© Borgis - Postępy Nauk Medycznych 2/2012, s. 147-151
Magdalena Atarowska, *Włodzimierz Samborski
Fibromialgia – choroba czy zespół bólowy?
Fibromyalgia – a disease or a pain syndrome?**
Department of Rheumatology and Rehabilitation, Poznań University of Medical Science
Head of Department: prof. dr hab. med. Włodzimierz Samborski
Streszczenie
Fibromialgia jest niezapalną chorobą z bólem, cechującą się uogólnionym bólem i rozlaną tkliwością. Głównymi objawami towarzyszącymi są: zmęczenie, zaburzenia snu, bóle głowy i zaburzenia pamięci. Przyczyna choroby jest nieznana i jest przedmiotem wielu hipotez. Rozpoznanie fibromialgii opiera się na różnorodności objawów, w tym nie zapalnym uogólnionym bólem tkanek miękkich. Leczenie chorych na fibromialgię jest trudne i obejmuje stosowanie antydepresantów, leków zmniejszających napięcie mięśni oraz edukację chorego, psychoterapię i fizjoterapię.
Summary
Fibromyalgia is painful, noninflammatory disease characterized by widespread pain and diffuse tenderness. The main symptoms are accompanied by fatigue, sleep disturbances, headaches and memory impairment. Etiology of fibromalgia remains unknown and is a subject of several hypotheses. Diagnosis of fibromyalgia is based on variety of symptoms including noninflammatory generalized pain of the soft tissues. Treatment of patients with fibromyalgia is difficult and includes administration of antidepressants, muscle relaxants as well as education, psychotherapy and physiotherapy.

Fibromyalgia (FM) belongs to the group of soft tissue rheumatism disorders. That group includes: chronic, systemic arthralgia and myalgia, as well as algesthesia in typical spots called “tender points” (1, 2). Other symptoms possible to appear during the course of the disease are: hypokinesia of muscles and joints, myasthenia gravis, chronic fatigue syndrome and persistent feeling of being shattered, sleep disorder, numerous functional and psychopathological symptoms (3,4). Progression of fibromyalgia and intensification of symptoms vary, therefore the clinical picture of fibromyalgia can be diverse (5).
Frequency of occurrence of fibromyalgia ranges from 2 to 4% of the population. In rheumatological practice that percentage is higher, reaching 7 to 8% (6). Patients who suffer from fibromyalgia are usually white, aged 20 to 50 (7), with female to male ratio from 6:1 to 9:1 (8). The number of cases of fibromyalgia observed by pediatricians is on the increase (9).
There are numerous hypotheses about factors which may trigger occurrence of the disease. Those include sleep disorder in phase IV (NREM – non-rapid eye movement sleep), abnormal serotonin (5-hydroxytryptamine or 5-HT) metabolism and stress. Recently, an essential role has been attributed to the effect of so called “central sensitization”. Other concepts listed by the available literature include: decreased concentration of serum calcitonin, disturbances within the immune system, as well as the hypothalamic-pituitary-adrenal (HPA) axis disorder, which manifests with decreased secretion of cortisol due to corticoliberin stimulation (corticotropin-releasing factor – CRF) or decreased synthesis of the growth hormone (GH) (10). The actual cause remains unexplained.
The most important and distinctive symptom of fibromyalgia is systemic pain. It is chronic with periods of intensification, described by the patients who suffer from it in a very dramatic and evocative way, compared to burning or mutilation of the body. The pain is usually located in the juxtavertebral and large juxtaarticular areas. Intensification of pain depends on various factors which may cause strain on the system. Those factors may be of both external and internal origin (11). External factors include excessive physical effort, viral and bacterial infections, invasive diagnostic procedures, ingested medicine, injuries and traumas, changing environmental conditions. Internal factors are: neurogenic mechanisms, hormonal disorders and hypohydration, psychosocial and personality-related factors, as well as other psychical disorders and disturbances.
Systemic, chronic pain and presence of “tender points” (second distinguishing feature of fibromyalgia) form the diagnostic criteria of the disease (12, 13). The pain should last at least 3 months and be systemic, that means affecting both sides of the body, over and under the thoracic diaphragm, in line with the body axis (in the cervical, thoracic and lumbar regions of the vertebral column or on the anterior surface of the chest. Therefore, this criterion is met if the patient describes pain as located, for example, in the right shoulder, left hip or cervical spine (14).
