*Sławomir Glinkowski1, 2, Daria Marcinkowska1
Laser hemorrhoidoplasty (LHP) using a 1470 nm radial fibre laser – early efficacy assessment based on own data
Laserowa hemoroidoplastyka (LHP) przy użyciu lasera radialnego 1470 nm – wczesna ocena skuteczności metody w materiale własnym
1Department of General and Oncologic Surgery in Tomaszów Mazowiecki Health Center
2MEDICALL – Institute of Health in Piotrków Trybunalski
Streszczenie
Wstęp. Choroba hemoroidalna należy do najczęstszych chorób kolorektalnych. Jest wiele sposobów jej leczenia, jednak najczęściej wykonywaną procedurą operacyjną jest hemoroidektomia sposobem Milligana-Morgana.
Cel pracy. Celem pracy było porównanie skuteczności najczęściej wykonywanej operacji sposobem Milligana-Morgana oraz hemoroidoplastyki laserowej z wykorzystaniem lasera radialnego 1470 nm. Uwzględniono takie zmienne, jak: czas trwania procedury, czas hospitalizacji związanej z zabiegiem, dolegliwości bólowe pacjentów po wykonanej procedurze, czas powrotu do normalnej codziennej aktywności.
Materiał i metody. Grupę badaną tworzyło 178 pacjentów, w tym 82 poddanych zabiegowi hemoroidoplastyki laserowej oraz 96 pacjentów zoperowanych sposobem Milligana-Morgana. 45% grupy stanowiły kobiety, 55% – mężczyźni. Średni wiek pacjentów wynosił 50 lat, najmłodszy pacjent miał 19 lat, najstarszy – 65 lat. Średni wiek pacjentów był niższy w grupie osób zoperowanych LHP (54,23 vs 45,15 roku). Obserwacja pacjentów trwała średnio 14 miesięcy (przedział 3-35 miesięcy).
Wyniki. Średni czas operacji LHP był krótszy niż sposobem Milligana-Morgana (13,9 vs 22,3 min). Po operacji LHP nie było konieczności reoperacji, natomiast po klasycznej hemoroidektomii trzykrotnie trzeba było reoperować. Średni czas powrotu do pracy po zabiegu LHP wyniósł 14 dni (najkrótszy 5 dni), po klasycznej hemoroidektomii było to 21 dni (najkrótszy 15 dni). Po operacji Milligana-Morgana 51% pacjentów wymagało podania opioidowych leków przeciwbólowych, po zabiegu LHP nie było takiej potrzeby w żadnym przypadku.
Wnioski. Metoda LHP jest skutecznym sposobem leczenia choroby hemoroidalnej II-IV stopnia i wiąże się z mniejszymi dolegliwościami bólowymi niż klasyczna hemoroidektomia. Czas operacji oraz czas hospitalizacji po LHP jest krótszy niż po operacji sposobem Milligana-Morgana. Krótszy jest także czas powrotu do normalnej codziennej aktywności.
Summary
Introduction. Haemorrhoidal disease is one of the most common colorectal conditions. Although many treatment methods have been developed, Milligan-Morgan hemorrhoidectomy remains the most widely practised surgical technique.
Aim. The aim of this study was to compare the effectiveness of Milligan-Morgan hemorrhoidectomy and laser hemorrhoidoplasty using a 1470 nm radial fibre laser. The following variables were analysed: procedure duration, length of procedure-related hospital stay, postoperative pain, and time to return to normal daily activities.
Material and methods. The study group included 178 patients (women 45%, men 55%), including 82 patients undergoing laser hemorrhoidoplasty and 96 patients undergoing Milligan-Morgan hemorrhoidectomy. The mean age of the patients was 50 years, with the youngest patient aged 19 years and the oldest patient aged 65 years. The mean age of patients was lower in the laser hemorrhoidoplasty group (54.23 vs 45.15 years). The mean follow-up was 14 months (3-35 years).
