*Éva Gellèrnè Lukács1, Laura Gyeney2, Gábor Kovács3, Sándor Illès4
Third-country nationals in the Hungarian public health care sector
1Postgraduate Institute, Faculty of Law, Eötvös Loránd Tudományegyetem University, Budapest
Head of Faculty: prof. Miklós Király
2Faculty of Law, Pázmány Pèter University, Budapest
Head of Faculty: prof. András Zs.Varga
3István Szèchenyi University, Győr
Head of Faculty: prof. Judit Fazekas Lèvaynè
4Director, Active Society Foundation, Director, Budapest
Summary
Health care effects of international migration are the emerging themes within mobility studies. Unfortunately, there is scarce information on health situation of international migrants in Hungary. This paper tries to fill in this gap partly. The research deals with the access of third-country nationals to the Hungarian public health care system and the practices in reality. The authors carried out field works with the holistic approach in National Ambulance Service and Semmelweis University due to approximately half of the medical treatment for third-country nationals occur in Central Region. The volumes and rates of Ukrainian, Serbian, American, Russian and Chinese nationals are the dominant groups both institutions. Most third country citizens appear at the Obstetric Clinic because of childbirth. The second most demanded health care provider is the Central Laboratory. The third largest number of cases measure in the Transplant Clinic as a consequence of ageing process. According to the interviews, we suppose that the high standard of services make these clinics attractive to third country citizens. Lastly, we identify the main factors affecting the provider and supplier side of public health care system in Hungary.
Introduction
The research, on the findings of which this article is based on, aimed at examining the access of third-country nationals to the Hungarian public health care system1. The zero hypothesis of the research emphasised that access of third-country nationals to the Hungarian health care system goes along the same lines (procedures) with Hungarian insured persons, albeit certain cultural, linguistic and administrative differences (difficulties) might occur. The research tried to reveal data, trends and specific characteristics which would support or tinge the hypothesis.
Various data types and methods were used during the research. Firstly, field work was carried out with multiple methods, according to the requirements of the holistic approach. With the help of in-depth interviews valuable quantitative and qualitative information was obtained from publicly financed service providers. Secondly, in order to provide for a basis of comparison, quantitative data from larger administrative sources was also collected and also the legal rules in force were analysed. The basic macro data of the project erected, on the one hand, from the National Ambulance Service (NAS). Hence NAS is the sole Hungarian publicly financed emergency health care service provider, data handed over by the NAS shall be looked at as representative. On the other hand, data was provided by the Semmelweis University Budapest (SE), Hungary’s oldest medical school and one of its largest health care provider that runs 27 clinics.
The general characteristics of the data were as follows: full scope and register-based. Firstly, it meant that the inevitable distortions of data types did not burden the validity of information. Secondly, time series could have been created in order to discover short and medium term trends related to demographic and labour market situation, legal status of third-country nationals. Hence dual citizens tend to resort to health care benefits on the basis of their Hungarian nationality (e.g. Serbia, Croatia, The Ukraine, USA) data reflect the actual citizenship without Hungarian nationality.
Review of literature
The selective structure of migrant subpopulation is mostly valid for the health conditions of mobile people in modern era. The health status of migrants with the decision of free will is better than that of the inhabitants of the receiving or sending areas in general (1, 2). The interrelation between health and migration is a multifaceted part of scientific exploration. There has been growing interest on these relations in Hungary since the change of the political regime. The topic of health conditions of foreign immigrants were underexplored (3). The health status of Hungarian emigrants was completely out of the scope of research and public debates. In contrast, international migration of health professionals has been in the highlight of migration studies and media coverage due to the continuous emigration of Hungarian health personnel (4-7). In fact, Hungary’s accession to the European Union and the Schengen Area created a completely new international migration situation both for third-country nationals and for the destination countries (8-10). In the context of defending national interest more and more information became necessitated for Hungarian authorities and other bodies, including on the volume of third-country nationals’ access to the health care system, in order to judge the potential effects. There is scarce information on the health situation of international migrants in Hungary. This paper tries to partly fill in this gap by giving some facts and figures on the participation of third-country nationals in the Hungarian public health care system.
