© Borgis - Postępy Nauk Medycznych 2/2015, s. 108-116
*Anna Drelich-Zbroja1, Tomasz Jargiełło1, Elżbieta Czekajska-Chehab2, Monika Miazga1, Michał Sojka1, Anna Szymańska1, Krzysztof Pyra1, Klaudia Karska1, Małgorzata Szczerbo-Trojanowska1
Czy TK jest nadal metodą monitorowania chorych po wewnątrznaczyniowym leczeniu tętniaków aorty brzusznej?
Is CT still a method of monitoring patients after endovascular treatment of abdominal aortic aneurysms?
1Department of Interventional Radiology and Neuroradiology, Medical University, Lublin
Head of Department: prof. Małgorzata Szczerbo-Trojanowska, MD, PhD
2Department of Radiology and Nuclear Medicine, Medical University, Lublin
Head of Department: prof. Andrzej Drop, MD, PhD
Streszczenie
Wstęp. Metoda wewnątrznaczyniowa leczenie chorych z tętniakami aorty brzusznej stała się uznaną alternatywą dla operacji klasycznej. Jednym z najczęściej spotykanych powikłań jest zaciek krwi do worka tętniaka, pojawiający się w wyniku niecałkowitego wyłączenie worka tętniaka z krążenia.
Cel pracy. Ocena przydatności ultrasonograficznych środków kontrastujących w diagnostyce zacieków u chorych z TAB leczonych na drodze śródnaczyniowej.
Materiał i metody. 198 chorych z TAB było leczonych na drodze śródnaczyniowej. U każdego chorego 6 miesięcy po implantacji stentgraftu przeprowadzono badanie kontrolne; najpierw badanie ultrasonograficzne przed podaniem i po podaniu środka kontrastującego, a następnie badanie TK. Każde badanie usg wykonywano w opcji color, power, Bflow przed podaniem, a następnie po podaniu środka kontrastującego, dodatkowo po podaniu środka kontrastującego przeprowadzono badanie w technice CEUS.
Wyniki. W badaniu kontrolnym po 6 miesiącach w usg przed podaniem kontrastu we wszystkich trzech technikach: color, power, Bflow rozpoznano 16 zacieków, w tym: 6 typu IA, 4 typu IB, 2 typu IIA, 4 typu IIB. W badaniu ultrasonograficznym po podaniu środka kontrastującego we wszystkich opcjach – color, power i Bflow – potwierdzono wcześniej rozpoznane 16 zacieków i dodatkowo zdiagnozowano 6 zacieków: 1 typu IB, 2 IIA i 3 IIB. W badaniu usg po podaniu środka kontrastującego w technice CEUS potwierdzono 22 rozpoznane zacieki i dodatkowo zdiagnozowano: 2 zacieki typu IIA i 2 IIB. W badaniu angio-TK rozpoznano 22 zacieki: 6 typu IA, 5 IB, 4 IIA i 7 IIB. Żadnego z 4 zacieków dodatkowo rozpoznanych w technice CEUS nie zdiagnozowano w angio-TK.
Wnioski. Zastosowanie środków kontrastujących znacząco podnosi czułość badania ultrasonograficznego w rozpoznawaniu zacieków, szczególnie typu II.
Badanie z użyciem techniki CEUS wykazało najwyższą czułość w rozpoznawaniu zacieków, bo ujawniło te, których nie rozpoznano w innych technikach, łącznie z angio-TK.
Technika CEUS może zastąpić badania angio-TK w monitorowaniu chorych po implantacji stentgraftów.
Summary
Introduction. The endovascular treatment of patient with abdominal aorta aneurysms has been a recognized alternative to classic surgery. One of the most common complications is an endoleak developing due to incomplete exclusion of the aneurysmal sac from circulation.
Aim. To assess the value of ultrasound contrast agents for the diagnosis of endoleaks in patients with AAA treated by stent graft implantation.
Material and methods. One hundred and ninety-eight patients with AAA were treated with stent graft implantation. Follow-up examinations, i.e. pre- and post-contrast ultrasound and angio-CT, were performed 6 months after treatment in all patients. In each ultrasound examination, colour, power, Bflow options were used before and after contrast injection; additionally, contrast-enhanced ultrasound (CEUS) was performed after contrast administration.
