Tomasz Lis, *Lidia Zawadzka-Głos
Diagnosis and evaluation of a child suspected for obstructive sleep apnea: an overview
Diagnoza i ocena dziecka z podejrzeniem obturacyjnego bezdechu sennego: przegląd
Department of Pediatric Otolaryngology, Medical University of Warsaw, Poland
Head of Department: Associate Professor Lidia Zawadzka-Głos, MD, PhD
Streszczenie
Obturacyjny bezdech senny (OBS) jest często występującym zaburzeniem w populacji pediatrycznej, charakteryzującym się blokadą dróg oddechowych w trakcie snu, prowadzącym do wielu niekorzystnych efektów zdrowotnych. Te dotyczą przede wszystkim układu sercowo-naczyniowego, funkcji poznawczych i metabolizmu. Wczesna diagnoza OBS jest ważna, aby zapobiec poważnym negatywnym konsekwencjom zdrowotnym. W tej pracy przeglądowej zawarliśmy bieżącą wiedzę dotyczącą oceny dziecka z podejrzewanym OBS. Skupiliśmy się na możliwościach diagnostycznych, do których należą nadzorowane badania w laboratorium snu, z polisomnografią (PSG), pozostającą złotym standardem diagnostyki OBS u dzieci, oraz szeroko rozwijanymi domowymi badaniami bezdechu sennego (HSAT – home sleep apnea testing) należącymi do badań ambulatoryjnych. Kolejna przedstawiona kwestia dotyczy dostępnych technik ewaluacji. Do tych należą badanie podmiotowe i przedmiotowe oraz kwestionariusze jakości snu. Ewaluacja jest również oparta na badaniach endoskopowych przy użyciu giętkich fiberoskopów oraz szerokiej puli radiologicznych badań obrazowych. Te dwie formy obrazowania pomagają zidentyfikować miejsce lub miejsca występującej obstrukcji dróg oddechowych.
Summary
Obstructive sleep apnea (OSA) is a frequent disorder in pediatric population characterized by airway blockage while asleep, leading to many adverse health effects. These involve foremost cardiovascular, neurocognitive, and metabolic systems. Early identification of OSA patient is crucial in order prevent serious negative health consequences. In this review article we provide up-to-date overview concerning assessment of a child with suspected OSA. We focus on available diagnostic modalities, which include attended in-lab sleep studies, with polysomnography (PSG) remaining a gold standard in diagnosing OSA in children, and widely developed home sleep apnea testing (HSAT) belonging to ambulatory sleep studies. The other presented matter apply to available evaluation techniques. These feature history and physical examination as well as sleep questionaires. Evaluation is also based on endoscopic procedures using mainly flexible devices, as well as wide variety of radiology imaging modalities. These two forms of imaging are used to help to identify site or sites of airway obstruction.
Introduction
Obstructive sleep apnea (OSA) is a common sleep-related breathing disorder (SRBD) characterized by episodes of complete and/or partial upper airway obstruction during sleep, followed by alteration in gas exchange. According to recent American Academy of Sleep Medicine (AASM) guidelines (1), diagnostic criteria for pediatric OSA include presence of one or more clinical symptoms as well as one or both polysomnographic (PSG) findings:
1. clinical criteria (A criteria):
– snoring,
– laboured/obstructive breathing,
– daytime consequences (sleepiness, hyperactivity, behavioral problems),
2. polysomnographic criteria (B criteria):
– one or more obstructive event per hour of sleep,
– obstructive hypoventilation, manifested by partial pressure of carbon dioxide (PaCO2) > 50 mmHg for at least 25 percent of total sleep time, coupled with snoring, paradoxical thoracoabdominal movement, or flattening of the nasal airway pressure waveform.
This study focuses on describing different possibilities to diagnose and evaluate child with suspected OSA and does not take into account indications to use certain diagnostic method, which may vary depending on guidelines, e.g. indications for PSG according to AASM, American Academy of Pediatrics (AAP) and American Academy of Otolaryngology-Head and Neck Surgery Foundation (AAO-HNSF). In some cases though, usually when these guidelines comply with each other, indications are presented.
Epidemiology
The estimated prevalence of pediatric OSA range between 1 to 5% (2). It affects mostly children between two and eight years of age (2), which coincides with the peak age of the overgrowth of the upper airways’ lymphatic tissue.
Untreated OSA is associated with academic difficulties, behavioral and neurocognitive problems (3, 4), cardiovascular complications (5-7), metabolic disorders (7) as well as failure to thrive (8). Additionally children with OSA are more likely to have significant decrease in quality of life (4). Early identification and treatment can prevent or reverse many of these negative health effects. Nonetheless, diagnosis is often delayed.