Spatial aspect
Both statistical data collected during the research and the interviews showed that if third-country nationals decide to obtain health care services in one of the publicly funded health care providers in Hungary, they are likely to acquire it in the Central Region. In the capitol Budapest and in the county surrounding Budapest (Pest county) approximately half of all medical treatments of third-country nationals occurred. SE and its institutions provide 80% of the public health care services for non-Hungarian and non-EU nationals in Budapest. In this geographical region data from 19 clinics, 3 hospitals and 2 health centres were processed thoroughly.
Looking at the regional service suppliers, almost exclusively universities’ clinic centres provide in kind health care services, e.g. Szeged University that is situated very close to the Hungarian-Serbian border. Third-country nationals rarely attend other hospitals, and these in-patient cases mostly fall within the sphere of emergency care. The contribution of regional out--patient clinics is also minimal in this field. For example third-country national patients are not recorded to receive treatment in the Western counties (counties Győr--Moson-Sopron, Fejèr and Baranya). Data on in-patient and out-patient care from the countryside derived from the database of the National Health Insurance Fund and 3 county-level centres. Moreover, data provided by the 18 county-level branches of the NAS have been analysed. Interviews revealed that – in addition to linguistic problems- in these institutions there is a lack of actual knowledge on the legal background of providing health care benefits for non-Hungarians, especially as regards the method of accounting. This applies equally to the acceptance of travel insurance and health care cards used by non-Hungarian citizens.
National Ambulance Service
Pursuant to Act CLIV of 1997 on Health non-Hungarian nationals staying or residing in Hungary shall be given immediate medical care if their medical status threatens their live, physical or mental integrity. The intervention shall be provided on the basis of the same criteria as for Hungarian nationals, including ambulance services. Ambulance service – due to its character – is unplanned care, consequently, the analysis of the statistical data of the sole Hungarian public provider, NAS, gives real information on the volume of unplanned medical cases of third-country nationals in Hungary. The reliability of the data is ensured by the fact that this service is provided by a state-funded organisation and all ambulance services belong to this organisation. Ambulance service as a task is base-financed, so data is not distorted by the anomalies in the reporting of financing scores. NAS has 230 stations in the 7 regions of Hungary and employs more than 7000 ambulance officers. It provides national emergency healthcare services which cover the whole territory of the country. It gives services for approximately 1 million patients yearly.
Data of the NAS give a comprehensive and complete overview on the characteristics of persons in need of ambulance services. The following four elements are presented here: the total number of cases in which third-country national patients were involved, spatial aspect (share of patients per regions), distribution per nationality and the types of healthcare needed by migrants in the years of 2011 and 2012.
Table 1 shows the total number of cases in which third-country national patients were involved in the years of 2011 and 2012 by months.
Table 1. Total number of cases of NAS in 2011 and 2012 by month (except October to December 2012 which data was not available during the research) (1: 175).
| Month | 2011 | 2012 |
| 01 | 158 | 160 |
| 02 | 153 | 127 |
| 03 | 145 | 153 |
| 04 | 172 | 168 |
| 05 | 164 | 187 |
| 06 | 211 | 238 |
| 07 | 259 | 263 |
| 08 | 226 | 234 |
| 09 | 225 | 235 |
| 10 | 217 | 0 |
| 11 | 147 | 0 |
| 12 | 153 | 0 |
The rate of third-country nationals is low in the NAS’s service, it amounts to 100-200 cases per month, out of the appr. 1 million cases per year. The number of cases increases in the summer and in the beginning of autumn. It is likely to be attributed to tourism because in these seasons a lot of third country nationals visit Hungary, primarily the shores of Lake Balaton (11). This sequence is well observable in both of the examined years.
Table 2 contains the spatial aspect of data in the years of 2011 and 2012.
Table 2. Spatial aspect (regional split up) of cases of NAS in 2011 and 2012 (16: 177).
| Region | 2011 | 2012 |
| Central Hungary | 43.59% | 47.59% |
| Northern Great Plain | 22.15% | 18.75% |
| Southern Great Plain | 11.43% | 12.12% |
| Western Transdanubia | 6.19% | 6.23% |
| Central Transdanubia | 5.92% | 6.01% |
| Southern Transdanubia | 5.65% | 4.87% |
| Northern Hungary | 5.07% | 4.42% |
The overwhelming majority of third-country nationals (almost half of all cases) were treated in Central Hungary: in the capitol Budapest and in its surrounding county Pest. The proportion of the Regions of Northern Great Plain and Southern Great Plain is also significant – the share of the remaining four regions amounts altogether to appr. 20 percent.
