboratory parameters (haemoglobin, white blood cell number, serum albumin, carbamide, and electrolytes) can also serve as good indicators of nutritional status (5). Because of these two parameters accepted internationally as good indicators of malnutrition, data obtained by them can be used for compare results with other studies, where the same methodology was applied, hence evaluation of the data can be easier.
AIMS AND HYPOTHESISES
Aim of our study was to investigate the correlation of nutritional and clinical parameters among adult patients with cystic fibrosis.
We aimed to search for correlations between nutritional status and clinical conditions among woman and man; out- and inpatients; transplanted and non-transplanted; mono or multi organ affected; and patients with or without accompanied diseases and bacterial infections.
We hypothesised that muscle% and body fat% of physically inactive patients and patients who do sports regularly are differ significantly.
We reckoned that results obtained by NRS2002 validated screening method will show that malnutrition will be occurred at higher number than normal nutritional status among the involved subjects.
MATERIAL AND METHODS
Nutritional status analysis was performed with Inbody 170 and Omron BF500 bioimpedancy meters. Clinical status was recorded with interview based on the self-response of patients. Risk assessment of malnutrition was performed by the NRS2002 validated screening method.
Answer to questions was voluntary, thus item numbers at the case of different results might be different.
Student t-test at 5%-significance level (p = 0.05) was used to compare values of the different groups with the Microsoft Excell 2010 software, respectively (14).
RESULTS
Table 1 contains the physical parameters of patients involved to the study.
Table 1. Physical parameters of patients with cystic fibrosis involved to the study.
| | Men (n = 20) | Women (n = 24) |
| Age (year) | 27.6 (max. 65) | 27.83 (max. 47) |
| BMI (kg/m2) | 20.57 | 18.63 |
| | Men (n = 15) | Women (n = 20) |
| Body Fat (%) | 14.91 | 21.01 |
| Muscle (%) | 42.85 | 32.35 |
44 patients with mean age of 27.8 years and, mean BMI of 19.51kg/m2 were participated in the study. Their distribution by the BMI categories shown in figure 1.
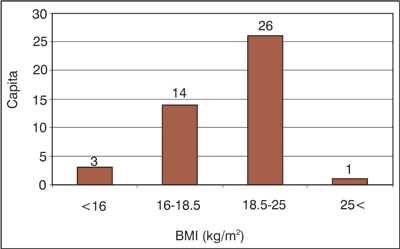
Fig. 1. Patient distribution by BMI categories (n = 44).
BMI means by gender was also different: mean values of men (n = 20) was 20.57 kg/m2 which differed significantly (p = 0.01) from the 18.63 kg/m2 mean value of women (n = 24).
Inpatients (n = 12) had got significantly (p = 0.0114) lower BMI mean(18.05 kg/m2) than outpatients (n = 32, BMI = 20.06 kg/m2). Mean body fat% was not different between them (p = 0.3095): mean of inpatients was 16.38%, while this values was 19.21% among outpatients.
From the investigated subjects, 34 were not transplanted, while 10 people were undergone transplantation surgery (9 lung, 1 liver). BMI mean value of transplanted group was 19.46 kg/m2, while their body fat% was 21.9% (n = 7). Patients without transplantation had got 19.52 kg/m2 BMI mean, and 17.52% body fat% (n = 28). Statistical comparison of these data could not indicate significant difference between groups (BMI p = 0.9406; body fat% p = 0.1009). In the case of comparison of the dominantly pulmonary affected patients (n = 15, BMI = 19.1 kg/m2) with the pulmonary and gastro intestinally affected ones (n = 13, BMI = 19.59 kg/m2), significant differences could not be demonstrated (p = 0.6480).
Body fat% of pulmonary affected patients (n = 15) was 18.29%. It is not different significantly (p = 0.9604) compare to patients affected at both organ systems (n = 9, body fat% = 17.66%).
43.2% (n = 44) of the investigated patients suffered from other diseases (e.g.: diabetes mellitus, Gastroesophageal Reflux Disease (GERD), cirrhosis hepatis, hepato-, splenomegaly) as well, while the remaining patients were not diagnosed with any other pathological disorder than CF yet.
Among patients with co-morbidity 36.85% (n = 19) suffered from more than one additional disorders while 63.2% had got only one additional disease beside CF.
