*Dorota Olczak-Kowalczyk1, Maria Borysewicz-Lewicka2, Barbara Adamowicz-Klepalska3, Teresa Jackowska4, Urszula Kaczmarek5
Consensus statement of Polish experts on individual caries prevention with fluoride in children and adolescents
Stanowisko polskich Ekspertów dotyczące indywidualnej profilaktyki fluorkowej choroby próchnicowej u dzieci i młodzieży
1Department of Paediatric Dentistry, Medical University of Warsaw; national consultant in paediatric dentistry
Head of Department: prof. Dorota Olczak-Kowalczyk, MD, PhD
2Chair and Clinic of Paediatric Dentistry, Karol Marcinkowski University of Medical Sciences in Poznań
Head of Chair and Clinic: prof. Maria Borysewicz-Lewicka, MD, PhD
3Former national consultant in paediatric dentistry
4Department of Paediatrics, Centre of Postgraduate Medical Education, Warsaw; national consultant in paediatrics
Head of Department: prof. Teresa Jackowska, MD, PhD
5Chair and Department of Conservative Dentistry and Pedodontics, Wrocław Medical University of Silesian Piasts
Head of Chair and Department: prof. Urszula Kaczmarek, MD, PhD
1,2,3,5The Alliance for a Cavity-Free Future, Polish Society of Pediatric Dentistry
Streszczenie
Jednym z głównych elementów zapobiegania chorobie próchnicowej jest stosowanie środków profilaktycznych zawierających związki fluoru. Skuteczność i bezpieczeństwo profilaktyki fluorkowej wymaga znajomości mechanizmu kariostatycznego działania fluoru oraz przestrzegania zasad stosowania środków profilaktycznych zawierających fluorki. W ramach działalności Grupy Roboczej ds. Profilaktyki Fluorkowej Polskiego Oddziału Sojuszu dla Przyszłości Wolnej od Próchnicy (ACFF) powołano zespół Ekspertów w dziedzinie stomatologii dziecięcej i pediatrii w celu opracowania stanowiska dotyczącego indywidualnej profilaktyki fluorkowej u dzieci i młodzieży w Polsce.
Dokonano przeglądu piśmiennictwa dotyczącego stomatologicznych potrzeb profilaktycznych pacjentów w wieku rozwojowym w Polsce, skuteczności i bezpieczeństwa stosowania środków profilaktycznych zawierających związki fluoru oraz zaleceń towarzystw naukowych w zakresie profilaktyki fluorkowej. Opracowaną pierwszą wersję dokumentu zrecenzował zespół Ekspertów w dziedzinie pediatrii i stomatologii dziecięcej oraz przedstawiciele rodziców/opiekunów dzieci. Ostateczny dokument został zaakceptowany przez zespół Ekspertów 12 grudnia 2015 roku. Aktualizację zaplanowano nie później niż po 5 latach od jego publikacji.
Dokument zawiera podstawowe informacje dotyczące potrzeb w zakresie zapobiegania próchnicy zębów u dzieci i młodzieży, mechanizmu przeciwpróchnicowego działania fluoru, bezpieczeństwa i skuteczności różnych metod profilaktyki fluorkowej i zasad jej stosowania w zależności od wieku i poziomu ryzyka próchnicy.
Summary
Using fluoride agents is one of key elements of caries prevention. For it to be safe and effective, it is crucial to know the cariostatic mechanisms of fluoride and follow the guidelines of fluoride use for caries prevention. Experts in paediatric dentistry and paediatrics prepared, within the The Alliance for a Cavity-Free Future working group (ACFF), guidelines on individual caries prevention for children and adolescents in Poland.
Publications featuring the need for prevention in children and adolescents in Poland, the effectiveness and safety of preventive fluoridation methods and guidelines of scientific societies on caries prevention have been reviewed. The first draft was reviewed by paediatricians, paediatric dentists, and the representatives of parents/legal guardians of patients. The final version of the document was approved on 12 December 2015. It will be updated not later than five years after it is published.
The document defines the basics of preventing dental caries in children and adolescents, the anticaries mechanisms of fluoride, the safety and effectiveness of different fluoridation methods, and their use depending on patient age and risk of caries.

Introduction
The basics of preventing dental caries include: proper nutrition, oral hygiene and preventive fluoride usage. Fluoride is used in mass, group-based and individual preventive methods. The World Health Organisation (WHO) and the World Dental Federation (FDI) recommend prevention with fluoride and underline its efficacy and safety. At the same time, they draw attention to the necessity of fluoride exposure monitoring and evaluation of its efficacy (1-3).
In individual prevention, fluoride can be delivered:
– orally (tablets or drops) – an endogenous method (supplementation); it affects the developing dental enamel,
– externally – an exogenous method by topical application on erupted teeth.
