*Konrad Kobryń1, Małgorzata Kołodziejczak2, Krzysztof Zieniewicz1, Tadeusz Wróblewski1
Leczenie olbrzymich, zakrzepowo zmienionych hemoroidów – opis przypadku
Treatment of giant thrombosed external hemorrhoids – a case report
1Department of General, Transplant and Liver Surgery, Medical University of Warsaw
Head of Department: prof. Marek Krawczyk, MD, PhD, prof. FEBS
2Department of General Surgery and Proctology, Mokotów Medical Centre, Warszawa
Head of Department: Małgorzata Kołodziejczak, MD, PhD
Summary
Hemorrhoid thrombosis is a rare but dangerous complication of hemorrhoid disease. The main symptom of the disease, causing patients to go to hospital is severe pain. This is caused by hypertonicity of the internal sphincter. The pain itself is expressed during sitting and defecating. Our report describes the case of 64-year-old patient admitted to the emergency room due to external thrombosed gangrenous hemorrhoids. He presented inability to defecate due to excessive pain, mild abdominal pain, discomfort and irritation withholding him from walking and sitting. In his medical records, only arterial hypertension was noted and treated pharmacologically for the last ten years. The patient previously was treated for 5 years in a non-operative manner, this included diet, sitz-baths, suppositories and banding of hemorrhoids in the outpatient room.
Following a short preoperative work up, the patient was qualified for emergent surgery. He received antibiotic therapy (amoxicillin with clavulanate potassium 1,2 g x 3 daily) and antithrombotic prophylaxis (nadroparine 0,4 ml x 1 daily s.c.). A Milligan-Morgan open procedure was performed as method of choice. The hemorrhoids were dissected from the sphincter mechanism and all were resected. All three quadrants were excised identically. Pedicles were then ligated, thus hemostasis was satisfactory. The course of surgery was uneventful, the wound healed without swelling, pain subsided and the patient was discharged on the 3rd post-operative day in good general condition.
Conclusions: Patients with thrombosis hemorrhoids should be operated on as soon as possible because of threatening septic complications, including Fournier gangrene. Antibiotic treatment and prophylaxis is necessary. Surgical treatment of patients with thrombosed hemorrhoids results in prompt and good therapeutic outcome.

Introduction
Thrombosis of external hemorrhoids are among the most acute anorectal diseases attended to in the emergency department or proctology outpatient clinic (1, 2). The main symptom of the disease, causing patients to go to hospital is severe pain. This is caused by hypertonicity of the internal sphincter. The pain itself is expressed during sitting and defecating, however it is also often present during standing and walking in seriously advanced states. Further symptoms accompanying large external thrombosed hemorrhoids are bleeding, failure to pass stool, constipation, swelling, mild discomfort, irritation, abdominal pain and mild fever (1-3).
Anatomically hemorrhoids are submucosal vascularized cushions lined in three columns around the anal canal. We distinguish three positions – right anterior, right posterior and left lateral. It’s important to understand that their presence is physiological and they play a considerable role of protecting the anal sphincter and preventing incontinence by propagating the closure of the anal canal during increased abdominal pressure (3-5). Some authors presume that hemorrhoids also differentiate stool, from liquid and gas residing in the anal canal (3, 4, 6).
Case report
A 64-year-old male patient was admitted to the Department through the emergency room due to severe pain caused by giant thrombosed external hemorrhoids (grade IV) (fig. 1). He presented inability to defecate due to excessive pain, mild abdominal pain, discomfort and irritation withholding him from walking and sitting. Fever was not noted at the time being. Bleeding was reported in past history but not observed during per rectum examination. His medical history, besides arterial hypertension treated pharmacologically for the last ten years, recorded no other comorbidities. Though during history taking the patient admitted to a 5 year non-operative treatment (diet, sitz-baths, suppositories and banding) of hemorrhoids in the outpatient room.
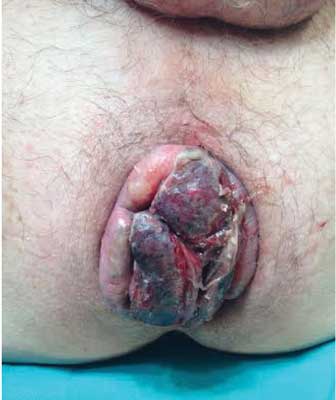
Fig. 1. Thrombosed external hemorrhoids – grade IV.
Powyżej zamieściliśmy fragment artykułu, do którego możesz uzyskać pełny dostęp.