Table 3 presents the share of third-country national patients based on their nationality.
Table 3. Share of third-country national patients in 2011-2012 by nationality (16: 178).
| Country | 2011 |
| Ukraine | 15.11% |
| Ex-Yugoslavia (Serbia, Montenegro) | 9.37% |
| United States of America | 8.52% |
| Russia | 6.32% |
| Afghanistan | 6.32% |
| China | 5.78% |
| Other | 48.57% |
| Country | 2012 |
| Ukraine | 14.39% |
| Russia | 7.76% |
| Ex-Yugoslavia (Serbia, Montenegro) | 7.54% |
| United States of America | 6.80% |
| Turkey | 6.01% |
| China | 6.01% |
| Afghanistan | 5.33% |
| Other | 46.18% |
There is no relevant difference between the most numerous nationalities in the examined two years. The share of Ukrainian, Serbian, Russian, American and Chinese nationals is the highest. The significant percentages of other citizens echo the large heterogeneity of internationally mobile people arriving in Hungary with different status (12).
It is to be noted that the split up by nationality and by region of the NAS data shows strong correlation with the administrative data gained from the National Health Insurance Fund (NHIF) on the total numbers of third-country national patients in Hungary. The data of the NHIF from 2006-2010 (tab. 4) stresses that the aggregate share of the most considerable nationalities is outstandingly high, and these nationals came from seven countries, namely Ukraine, China, Vietnam, former Yugoslavia, Serbia, Russia and Mongolia. Also, the geographical concentration is essential, almost the entire third-country population was treated in Budapest and in five counties (Szabocs-Szatmár-Bereg, Pest, Csongrád, Bács-Kiskun and Hajdú Bihar). Besides Budapest having the leading role, these counties are remarkably characterised by having a well-known university clinic or large hospital in their territory.
Table 4. Aggregate data on third-country nationals medical care in Hungary between 2006-2010 (16: 26).
| Type of treatment | Number of care recipients | Proportion of the seven most considerable nationalities of care recipients (%) | Proportion of the care recipients treated in the six most considerable counties (%) | Proportion of Budapest (%) |
| Acute care | 11 776 | 82 | 94 | 61 |
| In-patient care | 9414 | 94 | 95 | 63 |
| Dental care | 18 123 | 86 | 86 | 55 |
| Out-patient care | 72 306 | 79 | 85 | 57 |
| Cash benefit | 3961 | 93 | 94 | 66 |
It is to be traced that the appearance of third-country national patients echoes some of the former socialist countries of the past century. It is suggested that the research, parallel to describing current trends, also faced the heritage of the past, almost 50 years long history.
The Semmelweis University (SE) as a central provider
Based on the countrywide statistical findings as regards nationality and geographical split up of third-country patients (as described above), our research foresaw an in-depth assessment of the situation in the largest health care institution of Budapest, in the SE. This seemed reasonable hence SE covers six percent of the entire population’s health care needs, which translates to around 2.3 million cases per year, with its 27 clinics and more than 8000 employees. The SE submitted its full-scale statistical data from the year of 2011 regarding patients from third countries. The statistical data respond many relevant questions, it shows the different nationalities of patients in the public health care system, as well as lists those clinics where these services were obtained. Table 5 gives a general overview on the absolute number of cases, attributed to the clinics providing professional health care.
Table 5. Absolute number of third-country national patients in the clinics of the SE in 2011 (16: 219).