Toothpastes, mouthwashes, foams, gels and varnishes contain various fluoride concentrations. They can be used either in home settings (home prevention) or in a dentist’s office (professional prevention). Caries prevention with fluoride is safe and effective when the principles of individual preventive method selection are followed, taking into account exposure to fluoride from various sources, child’s age and risk of caries. According to the results of survey-based studies conducted in 2014 in Poland, 14.0% of dentists do not estimate the risk of caries prior to the selection of a preventive measure. Over a half of respondents believed that caries prevention with fluoride should be implemented in each patient, 38.9% claimed that it should be used irrespective of age when the risk of caries is high, and 21.3% responded that it is needed only for primary and mixed dentition (4).
It must be emphasised that the basic caries prevention in Poland can be conducted as part of publicly funded benefits (List of general dental benefits for children and adolescents under the age of 18 as well as List of dental benefits for children older than 6 months of age up to the age of 19 in the form of 13 packages of preventive treatments depending of age).
In 2013, a statement of the Independent Expert Panel on individual caries prevention was published (5). Due to the appearance of new studies and meta-analyses that reveal differences in the safety and efficacy of various fluoride-containing products in caries prevention, an update of this document is needed.
Material and methods
The working group of The Alliance for a Cavity-Free Future (ACFF) has conducted literature reviews on dental preventive needs of children and adolescents in Poland, mechanisms of action, efficacy and safety of fluoride in caries prevention in this group of patients and analyses of recommendations concerning caries prevention prepared by academic societies, such as: American Academy of Paediatric Dentistry (AAPD), European Academy of Paediatric Dentistry (EAPD) and American Dental Association (ADA). The outcomes constituted the basis for the first draft version (prepared by Professor Dorota Olczak-Kowalczyk and Professor Urszula Kaczmarek) which was handed to experts in paediatrics (Professor Teresa Jackowska) and paediatric dentistry (Professor Barbara Adamowicz-Klepalska and Professor Maria Borysewicz-Lewicka) as well as to the representatives of parents. Finally, having considered their remarks, the document was completed. Its final version was approved by a panel of experts on 30 November 2015. It will be updated not later than 5 years after it is published.
Results
Needs concerning dental caries prevention in Polish children
The fact that dental caries prevention is needed in Polish children has been confirmed by Polish epidemiological studies conducted since 1987 in concert with the World Health Organisation (6-9). The results of oral health status monitoring indicate that, in children aged 3-6, the number of primary teeth affected by caries increases from 2.7 to 5.3 and the frequency of caries increases by approximately 30%, from 57.2 to 85.6%. At 12 years of age, caries affects 2.8 permanent teeth, and this number doubles after 3 years (to 6.12 at the age of 15). After further 3 years, it increases by 2.4-fold and reaches 7.65 at the age of 18 (10-14). The presence of caries in the developing first molars is alarming. It is found in 3 children aged 5, 18 aged 6 and 56 aged 7 per 100 examined children (12, 14). When considering the tendencies of caries in 12-year-olds within 27 years (1987-2014), the frequency and intensity of caries was found to have decreased (from 89.9 to 75.9%, and from 4.4 to 2.8 affected teeth) (6, 13). The WHO and FDI’s global aim regarding oral cavity health was to reduce dental caries to 3 or fewer teeth to the year 2000 (15, 16). This aim was achieved in 70% of countries in the world, i.e. in 128 countries representing 85% of the world population, and the global average caries index (DMFT) was 1.74 (17). Unfortunately, only 48.9% of children achieved this aim by 2000. Ten years later, the value is greater by merely 10% (58.7%) (13, 18).
These data emphasise the relevance of strengthening dental preventive efforts in Poland and the need to engage not only dental professional practitioners, but also medical staff and patients’ guardians (19, 20).
The epidemiological studies have also confirmed the polarisation of dental caries, i.e. the presence of persons with high dental caries rates even when rates are generally low or moderate. It is therefore significant to distinguish high-risk individuals and implement intensive, individualised prevention in this group of patients.
Risk of caries and prevention with fluoride
The selection of a prevention method and type of fluoride products depends on multiple factors, including age, general health condition, systemic therapy used, preventive and therapeutic needs, caries risk level, exposure to fluoride from other sources as well as engagement and possibilities of parents. Caries prevention based on risk level assessment consists in the intensification of prevention when the risk increases. All children should undergo risk estimation before a preventive and caries-controlling treatment is implemented. This is critical for creating an individualised preventive plan.