Results. During the follow-up examinations after 6 months, pre-contrast ultrasound performed in all options (colour, power, Bflow) revealed 16 endoleaks: 6 type IA, 4 type IB, type 2 IIA and 4 type IIB; in post-contrast ultrasound using CEUS 22 endoleaks were confirmed and additionally 4 endoleaks were diagnosed: 2 type IIA, and 2 type IIB. In angio-CT, 22 endoleaks were diagnosed: 1 type IA, 5 type IB, 4 type IIA, and 7 type IIB. None of the four additional endoleaks observed with CEUS was found in angio-CT.
Conclusions. The use of ultrasound contrast media significantly increases the sensitivity of ultrasound in the diagnosis of endoleaks, particularly type II ones.
CEUS examinations show the greatest sensitivity in detecting endoleaks, as they disclose the endoleaks unrecognized by other techniques, including angio-CT.
Post-contrast ultrasound can replace angio-CT in monitoring patients after stent graft implantations.

Introduction
An aneurysm is the local dilation of the lumen of a vessel by 50% compared to the proximal, unaffected segment. In practice, the abdominal aortic aneurysm is diagnosed when its diameter is at least 30 mm, measured from the internal to external vessel outline (1-7). The normal diameter of aorta in the subrenal segment is 1.66-2.16 cm in women and 1.99-2.39 in men (8, 9). With age, the aorta lumen gradually dilates. Aneurysms develop due to lesions in the vascular wall. The diameters of aortic aneurysms range from 30 to 150 mm. The frequency of abdominal aortic aneurysms is 4-7.6% in the population > 55-65 years, is believed to increase with age, and is 4-8 times higher in men. Screening examinations are the most objective assessments of the incidence of this pathology. The majority of aneurysms are asymptomatic until complications develop, such as rupture or secondary thromboembolic incidents. Small aneurysms do not generally cause any characteristic symptoms. Their growth may not be detectable due to a relative large area in the retroperitoneal space and susceptibility of the parietal peritoneum.
The most severe complication of abdominal aortic aneurysm is its rupture, which mainly depends on diameter. Abdominal aortic aneurysms of diameters < 5 cm were demonstrated to rupture in 0.5-5% of cases while those with diameters > 7 cm rupture in 20-40% of patients within one year after diagnosis (10, 11).
Abdominal aortic aneurysms are treated with surgical and endovascular methods. Conservative treatment is to inhibit the growth of aneurysm, predominantly by normalisation of arterial blood pressure (pharmacological treatment).
The first recognized surgery of abdominal aortic aneurysm was carried out by an excellent English surgeon, Sir Astley Cooper in London in 1817 (12, 13). Moreover, the surgical procedure performed by Charles Dubost was of importance for further development of surgery; in 1951, he excised an aortic aneurysm and implanted a cadaveric human (homograft) thoracic aorta (14). In 1952, Voorhees produced the first synthetic graft, which successfully replaced a homograft (12). In 1966, Oscar Creech suggested to cover the implanted graft with the aneurysmal sac during reconstruction. Since then, this method has been used with very good remote outcomes (15).
Endovascular treatment involves the exclusion of aneurysms from the circulation by inserting a stent graft to the lumen of aneurysm-containing aorta.
A new era in the treatment of abdominal aortic aneurysms started in 1991, when in Buenos Aires Juan Parodi performed the exclusion of abdominal aortic aneurysm from the circulation using the Palmaz stent expanded on a balloon attached to a knitted Dacron prosthesis (1, 16-18). In the same year, Volodosa published his report on endovascular treatment of abdominal and thoracic aortic aneurysms (19). In Poland, the first stent graft implantation into the affected abdominal aorta was carried out in the Department of Interventional Radiology and Neuroradiology, Medical University of Lublin in 1998.
The endovascular treatment of patients with abdominal aortic aneurysms has been a recognized alternative to classic surgery. However, the method is not free of complications.
