© Borgis - New Medicine 3/2014, s. 83-85
*Konrad Wroński1, 2, Maciej Biernacki2, 3, Andrzej Lachowski2
Giant simple non-parasitic hepatic cyst – case report and review of literature
1Department of Oncology, Faculty of Medicine, University of Warmia and Mazury, Olsztyn, Poland
Head of Department: prof Sergiusz Nawrocki, MD, PhD
2Department of Surgical Oncology, Hospital Ministry of Internal Affairs with Warmia and Mazury Oncology Centre, Olsztyn, Poland
Head of Department: Andrzej Lachowski, MD
3Department of General Surgery, Hospital Ministry of Internal Affairs with Warmia and Mazury Oncology Centre, Olsztyn, Poland
Head of Department: prof. Jadwiga Snarska, MD, PhD
Summary
Giant simple hepatic cysts are observed in less than 5% of the general population. Cysts are usually seen in patients older than 40 years old, but giant cysts are diagnosed in patients older than 50 years old. Hepatic cysts are more commonly diagnosed in females than in males (49:8). There are observes more often in the right lobe of the liver. Most of the simple hepatic cysts are asymptomatic and do not indicate abnormal liver function. The authors of this article presented a case of a woman who was admitted to the hospital because of giant simple hepatic cyst. The patient was suffering for abdominal pain for two years. She underwent surgical operation and left the ward in the 5th day after surgery. After operation the symptoms of disease were alleviated. The authors performed a literature review on giant hepatic cysts.
INTRODUCTION
Giant non-parasitic simple hepatic cysts are observed in less than 5% of the general population (1). Cysts are usually seen in patients older than 40 years old, but giant cysts are diagnosed in patients older than 50 years old (2). Hepatic cysts are more commonly diagnosed in females than in males (49:8) (3). There are observes more often in the right lobe of the liver (3). Most of the simple hepatic cysts are asymptomatic and do not indicate abnormal liver function (4).
CASE REPORT
A 73-year-old white lady, Caucasian race, referred to the Department of Surgical Oncology due to diagnosed in computer tomography giant simple hepatic cyst. The patient has reported pain in the right hypochondrium region for two years. She had no any other symptoms, drug abuse and there was no history of weight loss and loss of appetite. She had cholecystectomy in early 90’s XX century. There was no history of carcinoma in patient family.
On physical examination, in the right hypochondrium patient reported pain. There were no peritoneal symptoms. Blood tests were normal and indicators of liver function was with normal limits. There was no histopathology examination of the fine-needle aspiration biopsy before planned surgery.
Abdominal CT image shows giant simple hepatic cyst diameter 110 x 74 x 120 millimeters (fig. 1). CT image shows a solitary, thin walled, cystic lesion located in area were was located gallbladder and in 4th liver segment. Hepatic cyst modeled adjacent vessels and oppressed for extended piecewise around changing the bile ways. Common bile duct was not extended.
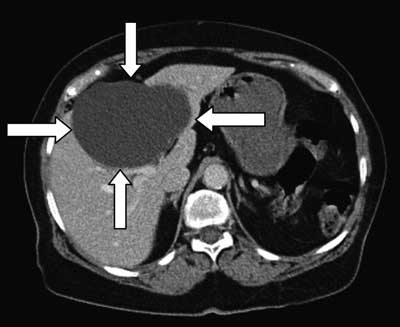
Fig. 1. Abdominal CT image shows giant simple hepatic cyst diameter 110 x 74 x 120 millimeters. CT image in axial view shows a solitary, thin walled, cystic lesion located in area were was located gallbladder and in 4th liver segment.
The patient was taken to the operating room for partial excision of the giant hepatic cyst. After entering the abdominal wall a giant hepatic cyst was opened (fig. 2, 3). About 3 liters of serous fluid was aspirated and 80% of the cyst wall was removed. The material was sent for routine histopathology examination. The time of surgery was about 60 minutes.
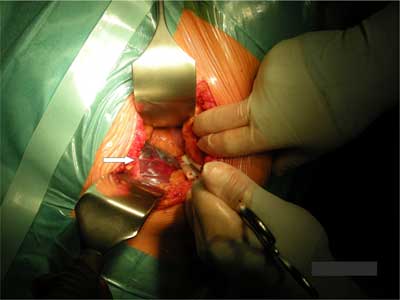
Fig. 2. Thin wall of giant simple hepatic cyst.
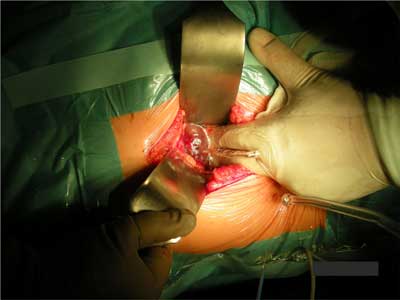
Fig. 3. Aspiration of serous cystic fluid during an open surgery.
Histopathology examination showed no neoplasm component in the hepatic cyst wall. Patient after surgery felt good and did not complain of pain. After operation the symptoms of disease were alleviated. The postoperative period was uncomplicated and the patient left the ward in the 5th day after surgery.
