Wiktoria Olińska1, 2, Jure Urbančič1, 3, Piotr Kwast4, *Lidia Zawadzka-Głos4
Children who underwent tonsillectomy due to OSAS have significantly bigger tonsils than those with hypertrophic tonsils without OSAS
Pacjenci pediatryczni skierowani do zabiegu wycięcia migdałków z powodu OBPS mają znacząco większe migdałki w porównaniu do grupy pacjentów z przerostem migdałków bez współtowarzyszącego OBPS
1Faculty of Medicine, University of Ljubljana, Slovenia
Head of Faculty: prof. dr Igor Švab, PhD med
2Pediatric Otolaryngology Student Scientific Group, Medical University of Warsaw, Poland
Tutor: lek. Piotr Kwast
3Department of Otorhinolaryngology and Cervicofacial Surgery, University Medical Center Ljubljana, Slovenia
Head of Department: Prof. dr Irena Hočevar Boltežar, PhD med
4Department of Pediatric Otolaryngology, Medical University of Warsaw, Poland
Head of Department: Associate Professor Lidia Zawadzka-Głos, MD, PhD
Streszczenie
Wstęp. Tonsillektomia jest jedną z najczęściej wykonywanych operacji w oddziałach otolaryngologicznych. Do głównych wskazań do jej wykonania należy przerost migdałków podniebiennych bez lub z towarzyszącym obturacyjnym bezdechem podczas snu oraz nawracające infekcje gardła. Wielkość migdałków u dzieci kwalifikowanych do tonsillektomii z rozpoznanym obturacyjnym bezdechem podczas snu może różnić się od wielkości migdałków w grupie bez rozpoznanych bezdechów.
Cel. Porównanie cech morfologicznych migdałków u dzieci po przebytym zabiegu tonsillektomii z oraz bez współwystępującego obturacyjnego bezdechu podczas snu (OBPS).
Materiał i metody. Badanie retrospektywne przeprowadzone w latach 2011-2020 obejmujące pacjentów w wieku poniżej 18 roku życia po przebytym zabiegu wycięcia migdałków w Oddziale Otolaryngologii Uniwersytetu Medycznego w Ljubljanie.
Wyniki. Wśród 824 pacjentów włączonych do badania, 96 miało wykonany zabieg wycięcia migdałków z powodu OBPS, a 728 z powodu przerostu migdałków bez współtowarzyszącego obturacyjnego bezdechu sennego. Obydwie grupy były porównywalne pod względem średniego wieku pacjentów oraz płci, natomiast wielkość migdałków statystycznie się różniła w obydwu grupach (p=0.01). W grupie pacjentów bez OBPS przeważały duże migdałki (stopień 3/4 u 47% pacjentów), a w grupie z OBPS bardzo duże (stopień 4/4 u 53% pacjentów).
Wnioski. Pacjenci pediatryczni porównywalni pod względem wieku i płci po przebytych zabiegach całkowitej i częściowej tonsillektomii ze współwystępującym OBPS mieli znacząco większe migdałki niż pacjenci z przerostem migdałków bez OBPS.
Summary
Introduction. Tonsillectomy is one of the most commonly performed procedures in otolaryngology departments. Main indications include tonsil hypertrophy with or without obstructive sleep apnea and recurrent throat infections. The size of tonsils in the group of children qualified for tonsillectomy with obstructive sleep apnea may differ from the size of tonsils in the group without obstructive sleep apnea.
Aim. Comparison of morphological features of tonsils in children with and without OSAS undergoing tonsillectomy.
Material and methods. Retrospective study conducted from 2011 until 2020, including patients under 18 years old who underwent a total or partial tonsillectomy at the Department of Otorhinolaryngology at the University Medical Center in Ljubljana.
Results. Among 824 patients included in the analysis, 96 underwent tonsillectomy due to OSAS and 728 due to tonsil hypertrophy without OSAS. Both groups were comparable in terms of mean age and sex distribution. Tonsil size statistically differed in both groups (p = 0.01), with the prevalence of big tonsils (grade 3 of 4) in the non-OSAS group (in 47% of patients) and large tonsils (grade 4 of 4) in the OSAS group (in 53% of patients).