| Clinic | Number of cases |
| Obstetric Clinic | 1432 |
| Central Laboratory | 1348 |
| Transplant Clinic | 754 |
| Kútvölgyi Hospital | 602 |
| Paediatric Clinic | 559 |
| Ophthalmology Clinic | 551 |
| Internal Medicine Clinic | 432 |
| Dermatology Clinic | 319 |
| Cardiology Centre | 231 |
| Otolaryngology Clinic | 190 |
| Surgical Clinic | 171 |
| Pulmonology Clinic | 167 |
| Radiology Clinic | 165 |
| Urology Clinic | 130 |
| Pathology Institute | 124 |
| Neurology Clinic | 116 |
| Psychiatry Clinic | 59 |
| Anaesthesiology Clinic | 52 |
| Orthopaedics Clinic | 49 |
| Vascular Surgery Clinic | 25 |
| Clinical Psycholgy | 23 |
| Kútvölgyi Psychology | 15 |
| Nuclear Medicine | 11 |
| Cardiac-surgery Clinic | 9 |
| Other | 9 |
| Total | 7543 |
Pursuant to the data from 2011 appr. 7500 patients were third-country nationals out of the total number of patients, appr. 2.3 million. This amounts to an appr. 0.32%. Most third country nationals appeared at the Obstetric Clinic. Although the large number of obstetric cases reflects the number of childbirth (birth in hospital as a general example) it may also suggest the demand for in vitro fertilization. However, there is no separate data available in this topic. The second most demanded health care provider is the Central Laboratory. The number of cases indicates that diagnostic and laboratory tests are essential, as there is no proper medical care without laboratory diagnostics. The third largest number of cases is attributed to the Transplant Clinic as a probable consequence of the ageing process. The percentages of cases attributable to clinics on the basis of table 5 result in 19% of the cases for the Obstetric Clinic, 18% for the Central Laboratory and 10% for the Transplant Clinic. It is even more visible that almost one fifth of the cases are related to obstetric cases. According to the interviews, the high standard of services makes these clinics attractive to third-country nationals.
Table 6 and figure 1 below display the absolute numbers and relative values of the share of third-country national patients in 2011 in the SE.
Table 6. Absolute numbers and relative values of the share of third-country national patients in 2011 in the SE (16: 223).
| Nationality | Number | % |
| Ukraine (UKR) | 951 | 13% |
| United State of America (USA) | 782 | 10% |
| China (CHI) | 666 | 9% |
| Russia (RUF) | 646 | 9% |
| Vietnam (SRV) | 594 | 8% |
| Iran (IRN) | 540 | 7% |
| Serbia (SRB) | 240 | 3% |
| Nigeria (NIG) | 223 | 3% |
| Montenegro (MNG) | 218 | 3% |
| Kazakhstan (KAZ) | 211 | 3% |
| Turkey (TUR) | 193 | 3% |
| Canada (CAN) | 180 | 2% |
| Syria (SYR) | 175 | 2% |
| Iraq (IRQ) | 150 | 2% |
| Afghanistan (AFG) | 138 | 2% |
| Israel (ISR) | 129 | 2% |
| Other | 1507 | 20% |
| Total | 7543 | 100% |
Fig. 1. Absolute numbers and relative values of the share of third-country national patients in 2011 in the SE (16: 223).
As regards the large number of Ukrainian and Serbian nationals, the question arose whether these persons belong to the Hungarian minority community from Lower-Carpathia and Vojvodina and whether they seek medical care on a regular basis in Hungary (mainly as habitual residents). We crosschecked this data with the data of the Office of Immigration and Nationality (OIN), which suggested, that indeed, many Serbian and even more Ukrainian citizens had applied for national residence permit at the authorities2. (Ukrainian, Serbian and Croatian citizens are eligible for submitting applications for national visa and national residence permit which is strongly related to preserving cultural identity)3. Consequently, in their case the primary aim of being in Hungary is overwhelmingly the habitual residence itself and not social tourism.
Also, we assessed the probability, whether other foreigners, for example Russian and US nationals do have the initial intention to resort to Hungarian health care services or the case numbers are rather attributable to occasionally returning immigrants of Hungarian origin. This data has been crosschecked with the data of the OIN that showed very small numbers of persons who applied for residence permits in Hungary. Albeit the number of medical treatments is high compared to the number of the immigrant population, there does not evolve any tendency of requiring high cost medical care and in big numbers. In case of US nationals the regular medical visits may be construed as a cultural attitude and in the light of the old age structure of American immigrants (13, 14).
It can also be stated, that the number of Iranian patients is surprisingly large. According to the data of the OIN many of them are elderly immigrants who had arrived to Hungary 50 years ago. However, most of them are young university students because Iranian students are being positively encouraged by their government to enter Hungarian higher education. Their number is about 2000. There is a Hungarian-Iranian cultural framework convention, renewed every 4 or 5 years, very much supported by Hungarian institutions as well. There are 400 Iranian students at the University of Debrecen, 200 at the University of Pècs. Most of the students attend the SE in Budapest, medicine and pharmacy are the most popular faculties. Also, there are a few students at the Technical University of Budapest and at the Central European University. These Iranian youngsters have a secularised lifestyle, they do not find it hard to fit in, and most of them come from wealthy families. This, however, might also mean that their stay is not long term.