The minor complications of endovascular treatment of abdominal aortic aneurysms include post-implantation syndrome, which occurs in less than 50% of cases and manifests with elevated body temperature, leucocytosis, and elevated heart rate above 90/min (16-18). Infections of stent grafts are extremely rare. The cases described in literature resulted from inadequate sterility of treatment rooms. The presence of gas bubbles in computed tomography angiography (angio-TK) around the stent graft is pathognomic for the infected prosthesis (19). The more serious complications, occurring despite fully effective procedures of prosthesis implantation, are ruptures, migrations, and bending of stent grafts, endoleaks, endotension, thrombosis of the main branch or femoral branches of stent grafts (19, 20). Stent graft rupture is one of the most dramatic complications (1). According to the EUROSTAR report of 2003, this complication develops in 1% of patients within the 5-year period of observation (19). Stent graft migration, thrombosis, obstruction are currently rare complications and occur in about 4% of patients within the first year of observation. A substantial reduction in the number of these complications is associated by wide availability of new generation stent grafts, which are more advanced and enable permanent suprarenal fixation of prosthesis (21). Stent graft shift by over 10 mm in relation to renal arteries is considered its migration. The migration can be caused by unstable fixation of the main prosthetic branch, lesions in the wall of the vessel adjacent to a stent graft, dilation of the aneurysm neck (22). Stent graft thrombosis is usually caused by angular bending of the prosthetic iliac branch; its risk is 2.4-11.7%. The main risk factors of thrombosis is bending of a stent graft and significant atherosclerotic changes in the iliac segment. Stenosis of the main branch or iliac branches of stent grafts is more common in cases of tortuous iliac or femoral branches of stent grafts (3, 19). One of the most common complications is an endoleak developing due to incomplete exclusion of the aneurysmal sac from circulation (23, 24). Endoleaks are classified according to their source; five types of endoleaks are known (fig. 1).
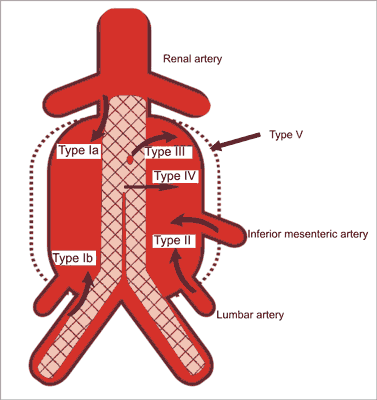
Fig. 1. Five types of endoleaks.
There are also the following subtypes of endoleaks:
– type I a: in the region of proximal stent graft fixation,
– type I b: in the region of distal stent graft fixation,
– type I c: in the region of iliac artery occluder,
– type II a: from the inferior mesenteric artery,
– type II b: from the lumbar artery,
– type III a: due to disconnection of stent graft parts,
– type III b: due to tears of the material covering the stent graft,
– type IV: due to porosity of the material covering the stent graft,
– type V: endotension, endoleaks of undetermined origin.
Patients after stent graft implantation require follow-up examinations to detect possible complications. Spiral computed tomography is considered to be the gold standard for monitoring of this group of patients 3, 6, 12 months after implantation and then once a year.
Aim
To determine the usefulness of ultrasound examinations with Doppler options, with special attention paid to ultrasound contrast media (UCM), for monitoring patients with abdominal aortic aneurysms treated with the endovascular stent grafting and for exclusion or confirmation of endoleaks.
Material and methods
The study included 198 patients treated with the endovascular technique due to abdominal aortic aneurysms in the Department of Interventional Radiology and Neuroradiology in Lublin. The study population consisted of 166 men and 32 women aged 46-90 years. All patients with abdominal aortic aneurysms underwent stent graft implantation in the angiographic laboratory of the Department of Interventional Radiology and Neuroradiology in Lublin.
Each patient after endovascular treatment of abdominal aortic aneurysms had follow-up examinations 6 months after the procedure; first pre- and post-contrast ultrasound (SonoVue), followed by abdominal angio-CT performed several days later.
Ultrasound examinations were conducted in the Department of Interventional Radiology and Neuroradiology, whereas angio-CT in the Department of Radiology and Nuclear Medicine, Medical University of Lublin.
All ultrasound examinations were performed using the LOGIQ 7 device (GE), equipped with a 3.5 MHz probe enabling imaging of blood flow with Doppler (colour, power) and non-Doppler (Bflow) options. The machine is adjusted to examinations with UCM, is equipped with harmonic imaging and special software for contrast examinations, in which colour-coded Doppler blood flow is not used. After the administration of UCM, CEUS followed by typical Doppler examination was performed in each patient. Sonographic procedures were carried out in the dorsal decubitus position with knees of lower limbs slightly bent and the abdomen, sides and the region of groins (bilaterally) exposed. In the majority of patients, additionally the right and left side positioning was used. The lateral access enables to overcome effectively the limitation associated with the depth and tortuosity of vessels or presence of intestinal gases.