Conclusions. In age and sex-matched groups of children who underwent total or partial tonsillectomy, patients who underwent the procedure due to OSAS had bigger tonsils than those with hypertrophy without OSAS.
Introduction
Tonsillectomy is one of the most commonly performed procedures in otolaryngology departments. Main indications can be divided into two groups: infectious: chronic tonsillitis, peritonsillar abscess, and obstructive: slurred speech, difficulty swallowing, obstructive sleep apnea syndrome (OSAS) (1, 2). OSAS is a common, chronic, sleep-related breathing disorder, characterized by periodic narrowing and obstruction of the pharyngeal airway during sleep (3). Untreated it has the potential to produce various chronic diseases. This is especially worrying in the pediatric OSAS population. Adenotonsillar hypertrophy is the primary cause of OSAS in children. In contrast to simple hypertrophy the clinical picture is accompanied by habitual (nightly) snoring (often with intermittent pauses, snorts, or gasps), disturbed sleep, and daytime neurobehavioral problems. The gold standard for diagnosing OSAS is polysomnography (PSG) (3, 4). Still due to the vastness of population affected PSG seems unfeasible to conduct in all cases. A straightforward otorhinolaryngologic diagnostic procedure in cases of major tonsillar hypertrophy and obvious history makes PSG redundant (5). Its results are sometimes ambigous but cannot be overlooked in cases of difficult ethiology of sleep disorders (6). From the standpoint of a pediatric otorhinolaryngologist in a tertiary institution mixed breathing disorders aetiology should not be overlooked or even hastily put under an umbrella of adenotonsillar hypertrophy especially if there is not one (7).
Hypertrophy of the tonsils can be defined as a noninfectious overgrowth of the tonsils. It’s common in children and might resolve spontaneously. Tonsillectomy consists of removal of the palatine tonsils with or without their capsules (total and partial tonsillectomy, respectively) by use of different surgical procedures (8). In pediatric patients, the two main indications for this procedure are OSAS and recurrent throat infections (9). In children with OSAS, the procedure eliminates the obstructive portion of the tonsil while preserving the tonsillar capsule and a base of lymphoid tissue. The capsule integrity is maintained, and a natural biologic dressing is left in place over the pharyngeal muscles, preventing them from injury, inflammation, and infection. The indication for tonsillectomy and choice of the particular tonsillar procedure is made after history taking and otorhinolaryngologic clinical examination (4). In more difficult cases, case of OSAS clinically not fitting or with added central hypoventilation syndromes, the polysomnography (PSG) may be mandatory (3, 4, 6).
Aim
The purpose of this work is to review and analyze the differences in estimated morphology of the tonsils in children who underwent a procedure on tonsillar tissue for OSAS and hypertrophic tonsils. Since OSAS can have many causes, we believe the difference in sheer estimated size might not be significantly different for children with OSAS and hypertrophic tonsils.
Material and methods
Our retrospective study included children, who underwent a total or partial tonsillectomy at the Department of Otorhinolaryngology at the University Medical Center in Ljubljana as a tertiary referral centre in the period from September 2011 until November 2019. All patients were examined and qualified for the procedure by an otolaryngologist. Inclusion criteria for the OSAS group were: history of apnea during sleep with positive ENT examination (voluminous tonsils and adenoids) or CMCRF (Continuous Monitoring of Cardio-Respiratory Functions) in case of ambivalent history. Patients with no history of OSAS or inflammation but with voluminous tonsils have been included in the hypertrophic group. The indication for the tonsillar procedure was noted. Tonsillectomy was performed in cases with no history of tonsillitis. We collected the data from the hospital information system (HIS) including age, sex and clinical data including diagnosis and size of the tonsils. Drop-down choices (tab. 1) were used for the morphological assessment of the tonsils.
