© Borgis - New Medicine 2/2014, s. 67-71
*Veronika Rajki1, 2, Henriett Hirdi1, Judit Mèszáros3
Specifics of the nursing care of patients undergoing skin grafting, particularly the aspects of transfusiology
1PhD student, Doctoral School, Semmelweis University, Budapest, Hungary
2Faculty of Health Sciences, Institute of Applied Health Sciences, Semmelweis University, Budapest, Hungary
Head of Faculty: prof. Zoltán Zsolt Nagy, PhD
3Semmelweis University Faculty of Health Sciences
Head of Faculty: prof. dr. Zoltan Nagy
Summary
Aim. The authors’ aim was to collect experiences and most recent knowledge in nursing of burned patients around skin transplantation and to compare them with former experiences and knowledge on the same hospital ward and also with the professional materials.
Material and methods. One of the authors spent some weeks in a County Teaching Hospital, in Western Hungary with the aim of collecting experiences about the recent nursing practice of burned patients before and after skin transplantation. We used documentation analysis, observation and evaluation of completed nursing tasks.
Results. The authors got a lot of information in connection with the local practical routine in the following themes: pain-killing after skin grafting, wound care after skin grafting, artificial feeding of the patients after skin transplantation, the indication and application of transfusion in the care of patients after burn, and other aspects of routine nursing care.
Conclusions. The authors found deficiencies in writing the nursing care plan. Our experiences prove that the quality of patients’ care is excellent but there are some deficiencies in recording the nursing care plan. In this hospital field the results of the medical and nursing activities among burned patients are excellent. The authors hope that this institute visit may improve the whole of the nursing education.
INTRODUCTION
Annually lots of people are injured in burning in Hungary. Both adults and children are affected. Among 100 000 people there are approximatelly 1-1.5 fatal cases, 11-13 cases with hospital admission and 40-50 cases which need out-patient care if we see the statistical data of child injuries (data from 2005) (5.)
Children under 5 and adults over 65 years are mainly affected in this kind of injury. The causes of the burns frequency of these two age groups are the following: the possibility of their escape is limited and they can’t realize the danger properly.
In the whole population men are injured in burns more often (their ratio is 70%), but the mortality rate of women is the double of men’s.
Nowadays the care of burns with bigger surface is also successful as the result of the changes in the attitude towards burn care in the last 2.5 decades. Burn Centers have been established all around the world, and in Hungary as well, where the medical stuff are very well skilled in the care of burn injuries. Most of the Burn and Plastic Surgery Wards have already started their own intensive care departments for the care of the severely injured patients. The number of beds in these department amount to the 15-30% of the total number of hospital beds of the whole ward (5).
The incidence and the most frequent causes of the burn injuries among children and adults
1. Sunburn: There are no exact statistic data about its incidence, because only the severest cases of sunburn are cared by medical staff.
2. Scald: (60-70%). This is the most frequent type, the role of the parents and educational experts are very important in its prevention.
3. Flameburns: (15-20%). It’s a kind of severe burn injury after short contact with very high temperature. The burn of the respiartory tract is also accompanying with it. During the inhalation of the flame the respiratory tract is also injured just like the skin. In the case of flameburns of the face the eyes can also suffer.
4. Electrical burns: (2.5-3%). Externally the alteration is slight, but internally the necrosis of blood vessels, muscles, tendons, and bones can occur. Electric burn is an indication for surgery/skin grafting, sometimes care in ICU is necessary.
5. Contact burns: (2-5%). In childhood this type of burns is a very common form of injury at home after direct contact with a hot machine, a heater or other hot things. In the significant proportion of cases the damage is on the palms and soles of the feet, it often occurs in the form of deeply penetrating injury.
6. Chemical burns (1-2%). These are damage induced by acidic or alkaline agents. The surface of acidic burn injuries can slough quickly, the alkaline burn injuries penetrate increasingly deeper and deeper into the tissue owing to the affected tissue liquefaction. A corrosive substances in eyes can cause severe corneal injuries (5).