Risk factors
Adenotonsillar hypertrophy and obesity are recognized as the most significant risk factors for OSA in otherwise healthy children. Other risk contributors to OSA include craniofacial anomalies, and neuromuscular disorders (9). Examples of certain conditions associated with SRBD are in listed in table 1 (10) (fig. 1, tab. 1).

Fig. 1. Tonsillar hypertrophy
Tab. 1. Conditions associated with an elevated prevalence for SRBD (including OSA)
| High risk for SRBD | Intermediate risk for SRBD |
| Obesity | History of prematurity |
| Down syndrome | African American race |
| Prader-Willi syndrome | Family history of OSA |
| Duchenne muscular dystrophy | Allergic rhinitis |
| Achondroplasia | |
| Pierre Robin sequence | |
| Craniofacial dysostoses | |
| Chiari malformations and myelomeningocele | |
Children suffering from above demonstrated, especially high-risk complex-conditions, should be supervised for signs and symptoms of OSA. If present, PSG is usually recommended in such patients.
Diagnosis
Attended in-lab studies
The gold standard test for the diagnosis of OSAS and assessment of its severity is an overnight, attended, in-laboratory PSG. Following parameters are recorded during a typical PSG examination in children: electroencephalography (EEG), bilateral electrooculography (EOG), submental electromyography (EMG), limb movement, electrocardiography (ECG), snoring, airflow, respiratory effort, blood oxygenation, end-tidal or transcutaneous capnography, body position and behavioral observation (video monitoring system).
Nap PSG is an abbreviated study which may be conducted in children who could go asleep in the sleep laboratory during daytime. It is not as reliable as overnight PSG and is not recommended for definite diagnosis of obstructive sleep apnea syndrome in children (10).
Obstructive events recorded on PSG are summarized by the apnea-hypopnea index (AHI), which represents the average number of apneas and hypopneas per hour of sleep. There are special pediatric scoring rules for OSA severity, which are practice-derived and not evidence based. These are presented in table 2.
Tab. 2. OSA severity according to AHI
| OSA severity | AHI (events/h) |
| Mild | 1 to 4.9 |
| Moderate | 5 to 9.9 |
| Severe | > 10 |
There is a lack of consensus regarding the exact values of AHI to define OSA severity as well as what are the cutoff points to use adult criteria for the diagnosis of OSA in older children (for adolescents between 13 and 18 years old pediatric scoring rules are optional according to AASM). Therefore, there is a need for investigation of different diagnostic modalities or formulate more adequate criteria.
Ambulatory studies
Home sleep apnea testing (HSAT), which are unattended studies usually with limited montage, may be more economical and accessible option to diagnose OSA in children.
Home-based PSG, although not supervised, present a valuable research tool in school-aged children (11).
Ambulatory polygraphy, which does not include EEG, EOG, EMG in the montage, is an effective diagnostic technique for OSA in adults. In children, as the further HSAT modalities, it tends to underestimate presence of OSA and its severity, thus may be not sufficient to exclude OSA (12).
Devices using peripheral arterial tonometry (PAT) present high correlations for AHI in adults (13). Comprehensive studies in children are awaited.
Portable diagnostic tools that centre on ambulatory end-tidal capnography, due to unreliability, seem not yet able to be implemented in clinical practice (14).
Overnight oximetry is based on monitoring pulse rate, pulse amplitude, and oxygen saturation of blood during sleep. The study assessed using the McGill score has a relatively good positive predictive value but poor negative predictive value (15).
Video recordings at home during sleep are reported to a remarkable screening method for OSA in children (16).
Evaluation
History and physical examination
The symptoms of OSA include nocturnal symptoms and diurnal symptoms. Snoring is recognized as the most common nocturnal symptom of OSA. Still, not every child who snore, even habitually (more than 3 times a week), suffer from OSA. Daytime symptoms are characterized among others by excessive daytime sleepiness.
Besides the detailed assessment of the oropharynx, physical examination of a child with suspected OSA should take into account height, weight, evaluation of facial anatomy and cardiovascular system. There has been reported discordance between the tonsillar size and reported severity of OSA (17), which proves that even a thorough physical examination is not sufficient to diagnose OSA.
The symptoms and signs of OSA are listed in table 3 (9).
Tab. 3. Symptoms and signs of OSA
| History |
| Frequent snoring (> 3 nights/week) |
| Labored breathing during sleep |
| Gasps/snorting noises/observed episodes of apnea |
| Sleep enuresis |
| Sleeping in a seated position or with the neck hyperextended |
| Cyanosis |
| Headaches on awakening |
| Daytime sleepiness |
| Attention-deficit/hyperactivity disorder |
| Learning problems |
| Physical examination |
| Underweight or overweight |
| Tonsillar hypertrophy |
| Adenoidal facies |
| Micrognathia/retrognathia |
| High-arched palate |
| Failure to thrive |
| Hypertension |
Questionnaires
Several questionnaires have been developed to identify children at risk for OSA. The most popular one is Pediatric Sleep Questionnaire-Sleep Related Breathing Disorder (PSQ-SRDB) which is widely used and validated. The other example is short and simple I’M SLEEPY questionnaire.