Tab. 1. Drop-down choices scale
| Size of the tonsils | Description |
| Small | Tonsils deep in the tonsillar groove, not visible unless anterior pillar is retracted, or barely visible if shallow seated |
| Middle | Tonsils within in the tonsillar groove, visible without retraction of the anterior pillar |
| Big | Tonsils over the level of the tonsillar arches but not more than 50% of the tonsillar volume over the arches |
| Large | Tonsils over the arches with more than 50% of the volume or narrow intratonsillar space at children with shallow tonsils or extremely deep intratonsillar space after resection with deep seated tonsils |
Patients with incomplete hospital digital records were excluded from the study. We used appropriate statistical methods (Chi-square, Mann-Whitney test) after checking our data for normality with regard to the data distribution and corrections for the sample size. We regarded p < 0.05 as statistically significant. SPSS for Windows (IBM, Armonk, New York, USA), GraphPad (San Diego, California, USA), Microsoft Excel (Microsoft, Redmond, Washington, USA) and Epiinfo (CDC, Atlanta, Georgia, USA) were used for analysis.
Results
824 patients were included in the analysis and divided in 2 main groups: OSAS with 96 patients and Hypertrophic with 728. Our data was disaggregated by gender: 543 boys and 281 girls. Patients’ age ranged from 1.5 to 17 years (median age 4.9). Age, sex and size of the tonsils were analyzed (tab. 2). The patients’ age was not normally distributed; therefore, we used the Mann-Whitney test and found the OSAS group (5.8 years) and Hypertrophic (5.5 years) had a similar mean age (p = 0.94, tab. 2). They also have the same gender distribution with male predominance (females 41.1 vs 34.2%, p = 0.91, tab. 2). The OSAS and Hypertrophic group statistically differ in terms of the size of the tonsils. There is no significant difference in the prevalence of small (2.1 and 1.5% of patients in the OSAS and Hypertrophic groups, respectively) and middle-sized tonsils (9.4 and 14.6%, respectively). In the Hypertrophic group big tonsils were predominant (47.1%, in comparison to 35.4%, in the OSAS group) and large tonsils were significantly more often found in the OSAS group (53.1%, with 36.8% in the Hypertrophic group, p = 0.01). Results are summed up in table 2 and showed on figure 1.
Tab. 2. Study groups and data analysis
| N = 824 | OSAS | Hypertrophic | p-value |
| Number of cases | 96 | 728 | |
| Age (mean, median, interquartile range [IQR] – years) | 5.8, 4.9, IQR 3.5 | 5.5, 4.9, IQR 2.8 | p = 0.94* |
Sex
male
female |
64 (58.3%)
32 (41.7%) |
479 (65.8%)
249 (34.2%) | M vs F
OSAS p < 0.001
Hypertrophic p < 0.001
OSAS vs Hypertrophic p = 0.91** |
Size
small
middle
big
large |
2 (2.1%)
9 (9.4%)
34 (35.4%)
51 (53.1%) |
11 (1.5%)
106 (14.6%)
343 (47.1%)
268 (36.8%) |
p = 0.01**
|
*Mann-Whitney test
**Chi-Square
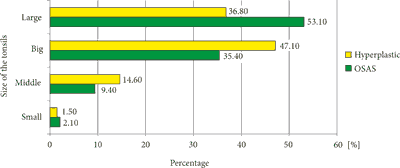
Fig. 1. Distribution of the size type in percentage
Discussion
OSAS and Hypertrophic tonsils remain an essential indication for tonsillectomy (1, 2). Estimation or objective measurement of the tonsil size may represent a potent research tool in the evaluation of OSAS (10). With a thorough search of confounders, maybe even help to find intimate differences in pathology behind the hypertrophy itself (11). Although it may intuitively seem the estimated size of tonsils are at least similar, we have found that in our group OSAS significantly predisposes bigger tonsils (tab. 3). This stands in contrast with data often encountered in the literature, stating there is no difference in tonsil size in the OSAS and non-OSAS groups (12). Therefore we had rejected our hypothesis that there is no difference in tonsil size. Especially in case of OSAS, it’s the lack of pharyngeal 3D space allowing to keep the airway open (4, 13). We haven’t measured the exact volume of tonsils as it was not possible due to the retrospective study design.
