*Małgorzata Kołodziejczak
Treatment of hemorrhoidal disease in an atypical patient
Leczenie choroby hemoroidalnej u nietypowego pacjenta
Warsaw Proctology Center, St. Elisabeth Hospital, Mokotów Medical Center, Warsaw
Streszczenie
Dostępne w piśmiennictwie algorytmy i zalecenia dotyczące leczenia choroby hemoroidalnej uwzględniają przede wszystkim etap zaawansowania choroby. Zazwyczaj pomijane są nietypowe sytuacje u pacjenta, takie jak: obniżona odporność w przebiegu zakażenia wirusem HIV, przyjmowanie chemioterapii przez pacjenta onkologicznego, stałe leczenie immunosupresyjne u pacjentów po przeszczepach narządów lub z nieswoistymi zapaleniami jelit, a także leczenie choroby hemoroidalnej u pacjentów w wieku podeszłym, u których współistnieją choroby zwiększające ryzyko powikłań okołooperacyjnych.
Z kolei publikacje dotyczące powikłań leczenia pacjentów z obniżoną odpornością marginalizują problem chorób proktologicznych, w tym często występującej choroby hemoroidalnej. W niniejszym artykule przedstawiono postępowanie terapeutyczne w chorobie hemoroidalnej u nietypowego pacjenta. Dodatkowo omówiono też specyfikę postępowania w chorobie hemoroidalnej u pacjentki ciężarnej i w okresie okołoporodowym.
Summary
Therapeutic algorithms and recommendations for haemorrhoidal disease proposed in the literature are based on the stage of the disease. Less typical situations, such as reduced immunity in HIV infection, cancer patients on chemotherapy, chronic immunosuppressive treatment in patients after organ transplantation or patients with inflammatory bowel disease, as well as elderly patients with comorbidities that increase the risk of perioperative complications, are not usually discussed.
On the other hand, publications on treatment complications in immunocompromised patients marginalise the problem of anorectal conditions, including common haemorrhoids. This paper presents the therapeutic management of haemorrhoidal disease in atypical patients. Furthermore, the specifics of the management of haemorrhoidal disease in a pregnant patient and in the perinatal period are also discussed.

Introduction
Haemorrhoidal disease is a common modern-age disease, which affects about 11% of adult population and 80% of pregnant women in the third trimester (1). The peak incidence is between the ages of 45 and 65 years, which means that haemorrhoids generally affect professionally active persons. Painless anal bleeding after bowel movement and haemorrhoidal prolapse are the most common clinical symptoms. The degree of haemorrhoidal prolapse is the basis for the four-grade Goligher’s classification. The algorithms and recommendations for the treatment of haemorrhoidal disease available in the literature are mainly based on the stage of the disease. Less typical situations, such as reduced immunity in HIV infection, chemotherapy in an oncological patient, chronic immunosuppressive treatment in patients after organ transplants or patients with inflammatory bowel disease, as well as elderly patients with comorbidities that increase the risk of perioperative complications, are not usually discussed.
This paper presents the therapeutic management in such unusual situations.
Cancer patient on chemotherapy
Even though curing cancer is, from a rational point of view, the primary goal in oncological patients, anorectal symptoms may paradoxically have a greater impact on reducing the quality of life in these patients than the cancer itself. Chemotherapy often exacerbates anal pruritus, while coagulation disorders, which are common in these patients, may contribute to haemorrhoidal bleeding. Leukaemia and the accompanying neutropenia particularly increase the risk of haemorrhoidal bleeding. Conservative treatment is the method of choice, whereas surgical interventions should be used as a last resort, e.g. in cases of heavy bleeding requiring transfusion. In the case of less advanced disease and frequent bleeding resistant to conservative treatment, rubber band ligation (RBL) is performed. If a decision is made to perform surgery, which usually takes place in grade IV haemorrhoids, the procedure should be performed after reaching the best possible immunity in the patient (fig. 1). Providing the patient with detailed dietary guidelines and prescription of pharmacological agents to alleviate local symptoms can significantly improve the patient’s quality of life and help avoid surgery.
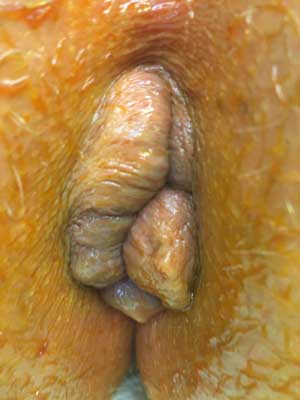
Fig. 1. Grade IV haemorrhoids
Pregnant patients and perinatal period
Pregnancy and vaginal childbirth predispose women to haemorrhoid enlargement due to hormonal changes and increased intra-abdominal pressure as a result of the stretched uterus. Constipation is considered to be the main cause of symptom aggravation, which in turn is associated with increased progesterone that inhibits intestinal peristalsis, mechanical factors (uterine enlargement in the second and third trimester of pregnancy), and iron preparations often received by pregnant women. It is estimated that 25% to 35% of pregnant women are affected (2). Epidemiological data show that in some populations up to 85% of pregnant women report haemorrhoids in the third trimester of pregnancy (3).
