Lukasz Szarpak1, 2, *Agnieszka Madziala1, Marek Dabrowski4, Halla Kaminska5, Wojciech Wieczorek6, Jacek Smereka7, Klaudiusz Nadolny2, Jerzy Robert Ladny2, Robert Galazkowski3, 8
Impact of chest compression on endotracheal intubation efficacy: a randomized crossover trial
Wpływ uciskania klatki piersiowej na efektywność intubacji dotchawiczej: badanie randomizowane krzyżowe
1Department of Emergency Medicine, Medical University of Warsaw, Poland
2Department of Emergency Medicine and Disaster, Medical University of Bialystok, Poland
3Polish Medical Air Rescue, Warsaw, Poland
4Department of Medical Rescue, Poznan University of Medical Sciences, Poland
5Department of Children’s Diabetology, Medical University of Silesia in Katowice, Poland
6Department of Anaesthesiology, Intensive Care and Emergency Medicine in Zabrze,
Medical University of Silesia in Katowice, Poland
7Department of Emergency Medical Service, Wroclaw Medical University, Poland
8Department of Emergency Medical Service, Medical University of Warsaw, Poland
Streszczenie
Wstęp. Laryngoskopia bezpośrednia z zastosowaniem standardowego laryngoskopu z łopatkami Millera bądź Macintosha może stanowić trudność w przypadku resuscytacji krążeniowo-oddechowej. Dobre uwidocznienie głośni może wpływać na skuteczność intubacji dotchawiczej.
Cel pracy. Celem badania było porównanie efektywności intubacji dotchawiczej wykonywanej przez studentów medycyny z zastosowaniem laryngoskopii bezpośredniej i wideolaryngoskopii podczas resuscytacji krążeniowo-oddechowej z uciskaniem i bez uciskania klatki piersiowej.
Materiał i metody. Badanie było badaniem randomizowanym, krzyżowym. Pięćdziesięciu siedmiu studentów ostatniego roku studiów medycznych, którzy mieli ograniczone doświadczenie w zakresie laryngoskopii bezpośredniej oraz brak doświadczenia w zakresie wideolaryngoskopii, uczestniczyło w badaniu. Intubacja dotchawicza była wykonywana z zastosowaniem wideolaryngoskopu C-MAC oraz standardowego laryngoskopu z łopatką Macintosha (MAC) z uciskaniem i bez uciskania klatki piersiowej.
Wyniki. Mediana czasu intubacji dla MAC i C-MAC podczas scenariusza bez uciskania klatki piersiowej wynosiła odpowiednio 21 (IQR: 20-27) i 18 s (IQR: 16,5-24). Podczas scenariusza z nieprzerwalnym uciskaniem klatki piersiowej mediana czasu intubacji wynosiła odpowiednio 39 s (IQR: 24-47) dla MAC oraz 22,5 s (IQR: 17-25) dla C-MAC. Skuteczność pierwszej próby intubacji w warunkach bez uciskania i z uciskaniem klatki piersiowej z wykorzystaniem MAC wynosiła odpowiedni 54,3 oraz 28,1%. W przypadku zastosowania C-MAC otrzymano skuteczność pierwszej próby intubacji na poziomie 100% dla scenariusza bez uciskania klatki piersiowej oraz 96,5% dla scenariusza z ciągłym uciskaniem klatki piersiowej.
Wnioski. Uciski klatki piersiowej wpływają na wydłużenie czasu procedury intubacji oraz skuteczność intubacji w przypadku wykorzystania laryngoskopii bezpośredniej. Wideolaryngoskop C-MAC może być wykorzystywany przez niedoświadczony w intubacji personel medyczny bez konieczności wykonywania przerw w uciskaniu klatki piersiowej na czas trwania intubacji. Dalsze badania są konieczne celem potwierdzenia uzyskanych wyników.
Summary
Introduction. Direct endotracheal intubation with a conventional laryngoscope such as Miller or Macintosh laryngoscopes may be problematic during cardiopulmonary resuscitation. A degree of the glottis visualization may affect the effectiveness of intubation.
Aim. Aim of this study was to compare intubation efficacy using direct and video-laryngoscopes during resuscitation with and without chest compression performed by medical students.
Material and methods. This was a randomized crossover trial. Fifty-seven last year medical students who have limited experience in direct laryngoscopy and none prior experience in videolaryngoscopy participated in this trial. The endotracheal intubation using C-MAC videolaryngoscope and standard Macintosh laryngoscope with and without chest compressions were compared.
