Maria Wolniewicz, *Lidia Zawadzka-Głos
Idiopathic left-sided buccal abscess – a case report
Idiopatyczny ropień policzka lewego – opis przypadku
Department of Pediatric Otolaryngology, Medical University of Warsaw, Poland
Head of Department: Associate Professor Lidia Zawadzka-Głos, MD, PhD
Streszczenie
Ropnie regionu głowy i szyi to istotny problem kliniczny. Znaczącą rolę w ich powstawaniu odgrywają zakażenia zębopochodne (przede wszystkim zmiany próchnicze czy stan po zabiegach stomatologicznych), odpowiadające za ok. 1/3 stanów zapalnych policzka. Właściwa diagnoza jest kluczowa dla ustalenia drogi postępowania terapeutycznego. Wśród dostępnych metod leczenia wyróżniamy antybiotykoterapię ogólnoustrojową samodzielnie lub w połączeniu z interwencją zabiegową, bądź też rzadziej interwencja zabiegowa jako jedyne działanie. Głównym celem leczenia jest ograniczenie infekcji oraz prewencja jej dalszego rozprzestrzeniania do głębiej położonych struktur (w tym istnieje ryzyko przekroczenia bariery krew-mózg). Dla zmian obejmujących przestrzenie powierzchowne zazwyczaj wystarczające jest badanie ultrasonograficzne odpowiedniej okolicy pozwalające na wstępną ocenę, a następnie monitorowanie procesu leczenia. Alternatywą wobec badania ultrasonograficznego jest badanie rezonansem magnetycznym, pozwalające na znacznie dokładniejszą, wielowymiarową analizę zajętego obszaru i łatwiejsze zróżnicowanie tkanek, jednak jest ono znacznie droższe i trudniej dostępne, a przez to też mniej dostępne w monitorowaniu efektów leczenia. Poniżej przedstawiamy przypadek nastolatki, u której rozwinął się idiopatyczny jednostronny ropień policzka lewego.
Summary
Abscesses of the head and neck region account for an important clinical problem. They are most frequently of dental origin (mainly due to carious changes or state after dental interventions), especially when located in the buccal region (about 1/3 cases). The correct diagnosis is the key to determine the proper treatment protocol: systemic antibiotics and/or surgical procedure (usually drainage) in order to prevent further progression of the inflammatory process (including transgression of the blood-brain barrier). Ultrasound is a sufficient first line diagnostic tool for the changes localized in the superficial spaces. Additionally, it is helpful in monitoring the effectiveness of the introduced treatment. Alternatively, MRI could be used, enabling more thorough 3D visualization of the affected areas and tissues differentiation, but due to its cost and availability its role is restricted, especially in monitoring (when examination needs to be repeated regularly). Below we would like to present a case report of our teenage patient, who developed idiopathic left-sided buccal abscess.
Introduction
Abscesses of the head and neck region stand for one of the basic problems for general practitioners’ everyday practice (1). They can develop as single-space or multiple-space abscess (2). The most frequently involved are the submandibular, buccal, submental or canine spaces (2, 3). The crucial step is the right diagnosis enabling to assess the risk of purulent changes, which would further determine the proper treatment protocol: ambulatory treatment or the need of specialist surgical procedure (4, 5). Below we would like to present a case report of our teenage patient, who developed left-sided buccal abscess that required surgical intervention due to the emphasized local complaints and the evidence of an abscess in the ultrasound. Unfortunately, we could not identify one clear factor underlying for the observed inflammatory process.
Case report
Seventeen-year-old patient was admitted to our department during emergency service due to increasing swelling of the left cheek for the last few days with associated pain, without fever. She had no problems with breathing, had slightly deformed voice and suffered from problems with eating and drinking (mostly because of the pain discomfort). Physical examination on admission showed emphasized redness and edema of the left cheek, on palpation an inflammatory infiltration sized about 4 x 3 cm with fluid-filled area on pressing in its lower parts, localized superficially, was remarkable. Apart from that pronounced acnes on the face was noticeable. In laryngological examination of the mouth mucous was unremarkable, there were no carious lesions, no dental or gingival abnormalities. According to our patient she is regularly checked up by her dentist, has had no interventions recently. Her hair was dyed in various colors, she had a lot of earrings in her auricles, but denied self-piercing or other interventions in her cheek. She did not suffer from any chronic illnesses. She admitted to drinking alcohol occasionally on social meetings and smoking cigarettes, but denied drug in-take. One day before admission she was prescribed ambulatorily Amoxicillin/Clavulanic acid 1.0 g, one pill two times daily, but due to worsening of the complaints she referred to the emergency unit.