Before skin transplantation the selection of the donor place is needed. Semi-thick skin graft means: 0.25 to 0.5 mm or 0.55 to 0.75 mm, and full-thickness skin graft means: 0.8 to 1.1 mm. Free transposition of skin is applied. The highest risk of the freely transplanted skin is hematoma, this hinders revascularization. For its prevention the frequent perforation and sewing under the strain is recommended → the blood can flow through the dilated gaps.
Before incision lubrication of the donor area with vaseline is required. The lower surface of the blade should be lubricated with lubricant too. When simple skin piercing equipment is used, the area of donor skin must be stretched. The graft is placed onto the recipient location. Mesh-grafting: This is the procedure of Vandeput and Tanner from 1967. The skin graft is meshed with the Mesh graft dermatome, so the surface of the piece of skin can be enlarged threefold. The well prepared wound surface can be epithelialising within 7-15 days (1).
| | Number of beds | ICU beds | Resp | Fluid | Physician (e.g. specialist) | Health care | ADM (1999)
Tot/Bpts | OP (1999)
Tot/Bpts | ADM (2000)
Tot/Bpts | OP (2000)
Tot/Bpts | ADM (2001)
Tot/Bpts | OP (2001)
Tot/Bpts | ADM (2002) Tot/Bpts | OP (2002)
Tot/Bpts | ADM (2003) Tot/Bpts | OP (2003)
Tot/Bpts | Chief physician directing the department |
| Szent István Hospital Dept. of Burn and Plastic Surgery | 31 | 4 | 4 | 3 | 7 plastic surgeon
+ 2 anaesthesiologists | 39 | 770/ 341 | 1435/ 443 | 942/ 392 | 1569/ 473 | 837/ 364 | 1659/ 394 | 839/ 338 | 1531/ 563 | 888/ 315 | 1747/ 437 | Dr. GáMonbor Mèszáros (2001-) |
| Central Army Hospital, Dept of Burns | 10 | 2 | 2 | 2 | 6 surgeons (3 plastic surgeons) | | 155/
155 | 422/ 422 | 164 | 450/ 280 | 85 | 464/ 195 | 142 | 520/ 320 | | | Dr. András Szűcs
(1989- ) |
| Szent János Hospital, Burn Unit of the Dept. of Ped. Surg. | 6 | Avail.at Cent. ICU | Avail. At Cent. ICU | 3 + 2 pneumatic | 4 peg. surgeons (3 plastic surgeon. 1 resident) | 9 | X/ 64 | X/ 143 + 145rec | X/ 85 | X /145 | X/ 93 | X/ 160 | X /53 | X/ 94 | X/57 | X/154 | Dr. Sándor Győri
(2001-) |
| Univ. of Pècs, Burn and Plast. Surg. Dept. | 16 | 2 + Cent. ICU | Cent. ICU | 2 | 5 surgeons (3 plastic surgeonr) | 18 | 477/ 165 | 720/ 180 | 395/ 184 | 868/ 122 | 307/ 147 | 782/ 106 | 312/ 163 | 655/ 114 | X/131 | 543/ 305 | |
| Petz A. Hosp. Győr Dept. of Burn and Plast Surg. | 19 | 3 | 1 | 2 | 4 surgeons (2 plastic surgeons, 1 traumatol.) | 26 | 314/ 228 | 842/ 303 | 335/ 234 | 737/ 316 | 401/ 232 | 858/ 354 | 366/ 227 | 1056/ 346 | 295/ 201 | 1104/ 276 | Dr. Pèter Jakabos
(1994-) |
| Univ. of Szeged, Dept of Derm. Burn and Plastic Surgery Unit | 20 | 1 | 1 | 1 | 4 plastic surgeons | 18 | 743/ 76 | 685/ 107 | 827/ 80 | 817/ 105 | 823/ 59 | 3149/ 101 | 737/ 85 | 893/ 103 | 895/ 101 | 993/ 113 | Dr. Klára Kapitány (1995-) |
| Univ of Debrecen, Dept of Derm. Burn and Derm. surgery Unit | 28 | 4 | 1 | 2 | 2 surgeons (1 plastic surgeon) 1 int-anest, 1 surgeon in training for board exam | 18 | 1187 /295 | 2120 /211 | 1352 /237 | 2294 /186 | 1455 /260 | 2420 /209 | 1395 /251 | 2299 /178 | 1356/ 209 | 2461/ 176 | Dr. István Juhász
(1995-) |
| Miskolc,Dept. of Traumatology, Burn Unit | 16 | 4 | 1 | 1 | 1 surgeon | 9 | 101/ 80 | 216/ 83 | 189/ 102 | 172/ 148 | 197/ 132 | 178/ 151 | 173/ 115 | 181/ 151 | | | Dr. Sarolta Tarr