The risk of caries is understood as the likelihood of new carious lesions in the future and progression of already existing ones. According to the concept of dynamic balance between tooth demineralisation and remineralisation, caries risk estimation is based on the relationship between factors considered to be preventive, which favour enamel remineralisation (fluoride usage, using antibacterial agents and fissure sealants, proper dietary habits, normal salivary flow) and pathological ones that cause its demineralisation (level of acid-producing bacteria, frequent consumption of fermenting carbohydrates, reduced salivary flow) as well as on establishing disease indicators (presence of incipient caries in the form of white spots, developmental enamel defects that favour plaque retention, number of fillings placed within < 3 years and the number of cavities reaching the dentine) (21-23).
There are no validated tools with known sensitivity and specificity to assess the risk of caries in children. This makes it challenging to establish basic preventive recommendations associated with the future risk of the disease. The assessment of validated tools for caries risk evaluation in adults has demonstrated that these tools are not highly accurate in establishing a prognosis for future caries. The best predictor of individual future caries development is current presence of affected teeth. There are several methods of assessing the said risk. The AAPD has proposed the CRA system (Caries Risk Assessment), which consists of three tools for caries risk evaluation, including two used by dental practitioners: for children aged 0-5 and > 6, and a non-dental one to be used by medical professionals for children aged 0-3 (tab. 1-3) (24).
Tab. 1. Caries risk assessment in children aged 0-5 by professional practitioners according to the CRA system (Caries Risk Assessment Test by AAPD) (24)
| Factors | High risk | Moderate risk | Low risk |
| Biological factors |
| Active caries in the mother/guardian | Yes | | |
| Low socioeconomic status of the family | Yes | | |
| Child consumes more than 3 sugar-containing snacks or sweet drinks daily | Yes | | |
| Child falls asleep with a bottle containing feed/fluid with natural or added sugar | Yes | | |
| Child requires specialist paediatric care | | Yes | |
| Child comes from immigrant family | | Yes | |
| Preventive factors |
| Optimal endogenous fluoride exposure (water, fluoride tablets/drops) | | | Yes |
| Daily usage of fluoride toothpaste | | | Yes |
| Professional local fluoride application | | | Yes |
| Regular dental appointments/ home prevention | | | Yes |
| Dental check-up |
| DMFT > 1 | Yes | | |
| Active white stains or enamel defects | Yes | | |
| High level of Streptococcus mutans | Yes | | |
| Present (bacterial) plaque | | Yes | |
Tab. 2. Caries risk assessment in children ≥ 6 years of age to be used by professional dental practitioners (24)
| Factors | High risk | Moderate risk | Low risk |
| Biological factors |
| Low socioeconomic status | Yes | | |
| Intake of more than 3 sugar-containing snacks or sweet drinks between meals daily | Yes | | |
| Need for specialist medical care | | Yes | |
| Immigrant family origin | | Yes | |
| Preventive factors |
| Drinking water with optimal fluoride content | | | Yes |
| Daily tooth brushing with fluoride toothpaste | | | Yes |
| Professional local fluoride application | | | Yes |
| Using xylitol, MI toothpaste (Tooth Mousse), antibacterial products at home | | | Yes |
| regular dental appointments/home prevention | | | Yes |
| Dental check-up |
| ≥ 1 carious lesion on the interproximal surface | Yes | | |
| Active white stains or enamel defects | Yes | | |
| Low salivary flow | Yes | | |
| Fillings with secondary caries | | Yes | |
| Braces or movable prosthetic appliances | | Yes | |
Tab. 3. Caries risk assessment in children younger than 3 years of age by non-dental medical professionals according to the CRA system (Caries Risk Assessment Test by AAPD) (24)
| Factors | High risk | Low risk |
| Biological factors |
| Active caries in the mother/guardian | Yes | |
| Low socioeconomic status of parents/guardians | Yes | |
| Child consumes more than 3 sugar-containing snacks or sweet drinks between meals daily | Yes | |
| Child falls asleep with a bottle containing natural or added sugar (other than water) | Yes | |
| Child requires specialist paediatric care | Yes | |
| Child comes from immigrant family | Yes | |
| Preventive factors |
| Endogenous fluoride prevention (tablet, drops) or fluoridated water | | Yes |
| Daily usage of fluoride toothpaste | | Yes |
| Professional topical fluoride application | | Yes |
| Regular dental appointments/preventive care at home | | Yes |
| Clinical manifestations |
| Active white stains or enamel defects | Yes | |
| Presence of caries or fillings | Yes | |
| Child has bacterial plaque | Yes | |
CRA is easily applicable in the clinical practice and enables not only caries risk evaluation (low, moderate or high), but also makes patients and their guardians aware of the causes of dental caries and facilitates medical recommendations and selection of appropriate dental preventive measures.