The first stage of examination without UCM was initiated with imaging in the B presentation; first in the transverse projection followed by longitudinal projection visualizing the aorta from the level of visceral trunk ostium (with the superior mesenteric and renal arteries included), accurate analysis of aneurysmal sac, measurement of its diameter, evaluation of the course of graft branches and iliac arteries to the level of the inguinal ligament or even common femoral arteries. Within the thrombus, in the aneurysmal sac excluded from circulation, the presence of echoless areas was meticulously analysed, which can evidence the presence of endoleaks. The next stage involved the use of Doppler options (colour-coded blood flow, including the power option) and non-Doppler (Bflow) options for exclusion or confirmation of endoleaks. All the options mentioned above were applied in each patient in search for possible pathologies. Subsequently, blood flow parameters were recorded (spectral tracings) in the detected endoleaks by evaluating the spectrum and velocity.
The second stage involved the administration of UCM (SonoVue, Bracco) in a dose of 2.4 ml. By mixing the powder with 0.9 sodium chloride solution, the suspension containing gas micro-bubbles was obtained (sulphur hexafluoride). Each bubble is smaller than the red blood cell. The bubbles reflect the ultrasound beam and ensure better signals than the body tissues. The agent is effectively present in the circulatory system for several minutes.
During the examination, the device was set at optimal performance values for UCM, i.e. 3.5 MHz at low mechanical index (MI 0.01-0.02), optimal settings of PRF and filters using harmonic imaging. Harmonic imaging at low MI prevents quick destruction of gas micro-bubbles.
After administration of SonoVue in a single dose of 2.4 ml, the examination was initiated. During the first stage, the examination was performed in the CEUS option to evaluate blood flow in the aneurysmal sac evidencing endoleaks. Subsequently, the same protocol was applied without UCM with exclusion of projection B imaging using Doppler options (colour-coded blood flow with the power option), non-Doppler options (Bflow) and spectral tracings.
Several days after ultrasound examinations, each patient underwent CT in the Department of Radiology and Nuclear Medicine, Medical University of Lublin (Head: prof. Andrzej Drop, MD, PhD).
The examinations were carried out with a 64-row CT scanner (General Electric LightSpeed Ultra). The abdominal aorta was visualized from the visceral trunk to the division of femoral arteries following the protocol of peak saturation within 30 seconds after administration of an iodine contrast medium (Ultravist 370 mg I/ml, Schering), 100-120 ml, through the automated syringe with the speed of 2.5 ml/s. The nominal slice thickness – 5 mm, table speed – 7.5 mm/s, pitch – 1.5, effective slice thickness – 2 mm.
The detailed evaluation of stent grafts was possible thanks to the use of the following options: multiplanar reconstruction (MPR), curve reconstruction, minimum and maximum intensity projection and a three-dimensional model – virtual reality (VR). Moreover, pre- and post-contrast ultrasound results were compared with angio-CT findings.
Results
Powyżej zamieściliśmy fragment artykułu, do którego możesz uzyskać pełny dostęp.
Mam kod dostępu
- Aby uzyskać płatny dostęp do pełnej treści powyższego artykułu albo wszystkich artykułów (w zależności od wybranej opcji), należy wprowadzić kod.
- Wprowadzając kod, akceptują Państwo treść Regulaminu oraz potwierdzają zapoznanie się z nim.
- Aby kupić kod proszę skorzystać z jednej z poniższych opcji.
Opcja #1
29 zł
Wybieram
- dostęp do tego artykułu
- dostęp na 7 dni
uzyskany kod musi być wprowadzony na stronie artykułu, do którego został wykupiony
Opcja #2
69 zł
Wybieram
- dostęp do tego i pozostałych ponad 7000 artykułów
- dostęp na 30 dni
- najpopularniejsza opcja
Opcja #3
129 zł
Wybieram
- dostęp do tego i pozostałych ponad 7000 artykułów
- dostęp na 90 dni
- oszczędzasz 78 zł
Piśmiennictwo
1. Kaufman JA, Geller SC, Brewster DC et al.: Endovascular repair of abdominal aortic aneurysms. AJR 2000; 175: 289-302.
2. Kinney KB, Riwiera-Sanfeliz GM, Ferrara S: Stent grafts for abdominal and thoracic aortic disease. Appl Radiol 2005; 34(3): 9-19.