DISCUSSION
Cyst formation may occur in ductal organs, particulary in the kidney but also in the liver, pancreas, ovary, spleen and central nervous system (1, 3). Hepatic cysts are divided into two categories: non-parasitic and parasitic (5). Non-parasitic hepatic cysts are the most frequent and are divided into simple an polycystic. Parasitic cysts are most commonly observed in endemic areas such as Mediterranean region, Australia and south Africa (5).
It is estimated that 5 to 15% of patients with hepatic cysts have symptoms related to the mass (1-4). Patients suffer from abdominal fullness, heartburn, change in bowel movements, swelling and continuous abdominal pain (2, 3). Liver cyst can be infected and patients can present fever and right upper quadrant tenderness (2, 4). Pyogenic liver abscess has polymicrobial etiology in 20 to 50% of cases (6). The most common microorganism which are observed in infected liver cysts are: Escherichia coli, Klebsiella pneumonia, Proteus spp., Pseudomonas spp., Streptococci and Enterococci (6). Rupture of pyogenic liver abscess into the abdominal cavity causes acute peritonitis and complications in many cases (6).
Most of hepatic cysts are diagnosed incidentally during sonogram examination (1). Typical radiological findings are very helpful in hepatic cyst diagnosis. US is the first diagnostic technique and usually confirmed by CT and MRI. In CT scans there are seen calcifications of the cyst wall or internal septa (1-3). However, MRI is more accurate in demonstrating parietal features and anatomical relationships nearby cyst wall (2-4).
Treatment of giant simple hepatic cyst is still controversial. Treatment is necessary when the cyst is very large and there are present signs of infection, rupture, biliary compression or cystic neoplasm (7). There are many options of liver cyst treatment such as: simple needle aspiration, aspiration with sclerotherapy, radiofrequency ablation, internal drainage, marsupialisation, laparoscopic or open surgery, complete excision and liver resection (8). Simple needle aspiration is associated with 100% recurrence rate. Aspiration with sclerotherapy is effective procedure with success rate of 70-90% and a recurrence rate less than 17% (5). Laparoscopic treatment is successful in 75-100% and recurrence rate less than 17% (1). Superior or posteriorly located cysts (segments: I, VII, VIII and the superior part of IV) are unsuitable for laparoscopic procedure (9). Cysts located in the anterolateral segments of the liver (segments: II, III, V, VI and the inferior part of IV) are considered good for laparoscopic resection (10,11). Surgical complications after laparoscopy occur in less than 15% procedures and include shoulder pain, haemorrhage, pleural effusion, infection and subhepatic bile collection (1, 5). The cyst wall consists irregularities must be examined intraoperatively due to indication cystadenoma or cystadenocarcinoma cells. In such case surgical team must remove whole cyst wall.
Liver cysts need to differentiate from polycystic liver disease, hydatid cyst, hepatobiliary cystadenoma and hepatobiliary cystadenocarcinoma.
CONCLUSIONS
1. Giant simple hepatic cysts are rare disease and are more often in female population.
2. Most hepatic cysts are asymptomatic and do not indicate abnormal liver function.
3. Simple hepatic cysts are diagnosed incidentally on sonogram examination and confirmed by CT or MRI images.
4. Radical surgical resection is the best treatment option.
Piśmiennictwo
1. Nagorney DM, Sarmiento JM: Surgical management of cystic disease of the liver. Surgery of the liver, biliary tract and pancreas. Philadelphia, PA: Saunders Elsevier 2007: 1021-1031. 2. Farges O, Vilgrain V: Non-parasitic cystic diseases of the liver and intrahepatic biliary tree. Surgery of the liver, biliary tract and pancreas. Philadelphia, PA: Saunders Elsevier 2007: 1005-1020. 3. Regev A, Reddy KR, Berho M et al.: Large cystic lesions of the liver in adults: a 15-year experience in a tertiary center. J Am Coll Surg 2001; 193: 36-45. 4. Sanders DM 2nd, Garrett JM: Solitary hepatic cysts: case reports. South Med J 1968; 61: 256-261. 5. Lalezari S, Coates M, Sorour N: A 77-year-old female with a giant hepatic cyst. BMJ Case Reports 2012; doi:10.1136/bcr.05.2011.4218. 6. Chan KS, Chen CM, Cheng KC et al.: Pyogenic liver abscess: a retrospective analysis of 107 patients during a 3-year period. Jap J Infect Dis 2005; 58(6): 366-368. 7. Becker S: Cysts of the liver. [In:] Bockus Gastroenterology, ed. Berk JE, W.B. Saunders, Philadelphia, pp 3278-3287. 8. Lin TY, Chen CC, Wang SM: Treatment of non-parasitic cystic disease of the liver: a new approach to therapy with polycystic liver. Ann Surg 1968; 168: 921-927. 9. Gagner M, Rogula T, Selzer D: Laparoscopic liver resection: benefits and controversies. Surg Clin North Am 2004; 84: 451-462. 10. Gigot JF, Glineur D, Santiago Azgra J et al.: Laparoscopic liver resection for malignant liver tumors: preliminary results of a multicenter European study. Ann Surg 2002; 236: 90-97. 11. Cherqui D, Husson E, Hammoud R et al.: Laparoscopic liver resections: a feasibility study in 30 patients. Ann Surg 2000; 232: 753-762.