The cariostatic mechanisms of fluoride
There is ample evidence suggesting that using fluoride compounds is effective for caries prevention and non-invasive treatment of incipient caries.
Endogenous oral administration of an optimal fluoride dose during tooth development increases fluoride content in the surface enamel layer enabling a stable apatite crystalline network to be formed. Fluoride has an impact on primary mineralisation of organic matter and pre-eruptive enamel maturation. It catalyses a reaction that produces hydroxyapatite, Ca10(PO4)6(OH)2. By replacing hydroxyl ions (OH-), it forms fluoridated hydroxyapatite, Ca5(PO4)3OH1-xFx. It is conductive to the formation of larger apatite crystals with lower carbonate content. In pre-eruptive enamel maturation, fluoride participates in water and protein removal (25).
Until recently, it was believed that lower susceptibility of enamel to acids is an effect of pre-eruptive fluoride action. Currently, it is known, however, that the fluoride content of enamel does not permanently reduce the risk of caries in a significant way, and its excessive delivery can result in dental fluorosis (26-28). It is therefore important to deliver slight amounts of fluoride to the oral cavity systematically after tooth eruption (mainly by means of fluoride toothpaste) due to its exogenous, topical action. Figure 1 presents what happens with fluorides delivered to the oral cavity.
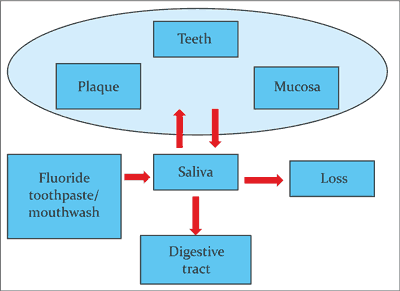
Fig. 1. Fluoride ions after topical application. The surface of the oral mucosa is a particularly important reservoir of fluoride ions; it is a storage of slowly released fluorides (according to ten Cate modification) (29, 30)
The anticaries action of fluoride after tooth eruption consists in:
a) limiting the influence of cariogenic bacteria by:
– decreasing acid production,
– reducing plaque deposition on tooth surfaces,
– inhibiting carbohydrate metabolic changes in bacterial cells (among others by lowering enolase activity and impairing glucose transport into cells),
b) inhibiting demineralisation and supporting remineralisation by:
– constant presence of low fluoride ion concentrations (< 50 ppm) enabling the reposition of mineral compounds lost during repeatable acid attacks with the formation of less susceptible crystals with fluorapatite-like coating (formation of fluoridated hydroxyapatite) (fig. 2),
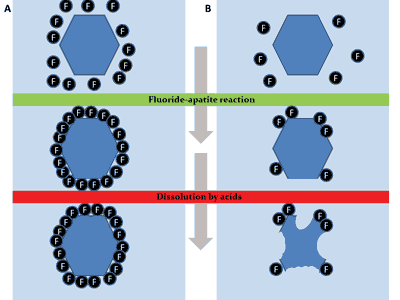
Fig. 2. Fluoride ions adsorbed on the surface of enamel crystals. A – presence of a sufficient quantity of fluoride ions prevents crystal dissolution during acid attack. B – insufficient quantity of fluoride ions on the surface of enamel crystals – partial crystal dissolution (according to ten Cate modification) (29, 33, 34)
– delivery of higher concentrations of fluoride ions (> 100 ppm) additionally ensures calcium fluoride (CaF2) formation which is a reservoir of fluoride ions released during bacterial acid attacks on dental enamel (25, 31, 32).
Safety of fluoride usage in children
Using fluoride requires care and reason since it is highly cytotoxic and the difference between its toxic and therapeutic doses is slight. Neglecting the principles of caries prevention is a risk factor for acute and chronic poisoning. In the WHO report from 1994, the role of fluoride exposure monitoring is underlined. This monitoring consists in balancing the severity of dental caries in children at risk of dental fluorosis resulting from the accumulation of fluoride from various sources (3). FDI recommends the establishment of health policies individually for a given country and advices to monitor the efficacy of caries prevention (1, 2).
Not only does the risk of dental fluorosis depend on fluoride exposure, but also on fluoride sensitivity of individual persons in a given population. That is why mild fluorosis can be observed also in areas where its content in drinking water is within an optimal range, i.e. 0.5-1.0 mg/l (3).
The elucidation of fluorosis is searched for in the accumulation of fluoride doses from various sources (e.g. bottled water, tea, fish products, imported food produced in areas with fluoridated water). Excessive fluoride exposure in a so-called critical developmental period, i.e. from 15 to 30 months of age, can cause fluorosis of permanent anterior teeth and first molars, whereas in the later age (6 years old) – of the remaining teeth. The causes of excessive fluoride delivery and consequent fluorosis can lie in:
– the preparation of infant formula based on water that contains too high fluoride concentrations (fluoride content in bottled water in Poland ranges from 0.1 to 1.39 mg F/L) (35),
– improper fluoride supplementation (other dietary components should be taken into account when implementing this type of prevention) (36, 37),
Powyżej zamieściliśmy fragment artykułu, do którego możesz uzyskać pełny dostęp.