(1989-) |
| Miskolc, Dept. of Pediatric, Surg. Burn Unit | 8 | Cent. ICU | Cent.ICU | 0 | 1 plastic surgeon + rotation system ped. Surgeons + 3 surgeons in training for board exam | 11 | 101 /80 | 71 /55 | X/ 109 | X/ 113 | X/ 108 | X/ 83 | X/ 114 | X/ 91 | 223/ 103 | 201/ 107 | Dr. Rózsa Papp
(1990-) |
| Bethesda Hospital National Center for Children with Burn Inj. | 6 | 4 | 4 | 1 | 2 surgeons (2 plastic surgeons) | 9 | The Department started its work in April 2002. | 122/ 83 | X/ 77 | 276/ 135 | 268/ 171 | Dr. Éva Csorba |
Fig. 1. Presents the situation of burn centers in Hungary in 2004. These figures are reported by the respective departments.
Tot: Total number of patients/year; Bpts: patient with burn injuries; Adm: Number of Admission/year; Op: Number of operations/year
AIM
Knowing the nurse education, the themes of nursing research, and reading the nursing literature it can be stated that the discussion of skin transplantation from the aspect of its nursing care is undeservedly rare. Mainly the medical relations of burns are known and can be read about. That’s why we think that it is important to deal with this theme in order to improve the quality of higher level nursing education.
During this research our aim was to collect experiences and most recent knowledge in nursing of burned patients before and after skin transplantation. We wanted to compare them with our former experiences and knowledge in this field of nursing.
MATERIAL AND METHODS
In the summer of 2011 one of the authors spent some weeks in a County Teaching Hospital, in Western Hungary. She gained experiences in the Burn and Plastic Surgery Ward. This hospital ward has 19 beds, 3 of them are for intensive care.
As data collection methods we used documentation analysis, observation and evaluation of implemented tasks. In this article we use our results without detailing the personal data of the patients.
RESULTS
Pain-killing after skin grafting
Verbal pain measurement scale is used as the part of nursing documentation.
Assessment of pain should include the followings:
– location of pain,
– nature of pain,
– length of the pain period,
– frequency of pain.
Presence of pain:
– in movement,
– under loading,
– at rest.
In pain management a medicine, called Tramadol is used as a well-tried medication.
Wound care after skin grafting
The following products are used in wound treatment with different indications:
– ALSOL – ung. alum. acetatum,
– silver sulfamidichum,
– mixture of Betadine and Gentamicine ointment,
– H2O2 (Hyperol),
– 0,5% hexochlorophen solution,
– 70% alcohol,
– octenisept,
– inadine,
– mercurochrom solution,
– suprasorb.
The shaving of the body hair on the donor area is required. Betadine „soaked” gauzes are wrapped around the limbs on the day of the operation/transplantation. The aim is the gauzes not to get stuck into the wound.
The bandage over donor area is changed the next day (1st postoperative day), and the bandage over the area of skin grafting is changed on the second postoperative day. Until that day the nurses wrap gauze pads with silver sulfamidichum around the area. During wound dressing, wound treatment they never use latex-based gloves, they use „Nitril” gloves instead of it, with their material the components of the ointments are neutral.
