Nóra Pető1, *Terèzia Seres2, Zoltán Szakács1, Veronika Fáy3, Jelena Karaszova3, Andrea Kontra3, Olivia Lalátka3, Gyula Domján4
Evaluation of the Brussells Questionnaire as a screening tool for obstructive sleep apnea syndrome
1Department of Neurology, Hungarian Defence Forces Military Hospital, Budapest, Hungary
Head of Department: Zoltán Szakács, MD, PhD
2Doctoral School, Semmelweis University, Budapest, Hungary
Head of Department: Gyula Domján, MD, PhD
3Rehabilitation Centre, Combined Szent István and Szent László Hospital, Budapest, Hungary
Head of Centre: Veronika Fáy, MD, PhD
4Department of Clinical Studies, Faculty of Health Sciences, Semmelweis University, Budapest, Hungary
Head of Department: Klára Gadó, MD, PhD
Summary
Introduction. Obstructive sleep apnea syndrome (OSAS) has been recently shown to be associated with an increased risk of traffic accidents. Expensive and not widely available polysomnography (PSG) is the gold standard for diagnosing OSAS. The questionnaire developed by the Obstructive Sleep Apnoea Working Group in 2013 in Brussells (termed the Brussels Questionnaire) was created as a screening strategy for those who apply for a driver’s license.
Aim. The aim of this study was to evaluate the sensitivity and specificity of the Brussels Questionnaire for detecting OSAS.
Material and Methods. 285 patients who reported to the Sleep Disorders Centre of the Neurology Department of the Hungarian Defence Forces Military Hospital for the portable monitoring (PM) completed the Brussels Questionnaire. A score of 10 or higher out of 24 indicated a high risk of OSAS. The results of the questionnaire were then compared with the results of the PM as well as of the polysomnography (PSG) when available.
Results. After the comparison of the results obtained with PM and the Brussels Questionnaire, the sensitivity and specificity of the questionnaire were calculated and amounted 0.64 and 0.49, respectively. After the comparison of the results obtained with PSG and the Brussels Questionnaire, the sensitivity and specificity of the questionnaire were calculated and amounted 0.83 and 0.55, respectively. The score of 10 points was found to be the optimal cut-off value.
Conclusions. The Bruxelles Questionnaire is a simple screening tool for OSAS in candidates for driver’s license, with a sensitivity of 0.64 and a specificity of 0.49. Its specificity and sensitivity are similar to those of other frequently used questionnaires.
Introduction
Obstructive sleep apnea syndrome (OSAS) is a significant medical problem affecting at least 2-26% of the general population (1). It is an important risk factor for cardiovascular diseases (2). It can also cause a significant decrease in the quality of life (1). In the recent years, the relationship of OSAS and traffic accidents have been studied. OSAS was found to be a risk factor for falling asleep while driving, which increased the risk of accidents and near-misses (3). The most common daily syptoms of OSAS include excessive sleepiness, which is probably the source of the increased accident rate in OSAS patients. Fortunately, current research indicates that adequate OSAS treatment, including the therapy with continous positive airway pressure (CPAP), decreases the risk of accidents to the risk of the general population (4). This emphasizes the importance of proper diagnosis and treatment.
Polysomnography (PSG) is the gold standard for diagnosing obstructive sleep apnea/hypopnea syndrome (OSAHS), but is expensive and time-consuming (5), and therefore, cannot be used for screening. An effective screening tool may help detect patients who are at risk of having OSAHS so that proper diagnostic process can be initiated. Several questionnaires have been developed for this purpose (6).
The Epworth Sleepiness Scale (ESS) measures sleep propensity in order to differentiate persons with excessive daytime sleepiness (EDS). The ESS is a simple, self-report questionnaire (5). It contains eight questions concerning the possibility of falling asleep in various daily situations, with answers on an interval scale from 0 to 3 (5). The Berlin Questionnaire (BQ) was designed to identify individuals at higher risk of OSAHS in primary care. It contains 10 questions divided into three cathegories (6):
– snoring severity,
– EDS, and
– history of hypertension or obesity.
The patient is subsequently cathegorized into a low or high risk group (6). The STOP questionnaire contains four forced-choice (yes/no) questions related to snoring, tiredness during daytime, observed apneas and high blood pressure (acronym STOP) (5). Persons answering positively two or more questions are considered at high risk of OSAHS. High risk for OSAHS is defined when two or more questions are answered positively. The STOP-Bang questionnaire was developed on the basis of the STOP questionnaire. The second part of the STOP-Bang questionnaire consists of the following criteria: BMI > 35 kg/m2, age > 50 years, neck circumference > 40 cm, and gender (male) (6). The 4-V is a tool for the identification of moderate to severe OSAHS and consists of four criteria (gender, blood pressure, BMI, and self-reported snoring) (6). Most of the questionnaires have already been validated. STOP-Bang and BQ are the most commonly used OSAS questionnaires in primary care (6).