The second diagnostic criterion, so called “tender points”, are hypersensitivity to pressure applied to specific points corresponding to tendon attachment points or other areas where they are located. There are nearly 100 distinguished spots, however only 20 are the most characteristic, while 18 of them are used for examination and diagnosis (15, 16). Those points are examined by palpation in order to test their sensitivity to pressure. Palpation is conducted with a thumb or index finger, with a pressure force of about 4 kg.
Locations of those points are:
– the occiput – tendon attachments in the occipital area,
– the inferior part of the net – intratransverse process spaces between C5-C7 vertebrae,
– a point on the superior margin of the trapezius muscle, in the middle of the distance between the shoulder and the neck,
– the supraspinatus – a point in the middle of the muscle, above the superior margin of the scapula,
– the second rib – on the superior margin, slightly lateral to the costal cartilage,
– lateral epicondyle – 2 cm distally from the lateral epicondyle of the humerus,
– regio glutealis – the region of superior, exterior quadrant of the gluteal sulcus,
– the greater trochanter – a point positioned behind prominentia trochanterica,
– the knee – the medial region of the knee (fad pad), proximally to the joint gap.
A spot is considered positive if applied pressure causes significant pain, reported by the patient verbally, by a grimace or wince of pain, alternatively by retraction of the extremity (‘a jump sign’) (17). The criterion pertaining to ‘tender points’ is met if at least 11 out of 18 examined points are hypersensitive (fig. 1).
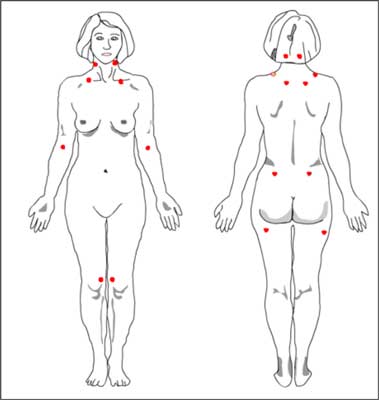
Fig. 1. “Tender points”.
Source: http://www.ucc-ny.com/conditions-treated/fibromyalgia.html
Several symptoms may be observed in the course of FM. Symptoms distinctive for FM include the following:
– hypokinesia of muscles and joints, which increases in the mornings, yet can last for the whole day, affects 80% of patients and requires differentiation from hypokinesia distinctive for other rheumatic diseases,
– weakening of the isometric and isokinetic strength of the muscles (myasthenia gravis) (18), with accompanying decreased endurance, work output and grasping power,
– chronic fatigue syndrome – constant fatugue, weariness, reluctance to any physical effort,
– sleep disorder (19): shallow, short and interrupted sleep with accompanying frequent breaks and, as a consequence, morning weariness and pains in muscles and joints.
Another group of FM symptoms comprises so called autonomic disorders, which are very difficult to substantiate, even with additional tests and object examination.
The most common of those symptoms are:
– feeling of cold hands and feet,
– dryness in the mouth and throat,
– excessive perspiration,
– vertigo,
– positive dermographism,
– headaches and migraines,
– gastrointestinal disorders (irritable bowel syndrome),
– foreign body sensation in the throat,
– sensation of irregular heartbeat (palpitation),
– temporary feeling of lack of air,
– paresthesia,
– dysuria.
Moreover, many neuropsychological disorders may also be observed, like emotional disturbances:
– anxiety,
– emotional stress,
– personality disorders,
Powyżej zamieściliśmy fragment artykułu, do którego możesz uzyskać pełny dostęp.
Mam kod dostępu
- Aby uzyskać płatny dostęp do pełnej treści powyższego artykułu albo wszystkich artykułów (w zależności od wybranej opcji), należy wprowadzić kod.
- Wprowadzając kod, akceptują Państwo treść Regulaminu oraz potwierdzają zapoznanie się z nim.
- Aby kupić kod proszę skorzystać z jednej z poniższych opcji.
Opcja #1
29 zł
Wybieram
- dostęp do tego artykułu
- dostęp na 7 dni
uzyskany kod musi być wprowadzony na stronie artykułu, do którego został wykupiony
Opcja #2
69 zł
Wybieram
- dostęp do tego i pozostałych ponad 7000 artykułów
- dostęp na 30 dni
- najpopularniejsza opcja
Opcja #3
129 zł
Wybieram
- dostęp do tego i pozostałych ponad 7000 artykułów
- dostęp na 90 dni
- oszczędzasz 78 zł
Piśmiennictwo
1. Mease PJ, Clauw DJ, Arnold LM et al.: Fibromyalgia syndrome. J Rheumatol 2005; 32: 2270-2277.
2. Turk DC, Flor H: Primary fibromyalgia is greater than tender points: toward a multiaxial taxonomy. J Rheumatol 1989; 19: 80-86.