Results. The mean duration of laser hemorrhoidoplasty was shorter than that of Milligan-Morgan hemorrhoidectomy (13.9 vs. 22.3 min). There was no need for a revision surgery after laser hemorrhoidoplasty, whereas reoperation was necessary in three cases after classical hemorrhoidectomy. The mean and the shortest time of return to work was 14 and 5 days for laser hemorrhoidoplasty compared to 21 and 15 days for classical hemorrhoidectomy, respectively. Opioid analgesics were needed in 51% of patients after Milligan-Morgan hemorrhoidectomy and none of the patients after laser hemorrhoidoplasty.
Conclusions. Laser hemorrhoidoplasty is an effective treatment approach in grade II-IV haemorrhoidal disease. It is associated with less pain compared to conventional hemorrhoidectomy. The duration of both the procedure itself and hospital stay is shorter after laser hemorrhoidoplasty compared to Milligan-Morgan hemorrhoidectomy. The return to normal daily activities is also faster in the first case.

Introduction
Haemorrhoidal disease is the most common colorectal condition. The estimated prevalence is 2.9 to 27.9%, including more than 4% of symptomatic patients (1). The occurrence of symptoms does not always result in the patient reporting to a general practitioner or directly to a general surgeon. This is most likely due to the embarrassment caused by the location of the disease. Very often, patients with long-term symptoms try to self-medicate with over-the-counter medications.
The most common symptoms of haemorrhoidal disease include bleeding during bowel movements, irritation around the anal area, and prolapsed haemorrhoids. Although not always severe, these symptoms contribute to reduced quality of life.
Treatment approaches in haemorrhoidal disease may be classified as conservative and surgical. It is estimated that up to 85% of patients may be successfully treated with conservative methods (2). Other patients require interventional management (instrumental or surgical).
Instrumental methods include, among others (3):
– Barron’s Rubber Band Ligation (1963) (4),
– sclerotherapy,
– infrared coagulation.
These are outpatient instrumental approaches, which may be performed without the need for hospital stay. They are recommended for patients with grade I-III haemorrhoids; however, each of these techniques has its own indications and contraindications.
The 2018 American Society of Colon and Rectal Surgeons (ASCRS) Clinical Practice Guidelines for the Management of Hemorrhoids, published in “Diseases of the Colon & Rectum”, are current guidelines that standardise the management in a patient with haemorrhoidal disease (3). They strongly emphasise the role of diet and lifestyle modification, as well as present data on pharmacotherapy. Diet and lifestyle modification plays a crucial role in both conservative treatment, as well as pre- and post-operative management.
Surgical approaches include conventional haemorrhoidectomy, which may be classified as open (Milligan-Morgan) and closed (Ferguson). Although no significant advantage of Milligan-Morgan haemorrhoidectomy has been demonstrated in many studies and, on the contrary, Ferguson method was shown to yield better treatment outcomes, open haemorrhoidectomy remains the most common conventional procedure (2). Laser hemorrhoidoplasty (LHP), which uses a 1470 nm radial fibre laser, also falls in the group of surgical techniques.
We present data based on a study and a follow-up in 82 patients after laser hemorrhoidoplasty. The obtained results were compared with treatment outcomes of Milligan-Morgan haemorrhoidectomy, which is the most common surgical technique used in our country to treat haemorrhoidal disease. The latter approach was used in 96 patients.
Aim
The aim of this study was to compare the effectiveness of conventional hemorrhoidectomy and laser hemorrhoidoplasty for procedure duration, length of procedure-related hospital stay, postoperative pain, and time to return to normal daily activities.
Material and methods
The study group included a total of 178 patients (80 women and 98 men) aged between 19 and 65 years (mean age 50 years), who underwent a surgery due to grade I-IV haemorrhoidal disease. This group included 96 patients (54%) who underwent Milligan-Morgan procedure due to haemorroidal disease, whereas other patients (46%, n = 82) were treated with a radial fibre laser.
Patients treated with the Milligan-Morgan (M-M) method were hospitalised in a general surgery ward of a district hospital (patients operated by a team of physicians working in a given ward), while those treated with the laser method were admitted to a private facility (all patients were operated on by the authors of the study). This is because LHP is not reimbursed and may be only used in private medical centres. Patients undergoing the M-M procedure were included in group 1, and those treated with LHP were included in group 2.
The mean follow-up was at least 3 months (from December 2017 to July 2020). The mean follow-up was 14 months (3-35 months).