Although, sleep questionnaires are useful screening tools, especially when access to in-lab PSG is limited, they can not replace it.
Endoscopy
Endoscopy in OSA favors flexible devices because they enable to assess all of the anatomic sites where obstruction could occur: nasal cavity, nasopharynx, the posterior oropharynx and lateral pharyngeal walls, base of the tongue, and the supraglottic larynx. The sites of narrowing with possible source of problem are presented in table 4.
Tab. 4. Sites of narrowing in upper airways with a possible source of obstruction, based on (18)
| Site of obstruction | Possible source |
| Nasal cavity | Septal deviation |
| Nasal turbinates hypertrophy |
| Nasopharynx | Adenoid hyperthropy |
| Maxillary hypoplasia |
| Oropharynx | Tonsillar hyperthropy |
| Soft palate redundancy |
| Tongue | Lingual tonsil hyperthropy |
| Retroglossal narrowing |
| Glossoptosis |
| Micrognathia/rethrognathia |
| Larynx | Laryngomalacia – congenital |
| Laryngomalacia – sleep state dependent |
Awake flexible endoscopy can help to assess sites of obstruction, such as enlarged adenoid in nasopharynx. The examination requires cooperation with pediatric patient.
Drug-induced sleep endoscopy (DISE) provides evaluation of upper airways during sedation. It has been shown that sites of obstruction during sleep not always correlate with awake nasopharyngoscopy findings (19). In spite of clear benefits, there is lack of consensus regarding grading system of DISE and a choice of appropriate anesthetic agent to obtain an induced sleep state (20, 21).
Radiology imaging
Recently Slaats et al. summarized different radiological techniques which have been used to evaluate the anatomical alterations in upper airway and their role in the pathogenesis of OSA in children (22). These techniques include lateral neck radiography, cephalometry, computed tomography (CT), magnetic resonance imaging (MRI) and functional imaging.
Some of these imaging techniques may be performed either or both in erect and supine position. As there is an explicit reduction in airway size when changing from upright to horizontal position, techniques such as MRI, multi-slice CT (MSCT) and supine cone-beam CT (CBCT) are preffered (23).
Lateral neck radiography and cephalometry are simple, widely available and come with a small amount of radiation. And though lateral neck X-ray has relatively good predictive values for the diagnosis of OSA, there are limited data on the usefulness of cephalometry (fig. 2).
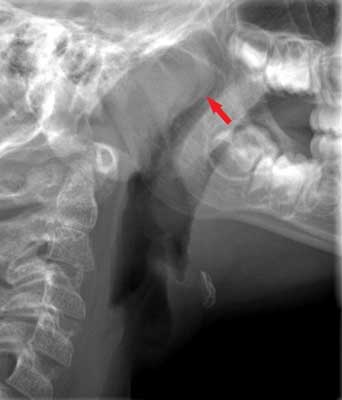
Fig. 2. Adenoid hypertrophy: lateral neck multi-slice CT (MSCT) radiography
CT and MRI offer deeper insight into upper airway structures as a result of the ability to assess them in three planes.
MSCT employs larger radiation dose which is much lower for CBCT. Still the image from CBCT may be not satisfactory due to not providing soft tissue detail.
MRI is performed under mild sedation and doesn’t come with radiation exposure. MRI and in particular its special sequence – cine-MRI (as in cinema) is the most accurate imaging method for evaluating the soft tissues surrounding the airway. It is shown to identify the site or sites of obstruction in up to 93% of cases (24). The major limitation is its cost and availability.
At last, computed functional dynamics (CFD) based on CT and MRI images, give more insight into performance of upper airways, monitoring its flow characteristics and aerodynamic forces. However, there are only limited data available about clinical usage of these modalities and they need to be further investigated.
Conclusions
In summary, OSA is a complex disorder which need multi-layered approach. Assessment of a child suspected for OSA should be based on through history and physical examination. Sleep questionaries are valuable tools but alone are not sufficient to diagnose OSA. The diagnostic standard for OSA remains nocturnal attended in-lab PSG study. However, the development of HSAT devices proceed. Evaluation usually consists of endoscopy and imaging among which DISE and cine-MRI are worth mentioning respectively.
Piśmiennictwo
1. Sateia MJ: International classification of sleep disorders-third edition: highlights and modifications. Chest 2014; 146(5): 1387-1394.