Results. The median time of the MAC and C-MAC devices in the scenario without chest compressions were 21 (IQR: 20-27) vs. 18 sec (IQR: 16.5-24) respectively. During scenario with uninterrupted chest compressions, median intubation time using distinct devices varied and amounted to 39 (IQR: 24-47) vs. 22.5 sec (IQR: 17-25). The efficacy rate of first intubation attempt with MAC was 54.3% without chest compressions and 28.1% during chest compression conditions. For C-MAC the first intubation success rate was 100% for scenario without chest compressions and 96.5% for scenario with uninterrupted chest compressions.
Conclusions. Within limitations, we conclude that performing chest compressions during direct laryngoscopy prolongs the procedure and lowers the efficacy rate. C-MAC videolaryngoscope can be used by inexperienced intubators without interruptions in chest compressions. Additional studies are required to validate those results.

INTRODuCTION
Endotracheal intubation is commonly considered a life-saving procedure, especially in the emergency medicine (1, 2). Cardiopulmonary resuscitation is an example of one of many procedures where endotracheal intubation is considered the gold standard for maintaining the airway patency (3). Current American Heart Association guidelines recommend that the maintaining of the airway patency, endotracheal intubation included, should be performed with uninterrupted chest compressions (4). Performing the procedure in this way allows for minimizing the pauses during chest compressions and enables for the blood flow through the vital organs. The Resuscitation Guidelines recommend that the intubation should be performed with simultaneous chest compressions, preferably without a pause or with a short one to allow the insertion of the endotracheal tube between the vocal folds.
Performing the procedure with such prerequisites requires a lot of skill and experience from the person who performs it (5-7). What is worth noting is also that the efficacy of endotracheal intubation in anti-vital conditions is insufficient (8, 9). Additionally, intubation during chest compressions may result in an extended duration of the procedure when using direct laryngoscopy (10-12). The potential consequences to the patient of a failed endotracheal intubation are death or serious complications (13, 14).
We hypothesize that videolaryngoscope C-MAC reduce time of endotracheal intubation and increases intubation success rate compared to standard laryngoscope with Macintosh blade, when intubation is performed during cardiopulmonary resuscitation with uninterrupted chest compressions performed by inexperienced intubators.
AIM
The purpose of this study was to compare the endotracheal intubation using Macintosh laryngoscope and C-MAC videolaryngoscope with and without chest compressions by last year medical students in simulation setting.
MATERIAL AND METHODS
This is prospective, randomized, crossover, observational simulation study. After obtaining Institutional Review Board (Polish Society of Disaster Medicine; Approval number: 74.11.2017.IRB) approval and voluntary written informed consent, 57 last year medical students participated with this trial. All participants of the study had previously completed the anesthesiology and emergency medicine training modules and declared the ability to perform endotracheal intubation utilizing direct laryngoscopy. All participants watched a video demonstrating the correct intubation procedure with both the C-MAC videolaryngoscope and standard laryngoscope with Macintosh blade (fig. 1a, b), and instructor was giving verbal instructions regarding the correct use of each device. Subsequently, the correct use of both endotracheal intubation methods was demonstrated.
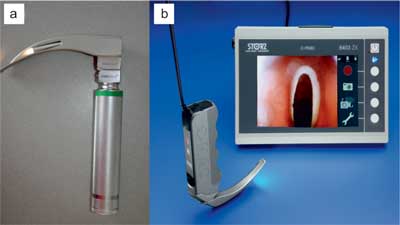
Fig. 1a, b. Laryngoscopes used in this trial: (a) Macintosh laryngoscope; (b) C-MAC laryngoscope
In order to demonstrate both the correct performance of intubation and for training Laerdal Airway Management Trainer (Laerdal, Stavanger, Norway) was used. After theoretical part, each of the participants of the study had a maximum of 5 minutes to get acquainted with individual laryngoscopes and to perform training endotracheal intubation in normal airway conditions.
During the target study, the participants were asked to perform endotracheal intubation using the C-MAC and Macintosh laryngoscope during cardiopulmonary resuscitation. In order to assess the influence of chest compressions on the effectiveness of endotracheal intubation, participants performed intubation in two scenarios:
1. Scenario A – normal airways without chest compressions.
2. Scenario B – normal airways with constant chest compressions. In order to simulate the difficulties resulting from constant chest compressions, the LUCAS 3 system (Physio-Control, Lund, Sweden) was used.