Enrolment for the study was performed in parallel with qualification for a surgery. All patients completed a preoperative questionnaire before treatment initiation (Appendix 1). Then, a follow-up was performed by the doctor, who entered data in the patient’s record based on the information obtained from the patient (fig. 1) .
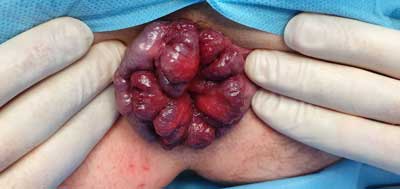
Fig. 1. Grade IV haemorrhoidal disease qualified for Milligan-Morgan haemorrhoidectomy
Results
Full responses were obtained from 178 patients. A total of 80 women (45%) and 98 men (55%) participated in the study. Males accounted for the majority of patients in both groups, i.e. 50 (52%) men in group 1 and 48 (58.6%) men in group 2. There were 46 (48%) women in group 1 and 34 (41.4%) in group 2.
The mean age of patients was higher in group 1 (54.23 years) than group 2 (45.15 years). The upper age limit was also lower in group 2 (58 years) than group 1 (65 years) (tab. 1).
Tab. 1. Comparison of group variables 1 (M-M) and 2 (LHP)
| | M-M | LHP |
| Number of patients | 96 | 82 |
| Females | 46 (48%) | 34 (41.4%) |
| Males | 50 (52%) | 48 (58.6%) |
| Mean age (years) | 54.23 | 45.15 |
| The youngest patient (years) | 31 | 19 |
| The oldest patient (years) | 65 | 58 |
| Median age (years) | 54 | 42 |
It was also found from patients’ medical records that comorbidities and chronic pharmacotherapy were less common in group 2. In both groups, these were mostly medications for cardiovascular diseases. Patients with comorbidities accounted for 69.8% (n = 67) in group 1 and 45.1% (n = 37) in group 2.
Five most common comorbidities reported by our patients are summarised in table 2.
Tab. 2. Five most common comorbidities in groups 1 (M-M) and 2 (M-M)
| Comorbidities | M-M | LHP |
| Hypertension | 52 | 26 |
| Ischaemic heart disease | 5 | 1 |
| Diabetes mellitus | 21 | 9 |
| Hypercholesterolaemia | 8 | 5 |
| Depression | 11 | 6 |
Medical history of comorbidities was collected directly from patients and their medical records from previous hospital stays and follow-up visits.
Patients with grade IV haemorrhoidal disease accounted for the majority of group 1 (52.1%). Most patients in group 2 (64.6%) presented with grade III haemorrhoids. The smallest group of patients in groups 1 (10.4%) and 2 (3.7%) were those with grade II and grade IV haemorrhoids, respectively.
The mean duration of surgery was shorter in group 2 (13.9 min) compared to group 1 (22.3 min). The surgical treatment in group 1 was longer despite the fact that three haemorrhoidal columns were usually managed in both these groups (87.5% in group 1 vs. 91.5% in group 2) (tab. 3).
Tab. 3. Comparison of the main features of operations performed in group 1 (M-M) and group 2 (LHP)
| | | M-M | LHP |
| Grade | Grade II | 10 (10.4%) | 26 (31.7%) |
| | Grade III | 36 (37.5%) | 53 (64.6%)
|
| | Grade IV | 50 (52.1%) | 3 (3.7%) |
| Combined procedures | | 8 (8.3%) | 10 (12.2%) |
| Mean surgery time [minutes] | | 22.3 | 13.9 |
| Number of columns managed | 1 | 1 (1.04%) | 2 (2.4%) |
| | 2 | 4 (4.16%) | 5 (6.1%) |
| | 3 | 84 (87.5%) | 75 (91.5%) |
| | 4 | 7 (7.3%) | 0 |
Combined procedures were used in 84 patients in group 1 (97.7%) and 19 patients in group 2 (23.17%).
In group 1, these were:
– excision of a chronic anal fissure with superficial sphincterotomy of the internal sphincter fibres – 5 cases,
– excision of skin tags – 79 cases.