The questionnaire developed by the Obstructive Sleep Apnoea Working Group in 2013 in Brussells (termed Brussels Questionnaire) was created as a screening startegy for those who apply for a driver’s license (7).
Aim
The aim of this study was to evaluate the sensitivity and specificity of the Brussels Questionnaire for detecting OSAS.
Material and Methods
The materials for the study were collected from November 2015 to February 2016. 285 patients were enrolled: 111 women (38.95%) and 174 men (61.05%). 22 (7.72%) of the participants were younger than 30 years old, 263 (92.28%) were 30 years old or older. 150 (52.63%) subjects had BMI lower than 30, 86 (30.18%) of them were obese with a BMI of 30-35, and 49 (17.19%) were morbidly obese with BMI ≥ 35.
Patients who reported to the Sleep Disorders Centre of the Neurology Department of the Hungarian Defence Forces Military Hospital for the portable monitoring (PM) were asked to complete the Brussels Questionnaire. If needed, they were provided with a physician’s help in filling in the questionnaire. In patients in whom moderate or severe OSAS was suspected after PM and a consultation with a somnologist, the patient was referred for nocturnal, laboratory-based polysomnography (PSG). PSG recordings were subsequently assessed by an expert somnologist. Sleep stages were distinguished and the Apnea-Hypopnea Index (AHI) was calculated according to the recommendations of the Task Force of the American Academy of Sleep Medicine (4).
The Brussels questionnaire consists of objective questions (gender, age, weight, height, and history of traffic accidents), as well as symptoms constituing the clinical picture of OSAS (tab. 1). All the questions have three possible answers: YES, NO, and DON'T KNOW. Daytime sleepiness is assessed with the ESS scale. The questions are attributed a value, reflecting the strength of the association between a given answer and the risk of motor vehicle accidents (MVAs) or the possibility of suffering from OSAS, as well as the level of uncertainty concerning this strength. The values are represented in table 2. The maximal possible score in this questionnaire is 24. If the result is 10 or higher, the screening is defined as positive and a medical advice should be required before a decision is reached on the driving license to be delivered (6).
Tab. 1. The Brussels Questionnaire (6)
| 1. Gender |
| 2. Age |
| 3. Weight |
| 4. Height |
| 5. Did it already happen to you to doze off while driving? |
| YES | NO | DON’T KNOW |
| 6. Did you have a serious accident (with personal injuries or property damage) due to sleepiness in the last 3 years? |
| YES | NO | DON’T KNOW |
| 7. Do you usually snore loudly almost every night? |
| YES | NO | DON’T KNOW |
| 8. Have you been told your breathing stops during your sleep? |
| YES | NO | DON’T KNOW |
| 9. Do you usually wake up refreshed after a full night sleep? |
| YES | NO | DON’T KNOW |
| 10. Do you suffer from, or are you being treated for, Arterial Hypertension? |
| YES | NO | DON’T KNOW |
| 11. Please complete the questionnaire on usual daytime sleepiness, called the Epworth Sleepiness Scale, on the next page |
Tab. 2. Values of the Brussels Questionnaire items (6)
| Q. 1: Female = 1; Male = 2 |
| Q. 2: Age below 30 yo = 2; Age 31 yo or above = 1 |
| Q. 3-4: A BMI below 30 kg/m2 = 1, 31-35 kg/m2 = 2; 36 kg/m2 or higher = 3 |
| Q. 5: A positive answer = 3; negative answer = 0; don’t know = 2 |
| Q. 6: A positive answer = 4; negative answer = 0; don’t know = 3 |
| Q. 7: A positive answer = 2; negative answer = 0; don’t know = 1 |
| Q. 8: A positive answer = 1; negative answer = 0; don’t know = 0 |
| Q. 9: A negative answer = 2; positive answer = 0; don’t know = 1 |
| Q. 10: A positive answer = 2; negative answer = 0; don’t know = 1 |
| ESS: From 11 to 14 = 2; 15 or higher = 4 |
In our study, the score of the survey was compared with the results of PM and PSG.
The data were analyzed using R and SPSS Statistica software. Sensitivity and specificity for AHI ≥ 15 were calculated. The discrimination ability of the questionnaire was evaluated using a receiver operating characteristic (ROC) curve that was calculated for the score of the questionnaire ≥ 10.