Between the BMI and body fat% values of the two groups, there were no significant differences (p = 0.7458; p = 0.8618). Number of the additional diseases did not affect the BMI, neither the body fat%.
Bacterial infection occurred at 72.3% of the responders, while only 27.7% (n = 30) were free of infection.
Among the infected patients, Pseudomonas aeruginosa, Staphylococcus aureus, or Burkholderia cepacia were the clinically identified pathogens.
CF patients without bacterial infection (n = 8) had got BMI mean value of 19.05 kg/m2, and body fat% = 14.61% (n = 7). In the group of infected patients BMI value was 19.44 kg/m2 (n = 22) and body fat% of 18.55% (n = 19). None of these values were differ significantly (p = 0.8411, p = 0.2166).
37.5% of the responders did sports regularly (at least 3 times per week), while 62.5% did casually, or they were physically inactive.
Although body fat% were not differ considerably, muscle percentage were significantly higher (n = 11, muscle% = 41.59, p = 0.0126) compare to inactive group (n = 20, muscle% = 34.06).
Malnutrition risk assessment tests were appreciable in the case of 22 patient. Results showed that 77.3% were suffered from malnutrition, and only 22.7% could characterised with normal nutritional status.
CONCLUSIONs
Literature contains data about similar BMI values between genders (8), as well as significant differences (15). In our current study, mean value of men was significantly higher than in the case of woman patients.
Because of patients with CF usually hospitalized the purpose of antibiotic therapy or bad healthy condition, it was predictable that inpatients will be characterised with worse nutritional status. Our results could fortified that, because outpatients had got significantly higher body mass index. In the case of body fat%, there were no such difference measured.
Studies of Kalnins and Hollander emphasised that nutritional status of patients waiting for transplantation surgery worse compared to transplanted subjects (16, 17). When they compared the status of transplanted and non- transplanted patients, significant differences could not be demonstrated (18).
In our study we did not investigate the patients who have been waiting for transplantation, but we assessed the value of already transplanted, and the patients who do not require this kind of treatment. In this classification we could not demonstrate differences between groups. Researches of Kalnins & Wilschanski on the nutritional status of patients with CF and diabetes mellitus as co-morbidity highlights that in the case of appropriate nutritional education no differences can be found in nutritional status (16).
In many cases patients with CF cannot provide the necessary energy intake due to many factors, such as co-morbidities, which are getting more and more frequent as the population of CF patients getting older (15). Distal Intestinal Obstruction Syndrome (DIOS), Gastroesophageal Reflux Disease (GERD), and hepato-, splenomegaly all can lead to decreased energy intake (18), furthermore cough and vomiting also badly influence appetite, thus we can hypothesise that CF patients with additional disorders possess worse nutritional status. We could not verify this phenomenon, because neither BMI nor body fat% differ significantly between patients without additional diseases and the group of co-morbidity.
About the bacterial infection of chest, Bell and co-workers found that differences can be detected only in lung function compare to patients without infection (13). Our results are in line with this observation, because we could not demonstrate significant differences in BMI, and body fat% between infected and uninfected group. One of the possible reasons behind this is the low number of uninfected cases, which is due to the increasing prevalence of infection as the age increasing.
Relevance of the results of muscle percentage is high for the purpose of deceleration of progression, because the gained muscle mass positively affects the lung muscle efficiency, which helps to maintain or perhaps improve the lung function.
Until now, only limited information were available about the Hungarian CF patient population.
Our results showed that prevalence of malnutrition in the Hungarian CF population high, just as in case of patients from other countries.
This draws the attention of health professions to the need of nutritional status restore in CF.
Because of these, one of our aim in the future is to prevent malnutrition, and restore the normal nutritional status of the already malnutrition cystic fibrosis patients with appropriate dietotherapy.
Women patients require special attention due to their worse nutritional status compare to men. It is similar to the case of in- and outpatients, where inpatients need extra care from the medical team. These reasons emphasised the meaning of feeding, and hipercalorisation, especially when the patient await for transplantation, as good nutrition status is a criteria for the surgery.
Of course, after transplantation the maintain of the nutritional status has got important role as well for the fast recovery.
Our further results can stimulate patients for regular sport activity to achieve higher muscle mass, thus achieve better health status, and longer period of good quality of life, hopefully.
Nutritional status affects the general condition of CF patients, and better nutritional status leads to slower progression, less breathing symptoms and chest infections (19). It is a vice versa situation, since frequent infections and gastrointestinal symptoms worsens the nutritional status, hence we can state that clinical and nutritional status correlate well.