Figure 2 shows lists the SE clinics where third-country nationals obtained health care services in 2011. Patients coming from the 5 largest migrants groups by order of the clinics are presented (SRV – Vietnam, RUF – Russia, CHI – China, USA – United States of America, UKR – Ukraine).
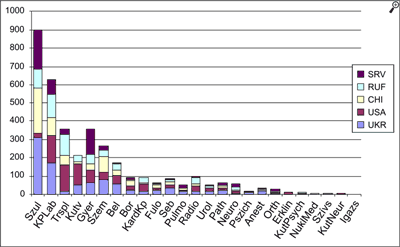
Fig. 2. Type of care by the 5 largest third-country national groups in 2011 (16: 229).
The statistical data suggests that the high number of obstetric care among the Ukrainian, Chinese and Vietnamese citizens presupposes and indicates habitual residence in Hungary. In contrast, the number of obstetric care of US national is relatively small, probably because generally the middle-aged or the elderly obtain medical care.
Among the Vietnamese nationals paediatric cases are quite prevalent. However, the exact type of treatments in these cases is not known. Hence the majority of the Vietnamese population reside in Hungary with their families (and small children) it would seem a logical explanation that they claim general health care services also for their children, and in this way, depending on their children’s age, predominantly paediatrics, ophthalmology and otolaryngology. One of our interviewees mentioned, that the Paediatric Clinic is very popular among the foreign population in Budapest, as the hospital is a research centre and there are fundamental requirements for all the doctors to speak English.
It is striking from the statistics that among Chinese nationals there are no cardiologic cases. The rate of Americans however, is high at the cardiology, vascular surgery and cardio-surgery clinics. The data may be traced back to the higher age composition of the residing Americans, and also in their social attitude towards health care. In western medicine even the slightest heart disorder is taken very seriously and treated as cardiologic problem while eastern prospective treats it as part of the traditional medicine.
The data shows high transplantation rate among Russian nationals. Russian nationals had arrived in Hungary for several different reasons in the past. During the era of the Soviet Union, there were plenty of Russian nationals moving to Hungary, due to professional relations: engineers, agricultural- and industrial professionals and their families accompanying them. There was a major change in the 90ties, many of the former Russian residents left the country after 1989 but many new business representatives moved to Hungary. The higher rate in transplants could also be connected to wealthy Russian nationals who may be travelling in order to access a higher standard of healthcare as health-care-tourists. But this is deteriorated by the presumption that they probably tend to obtain health care services from private health care providers and not from the public health care system. For them the sphere of private service providers might be regarded as a serious alternative.
The number of radiological cases is rather high. We believe that especially in this segment immigrants – due to language problem issues – simply skip the primary care (basic level of health care in out-patient care) and enter the system directly at the higher level (professional health care in the Clinics). As it has been emphasised by many of the interviewees, the Clinics are the easiest to access for foreigners considering the fact that language skills of the staff – the doctors, and part of the nurses speak different languages – are very good. It is also important to mention, that foreigners share their experience within their community, they spread the information and they have very accurate knowledge – in almost every case – how to use best the available health care services.
Factors affecting the provider and recipient side of health care system
The results of the empirical data collection on the most relevant factors that can affect third country nationals’ decision on choosing the Hungarian healthcare system can be summarised as follows.
The high-standard physician-education and its „internationalization”
The reputation of the Hungarian physician education (in particular general medical and dental training) is high which attracts a significant number of foreign students, and not only in Budapest, but also in other universities in the countryside (e.g. in Szeged, Debrecen). The participation of foreign medical students in the Hungarian physician education not only sensitizes the university clinics but gives impetus to internationalization both in the provider and the recipient side.
„The number of foreign students enrolled in the Semmelweis University was increased with 145 persons last year, so almost each fourth student learns in English or in German, there are 2977 foreign students from the 12 thousand. Most of them attend the General Medicine Faculty, there are 2103 foreigners from the 4321 students” – reports the Semmelweis News on the school year 2011/12. SE treats internationalization as a priority; its speciality is the three language education (Hungarian, English and German). 20 per cent of the students are non-Hungarian, they come from 60 countries and 5 continent, dominated by European sending countries (Germany, Norway, Italy Spain) and followed by Israel and Iran.