3. Pasierski T: Angiologia. PZWL, Warszawa 2004: 215-220.
4. Sakalihasan N, Limet R, Defawe OD: Abdominal aortic aneurysm. Lancet 2005; 6(365): 1577-1589.
5. Upchurch GR, Schaub TA: Abdominal aortic aneurysm. Am Fam Physician 2006; 73: 1198-1204.
6. Waliszewski K, Słomski R, Oszkinis G, Majewski W: Genetyczne aspekty powstawania tętniaków aorty brzusznej. Pol Merk Lek 2005; 18(103): 111-114.
7. Yeung BKF, Pearce WH: Surgical management of abdominal aortic aneurysm. Vascular Medicine 2000; 5: 187-193.
8. Volodos NL, Karpovich IP, Troyan VI et al.: Clinical experience of the use of self-fixing synthetic prostheses for remote endoprosthetics of the thoracic and the abdominal aorta and iliac arteries through the femoral artery and as intraoperative endoprosthesis for aorta reconstruction. Vasa Suppl 1991; 33: 93-95.
9. Parodi JC, Palmaz JC, Barone HD: Transfemoral intraluminal graft implantation for abdominal aortic aneurysms. Ann Vasc Surg 1991 Nov; 5(6): 491-499.
10. Lederle FA, Johnson GR, Wilson SE et al.: Veterans Affairs Cooperative Study #417 Investigators. Rupture rate of large abdominal aortic aneurysms in patients refusing or unfit for elective repair. JAMA 2002 Jun 12; 287(22): 2968-2972.
11. Szmidt J: Tętniaki aorty brzusznej. [W:] Szmidt J (red.): Podstawy chirurgii. T. I, Medycyna Praktyczna, Kraków 2003: 951.
12. Cervantes J: Reflection on the 50th anniversary of the first abdominal aortic aneurysm resection. World J Surg 2003; 27: 246-224.
13. Thompson JE: Early history of aortic surgery. Invited comments. J Vasc Surg 1998; 28: 746-752.
14. Kinney KB, Riwiera-Sanfeliz GM, Ferrara S: Stent grafts for abdominal and thoracic aortic disease. Appl Radiol 2005; 34(3): 9-19.
15. Creech O Jr: Endo-aneurysmorrhaphy and treatment of aortic aneurysm. Ann Surg 1966 Dec; 164(6): 935-946.
16. Katzen BT, MacLean AA: Past, present, and future endograft devices. Tech Vasc Interv Radiol 2005; 8(1): 16-21.
17. Nicholson A: Endovascular stent grafting of abdominal aortic aneurysms: a radiologists view on a new potential issue in renovascular disease. Journal of Renovascular Disease 2003; 2: 34-36.
18. Veith FJ, Martin ML, Cynamon J et al.: 1992: Parodi, Montefiore, and the first abdominal aortic aneurysm stent graft in the United States. Ann Vasc Surg 2005; 19: 749-751.
19. Zubilewicz T: Ponowne zabiegi u chorych leczonych na tętniaka aorty brzusznej stentgraftami wewnątrznaczyniowymi. Praca habilitacyjna. Akademia Medyczna w Lublinie.
20. Baum RA, Carpenter JP, Stavropoulous SW, Fairman RM: Diagnosis and management of type 2 endoleaks after endovascular aneurysm repair. Tech Vasc Interv Radiol 2001; 4(4): 222-226.
21. Fogarty TJ, Arko FR, Zarins CHK: Endograft technology: highlights of the past 10 years. J Endovasc Ther 2004; 11(suppl. II): 192-199.
22. Magennis R, Joekes E, Martin J et al.: Complications following endovascular abdominal aortic aneurysm repair. The British Journal of Radiology 2002; 75: 700-707.
23. Napoli V, Bargellini I, Sardella SG et al.: Abdominal aortic aneurysm: contrast-enhanced US for missed endoleaks after endoluminal repair. Radiology 2004; 233(1): 217-225.
24. Wilson SE, Gelfand D, White GH: Clinical significance of type II endoleaks occuring after endovascular aortic aneurysm repair. Ann Vasc Surg 2006; 20(1): 69-74.
25. Laborde JC, Parodi JC, Clem MF et al.: Intraluminal bypass of abdominal aortic aneurysm: feasibility study. Radiology 1992 Jul; 184(1): 185-190.