Mam kod dostępu
- Aby uzyskać płatny dostęp do pełnej treści powyższego artykułu albo wszystkich artykułów (w zależności od wybranej opcji), należy wprowadzić kod.
- Wprowadzając kod, akceptują Państwo treść Regulaminu oraz potwierdzają zapoznanie się z nim.
- Aby kupić kod proszę skorzystać z jednej z poniższych opcji.
Opcja #1
29 zł
Wybieram
- dostęp do tego artykułu
- dostęp na 7 dni
uzyskany kod musi być wprowadzony na stronie artykułu, do którego został wykupiony
Opcja #2
69 zł
Wybieram
- dostęp do tego i pozostałych ponad 7000 artykułów
- dostęp na 30 dni
- najpopularniejsza opcja
Opcja #3
129 zł
Wybieram
- dostęp do tego i pozostałych ponad 7000 artykułów
- dostęp na 90 dni
- oszczędzasz 78 zł
Piśmiennictwo
1. Aigner F, Gruber H, Conrad F et al.: Revised morphology and hemodynamics of the anorectal vascular plexus: impact on the course of hemorrhoidal disease. Int J Colorectal Dis 2009; 24(1): 105-113. 2. Smith LE: Hemorrhoids. [In:] Fazio V (ed.): Current Therapy in Colon and Rectal Surgery. St. Louis, MO: Mosby 2004: 11-18. 3. Johanson JF, Sonnenberg A: The prevalence of hemorrhoids and chronic constipation. An epidemiologic study. Gastroenterology 1990; 99: 1856-1857. 4. Ganchrow MI, Bowman HE, Clark JF: Thrombosed hemorrhoids; clinicopathologic study. Dis Colon Rectum 1971; 14: 331-340. 5. Cintron J, Abacarian H: Benign anorectal: hemorrhoids. [In:] Wolff BG, Fleshman JW (eds.): The ASCRS of Colon and Rectal Surgery. New York, NY: Springer-Verlag 2007: 156-177. 6. Andrews BT, Layer GT, Jackson BT, Nicholls RJ: Randomized trial comparing diathermy hemorrhoidectomy with the scissor dissection Milligan-Morgan operation. Dis Colon Rectum 1993; 36(6): 580-583. 7. Greenspon J, Williams SB, Young HA, Orkin BA: Thrombosed external hemorrhoids: outcome after conservative or surgical management. Dis Colon Rectum 2004; 47(9): 1493-1498. 8. Bayer I, Myslovaty B, Picovsky BM: Rubber band ligation of hemorrhoids. Convenient and economic treatment. J Clin Gastroenterol 1996; 23(1): 50-52. 9. Bat L, Melzer E, Koler M et al.: Complications of rubber band ligation of symptomatic internal hemorrhoids. Dis Colon Rectum 1993; 36(3): 287-290. 10. Barwell J, Watkins RM, Lloyd-Davies E, Wilkins DC: Life threatening retroperitoneal sepsis after hemorrhoid injection sclerotherapy: report of a case. Dis Colon Rectum 1999; 42(3): 421-423. 11. You SY, Kim SH, Chung CS, Lee DK: Open vs. closed hemorrhoidectomy. Dis Colon Rectum 2005; 48(1): 108-113. 12. Ratto C, Donisi L, Parello A et al.: Evaluation of transanal hemorrhoidal dearterialization as a minimally invasive therapeutic approach to hemorrhoids. Dis Colon Rectum 2010; 53(5): 803-811. 13. Bleday R, Pena JP, Rothenberger DA et al.: Symptomatic hemorrhoids: current incidence and complications of operative therapy. Dis Colon Rectum 1992; 35(5): 477-481. 14. Johanson JF, Rimm A: Optimal nonsurgical treatment of hemorrhoids: a comparative analysis of infrared coagulation, rubber band ligation, and injection sclerotherapy. Am J Gastroenterol 1992; 87(11): 1600-1606. 15. Savioz D, Roche B, Glauser T et al.: Rubber band ligation of hemorrhoids: relapse as a function of time. Int J Colorectal Dis 1998; 13(4): 154-156. 16. Khan S, Pawlak SE, Eggenberger JC et al.: Surgical treatment of hemorrhoids: prospective, randomized trial comparing closed excisional hemorrhoidectomy and the Harmonic Scalpel technique of excisional hemorrhoidectomy. Dis Colon Rectum 2001; 44(6): 845-849.