In 2010/2011 the situation in Szeged was also remarkable, there were 933 enrolled foreign students arriving from 49 different countries in the general medicine, dental and pharmacist faculties (15).
The role of the expertise in the healthcare services
The diagnostic potential (laboratory, CT) must be highlighted from the capacities that are provided for foreigners but ophthalmology, traumatology, orthopedia, surgery and rehabilitation also offer high-tech services. Several public healthcare institutions use the same methods like the expensive private clinics.
In ophthalmology, for example, some hospitals have really modern equipment like OCT (optical coherence tomograph), IT-based blood vessel colouring, digital video device, etc. On the one hand these instruments ensure up-to-date diagnostic method and ensure better consultative opportunities for the physicians, healthcare staff and patients, too. On the other hand in some cases the lack of infrastructure (i.e. operating room), the lack of appropriable staff (i.e. anaesthesiologist) might influence the overall quality of medical care.
Specific features of providing medical care for non-Hungarians
It is worth examining which factors are specific for non--Hungarian patients throughout the procedure of medical care by referring to the establishment of the anamnesis, to the lack of accessibility of the former medical records of the patient, to medication and to the issue of aftercare.
The starting point of each physician-patient relationship is the initiation of the anamnesis. Much confidence is needed to build it up and sometimes it is really problematic for the foreign patients to understand the physician’s questions and to respond. Also, important facts might be forgotten or not told because of shyness or any other reasons. The lack of accessibility of former medical records (even electronic [digital] healthcare records) and the lack of accessibility of documentations is of utmost importance, especially in the case of emergency. In several cases the medical staff cannot access and use this information which might aggravate their work. Medication of foreign patients could also be problematic because of possible allergy to medicaments. In turn drugs used by the patient at home are often unavailable in Hungary. Drugs whose name/trademark is unknown for the patient may make the compliance with the doctor’s orders dubious because the patient might be hesitant to use them.
Aftercare can also raise questions. For example, if a foreigner needs prosthesis it can only be granted if the possibility of permanent medical control is guaranteed. In case of artificial limbs the bone-relations are forming permanently, which means that newer and newer prosthesis is necessitated and its creation could be difficult after the patient’s return to his/her home country. The monitoring of the patient, the organization of the follow-up and the notification and information of the foreign physician who will continue to provide health care might pose significant problems. Additionally, distance from the domicile could be a serious difficulty including the lack of help of a relative, a friend, especially for patients suffering in chronic illnesses. Sometimes data protection and patients’ rights issues arise. Patients are entitled to access their own health data during their stay in the hospital, they can initiate the modification of the data if they find it false or they can copy it, they can expressly prohibit the usage of data by third persons. They can delegate their rights to their relatives or any other person. It is usual that patients and their relatives do not have enough information on their data protection and patients’ rights and on the types of documents used in hospitals.
The block of socio-cultural elements (language, communication, cultural differences)
Linguistic and communication difficulties might negatively influence the quality of medical care. Firstly, physicians usually do not have interpreter. In turn, the patient shall be informed on his/her rights in writing, and – with exceptions – paper forms used in hospitals are unilingual: Hungarian.
It is important to distinguish between the university clinics and other non-university non-educational healthcare institutions in the field of communication difficulties. Physicians working in clinics had to spend at least a few years in foreign research institutes as scholars; they have no communication problem in a widespread language – typically in English or German (14). They frequently use a foreign language. Although physicians speak quiet good foreign language(s) only few nurses and other healthcare workers have appropriate language skills. Admittedly, the low number of foreigner patients in non-centralized institutions does not facilitate the development of communicating in foreign languages.
There are certain forms of medical methods and therapies which expressively need the usage of the native language. An example is the rehabilitation of patients having a brain infarct because for the recovery native language is needed and it cannot be ensured in most of the cases.