Artificial feeding of the patients after skin transplantation
The burned patients eat 5 times a day, they must drink 2.5 liters of fluid enterally per day. Liquid brought by family members can be consumed on the ward (carbonated, sugary drinks are not recommended). Salt intake should be monitored, supplement may be necessary. 120 grams protein/day is necessary for them. Among the vitamins, vitamin B and C intake must be increased, these are important.
Parts of parenteral nutrition:
– 20% fat,
– 10% amino acid,
– 40% carbohydrate,
– 10% fructose,
– 10% glucose,
– ringer-laktate (up to 4000 ml daily at the first day!),
– trace elements and fat-soluble vitamins.
Specifics of tube feeding:
Nutrition formulas are compiled by the dietitian (in the hospital kitchen). Original nutrition formulas are also given to the patients:
– nutridrink,
– ensure,
– reconvan,
– dipeptiven (this is very important because of the glutamine content).
Nurses use continuous tube feeding with gravity tube feeding bag, or nurses administer formulas through a pump (with 50 ml/h, or 80 ml/h flow rate).
Patients receive the formulas (factory formulas as well) in diluted form. For dilution the nurses use bitter tea (to avoid diarrhea). Bitter tea is also used to flush the feeding tube. Tap water is not suitable for dilution, because pseudomonas lives in the water pipes. Nutrition calorie value of 1.00 to 1.5 cal/ml are compiled by the dietitian in the kitchen.
The indication and application of transfusion in the care of patients after burn
In this hospital the online ordering of the blood products is current, with using a special computer program, according to EU standards. Only selected blood may be given for polytransfused patients. Before ordering a blood transfusion results of antibody screening not older than 3 months are needed. From the patients who require long-term care, they collect blood for antibody screening in every 3 months, because their condition may vary due to the repeated transfusions.
The blood can be transported by the medical professionals from the Hospital Blood Transfusion Service to the hospital ward. The unused blood can only be sent to the Hospital Blood Transfusion Service back if the packaging is intact, and if it is transported in chilled condition and it is also kept chilled. The „cold chain” must not be broken! Blood warmer machine is not used here, they heat the blood products up with hot running water. In general refrigerated products are used, only the plasma is a frozen blood product.
Determinants of burned patients’ transfusion indications:
– recent laboratory results (preoperative results are better than postoperative results, due to the possible deepening of the burn, and the blood loss!),
– affected area, the expected rate of blood loss,
– hematocrit level less than 0.30 (in non burned patients the indication of the transfusion is typical when hematocrit level is less than 0.24).
In most recent cases there happens „over ordering” (for example: 6 units of blood product are ordered, and it is given in fraction to the patient. In the evening of operation the doctor’s order depends on the laboratory results – when and how many (more) units of blood will be necessary for the patient. There are labolatory tests two times on the day of the operation. The first is before the surgery, and the second one is in the evening. Otherwise there is lab control once a day (in the case of burn patients, the ions are the most important, not the qualitative-quantitative blood count). After the transfusion therapy the equipments are stored in the fridge for 48 hours. Whole blood is not ordered and is not provided to the burned patients.
The types of the ordered blood products are as follows:
– fresh frozen plasma,
– platelet suspension,
– 20% human albumin,
– RBC concentrate.
A full lab test follows the transfusion therapy. The urine test is also included in the laboratory test! Blood selection is widespread in practice. The selected blood administration is safer if the patients get 3 units, or more than 3 units of blood. Usually they need 10 ml of native blood in tube, if the patients get at least 3 units of blood. In this case 10 ml is needed, 7 ml of blood sample is not enough! This blood sample is sent to the laboratory. Citrated tube is necessary for bedside blood grouping. If it is certain that the patient will need blood donation, transfusion anamnesis is included in the medical history (it has got special document). The patient’s name (and their other data) must be written on the bag of blood products before administration. If they use more than one bags, the patient’s name shall be written on each bag! It’s possible to use the medical labels.