On ultrasound on admission (fig. 1, 2) an oval lesion sized 15 x 19 x 13 mm with hypoechoic, heterogenous, thick contents reflecting abscess characteristics within edematous soft tissues with marked vessels and enhanced blood-flow was described. The center of the lesion was localized superficially, about 5 mm beneath the skin surface. On laboratory tests WBC was normal, CRP was at the boundary of the norm (1.0 with the norm 0.0-1.0).
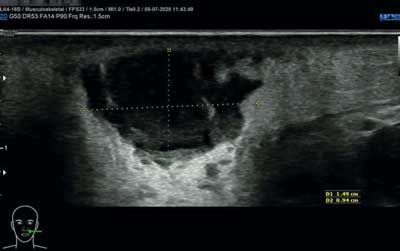
Fig. 1. Ultrasound on admission – oval lesion sized 15 x 19 x 13 mm with hypoechoic, heterogenous, thick contents, edema of the surrounding soft tissues – image reflecting an abscess
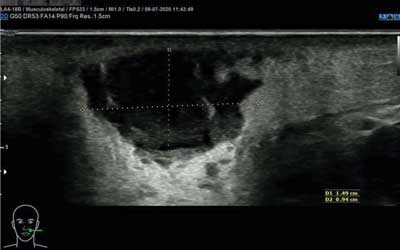
Fig. 2. Ultrasound on admission – edema within soft tissues, marked vessels with enhanced blood-flow surrounding the abscess
Continuation of the introduced ambulatorily Amoxicillin/Clavulanic acid in a does 1.2 g, 3 times daily, intravenously with additional Clindamycin 900 mg 3 times daily was planned. Moreover, our patient was qualified for the drainage of the abscess. The surgical intervention from the intraoral access was performed on the 2nd day of hospitalizations in general anesthesia as soon as we got SARS-CoV-2 results. A large amount of thick pus was drained from the lesion and sent for microbiological examination. During procedure ultrasound navigation was not used. The puncture of the lesion, followed by a drainage were performed after palpation and fixation of the cheek in the position, in which the lesion was best marked. The abscess’s cavity and the mouth were rinsed generously with Octenidine dihydrochloride (Octenisept), and then 0.9% natrium saline. Regular rinsing of the mouth with the solution of Octenidine dihydrochloride (Octenisept) and 0.9% natrium saline in a ratio 1:1 three times daily together with mechanical broadening of the abscess cavity were continued on the ward. Pus combined with blood was obtained till the 3rd day post-operatively during mechanical broadening when a serous content appeared and as a result it was decided to stop further interventions. With the course of treatment gradual relief of patient’s complaints and local improvement (diminished edema, inflammatory infiltration and blood flow resulting in reduced redness, no palpable fluid area) were observed. On the 7th day of antibiotic therapy we received microbiological results, which revealed growth of aerobic bacteria Citrobacter freundii and Enterococcus faecalis, with no resistance for standard antibiotics and at the same time prone to applied treatment (tab. 1).
Tab. 1. Microbiology results – antimicrobial resistance
| Antibiotics/identification | Citrobacter freundii ESBL- | Enterococcus faecalis |
| Susceptibility | MIC | Susceptibility | MIC |
| Ampicillin | | | S | |
| Piperacillin/Tazobactam | S | ≤ 4 | | |
| Cefotaxime | S | ≤ 0.25 | | |
| Cefepime | S | ≤ 0.12 | | |
| Amikacin | S | ≤ 2 | | |
| Gentamycin | S | ≤ 1 | | |
| Tobramycin | S | ≤ 1 | | |
| Linezolid | | | S | |
| Teicoplanin | | | S | |
| Vancomycin | | | S | |
| Trimethoprim/Sulfamethoxazole | S | ≤ 20 | | |
| Streptomycin – high concentration | | | S | |
| Gentamycin – high concentration | | | S | |
S – susceptible to standard dose of an antibiotics
We performed control ultrasound (fig. 3, 4) in order to verify observed clinical improvement and to exclude persistence of any fluid/pus concentrations. It showed no evidence of an abscess. A lesion sized around 7 x 5 x 10 mm – the remainder of a drained abscess and a fistula of 15 mm length and 0.5-1.5 mm diameter – the effect of a performed procedure were described. After delivery of microbiology results due to good general condition of the patient she was discharged from the hospital with recommendation to continue Amoxicillin/Clavulanic acid 1.0 g, one pill two times daily for the next 7 days, followed by ultrasound examination and laryngological check-up, together with dental consultation.