Conservative therapy and modified diet to include high intake of water and fibre and low intake of hot spices are used in pregnant women. Topical preparations, preferably non-absorbable, to moisturise the mucous membrane of the anal canal can be recommended, e.g. in the form of petroleum jelly or preparations with hyaluronic acid. Medications should be used with caution and only in cases of severe symptoms and after the first trimester of pregnancy. Diosmin and butcher’s broom are acceptable systemic agents. Topical rectal medications should be used with caution, bearing in mind that they are absorbed into the bloodstream and may be teratogenic to the foetus.
In my own practice, I use ointments and suppositories based on vitamins. Patients should be instructed to maintain adequate stool consistency; however, aggressive laxatives, which may lead to premature delivery, should not be prescribed to pregnant women. Emergency situations, such as massive haemorrhage that may cause increasing anaemia, which may lead to foetal hypoxia, and extensive thrombosis of haemorrhoids are indications for surgical treatment.
The most common alternative methods used in pregnant women include rubber band ligation (RBL) and sclerotherapy, but they are used after the first trimester of pregnancy and only in the case of severe symptoms, such as persistent bleeding, and after at least several weeks of attempting conservative treatment.
Powyżej zamieściliśmy fragment artykułu, do którego możesz uzyskać pełny dostęp.
Mam kod dostępu
- Aby uzyskać płatny dostęp do pełnej treści powyższego artykułu albo wszystkich artykułów (w zależności od wybranej opcji), należy wprowadzić kod.
- Wprowadzając kod, akceptują Państwo treść Regulaminu oraz potwierdzają zapoznanie się z nim.
- Aby kupić kod proszę skorzystać z jednej z poniższych opcji.
Opcja #1
29 zł
Wybieram
- dostęp do tego artykułu
- dostęp na 7 dni
uzyskany kod musi być wprowadzony na stronie artykułu, do którego został wykupiony
Opcja #2
69 zł
Wybieram
- dostęp do tego i pozostałych ponad 7000 artykułów
- dostęp na 30 dni
- najpopularniejsza opcja
Opcja #3
129 zł
Wybieram
- dostęp do tego i pozostałych ponad 7000 artykułów
- dostęp na 90 dni
- oszczędzasz 78 zł
Piśmiennictwo
1. Sheikh P, Règnier C, Goron F, Salmat G: The prevalence, characteristics and treatment of hemorrhoidal disease: results of an international web-based survey. J Comp Eff Res 2020; 9(17): 1219-1232.
2. Staroselsky A, Nava-Ocampo AA, Vohra S, Koren G: Hemorrhoids in pregnancy. Can Fam Physician 2008; 54(2): 189-190.
3. Gojnic M, Dugalic V, Papic M et al.: The significance of detailed examination of hemorrhoids during pregnancy. Clin Exp Obstet Gynecol 2005; 32(3): 183-184.
4. Salusso P, Testa V, Mochet S et al.: Management of Hemorrhoidal Disease in Special Conditions: A Word of Caution. Rev Recent Clin Trials 2021; 16(1): 22-31.
5. D’Ugo S, Stasi E, Gaspari AL, Sileri P: Hemorrhoids and anal fissures in inflammatory bowel disease. Minerva Gastroenterol Dietol 2015; 61(4): 223-233.
6. Lightner AL, Kearney D, Giugliano D et al.: Excisional Hemorrhoidectomy: Safe in Patients With Crohn’s Disease? Inflamm Bowel Dis 2020; 26(9): 1390-1393.
7. McKenna NP, Lightner AL, Habermann EB, Mathis KL: Hemorrhoidectomy and Excision of Skin Tags in IBD: Harbinger of Doom or Simply a Disease Running Its Course? Dis Colon Rectum 2019; 62(12): 1505-1510.
8. Picciariello A, Rinaldi M, Grossi U et al.: Management and Treatment of External Hemorrhoidal Thrombosis. Front Surg 2022; 9: 898850.
9. Sun Z, Migaly J: Review of Hemorrhoid Disease: Presentation and Management. Clin Colon Rectal Surg 2016; 29(1): 22-29.
10. Scaglia M, Delaini GG, Destefano I, Hultèn L: Injection treatment of hemorrhoids in patients with acquired immunodeficiency syndrome. Dis Colon Rectum 2001; 44(3): 401-404.
11. Tallarita T, Gurrieri C: Clinical features of hemorrhoidal disease in renal transplant recipients. Transplant Proc 2010; 42(4): 1171-1173.
12. Eberspacher C, Mascagni D, Antypas P et al.: External hemorrhoidal thrombosis in the elderly patients: conservative and surgical management. Minerva Chir 2020; 75: 117-120.
13. Awad AE, Soliman HH, Saif SA et al.: A prospective randomised comparative study of endoscopic band ligation versus injection sclerotherapy of bleeding internal haemorrhoids in patients with liver cirrhosis. Arab J Gastroenterol 2012; 13(2): 77-81.