Mam kod dostępu
- Aby uzyskać płatny dostęp do pełnej treści powyższego artykułu albo wszystkich artykułów (w zależności od wybranej opcji), należy wprowadzić kod.
- Wprowadzając kod, akceptują Państwo treść Regulaminu oraz potwierdzają zapoznanie się z nim.
- Aby kupić kod proszę skorzystać z jednej z poniższych opcji.
Opcja #1
29 zł
Wybieram
- dostęp do tego artykułu
- dostęp na 7 dni
uzyskany kod musi być wprowadzony na stronie artykułu, do którego został wykupiony
Opcja #2
69 zł
Wybieram
- dostęp do tego i pozostałych ponad 7000 artykułów
- dostęp na 30 dni
- najpopularniejsza opcja
Opcja #3
129 zł
Wybieram
- dostęp do tego i pozostałych ponad 7000 artykułów
- dostęp na 90 dni
- oszczędzasz 78 zł
Piśmiennictwo
1. FDI Policy Statement Stanowisko PTS: Poprawa zdrowia zębów poprzez fluoryzację. J Stoma 2011; 64(10): 808-809. 2. FDI Policy Statement Stanowisko PTS: Poprawa zdrowia zębów poprzez fluoryzację wody. J Stoma 2011; 64(10): 810-811. 3. Fluorides and Oral Health. Report of a WHO Expert Committee on Oral Health Status and Fluoride Use. WHO Technical Report Series No. 846. Geneva 1994; 37: 1-19. 4. Kaczmarek U, Majewska L, Olczak-Kowalczyk D: Postawa i wiedza stomatologów w zakresie profilaktyki fluorkowej. Nowa Stomatol 2015; 20(1): 23-28. 5. Adamowicz-Klepalska B, Borysewicz-Lewicka M, Dobrzańska A et al.: Aktualny stan wiedzy na temat indywidualnej profilaktyki fluorkowej choroby próchnicowej u dzieci i młodzieży. Niezależny Panel Ekspertów. J Stoma 2013; 66(4): 428-453. 6. Jańczuk Z: Stan narządu żucia polskiej populacji. Pomorska Akademia Medyczna, Szczecin 1990. 7. Szatko F, Boczkowski A: Skuteczność opieki stomatologicznej w Polsce. Fakty, oceny, perspektywy. Instytut Medycyny Pracy, Łódź 1995. 8. Oral health surveys: basic methods. 4th ed. World Health Organization, Geneva 1997. 9. Wierzbicka M, Szatko F, Michalski A et al.: Adaptacja i wdrożenie systemu monitorowania stanu zdrowia jamy ustnej. Ministerstwo Zdrowia, Warszawa 1997. 10. Wierzbicka M, Szatko F, Zawadziński M et al.: Ogólnokrajowy monitoring zdrowia jamy ustnej i jego uwarunkowań. Polska 2002. Ministerstwo Zdrowia, Zakład Stomatologii Zachowawczej AM w Warszawie, Katedra Higieny i Epidemiologii AM w Łodzi 2002. 11. Jodkowska E, Wierzbicka M, Szatko F et al.: Monitoring Zdrowia Jamy Ustnej. Polska 2009. Stan zdrowia jamy ustnej i jego uwarunkowania oraz potrzeby profilaktyczno-lecznicze dzieci i osób dorosłych w wieku 65-74 lata. Warszawa 2009. 12. Wierzbicka M, Szatko F, Strużycka I et al.: Monitoring Zdrowia Jamy Ustnej. Stan zdrowia jamy ustnej i jego uwarunkowania oraz potrzeby profilaktyczno-lecznicze dzieci w wieku 5, 7 i 15 lat. Polska 2010. Warszawa 2011. 13. Małkiewicz E, Wierzbicka M, Szatko F et al.: Monitoring Zdrowia Jamy Ustnej. Stan zdrowia jamy ustnej i jego uwarunkowania oraz potrzeby profilaktyczno-lecznicze dzieci w wieku 6 i 12 lat oraz osób dorosłych w wieku 35-44 lat. Polska 2010. Warszawa 2010. 14. Jodkowska E, Wierzbicka M, Szatko F et al.: Monitoring Zdrowia Jamy Ustnej. Stan zdrowia jamy ustnej dzieci i młodzieży. Polska 2008. Warszawa 2008. 15. FDI: Global goals for oral health in the year 2000. Int Dent J 1982; 32: 74-77. 16. Hobdell M, Petersen PE, Clarkson J, Johnson N: Global goals for oral health 2020. Int Dent J 2003; 53: 285-286. 17. Global caries data for 12-year-old age group WHO Oral Health Country/Area Profile Programme. http://www.mah.se/CAPP/Country-Oral-HealthProfiles/According-to-Alphabetical/Global-DMFTfor-12-year-olds-2011. 18. Wierzbicka M, Szatko F, Radziejewska M et al.: Ogólnokrajowy monitoring zdrowia jamy ustnej i jego uwarunkowań. Polska 2000. Ministerstwo Zdrowia, Zakład Stomatologii Zachowawczej AM w Warszawie, Katedra Higieny i Epidemiologii AM w Łodzi 2000. 