Cultural and religious differences create many fold challenges for providers and recipients. Beyond the fact that patients might not exercise their regular religious rituals, problems could arise concerning the meal. Certain religious rules of Muslims and Jews emphasize to enjoy „allowed” or „right” meals and deny the consumption of „forbidden” or „unclean” ones. I.e. consumption of swine-flesh and any parts of pork is denied by several religions. Another good example should be found in the Jewish religion which forbids the consumption of meaty and milky meals right after each other. There are issues related to clothing. For example Muslim women have to cover their whole body during the medical inspection which might make certain medical examination infeasible. Finally, as widely-known, the members of Jehova’s Witnesses refuse the transfusion of whole blood, concentrated red blood cell, plasma or white red cell. They also refuse the transfusion of their own blood previously get from their own body and the surgery technique of blood-holding and blood-diluting methods if this technique contains blood-storage.
Progress can be traced in this field on the side of service providers, nowadays medical staff handle this question with much greater sensibility than a few decades ago – in the light of the given opportunities and boundaries. Majority of the interviewees agreed that there should be employees knowing foreign cultures in the institutions having a lot of patients with specific cultural attitudes, however, linguistic and cultural difficulties are not dominant. Recently, the approach of trans-cultural attitude is taught in high schools and postgraduate courses in Hungary.
Related financial and legal matters
The interviewed service providers considered the complexity of financing and administration as a significant problem. Physicians providing health care usually do not know the exact legal terms on the basis of which third-country nationals have access to the health care benefits. The system is too complicated in this regard and it is difficult to check whether the person is entitled to benefits under Hungarian law, European law or bilateral agreement. Doctors typically turn to the administration of the hospital for help in this context.
In the examined period and in the examined segment no legal proceedings for damages or for other reasons (medical ethics or patients’ rights-related) were reported in the public funded health care initiated by third-country nationals.
If a foreign patient does not have the proper certification (e.g. Hungarian social insurance identification number or forms required under a bilateral agreement) healthcare institutions issue a receipt, but allow the patient to justify his/her right in a few weeks. In these cases no additional costs shall be borne by the patient. However, if it turns out that the patient has no right under the publicly financed system, s/he shall pay for the services as if s/he was a private patient. If the patient does not pay the hospital may have a financial problem. If the provided care was emergency care and it proves that it was not able to collect the debts, the National Healthcare Insurance Fund reimburses the costs of the hospital.
Conclusions
The examination of health care effects of international migration is a fiercely discussed topic within mobility studies. There is scarce information on the health situation of international migrants in Hungary. This paper, which summarises the essentials of an extensive research, tries to partly fill in this gap by examining the access of third-country nationals to the Hungarian public health care system and the relating practices in reality.
As regards the nationality and regional split up of third-country national patients treated in Hungary, it is to be concluded that the aggregate share of the most considerable nationalities is outstandingly high (above 80%), and these nationals arrive from seven countries, namely Ukraine, China, Vietnam, former Yugoslavia, Serbia, Russia and Mongolia. Also, a significant geographical concentration is to be traced, almost the entire third-country population is treated in Budapest and in five counties (Szabocs-Szatmár-Bereg, Pest, Csongrád, Bács-Kiskun and Hajdú Bihar). Besides Budapest having the leading role, these counties are remarkably characterised by having a well-known university clinic or large hospital in their territory.
The authors carried out field works with a holistic approach in the National Ambulance Service and in the Semmelweis University Budapest. Approximately half of the medical treatments provided for third-country nationals occur in the Central Region. Most third country nationals visit the Obstetric Clinic because of childbirth. The second most demanded health care provider is the Central Laboratory. The third largest number of cases is attributed to the Transplant Clinic as a probable consequence of the ageing process. Here also the prevalence of Russian and American nationals can be traced.
The analysis revealed that third-country nationals residing in Hungary tend to skip the primary care (basic level of health care in out-patient care) and enter the system directly at the higher level (professional health care in the Clinics). The university clinics (being also research centres) are the easiest to access for foreigners considering the fact that the language skills of the staff are very good. It is also important to mention, that foreigners share their experience within their community, they spread the information and they have very accurate knowledge – in almost every case- how to use best the available health care services.
The main factors affecting the provider and recipient side of the public health care system in Hungary is presented. These are the high-standard physician-education and its „internationalization”, the role of the expertise in the healthcare services, specific features of providing medical care for non-Hungarians, the block of socio-cultural elements (language, communication, cultural differences) and related financial and legal matters.