In group 2, these were:
– excision of a chronic anal fissure + botulinum toxin injection into the internal anal sphincter – 5 cases,
– recto anal repair (RAR) – 5 cases,
– excision of hypertrophied anodermal folds – 9 cases.
Excision of hypertrophied skin tags was also considered a combined procedure in group 1, although it is a common element of such interventions.
The need for a revision surgery after both procedures was another compared parameter. There was no need for reoperation in any of the patients in group 2. In group 1, reoperation was needed in 3 patients on the first day after surgery due to bleeding. The bleeding was caused by inaccurate ligation of the vascular pedicle.
Powyżej zamieściliśmy fragment artykułu, do którego możesz uzyskać pełny dostęp.
Mam kod dostępu
- Aby uzyskać płatny dostęp do pełnej treści powyższego artykułu albo wszystkich artykułów (w zależności od wybranej opcji), należy wprowadzić kod.
- Wprowadzając kod, akceptują Państwo treść Regulaminu oraz potwierdzają zapoznanie się z nim.
- Aby kupić kod proszę skorzystać z jednej z poniższych opcji.
Opcja #1
29 zł
Wybieram
- dostęp do tego artykułu
- dostęp na 7 dni
uzyskany kod musi być wprowadzony na stronie artykułu, do którego został wykupiony
Opcja #2
69 zł
Wybieram
- dostęp do tego i pozostałych ponad 7000 artykułów
- dostęp na 30 dni
- najpopularniejsza opcja
Opcja #3
129 zł
Wybieram
- dostęp do tego i pozostałych ponad 7000 artykułów
- dostęp na 90 dni
- oszczędzasz 78 zł
Piśmiennictwo
1. Alsisy A, Alkhateep YM, Salem IEI: Comparative study between intrahemorrhoidal diode laser treatment and Milligan-Morgan hemoroidectomy. Menoufia Med J 2018; 32(2): 560-565.
2. Kołodziejczak M, Ciesielski P, Dutkiewicz P: Miejsce hemoroidektomii metodą Milligana-Morgana we współczesnym algorytmie leczenia choroby hemoroidalnej – przegląd aktualnego piśmiennictwa. Nowa Med 2016; 1: 22-28.
3. Bradley RD, Lee-Kong SA, Migaly J et al.: The American Society of Colon and Rectal Surgeons Clinical Practice Guidelines for the Management of Hemorrhoids. Dis Colon Rectum 2018; 61: 284-292.
4. Barron J: Office ligation of haemorrhoids. Am J Surg 1963; 195: 563.
5. Crea N, Patz G, Lippa M et al.: Hemorrhoidal laser procedure: short- and long-term results from a prospective study. Am J Surg 2014; 208(1): 21-25.
6. Faes S, Pratsinis M, Hasler-Gehrer S et al.: Short- and long-term outcomes of laser haemorrhoidoplasty for grade II-III haemorrhoidal disease. Colorectal Dis 2019; 21(6): 689-696.
7. Poskus T, Danys D, Makunaite G et al.: Results of the double-blind randomized controlled trial comparing laser hemorrhoidoplasty with sutured mucopexy and excisional hemorrhoidectomy. Int J Colorectal Dis 2020; 35(3): 481-490.
8. Brusciano L, Gambardella C, Terracciano G et al.: Postoperative discomfort and pain in the management of hemorrhoidal disease: laser hemorrhoidoplasty, a minimal invasive treatment of symptomatic hemorrhoids. Updates Surg 2020; 72(3): 851-857.
9. Plapler H, Hage R, Duarte J et al.: A New Method For Hemorrhoid Surgery: Intrahemorrhoidal Diode Lase, Does It Work? Photomed Laser Surg 2009; 27(5): 819-823.
10. Giamundo P, De Angelis M, Mereu A: Hemorrhoid laser procedure with suture-pexy (HeLPexx): a novel effective procedure to treat hemorrhoidal disease. Tech Coloproctol 2020; 24(2): 199-205.
11. Bachtsetzis G, Bachtsetzis C, El Dakroury N, Athanasiou G: ELITE: a diode laser minimal invasive technique for hemorrhoids during the surgical treatment for anal fissure. J Surg Case Rep 2019; 24(1): rjy363.