19. Jadach R, Siwek-Jadach K, Migas-Mastalerz A: Rola lekarza rodzinnego w prewencji próchnicy zębów u dzieci i młodzieży. Family Medicine and Primary Care Review 2007; 9(3): 442-444. 20. Janus S, Olczak-Kowalczyk D, Wysocka M: Rola lekarzy niestomatologów w zapobieganiu próchnicy wczesnego dzieciństwa. Nowa Pediatria 2011; 1: 6-14. 21. Featherstone JD: The caries balance: The basis for caries management by risk assessment. Oral Health Prev Dent 2004; 2 (suppl. 1): 259-264. 22. Featherstone JD, Adair SM, Anderson MH et al.: Caries management by risk assessment: Consensus statement, April 2002. J Calif Dent Assoc 2003; 31(3): 257-269. 23. Featherstone JDB, Domejean-Orliaguet S, Jenson L et al.: Caries risk assessment in 16 practice for age 6 through adult. J Calif Dent Assoc 2007; 35(10): 703-712. 24. Guideline on Caries-risk Assessment and Management for Infants, Children, and Adolescents. The American Academy of Pediatric Dentistry, 2014; http://www.aapd.org/media/policies_guidelines/g_cariesriskassessment.pdf. 25. Kaczmarek U: Mechanizmy kariostatyczne fluoru. Czas Stomatol 2005; 6: 404-413. 26. Szczepańska J: Wpływ różnych aspektów higieny jamy ustnej na występowanie próchnicy u dzieci w okresie poniemowlęcym. Nowa Stomatol 2003; 1: 4-9. 27. D’Hoore W, Van Nieuwenhuysen JP: Benefits and risks of fluoride supplementation: caries prevention versus dental fluorosis. Eur J Pediatr 1992; 152: 613-617. 28. Dąbrowska E, Balunowska M, Letko E: Zagrożenia wynikające z nadmiernej podaży fluoru. Nowa Stomat 2001; 4(18): 22-27. 29. ten Cate JM: Contemporary perspective on the use of fluoride products in caries prevention. British Dental Journal 2013; 214: 161-167. 30. Duckworth RM, Morgan SN: Oral fluoride retention after use of fluoride dentifrices. Caries Res 1991; 25: 123-129. 31. ten Cate JM, Larsen MJ, Pearce EIF, Fejerskov O: Chemical interactions between the tooth and oral fluids. [In:] Fejerskov O, Kidd EAM (eds.): Dental caries. The disease and its clinical management. Black-well Munksgaard 2003: 49-70. 32. Ogaard B: CaF2 formation: cariostatic properties and factors of enhancing the effect. Caries Res 2001; 35 (suppl. 1): 40-44. 33. Arends J, Christoffersen J: Nature and role of loosely bound fluoride in dental caries. J Dent Res 1990; 69: 601-605. 34. Buzalaf MA, Pessan JP, Honório HM, ten Cate JM: Mechanisms of action of fluoride for caries control. Monogr Oral Sci 2011; 22: 97-114. 35. Borysewicz-Lewicka M, Chłapowska J, Wagner L, Trykowski J: Ocena zawartości fluorków w niektórych krajowych wodach mineralnych. Czas Stom 1999; 52(1): 29-32. 36. Opydo-Szymaczek J: Znaczenie oceny ekspozycji na fluorki w profilaktyce stomatologicznej. Stomat Współ 2003; 5(10): 44-48. 37. Opydo-Szymaczek J: Fluoride Exposure from Diet in Infants and Young Children Fed with the Foodstuffs for Particular Nutritional Uses. Dent Med Probl 2012; 49(2): 209-215. 38. Borysewicz-Lewicka M, Opydo-Szymaczek J, Opydo J: Fluoride ingestion after brushing with a gel containing a high concentration of fluoride. Biol Trace Elem Res 2007; 120(1-3): 114-120. 39. Lis J, Pasieczna A: Atlas geochemiczny Polski. Państwowe Wydawnictwo Kartograficzne, Warszawa 1995. 40. Czarnowski W, Wrześniowska K, Krechniak K: Fluoride in drinking water and human urine in Northern and Central Poland. Sci Total Environ 1996; 191(1-2): 177-184. 41. Erdal S, Buchanan SN: A quantitative look at fluorosis, fluoride exposure, and intake in children using a health risk assessment approach. Environ Health Perspect 2005; 113: 111-117. 42. Bergmann R: Fluorid in der Ernährung des Menschen. Biologische Bedeutung für denwachsenden Organismus. Habilitationsschrift Medical Faculty, Free University Berlin 1994. 43. Guidelines on the use of fluoride in children: an EAPD policy document. Eur Arch Paediatr Dent 2009; 10(3): 129-135. 