2. Tan HL, Gozal D, Kheirandish-Gozal L: Obstructive sleep apnea in children: a critical update. Nat Sci Sleep 2013; 5: 109-123.
3. Beebe DW, Ris MD, Kramer ME et al.: The association between sleep disordered breathing, academic grades, and cognitive and behavioral functioning among overweight subjects during middle to late childhood. Sleep 2010; 33(11): 1447-1456.
4. Mitchell RB, Kelly J: Behavior, neurocognition and quality-of-life in children with sleep-disordered breathing. Int J Pediatr Otorhinolaryngol 2006; 70(3): 395-406.
5. Marcus CL, Greene MG, Carroll JL: Blood pressure in children with obstructive sleep apnea. Am J Respir Crit Care Med 1998; 157(4 Pt 1): 1098-1103.
6. Li AM, Au CT, Sung RY et al.: Ambulatory blood pressure in children with obstructive sleep apnoea: a community based study. Thorax 2008; 63(9): 803-809.
7. Sun SS, Grave GD, Siervogel RM et al.: Systolic blood pressure in childhood predicts hypertension and metabolic syndrome later in life. Pediatrics 2007; 119(2): 237-246.
8. Nieminen P, Löppönen T, Tolonen U et al.: Growth and biochemical markers of growth in children with snoring and obstructive sleep apnea. Pediatrics 2002; 109(4): e55.
9. Marcus CL, Brooks LJ, Draper KA et al.: Diagnosis and management of childhood obstructive sleep apnea syndrome. Pediatrics 2012; 130(3): e714-755.
10. Aurora RN, Zak RS, Karippot A et al.: Practice parameters for the respiratory indications for polysomnography in children. Sleep 2011; 34(3): 379-388.
11. Marcus CL, Traylor J, Biggs SN et al.: Feasibility of comprehensive, unattended ambulatory polysomnography in school-aged children. J Clin Sleep Med 2014; 10(8): 913-918.
12. Tan HL, Kheirandish-Gozal L, Gozal D: Pediatric Home Sleep Apnea Testing: Slowly Getting There! Chest 2015; 148(6): 1382-1395.
13. Choi JH, Kim EJ, Kim YS et al.: Validation study of portable device for the diagnosis of obstructive sleep apnea according to the new AASM scoring criteria: Watch-PAT 100. Acta Otolaryngol 2010; 130(7): 838-843.
14. Fishman H, Massicotte C, Li R et al.: The Accuracy of an Ambulatory Level III Sleep Study Compared to a Level I Sleep Study for the Diagnosis of Sleep-Disordered Breathing in Children With Neuromuscular Disease. J Clin Sleep Med 2018; 14(12): 2013-2020.
15. Brouillette RT, Morielli A, Leimanis A et al.: Nocturnal pulse oximetry as an abbreviated testing modality for pediatric obstructive sleep apnea. Pediatrics 2000; 105(2): 405-412.
16. Sivan Y, Kornecki A, Schonfeld T: Screening obstructive sleep apnoea syndrome by home videotape recording in children. Eur Respir J 1996; 9(10): 2127-2131.
17. Nolan J, Brietzke SE: Systematic review of pediatric tonsil size and polysomnogram-measured obstructive sleep apnea severity. Otolaryngol Head Neck Surg 2011; 144(6): 844-850.
18. Ehsan Z, Ishman SL: Pediatric Obstructive Sleep Apnea. Otolaryngol Clin North Am 2016; 49(6): 1449-1464.
19. Fishman G, Zemel M, DeRowe A et al.: Fiber-optic sleep endoscopy in children with persistent obstructive sleep apnea: inter-observer correlation and comparison with awake endoscopy. Int J Pediatr Otorhinolaryngol 2013; 77(5): 752-755.
20. Wilcox LJ, Bergeron M, Reghunathan S, Ishman SL: An updated review of pediatric drug-induced sleep endoscopy. Laryngoscope Investig Otolaryngol 2017; 2(6): 423-431.
21. Friedman NR, Parikh SR, Ishman SL et al.: The current state of pediatric drug-induced sleep endoscopy. Laryngoscope 2017; 127(1): 266-272.
22. Slaats MA, Van Hoorenbeeck K, Van Eyck A et al.: Upper airway imaging in pediatric obstructive sleep apnea syndrome. Sleep Med Rev 2015; 21: 59-71.
23. Camacho M, Capasso R, Schendel S: Airway changes in obstructive sleep apnoea patients associated with a supine versus an upright position examined using cone beam computed tomography. J Laryngol Otol 2014; 128(9): 824-830.
24. Manickam PV, Shott SR, Boss EF et al.: Systematic review of site of obstruction identification and non-CPAP treatment options for children with persistent pediatric obstructive sleep apnea. Laryngoscope 2016; 126(2): 491-500.