The study participants were divided into four groups, the first of which performed endotracheal intubation utilizing C-MAC during scenario A, the second one used C-MAC during scenario B, the third one used MAC during scenario A, and the fourth one performed intubation using MAC during scenario B. A detailed randomization procedure for the study is presented on figure 2. All intubations were performed using a cuffed endotracheal tube with an internal diameter of 7.5 mm, and all intubations were facilitated with a malleable IVORY stylet (Smiths Medical; Minneapolis, MN, USA). The tip of the stylet was bent individually by participants.
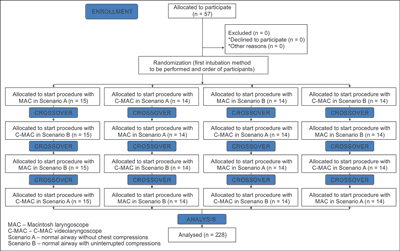
Fig. 2. Randomization flow chart
The primary aim of this trial was the comparison of intubation times using direct and video-laryngoscopes during resuscitation with and without chest compression. Intubation time was defined as the time since laryngoscope entered the oral cavity until the first chest inflation using a self-inflating bag was performed. Intubation failure was defined as follows: intubation time longer than 60 seconds (10, 15), the insertion of the endotracheal tube into the esophagus of the manikin as well as removal of the endotracheal tube from the manikin’s mouth before successful intubation. Secondary outcomes were: success rate of the first successful intubation attempt, overall intubation success rate, the best glottis view, and ease of intubation. The grading of the glottic view was based on the Cormack-Lehane system (16). To assess the subjective opinion about the easiness of using the intubation methods, participants were asked to rate the distinct device with a score from 1 (extremely easy) to 10 (extremely difficult).
Powyżej zamieściliśmy fragment artykułu, do którego możesz uzyskać pełny dostęp.
Mam kod dostępu
- Aby uzyskać płatny dostęp do pełnej treści powyższego artykułu albo wszystkich artykułów (w zależności od wybranej opcji), należy wprowadzić kod.
- Wprowadzając kod, akceptują Państwo treść Regulaminu oraz potwierdzają zapoznanie się z nim.
- Aby kupić kod proszę skorzystać z jednej z poniższych opcji.
Opcja #1
29 zł
Wybieram
- dostęp do tego artykułu
- dostęp na 7 dni
uzyskany kod musi być wprowadzony na stronie artykułu, do którego został wykupiony
Opcja #2
69 zł
Wybieram
- dostęp do tego i pozostałych ponad 7000 artykułów
- dostęp na 30 dni
- najpopularniejsza opcja
Opcja #3
129 zł
Wybieram
- dostęp do tego i pozostałych ponad 7000 artykułów
- dostęp na 90 dni
- oszczędzasz 78 zł
Piśmiennictwo
1. Chou HC, Tseng WP, Wang CH et al.: Tracheal rapid ultrasound exam (T.R.U.E.) for confirming endotracheal tube placement during emergency intubation. Resuscitation 2011; 82(10): 1279-1284.
2. Smereka J, Czyzewski L, Szarpak L, Ladny JR: Comparison between the TrueView EVO2 PCD and direct laryngoscopy for endotracheal intubation performed by paramedics: Preliminary data. Am J Emerg Med 2017; 35(5): 789-790.
3. Truszewski Z, Szarpak L, Czyzewski L et al.: A comparison of the ETView VivaSight SL against a fiberoptic bronchoscope for nasotracheal intubation of multitrauma patients during resuscitation. A randomized, crossover, manikin study. Am J Emerg Med 2015; 33(8): 1097-1099.
4. Link MS, Berkow LC, Kudenchuk PJ et al.: Part 7: Adult Advanced Cardiovascular Life Support: 2015 American Heart Association Guidelines Update for Cardiopulmonary Resuscitation and Emergency Cardiovascular Care. Circulation 2015; 132(18 suppl. 2): S444-464.
5. Moon YJ, Kim J, Seo DW et al.: Endotracheal intubation by inexperienced trainees using the Clarus Video System: learning curve and orodental trauma perspectives. J Dent Anesth Pain Med 2015; 15(4): 207-212.