1The project titled „Research about the access to the health care system” co-financed by Tullius Ltd., the European Integration Fund (EIA/2011/1.3.4.) and the Ministry of Home Affairs of Hungary, was implemented in 2012. The complete outcome of the research is available as a handbook under Gellèr Balázs József (szerk.) (2012) Harmadik országbeli állampolgárok hozzáfèrèse az egèszsègügyi ellátórendszerhez. Tullius Kiadó, Budapest, hereinafter referred to as (16).
2Office of Immigration and Nationality (OIN), www.bm-bah.hu (downloaded on 5 May 2012).
3See for more: http://www.bmbah.hu/jomla/index.php?option=com_k2&view=item&id=67:national-residence-permit&Itemid= 821&lang=en# (downloaded on 30 November 2014).
Piśmiennictwo
1. Termote M: Migration as a selection factor in a population. Some considerations on the relation between migration and genetics. [In:] Keyfitz N (ed.): Population and biology. Bridge between disciplines. Proceedings of a conference. Ordina Editions, Liege 1984: 133-146. 2. Loue S: (ed.): Handbook of Immigrant health. Plenum Press, New York and London 1998. 3. Szabó AF: Demográfiai problèmák biztonságpolitikai vonatkozásai egykor ès ma. (Demographic considerations of security policies in the past and recent era). Budapest, Zrínyi Miklós Nemzetvèdelmi Egyetem, 1999. 4. Vingender I, Mèszáros J, Kis J: Migration potential of Hungarian healthcare professionals – dynamics of attraction and repulsion. European Journal of Mental Health 2009; 4: 195-219. 5. Eke E, Girasek E, Szócska M: From melting pot to laboratory of change in central Europe. Hungary and health workforce migration. [In:] Wismar M, Maier CB, Glinos IA, Dussault GJ (eds.): Health Professional Mobility and Health Systems. Evidence from 17 European countries. Copenhagen, World Health Organisation – European Observatory on Health Systems and Policies 2011: 365-394. 6. Feith JH, Balázs P, Garaj E et al.: Plans for working abroad and career preferences among nursing students in Hungary. New Medicine 2010; 14: 22-24. 7. Matiscsák A: Applying the network research matrix methodology to identify and map the international migration of Hungarian nurses. New Medicine 2013; 17: 21-27. 8. Rèvai R, Görbe A, Zán K: Egèszsèg ès migráció az Európai Unióban ès Magyarországon. (Health and migration in European Union and Hungary). Hadmèrnök 2009; 4: 166-171. 9. Csepregi P, Huszár A, Rèvai R, Szilárd I: Migrációs egèszsègügyi kihívások a Schengeni határnyitás után. (Health care challenges of migration after Schengen epoch). Hadtudományi Szemle 2011; 4: 26-39. 10. Gellèrnè Lukács É: Free movement of persons – a synthesis. [In:] Somssich R, Szabados T (eds.): Central and Eastern European countries after and before the accession. I. Deparment of Private International Law and European Economic Law, Faculty of Law, ELTE University, Budapest 2011: 51-84. 11. Gödri I: International migration. [In:] Őri P, Spèder Zs (eds.): Demographic portrait of Hungary, Budapest. HCSO Demographic Research Institute 2012: 135-152. 12. Illès S, Michalkó G: Relationships between international tourism and migration in Hungary: Tourism flows and foreign property ownership. Tourism Geographies 2008; 10: 98-118. 13. Illès S, Kincses Á: Foreign retired migrants in Hungary. Hungarian Statistical Review 2008; 86: 88-111. 14. Illès S: International circular migration – brain circulation. [In:] Gellèrnè Lukács É, Ács V (eds.): Third-country national researchers’ integration in Hungary. Handbook and conference report. Tullius Publisher, Budapest 2011: 128-139. 15. Kereszty É: A Magyarországon tartózkodó külföldi szemèlyeknek nyújtott ellátások Szegeden. (Health care for foreigners staying in Hungary in Szeged). [In:] Gellèr BJ (ed.): Harmadik országbeli állampolgárok hozzáfèrèse az egèszsègügyi ellátórendszerhez. (Third-country nationals’ access to health care sector). Tullius Kiadó, Budapest 2012: 263-341. 16. Gellèr BJ (ed.): Harmadik országbeli állampolgárok hozzáfèrèse az egèszsègügyi ellátórendszerhez. (Third-country nationals’ access to health care sector). Tullius Kiadó, Budapest 2012.