44. Guideline on Fluoride Therapy. AAPD, 2014, http://www.aapd.org/media/policies_guidelines/g_fluoride therapy.pdf. 45. Policy on Early Childhood Caries (ECC): Classifications, Consequences, and Preventive Strategies. 2014, http://www.aapd.org/media/policies_guidelines/p_eccclassifications.pdf. 46. Weyant RJ, Tracy SL, Anselmo TT et al.: American Dental Association Council on Scientific Affairs Expert Panel on Topical Fluoride Caries Preventive Agents: Topical fluoride for caries prevention: executive summary of the updated clinical recommendations and supporting systematic review. J Am Dent Assoc 2013; 144(11): 1279-1291. 47. Rozier RG, Adair S, Graham F et al.: Evidence-Based Clinical Recommendations on the Prescription of Dietary Fluoride Supplements for Caries Prevention. A report of the American Dental Association Council on Scientific Affairs. JADA 2010; 141(12): 1480-1489. 48. American Dental Association Council on Scientific Affairs. Fluoride toothpaste use for young children. J Am Dent Assoc 2014; 145(2): 190-191. 49. Dietary Reference intakes for Calcium, Phosphorus, Magnesium, Vitamin D, and Fluoride. Standing Committee on the Scientific Evaluation of Dietary Reference Intakes Food and Nutrition Board Institute of Medicine. National Academy Press, Washington, D.C. 1997; 288-313. 50. Opinion of the Scientific Panel on Dietetic Products, Nutrition and Allergies on a request from the Commission related to the Tolerable Upper Intake Level of Fluoride. The EFSA Journal 2005; 192: 1-65. 51. Opydo-Szymaczek J, Opydo J: Salivary fluoride concentrations and fluoride ingestion following application of preparations containing high concentration of fluoride. Biol Trace Elem Res 2010; 137(2): 159-167. 52. Beltran-Aguilar ED, Barker LK, Canto MT et al.: Surveillance for dental caries, dental sealants, tooth retention, edentulism, and enamel fluorosis: United States, 1988-1994 and 1999-2002. MMWR Surveill Summ 2005; 54: 1-43. 53. Iida H, Kumar JV: The association between enamel fluorosis and dental caries in U.S. schoolchildren. JADA 2009; 140: 855-862. 54. European Commision. Directorate-Deneral for Health & Consumers. Scientific Committee on Health and Environmental Risks SCHER: Critical review of any new evidence on the hazard profile, health effects, and human exposure to fluoride and the fluoridating agents of drinking water. SCHER 16.05.2011. 55. Tubert?Jeannin S, Auclair C, Amsallem E et al.: Fluoride supplements (tablets, drops, lozenges or chewing gums) for preventing dental caries in children. Cochrane Database Syst Rev 2011; 7(12): CD007592. doi: 10.1002/14651858.CD007592.pub2. 56. Steinbacher DM, Glick M: The dental patient with asthma. An update and oral health considerations. JADA 2001; 132: 1229-1239. 57. Guide to children’s dental care in medicaid. 2004; http://www.aapd.org/assets/1/7/Periodicity-DentalGuide.pdf. 58. Pitts N, Duckworth RM, Marsh P et al.: Post-brushing rinsing for the control of dental caries: exploration of the available evidence to establish what advice we should give our patients. Br Dent J 2012; 212(7): 315-320. 59. Korporowicz E, Rożniatowski P, Sobiech P, Kochman K: Rodzaj i ilość past do zębów używanych przez rodziców u dzieci w wieku od 1 do 7 lat. Nowa Stomatol 2014; 3: 124-126. 60. Walsh T, Worthington HV, Glenny AM et al.: Fluoride toothpastes of different concentrations for preventing dental caries in children and adolescents. Cochrane Database Syst Rev 2010; 20(1): CD007868. doi: 10.1002/14651858.CD007868.pub2. 61. Wong MCM, Glenny A?M, Tsang BWK et al.: Topical fluoride as a cause of dental fluorosis in children. Cochrane Database Syst Rev 2010 Jan 20; 1: CD007693. doi: 10.1002/14651858.CD007693.pub2. 