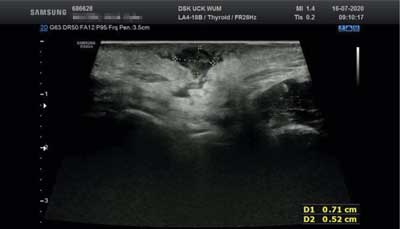
Fig. 3. Ultrasound before discharge from the hospital – the remainder of a drained abscess, sized around 7 x 5 x 10 mm, with no evidence of pus/fluid
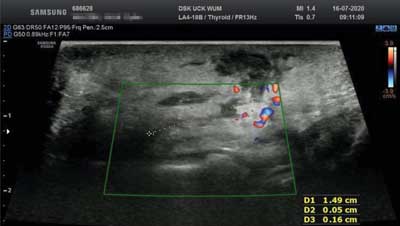
Fig. 4. Ultrasound before discharge from the hospital – the effect of a performed procedure, fistula of 15 mm length and 0.5-1.5 mm diameter, with no enhanced blood-flow or edema in surrounding tissues
Discussion
The buccal space consists anatomically of a few layers, namely (from the outside) skin, the adipose tissue (called buccal fat pad), the buccopharyngeal fascia, the masseter muscle (infiltrated by the duct of the parotid gland), buccal glands (mucoserous) and finally, the inner layer of the mucous tissue of the oral cavity. Anteriorly, the cheek sticks to the mimic muscles of the face and their fascia, laterally borders with the parotid gland and its fascia, medially with the maxillary alveolar ridge and posteriorly with the zygomatic fascia. Fascial coverings separating the buccal space from the surrounding tissues are not complete, which promotes local spread of the inflammatory processes in this region (6).
Dental infections stand for a predominant causative factor (carious lesions, dental or gingival abnormalities, post-intervention state) of all abscesses of the head and neck region (2, 7), especially for the inflammatory changes incorporating the buccal space (almost 1/3 infections of dental origin) (2, 3, 6, 8, 9). The correct diagnosis and its proper treatment are very important so as to prevent further spread of the inflammation to the deeper spaces, among which there is a risk of infiltrating the natural blood-brain barrier (9). In our case we did not identify a straightforward cause of the formed abscess. On laryngological examination of the oral cavity no oral lesions were detected, but our patient was referred to her dentist for a thorough check-up to finally exclude dental origin. Physical examination revealed enhanced acnes of the buccal skin, plenty spots on the face for earrings with co-existing syndrome of a young adult’s rebellion (alcohol, smoking, dyed hair), which altogether aroused our suspicions of a coincidence of this features as a possible causative factor.
The gold standard for soft tissue imaging is MRI (5, 9). However, it is a diagnostic tool of a worse availability and despite its good reproducibility much more expensive (5). It is worth mentioning that most of the head and neck structures are located relatively superficial, in a range from 1 to 5 cm, what makes ultrasound a perfect tool to diagnose its pathologies (4-6). On the other hand, such imaging, due to the variety of soft tissues is a difficult task and requires experience in its assessment, basing on the differences in the echogenicity of the defined anatomical structures. According to literature, tissues’ collagen concentration is considered to be the ground of those differences (10). Fascial spaces could stand for a diagnostic hint, because in physiological state they are practically unnoticeable (they form so called potential spaces), but when a pathology, such as pus, blood occurs or after a surgical intervention they are marked (4-6).
There are certain ultrasound features that are observed in the buccal swellings associated with the abscess. They include: the increased distance of soft tissue from skin to oral mucosa, well defined anatomical layers, the loss of the integrity of the subcutaneous tissue and/or muscle (due to lytic properties of bacterial enzymes), acoustic accentuation (reflecting fluid accumulation) (4). In the clinical material od Srinivas et al. in the majority of described cases the shape of the local lesion was irregular, and its content either hypo- (54.2%) or anechoic (45.8%) (6). Mass effect was detected only in 3 cases (12.5%). Ultrasound enabled also to distinguish between the cellulitis and the abscess, which is clinically important when deciding on the right treatment protocol. What is more, there is high sensitivity in detecting subcutaneous fluid compartments, even among less experienced doctors (5). It enables quick clinical assessment and verification of suspicions aroused in physical examination (5). If an abscess is confirmed it is recommended to perform a surgical drainage, apart from systemic antibiotics, as it is a structure of poor antibiotics’ penetration (1, 5, 6, 9).