3. Müller W, Lautenschläger J: Die generalisierte Tendomyopathie (GTM).
4. Klinik I: Verlaufund Differentialdiagnose. Z Rheumatol 1990; 49: 11-21.
5. Samborski W, Stratz T, Kretzmann WM et al.: Vergleichende Untersuchungen ueber das Vorkommen vegetativer und funktioneller Beschwerden bei Lumbalgien und generalisierten Tendomyopathien. Z Rheumatol 1991; 50: 378-381.
6. Littlejohn G, Walker J: Realistyczne podejście do problemu leczenia chorych na fibromialgię. Current Rheumatology Reports 2002; 4: 286-292 (Polish education).
7. Samborski W, Stratz T, Sobieska M et al.: Vergleichende Untersuchungen ueber Haeufigkeit, Geschlechts- und Altersverteilung bei generalisierten Tendomyopathie (GTM) und chronischem Lumbalsyndrom. Akt Rheumatol 1992; 17: 87-89.
8. Yunus MB, Holt GS, Masi AT et al.: Fibromyalgia syndrome among the elderly. Comparison with younger patients. J Am Geriatr Soc 1988; 36: 987-995.
9. Yunus MB: The role of gender in fibromyalgia syndrome. Curr Rheumatol Rep 2001; 3(2): 128-134.
10. Roizenblatt S, Tufik S, Goldenberg J et al.: Juvenile fibromyalgia: clinical and polysomnographic aspects. J Rheumatol 1997; 24: 579-585.
11. Samborski W: Fibromialgia – studium kliniczne i biochemiczne. Rozprawa habilitacyjna. AM Poznań 1998.
12. Samborski W: Fibromialgia. Reumatologia 1994; 32: 319-327.
13. Müller W: The fibrositis syndrome: diagnosis, differential diagnosis and pathogenesis. Scand J Rheumatol 1987; 65: 40-53.
14. Thompson EN: Diagnostic criteria for fibromyalgia. Arthritis Care Res (Hoboken) 2010; 62: 1674-1675.
15. Häuser W, Eich W, Herrmann M et al.: Fibromyalgia syndrome: classification, diagnosis, and treatment. Dtsch Arztebl Int 2009; 106: 383-391.
16. Harth M, Nielson RW: The fibromyalgia tender points: use them or lose them? A brief review of the controversy. J Rheumatol 2007; 34: 914-922.
17. Samborski W, Stratz T, Sobieska M et al.: Druckpunktenuntersuchungen bei der generalisierten Tendomyopathie (Fibromyalgie) (Vergleich verschiedener Methoden). Z Rheumatol 1991; 50: 382-386.
18. Salli A, Yilmaz H, Ugurlu H: The relationship between tender point count and disease severity in patients with primary fibromyalgia. Rheumatol Int 2010 (abstract PubMed).
19. Jacobsen S, Danneskioeld-Samsoe B: Dynamic muscular endurance in primary fibromyalgia syndrome compared with chronic myofascial pain syndrome. Arch Phys Med Rehabil 1992; 73: 170-173.
20. Leslie M: Fibromyalgia syndrome: a comprehensive approach to identification and management. Clin Excell Nurse Pract 1999; 3:165-171.
21. Watson NF, Buchwald D, Goldberg J et al.: Neurological signs and symptoms in fibromyalgia. Arthritis Rheum 2009; 60: 2839-2844.
22. Russell U: Biochemical abnormalities in fibromyalgia syndrome. J Musculoskeletal Pain 1994; 2: 101-115.
23. Lempp HK, Hatch SL, Carville SF, Choy EH: Patients’ experiences of living with and receiving treatment for fibromyalgia syndrome: a qualitative study. BMC Musculoskelet Disord 2009; 10: 124.
24. Samborski W, Stratz T, Schochat T et al.: Biochemische Veranderungen bei der Fibromyalgie. Z Rheumatol 1996; 55: 168-173.
25. Hedenberg-Magnusson B, Ernberg M, Alstergren P et al.: Effect on prostaglandin E2 and leukotriene B4 levels by local administration of glucocorticoid in human masseter muscle myalgia. Acta Odontol Scand 2002; 60: 29-36.
26. Karsdorp PA, Vlaeyen JW: Active avoidance but not activity pacing is associated with disability in fibromyalgia. Pain 2009; 147: 29-35.