26. Parodi JC, Palmaz JC, Barone HD: Transfemoral intraluminal graft implantation for abdominal aortic aneurysms. Ann Vasc Surg 1991 Nov; 5(6): 491-499.
27. Shah H, Kumar SR, Major K et al.: Technology penetration of endovascular aortic aneurysm repair in southern California. Ann Vasc Surg 2006 Nov; 20(6): 796-802.
28. Berge C, Haug ES, Romundstad PR et al.: Infrarenal abdominal aortic aneurysm repair: time-trends during a 20-year period. World J Surg 2007 Aug; 31(8): 1682-1686. Epub 2007 Jun 15.
29. Hill JS, McPhee JT, Messina LM et al.: Regionalization of abdominal aortic aneurysm repair: evidence of a shift to high-volume centers in the endovascular era. J Vasc Surg 2008 Jul; 48(1): 29-36.
30. Schanzer A, Greenberg RK, Hevelone N et al.: Predictors of abdominal aortic aneurysm sac enlargement after endovascular repair. Circulation 2011 Jun 21; 123(24): 2848-2855.
31. Cao P, Verzini F, Parlani G et al.: Clinical effect of abdominal aortic aneurysm endografting: 7-year concurrent comparison with open repair. J Vasc Surg 2004 Nov; 40(5): 841-848.
32. Bush RL, Johnson ML, Collins TC et al.: Open versus endovascular abdominal aortic aneurysm repair in VA hospitals. J Am Coll Surg 2006 Apr; 202(4): 577-587.
33. Matsumura JS, Brewster DC, Makaroun MS, Naftel DC: A multicenter controlled clinical trial of open versus endovascular treatment of abdominal aortic aneurysm. J Vasc Surg 2003 Feb; 37(2): 262-271.
34. Carpenter JP: Midterm results of the multicenter trial of the powerlink bifurcated system for endovascular aortic aneurysm repair. J Vasc Surg 2004 Nov; 40(5): 849-859.
35. Heikkinen MA, Arko FR, Zarins CK: What is the significance of endoleaks and endotension. Surg Clin North Am 2004 Oct; 84(5): 1337-1352.
36. Ouriel K, Clair DG, Greenberg RK et al.: Endovascular repair of abdominal aortic aneurysms: device-specific outcome. J Vasc Surg 2003 May; 37(5): 991-998.
37. AbuRahma AF: Fate of endoleaks detected by CT angiography and missed by color duplex ultrasound in endovascular grafts for abdominal aortic aneurysms. J Endovasc Ther 2006 Aug; 13(4): 490-495.
38. Wilson SE, Gelfand D, White GH: Clinical significance of type II endoleaks occuring after endovascular aortic aneurysm repair. Ann Vasc Surg 2006; 20(1): 69-74.
39. Tummala S, Powell A: Imaging of endoleaks. Techniques in Vascular and interventional. Radiology 2001; 4(4): 208-212.
40. Makaroun M, Zajko A, Sugimoto H et al.: Fate of endoleaks after endoluminal repair of abdominal aortic aneurysms with the EVT device. Eur J Vasc Endovasc Surg 1999 Sep; 18(3): 185-190.
41. Arko FR, Filis KA, Heikkinen MA et al.: Duplex scanning after endovascular aneurysm repair: an alternative to computed tomography. Semin Vasc Surg 2004 Jun; 17(2): 161-165.
42. Soulen MC, Fairman RM, Baum RA: Embolization of the internal iliac artery: still more to learn. J Vasc Interv Radiol 2000; 11: 543-545.
43. Farner MC, Carpenter JP, Baum RA, Fairman RM: Early changes in abdominal aortic aneurysm diameter after endovascular repair. J Vasc Interv Radiol 2003; 14: 205-210.
44. Henao EA, Hodge MD, Felkai DD et al.: Contrast-enhanced Duplex surveillance after endovascular abdominal aortic aneurysm repair: improved efficacy using a continuous infusion technique. J Vasc Surg 2006 Feb; 43(2): 259-264; discussion 264.
45. Clevert DA, Minaifar N, Weckbach S et al.: Color duplex ultrasound and contrast-enhanced ultrasound in comparison to MS-CT in the detection of endoleak following endovascular aneurysm repair. Clin Hemorheol Microcirc 2008; 39(1-4): 121-132.