Malnutrition leads to worse lung function, life quality, and life-span, so settlement of nutritional status is vital to proper therapy of CF. It can be achieved by dietotherapy and enzyme supplementation.
The success of this attempt lead to the deceleration of pulmonary status progression which is the main cause of early death of patients.
Piśmiennictwo
1. Madarasi A: A táplálkozás jelentősège a mucoviscidosis kórlefolyásában. Doktori (PhD) èrtekezès, Semmelweis Egyetem Doktori Iskola 2000. 2. Gyurkovics K: Cystás Fibrosis (mucoviscidosis). Budapest, Medicina Könyvkiadó 1991. 3. Holics K: CF-könyv szülőknek ès fiataloknak (cystás fibrosis). Semmelweis Kiadó, Budapest 2012. 4. Hornyák A, Marsal G: CF-regiszter 2012. Magyar Cisztás Fibrózis regiszter beszámolója Power Point előadás Cisztás fibrózis szülői találkozó, Csillebèrc 2014.05.17. 5. Sinaasappel M, Stern M, Littlewood J et al.: Nutrition in patients with cystic fibrosis: a European Consensus. Journal of Cystic Fibrosis 2002; 1: 51-52. 6. Schöni MH, Casaulta-Aebischer C: Nutrition and lung function in cystic fibrosis patients: review. Clinical Nutrition 2000; 19(2): 79-85. 7. Hollander FM, De Roos NM, De Vries JHM, Van Berkhout FT: Assessment of Nutritional Status in Adult Patients with Cystic Fibrosis: Whole-Body Bioimpedance vs Body Mass Index, Skinfolds, and Leg-to-Leg Bioimpedance. Journal of the American Dietetic Association 2005; 105(4): 549-555. 8. Gordon CM, Anderson EJ, Herlyn K et al.: Nutrient Status of Adults with Cystic Fibrosis. Journal of the American Dietetic Association 2007; 107(12): 2114-2119. 9. Abbott J, Morton AM, Musson H et al.: Nutritional status, perceived body image and eating behaviours in adults with cystic fibrosis. Clinical Nutrition 2007; 26: 91-99. 10. Richardson I, Nyulasi I, Cameron K et al.: Nutritional Status of an Adult Cystic Fibrosis Population. Nutrition 2000; 16: 255-259. Retrieved from http://www.sciencedirect.com. 11. Stallings VA, Stark LJ, Robinson KA et al.: Evidence-Based Practice Recommendations for Nutrition-Related Management of Children and Adults with Cystic Fibrosis and Pancreatic Insufficiency: Results of a Systematic Review. Journal of the American Dietetic Association 2008; 108(5): 832-839. 12. Bell SC, Bowerman AR, Davies CA et al.: Nutrition in adults with cystic fibrosis. Clinical Nutrition 1998; 17(5): 211-212. 13. King S, Sekuloska Z, Gallo R et al.: Changes in the Nutritional Status of Victorian Adults with Cystic Fibrosis since 1997: Improvements in Males but not Females. AuSpen Conference, Sydney 2013. 14. Pakai A, Kívès Zs: Kutatásról ápolóknak. Mintavètel ès adatgyűjtèsi módszerek az egèszsègtudományi kutatásokban. Nővèr, 2013; 26/3: 20-43. 15. Kalnins D, Pencharz PB, Grasemann H, Solomon M: Energy Expenditure and Nutritional Status in Pediatric Patients before and after Lung Transplantation. The Journal of Pediatrics 2013; 163: 1500-1502. 16. Hollander FM, Van Pierre DD, De Roos NM, Van de Graaf, EA, Iestra JA: Effects of nutritional status and dietetic interventions on survival in Cystic Fibrosis patients before and after lung transplantation. Journal of Cystic Fibrosis 2013; Advance online publication. 17. Witters P, Dupont L, Vermeulen F et al.: Lung transplantation in cysticfibrosis normalizes essential fatty acid profiles. Journal of Cystic Fibrosis 2012, 12: 222-228. 18. Robinson P: Nutritional status and requirements in cystic fibrosis. Clinical Nutrition 2001; 20(1): 81-86. 19. Sabolová G:. Nutrition of children and adults with cystic fibrosis. Slovak Cystic fibrosis Association 2010.