Tab. 3. Correlations of location and size of the tonsils
| Group | Size | p-value* |
| OSAS | Small | 0.998 |
| Middle | 0.999 |
| Big | 0.991 |
| Large | – |
| Small | 0.264 |
| Middle | 0.999 |
| Big | 0.991 |
| Large | – |
| Small | – |
| Middle | 0.999 |
| Big | 0.991 |
| Large | – |
| Hypertrophic | Small | 0.999 |
| Middle | 0.001** |
| Big | 0.872 |
| Large | – |
| Small | 0.999 |
| Middle | < 0.001** |
| Big | 0.916 |
| Large | – |
| Small | 0.999 |
| Middle | – |
| Big | 0.941 |
| Large | – |
*Logistic regression model
** Statistically significant
Nevertheless our study is one of the largest up to our knowledge in literature, we can propose there is a significant overall difference in the size of tonsils. It may overtly expose some of the clinical factors encountered during and after the surgical procedure. Directly it can help easily define patients with contradictory findings (lower volume of tonsils as expected) and allow additional diagnostics (PSG, CMCRF) in a follow-up. We certainly propose to extend the study towards an objective evaluation of the tonsil volume and stratification of patients size or percentile achieved for their age. We have knowingly disregarded other causes of OSAS as hypotonia or extreme oropharyngeal anatomy (syndromes) since our study did not involve patients with mixed obstructive breathing pathology. Concerning other studies majorly influencing our primary hypothesis (12) we are also implying it is not solely the size of the pharyngeal pathway but also the size of tonsils that matters but also as well as other potentially undiscovered factors.
Conclusions
Age and sex-matched groups of children who underwent tonsillectomy and had a diagnosis of OSAS have bigger tonsils than those who had the only diagnosis of hypertrophic tonsils.
Piśmiennictwo
1. Baugh RF, Archer SM, Mitchell RB et al.: Clinical Practice Guideline: Tonsillectomy in Children. Otolaryngol Neck Surg 2011; 144(1 suppl.): S1-30.
2. Kambič V: Otorinolaringologija. Mladinska kniga, Ljubljana 1984.
3. Osman AM, Carter SG, Carberry JC, Eckert DJ: Obstructive sleep apnea: current perspectives. Nat Sci Sleep 2018; 10: 21-34.
4. Bitners AC, Arens R: Evaluation and Management of Children with Obstructive Sleep Apnea Syndrome. Lung 2020; 198(2): 257-270.
5. Ameli F, Brocchetti F, Semino L, Fibbi A: Adenotonsillectomy in obstructive sleep apnea syndrome. Proposal of a surgical decision-taking algorithm. Int J Pediatr Otorhinolaryngol 2007; 71(5): 729-734.
6. Cornfield DN, Bhargava S: Sleep medicine: pediatric polysomnography revisited. Curr Opin Pediatr 2015; 27(3): 325-328.
7. Urbančič J: Obstruktivne motnje dihanja med spanjem pri otrocih. Medicinske fakultete: Univerzitetni klinični center, Klinika za otorinolaringologijo in cervikofacialno kirurgijo: Združenje otorinolaringologov Slovenije SZD 2013: 63-68.
8. Wall JJ, Tay KY: Postoperative Tonsillectomy Hemorrhage. Emerg Med Clin North Am 2018; 36(2): 415-426.
9. Mitchell RB, Archer SM, Ishman SL et al.: Clinical Practice Guideline: Tonsillectomy in Children (Update)-Executive Summary. Otolaryngol Head Neck Surg (United States) 2019; 160(2): 187-205.
10. Li AM, Wong E, Kew J et al.: Use of tonsil size in the evaluation of obstructive sleep apnoea. Arch Dis Child 2002; 87(2): 156-159.
11. Huang Q, Hua H, Li W et al.: Simple hypertrophic tonsils have more active innate immune and inflammatory responses than hypertrophic tonsils with recurrent inflammation in children. J Otolaryngol Head Neck Surg 2020; 49: 35.
12. Section on Pediatric Pulmonology, Subcommittee on Obstructive Sleep Apnea Syndrome, American Academy of Pediatrics: Clinical practice guideline: diagnosis and management of childhood obstructive sleep apnea syndrome. Pediatrics 2002; 109(4): 704-712.
13. Luana N, Marco Z, Francesca DB et al.: Age and upper airway obstruction: A challenge to the clinical approach in pediatric patients. Int J Environ Res Public Health 2020; 17(10): 1-9.