62. Lewis CL: Fluoride and Dental Caries Prevention in Children. Pediatrics in Review 2014; 35: 3. doi: 10.1542/pir.35-1-3. 63. Al-Mulla A, Karlsson L, Kharsa S et al.: Combination of high-fluoride toothpaste and no post-brushing water rinsing on enamel demineralization using an in situ caries model with orthodontic bands. Acta Odontol Scand 2010; 68(6): 323-328. 64. Nordström A, Birkhed D: Preventive effect of a high-fluoride dentifrice (5,000 ppm) in caries-active adolescents – a 2-year clinical trial. Caries Res 2010; 44: 323-333. 65. Alexander SA, Ripa LW: Effects of self-applied topical fluoride preparations in orthodontic patients. Angle Orthod 2000; 70: 424-430. 66. O’Reilly MM, Featherstone JD: Demineralization and remineralization around orthodontic appliances: an in vivo study. Am J Orthod Dentofacial Orthop 1987; 92: 33-40. 67. Marinho VC, Higgins JP, Logan S, Sheiham A: Fluoride mouthrinses for preventing dental caries in children and adolescents. Cochrane Database Syst Rev 2003; 3: CD002284. 68. Sköld UM, Birkhed D, Borg E, Petersson, LG: Approximal caries development in adolescents with low to moderate caries risk after different 3-year school-based supervised fluoride mouth rinsing programmes. Caries Res 2005; 39: 529-535. 69. Twetman S, Petersson L, Axelsson S et al.: Caries preventive effect of sodium fluoride mouthrinses: a systematic review of controlled clinical trials. Acta Odontol Scand 2004; 62: 223-230. 70. Adair SM: Evidence-based Use of Fluoride in Contemporary Pediatric Dental Practice. Pediatr Dent 2006; 28: 133-142. 71. Zero DT, Fu J, Espeland MA, Featherstone JD: Comparison of fluoride concentrations in unstimulated whole saliva following the use of a fluoride dentifrice and a fluoride rinse. J Dent Res 1988; 67: 1257-1262. 72. Duckworth RM, Horay C, Huntington E, Mehta V: Effects of flossing and rinsing with a fluoridated mouthwash after brushing with a fluoridated toothpaste on salivary fluoride clearance. Caries Res 2009; 43: 387-390. 73. Driscoll WS, Swango PA, Horowitz AM, Kingman A: Caries-preventive effects of daily and weekly fluoride mouthrinsing in a fluoridated community: final results after 30 months. J Am Dent Assoc 1982; 105: 1010-1013. 74. Heifetz SB, Meyers RJ, Kingman A: Comparison of the anticaries effectiveness of daily and weekly rinsing with sodium fluoride solutions: findings after three years. Pediatr Dent 1983; 4: 300-303. 75. Marinho VCC, Higgins J, Logan S, Sheiham A: Fluoride gels for preventing dental caries in children and adolescents. Cochrane Db Syst Rev 2002; 2. DOI: 10.1002/14651858.CDO002280. 76. Marinho VCC, Worthington HV, Walsh T, Chong LY: Fluoride gels for preventing dental caries in children and adolescents. Cochrane Clinical Answers, 2015; http://cochraneclinicalanswers.com/doi/10.1002/cca.876/full. 77. Ekstrand J, Koch G, Petersson LG: Plasma fluoride concentration and urinary fluoride excretion in children following application of the fluoride-containing varnish Duraphat. Caries Res 1980; 14(4): 185-189. 78. Ekstrand J, Koch G, Lindgren LE, Petersson LG: Pharmacokinetics of fluoride gels in children and adults. Caries Res 1981; 15(3): 213-220. 79. Whitford GM: The metabolism and toxicity of fluoride. Monogr Oral Sci 1989; 13: 1-160. 80. Pendrys DG, Haugejorden O, Bårdsen A et al.: The risk of enamel fluorosis and caries among Norwegian children: implications for Norway and the United States. J Am Dent Assoc 2010; 141(4): 401-414. 81. Browne D, Whelton H, O’Mullane D: Fluoride metabolism and fluorosis. J Dent 2005 Mar; 33(3): 177-186. 82. Holve S: An observational study of the association of fluoride varnish applied during well child visits and the prevention of early childhood caries in American Indian children. Matern Child Health J 2008; 12 (suppl. 1): 64-67.