Results
After the comparison of the results obtained with PM and the Brussels Questionnaire, the sensitivity and specificity of the questionnaire were calculated and amounted 0.64 and 0.49, respectively. AUC was 0.57 (tab. 3; fig. 1). After the comparison of the results obtained with PSG and the Brussels Questionnaire, the sensitivity and specificity of the questionnaire were calculated and amounted 0.83 and 0.55, respectively, with the AUC = 0.65 (tab. 3; fig. 2). The score of 10 points was found to be the optimal cut-off value with neither sensitivity nor specifity being priviledged at the cut-off point.
Tab. 3. Predictive parameters of the Brussels Questionnaire
| Results used for evaluation | Sensitivity | Specificity | AUC |
| PG | 0.64 | 0.49 | 0.57 |
| PSG | 0.83 | 0.55 | 0.65 |
AUC: area under curve; PG: polygraphy (portable monitor); PSG: polysomnography
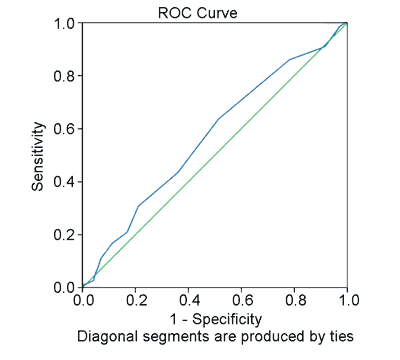
Fig. 1. ROC Curve based on PG results. AUC = 0.57
ROC: Reciever Operating Characteristic; AUC: Area Under Curve; PG: polygraphy (portable monitor)
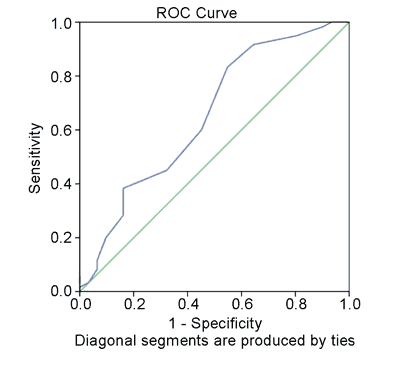
Fig. 2. ROC Curve based on PSG results. AUC = 0.65
ROC: Reciever Operating Characteristic; AUC: Area Under Curve; PSG: polysomnography
We have found that AHI measured with PG and with PSG had a significant positive correlation (Spearman’s r = 0.628; p < 0.005). AHI scores measured with PG did not differ significantly between the groups of patients with Brussels Score < 10 and ≥ 10, with mean AHI 25.475 and 34.41, respectively (p = 0.11). However, AHI scores measured with PSG did differ significantly for the two groups, being 25.444 and 44.616, respectively (p < 0.005).
Discussion
In general, a good screening tool for OSAS should have a high sensitivity and a high negative predictive value, i.e. it is most important for this tool to appoint most of the patients with severe or moderate OSAS that are eligible for treatment. On the other hand, high specificity would help to avoid unnecessary costs from excessive resource utilization. Improving the specificitiy of a subjective screening tool, such as a questionnaire, is a huge challenge, because the symptoms of OSAS are not specific to the disease.
According to the recommendations of the Obstructive Sleep Apnoea Working Group, a driver with an OSAS diagnosis may be authorized to drive if they have untreated mild OSAS with an AHI ≤ 15 (mild to moderate OSAS) (7). Therefore, sensitivity and specificity were calculated for AHI ≥ 15 in our study.
Several questionnaires has been created for screening for OSAS, many of which has been validated in primary care, surgical setting or sleep clinics (1, 5, 8). Most of the tests validated in primary care have an acceptable sensitivity (tab. 4) (7). A meta-analysis of screening tests for OSA identified STOP-Bang scale as an excellent method for diagnosing severe OSAS, although it is an average predictor for the diagnosis of OSAS (9). However, another study reported the sensitivity of STOP-Bang for screening for moderate OSAS to be 0.93 in patients without a history of sleeping disorders for AHI ≥ 15 (2). The sensitivity and specificity of other screening tools, as well as the results of our study, are listed in table 4.