In a comparative study of ultrasound versus MRI for superficial space infections of the head and neck region, incorporating the buccal, canine, suborbital, submandibular, submental or masseter spaces both imaging methods seemed to show similar accuracy in its assessment (8). In our case ultrasound was a sufficient tool to set the diagnosis of the superficial abscess and to determine indications for an effective treatment. The lesion was of an oval shape, contained hypoechoic fluid, while surrounding tissues showed features of the local inflammatory process. The superiority of the MRI was evidently marked for the deep space infections (parapharyngeal, retropharyngeal or sublingual space) due to disturbed penetration of the ultrasound waves or technical problems with the direct visualization of the involved area (sublingual space) (8).
In the same analysis it was noticed that ultrasound can help to differentiate between various stages of the inflammatory process, and then to trace its progress: edematous changes, cellulitis, preabscess, and complete abscess formation (4, 8, 11). In our example, because of a satisfying treatment response in clinical assessment, there was no need in repeating ultrasound examinations. However, according to our standard protocol, we performed an ultrasound visualization before discharge so as to definitely exclude any pus concentration and on that basis to finish intravenous treatment. We planned another follow-up ultrasound at the end of the ambulatory treatment. An useful advantage of the ultrasound is also the possibility of an intraoperative navigation enabling localization of small or difficult to find lesions (4, 8), which was not necessary in our case due to superficial and relatively easy visible location of the abscess. It is also worth mentioning that we performed the drainage from intraoral access to minimalize esthetic defects after healing.
The bacterial growth from the abscesses of the head and neck region is diversified, ranging both from aerobic and anaerobic species (12). According to the literature, in some researches aerobic species are the dominant ones, while in others the anaerobes are mostly cultured (1, 2). This difference can sometimes result from the method of sampling: smear or aspiration (with the prevalence of the anaerobes during aspiration) (2). It is also stated that early stage infections are usually of aerobic origin with a tendency of the anaerobes’ engagement in the prolonged inflammatory processes (3). Among aerobes the most commonly isolated species are Streptococcus viridans, beta-hemolytic Streptococcus, Staphylococcus, while Bacteroides and Peptostreptococcus prevail in the anaerobes (2, 3, 8, 9). In the most microbiological cultures more than 1 species are isolated (2, 7), on average even 2.6 species per 1 patient (2). Our microbiological results do not belong to the most typical ones, but they are mentioned in literature (9). Bacteria Citrobacter freundii is a Gram-negative bacteria that physiologically lives in the human gastrointestinal tract, often compared with Salmonella or Escherichia species. However, there are situations, in which it can promote infections locally presenting as diarrhea, as well as serious opportunistic systemic infections within predisposed patients (serious gastrointestinal infections, urinary tract infections, respiratory tract infections, peritonitis, endocarditis, wound infections, bacteremia and sepsis, meningitis) (13). The mortality rate for meningitis caused by Citrobacter freundii is very high, ranging 25-50% and the chronic persistent complications are estimated at the level of 75% (13). According to the literature, there is a high resistance of Citrobacter freundii against standard antibiotics (3rd generation cephalosporins, piperacillin, ciprofloxacin and amikacin) (13). In our patient’s history we did not find any factors predisposing for a serious Citrobacter freundii infection, her response to empirical treatment was good. This was also proved in the microbiological results – resistance for the typical antibiotics was excluded.
Sometimes cultures are negative despite evident pus infections, which can be due to bacterial high sensitivity to the methods of transportation, bacterial growth in the organized form of a biofilm unable to asses in classic analysis or as a result of the previously introduced treatment (3).
Bacteria from the Streptococcus viridans group are characterized by a good susceptibility to penicillin, while Staphylococcus are usually reluctant, with good response to cefazoline, ciprofloxacin, clindamycin or vancomycin (2). Standard empirical antibiotics therapy is composed of antibiotics from penicillin groups, sometimes beta lactams or combined with beta lactamase inhibitors (3), together with metronidazole (directed anti-anaerobes) or clindamycin alone (7), both variants showing similar efficacy (7). It is advisable to narrow down antibiotic spectrum after getting microbiological results (7, 9). Aerobes are susceptible to amoxicillin/clavulanic acid in 71%, anaerobes in 45%, while 73% anaerobes respond good to metronidazole (3), what explains supplementary treatment of these antibiotics. In one paper it was analyzed whether conjoined treatment of metronidazole and amoxicillin/clavulanic acid have advantage over amoxicillin/clavulanic acid in monotherapy. It turned out that it is not always necessary, and even not recommended for generally healthy patients with less intensified symptoms of inflammatory process or only 1 fascial space incorporated (3). In some cases, on the other hand, the decision of adding another antibiotic should be taken after local assessment during drainage (the excess of involved tissues) or after poor response to the introduced treatment (what can suggest resistance) (3).