Some other aspects of routine nursing care
The oral care and the nail care happen with disinfected instruments. In-patients can’t use their own textiles (nightgown, pyjamas, bathrobe) in the department. Patients are not allowed to leave the ward, and no other patient can come to visit this unit. Children under six and pregnant mothers can’t come to visit the burned patient. Visiting hours are between 14:00 to 18:00 pm! It is very important to strictly enforce it.
Burned children are located in the ICU or in the children surgery, but they change the wound dressings on this ward.
They use therapeutic bathing after admission, nothing else. Patients are bathed in the bath (over bath), using patient lifting device (fig. 2) and antiseptic solutions.

Fig. 2. Patient lifting device.
Cryogel cooling is carried out, cryogel bags are wrapped in textiles.
LMWH therapy is used for preventive purpose, in the case of lower risk 0.4 Clexane is given to the patients, and at higher risk the patients get Clexane 0.6 for some days. Quamatel therapy is used for ulcer prophylaxis with different doses (tablets or parenteral intake). At low risk the patients receive Aspirin.
They write the nursing care plan only on the day of admission, the plans are evaluated when the patients leave the ward. Guided, written materials are used for the formulation of nursing diagnoses.
As special equipment, the Fluidized bed (fig. 3, 4) is used in the care of burned patients.
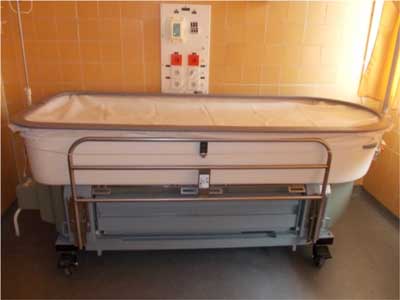
Fig. 3. Fluidized bed.

Fig. 4. Fluidized bed
Tetanus prophylaxis is used when it is necessary. Dietitians use NutriComp 3.0 program for planning the diet for the patients. The protein need of burned patients is changing, usually 120 grams of protein per day is required.
7 nursing care protocols are available for different specific nursing activities on this hospital ward:
– nursing care of the burned patient with burns of the body surface area less than 10% related,
– burned patient’s surgical preparation,
– face and neck burned patient’s care,
– nursing care of the burned patient with burns of the body surface area more than 10% related (intensive care),
– protocol of the admission of new patients,
– protocol of exchange of wound dressing,
– reconstructive surgery patient’s care.
DISCUSSION AND CONCLUSIONS
Regarding to the literature (2-5) it can be said that the quality of the patient’s care is excellent on this ward. Deficiencies in writing the nursing care plan are what can be mentioned as a drawback. The nursing activities, the patients „route” in the health care system meet the protocol requirements and the rules of the medical and nursing profession. The results of their medical, nursing activities among burned patients are excellent. We are sure that this institute visit improves the whole of our nursing education of BSc. nurses.
We used our own photos for this publication. We would like to thank the whole staff of the Burn and Plastic Surgery Ward for allowing the present research to be carried out.
Piśmiennictwo
1. Zoltán J: A bőrátültetès atlasza. Medicina Könyvkiadó, Budapest, 1984. 2. Az Egèszsègügyi Minisztèrium szakmai protokollja az ègèsi sèrültek ellátásáról 3. Bosworth Ch: Burns trauma: Nursing procedures. Whurr Publishers, London, 1999. 4. Berzènè VA, Rostásnè BT, Mersánynè GE: A transzfúziós ès infúziós tevèkenysèg ápolói vonatkozásai a Közèp-magyarországi Règió fekvőbeteg ellátásában. Nővèr, Budapest, 2007: 11-18. 5. Csorba Éva: A gyermekkori ès fiatalkori ègèsek kezelèsi stratègiája. Magyar Orvos 2005; 13(2): 43-46. 6. The present situation of burn centers (2004). www.doki.net/tarsasag/upload/egesi/document/2004angs.doc.