Tab. 4. Predictive parameters of questionnaires for screening for OSA (AHI ≥ 15) (1)
| Questionnaire/Study | Sensitivity | Specificity |
| ASA – Chung 2008 | 0.79 | 0.37 |
| Berlin – Pataka 2013 | 0.87 | 0.33 |
| Berlin – Chung 2008 | 0.79 | 0.50 |
| Berlin – Netzer 1999 | 0.54 | 0.97 |
| ESS – Pataka 2013 | 0.54 | 0.67 |
| STOP – Pataka 2013 | 0.96 | 0.13 |
| STOP – Chung 2008 | 0.74 | 0.53 |
| STOP-Bang – Pataka 2013 | 0.98 | 0.13 |
| STOP-Bang – Chung 2008 | 0.93 | 0.43 |
| Wisconsin – Young 1993 | 0.87 | 0.40 |
| 4-Variable ≥ 11 – Pataka 2013 | 0.79 | 0.36 |
| 4-Variable ≥ 14 – Pataka 2013 | 0.55 | 0.74 |
| Brussels Questionnaire 2016 PG | 0.64 | 0.49 |
| Brussels Questionnaire 2016 PSG | 0.83 | 0.55 |
AHI: apnea-hypopnea index; ASA: American Society of Anaesthesiologists’ checklist; STOP: snoring, tiredness, observed apnea, high blood pressure; STOP-Bang: STOP questionnaire and BMI, age, neck circumference, gender; in the last two rows, the results of this study are presented, using polygraphy (PG, portable monitor) and polysomnography (PSG) data, respectively.
The validation with the help of PSG is considered more accurate, given that it is the gold standard for the diagnosis (4). PM can be as accurate as PSG for the diagnosis in selected populations. According to the AASM guidelines, it can be used as an alternative to PSG for the diagnosis of OSAS in patients with a high pretest probability of moderate to severe OSAS (10). However, it is not the most appropriate method of general screening of asymptomatic population (10).
The ease of administration and scoring are important characteristics of a screening tool. Brussels Questionnaire only takes a few minutes to complete, in addition, the interpretation of the result is simple.
Our study indicates that among our sleep clinic patients, a Brussels score of 10 has the best discrimination for predicting moderate to severe OSA (AHI ≥ 15), as it was originally suggested by the Obstructive Sleep Apnoea Working Group (7).
There are some limitations to our study. It was performed on the patients of the Sleep Clinic and it may not be appropriate to transfer these conclusions to the asymptomatic population (10). However, we used in-laboratory polysomnography for the evaluation of 76 patients, which enabled us to find better predictive parameters.
Further research is needed to improve the Brussels Questionnaire and its specificity without compromising sensitivity.
Conclusions
We conclude that the Brussels Questionnaire is an acceptable screening tool for moderate and severe OSAS with the optimal cut-off point of 10. The Bruxelles Questionnaire is a simple tool for screening patients for OSAS before applying for driving license, with a sensitivity of 0.64, a specificity of 0.49 and AUC of 0.57. This correlates with the results of the most frequently used questionnaires.
Piśmiennictwo
1. Ulfberg J, Carter N, Talbäck M, Edling C: Excessive daytime sleepiness at work and subjective work performance in the general population and among heavy snorers and patients with obstructive sleep apnea. Chest 1996; 110: 659-663.
2. Abrishami A, Khajehdehi A, Chung F: A systematic review of screening questionnaires for obstructive sleep apnea. Can J Anesth 2010; 57: 423-438.
3. Turkington PM, Sircar M, Allgar V, Elliott MV: Relationship between obstructive sleep apnoea, driving simulator performance, and risk of road traffic accidents. Thorax 2001; 56: 800-805.
4. McNicholas WT, Rodenstein D: Sleep apnoea and driving risk: the need for regulation. Eur Respir Rev 2015; 24: 602-606.
5. Flemons WW, Buysse D, Redline S et al.: Sleep-related breathing disorders in adults. Sleep 1999; 22: 667-689.
6. Pataka A, Daskalopoulou E, Kalamaras G et al: Evaluation of five different questionnaires for assessing sleep apnea syndrome in a sleep clinic. Sleep Med 2014; 15: 776-781.
7. McNicolas WT, Walter T: New Standards and Guidelines for Drivers with Obstructive Sleep Apnoea syndrome. Report of the Obstructive Sleep Apnoea Working Group. European Commission. Directorate-General for Energy and Transport 2013.
8. Nahapetian R, Silva GE, Vana KD et al.: Weighted STOP-Bang and screening for sleep-disordered breathing. Sleep Breath 2015; 20: 597-603.
9. Ramachandran SK, Josephs LA: A Meta-analysis of Clinical Screening Tests for Obstructive Sleep Apnea. Anesthesiology 2009; 110: 928-939.
10. Collop NA, Anderson WM, Boehlecke B et al.: Clinical Guidelines for the Use of Portable Monitors in the Diagnosis of Obstructive Sleep Apnea in Adult Patients. J Clin Sleep Med 2007; 3.7: 737-747.