The assessment of the treatment response bases on the fever wear off, reduction or normalization of the inflammatory parameters (WBC, CRP) within 24 hours from the start of the treatment, which should correlate with the local improvement (3, 4). It is especially essential when assessing the effectiveness in young children, when the communication is harder due to the age border and the fear from contact with the medical staff. This correlation was useless in our case due to the lack of fever and normal inflammatory parameters on admission, what can happen in 30% of patients with abscesses in this region (3).
Conclusions
The abscesses of the head and neck region stand for an essential clinical problem, both from the patient’s perspective connected with intensive pain and its impact on eating, speech quality or esthetical issues, as well as doctor’s perspective who is conscious of the possible consequences of the hazardous spread to deeper spaces and structures of untreated or improperly treated cases. Therefore, it is very important to diagnose the patient quickly and introduce the correct treatment protocol, sometimes combined with surgical intervention (4, 12). Widely available and relatively easy to use for imaging is the ultrasound examination, which helps in the 1st line assessment and indicates the need for specialist intervention. It can also be repeatedly performed allowing for regular follow-up (4). Edematous changes or cellulitis can be treated ambulatorily, preabscess requires watchful observation, while complete abscess formation should be drained. The mean-time treatment of the widespread antibiotics therapy (ambulatorily, intravenous or a combination of both) is between 7 and 14 days, sometimes even longer, depending on the clinical effects of the treatment. The basic criteria enabling to withdraw from the antibiotics is the exclusion of any abscesses’ formations. Due to the localization and known ways of the possible infection spread, in all abscesses of the head and neck region a specialist dental consultation should be an inseparable element of the patient care.
Piśmiennictwo
1. Simo R, Hartley C, Rapado F et al.: Microbiology and antibiotic treatment of head and neck abscesses in children. Clin Otolaryngol Allied Sci 1998; 23(2): 164-168.
2. Rega AJ, Aziz SR, Ziccardi VB: Microbiology and Antibiotic Sensitivities of Head and Neck Space Infections of Odontogenic Origin. J Oral Maxillofac Surg 2006; 64(9): 1377-1380.
3. Bali R, Sharma P, Gaba S: Use of metronidazole as part of an empirical antibiotic regimen after incision and drainage of infections of the odontogenic spaces. Br J Oral Maxillofac Surg 2015; 53(1): 18-22.
4. Ramirez-Schrempp D, Dorfman DH, Baker WE, Liteplo AS: Ultrasound soft-tissue applications in the pediatric emergency department: to drain or not to drain? Pediatr Emerg Care 2009; 25(1): 44-48.
5. Coticchia JM, Getnick GS, Yun RD, Arnold JE: Age-, Site-, and Time-Specific Differences in Pediatric Deep Neck Abscesses. Arch Otolaryngol Head Neck Surg 2004; 130(2): 201-207.
6. Srinivas K, Sumanth KN, Chopra SS: Ultrasonographic evaluation of inflammatory swellings of buccal space. Indian J Dent Res 2009; 20: 458-462.
7. Bhagania M, Youseff W, Mehra P, Figueroa R: Treatment of odontogenic infections: An analysis of two antibiotic regimens. J Oral Biol Craniofac Res 2018; 8(2): 78-81.
8. Bassiony M, Yang J, Abdel-Monem TM et al.: Exploration of ultrasonography in assessment of fascial space spread of odontogenic infections. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 2009; 107(6): 861-869.
9. Chow AW: Complications, diagnosis, and treatment of odontogenic infections. UpToDate, This topic last up dated: Jun 17, 2019.
10. Rosenfield AT, Taylor KJ, Jaffe CC: Clinical applications of ultrasound tissue characterization. Radiol Clin North Am 1980; 18: 31-58.
11. Siegert R: Ultrasonography of inflammatory soft tissue swellings of the head and neck. J Oral Maxillofac Surg 1987; 45: 842-846.
12. Ungkanont K, Yellon RF, Weissman JL et al.: Head and neck space infections in infants and children. Otolaryngol Head Neck Surg 1995; 112(3): 375-382.
13. Pobucewicz A, Czernomysy-Furowicz D: Characteristics of Citrobacter freundii, with special of their ability to produce toxins. Post Mikrobiol 2010; 40(1): 43-46.