6. Sakles JC, Mosier J, Patanwala AE, Dicken J: Learning curves for direct laryngoscopy and GlideScope® video laryngoscopy in an emergency medicine residency. West J Emerg Med 2014; 15(7): 930-937.
7. Buis ML, Maissan IM, Hoeks SE et al.: Defining the learning curve for endotracheal intubation using direct laryngoscopy: A systematic review. Resuscitation 2016; 99: 63-71.
8. Ladny JR, Smereka J, Szarpak L: Comparison of the Trachway video intubating stylet and Macintosh laryngoscope for endotracheal intubation. Preliminary data. Am J Emerg Med 2017; 35(4): 574-575.
9. Caruana E, Duchateau FX, Cornaglia C et al.: Tracheal intubation related complications in the prehospital setting. Emerg Med J 2015; 32(11): 882-887.
10. Kurowski A, Szarpak L, Truszewski Z, Czyzewski L: Can the ETView VivaSight SL Rival Conventional Intubation Using the Macintosh Laryngoscope During Adult Resuscitation by Novice Physicians? A Randomized Crossover Manikin Study. Medicine (Baltimore) 2015; 94(21): e850.
11. Szarpak Ł, Czyżewski Ł, Truszewski Z et al.: Comparison of Coopdech®, CoPilot®, Intubrite®, and Macintosh laryngoscopes for tracheal intubation during pediatric cardiopulmonary resuscitation: a randomized, controlled crossover simulation trial. Eur J Pediatr 2015; 174(11): 1517-1523.
12. Szarpak L, Smereka J, Ladny JR: Comparison of Macintosh and Intubrite laryngoscopes for intubation performed by novice physicians in a difficult airway scenario. Am J Emerg Med 2017; 35(5): 796-797.
13. Martin LD, Mhyre JM, Shanks AM et al.: 3,423 emergency tracheal intubations at a university hospital: airway outcomes and complications. Anesthesiology 2011; 114(1): 42-48.
14. Simpson GD, Ross MJ, McKeown DW, Ray DC: Tracheal intubation in the critically ill: a multi-centre national study of practice and complications. Br J Anaesth 2012; 108(5): 792-799.
15. Kurowski A, Szarpak Ł, Zaśko P et al.: Comparison of direct intubation and Supraglottic Airway Laryngopharyngeal Tube (S.A.L.T.) for endotracheal intubation during cardiopulmonary resuscitation. Randomized manikin study. Anaesthesiol Intensive Ther 2015; 47(3): 195-199.
16. Cormack RS, Lehane J: Difficult tracheal intubation in obstetrics. Anaesthesia 1984; 39(11): 1105-1111.
17. Kim W, Choi HJ, Lim T, Kang BS: Can the new McGrath laryngoscope rival the GlideScope Ranger portable video laryngoscope? A randomized manikin study. Am J Emerg Med 2014; 32(10): 1225-1229.
18. Ray DC, Billington C, Kearns PK et al.: A comparison of McGrath and Macintosh laryngoscopes in novice users: a manikin study. Anaesthesia 2009; 64(11): 1207-1210.
19. Jeon WJ, Kim KH, Yeom JH et al.: A comparison of the Glidescope® to the McGrath® videolaryngoscope in patients. Korean J Anesthesiol 2011; 61(1): 19-23.
20. Brown CA 3rd, Bair AE, Pallin DJ, Walls RM; NEAR III Investigators: Techniques, success, and adverse events of emergency department adult intubations. Ann Emerg Med 2015; 65(4): 363-370.
21. Bossers SM, Schwarte LA, Loer SA et al.: Experience in Prehospital Endotracheal Intubation Significantly Influences Mortality of Patients with Severe Traumatic Brain Injury: A Systematic Review and Meta-Analysis. PLoS One 2015; 10(10): e0141034.
22. Arima T, Nagata O, Miura T et al.: Comparative analysis of airway scope and Macintosh laryngoscope for intubation primarily for cardiac arrest in prehospital setting. Am J Emerg Med 2014; 32(1): 40-43.
23. Schuerner P, Grande B, Piegeler T et al.: Hands-Off Time for Endotracheal Intubation during CPR Is Not Altered by the Use of the C-MAC Video-Laryngoscope Compared to Conventional Direct Laryngoscopy. A Randomized Crossover Manikin Study. PLoS One 2016; 11(5): e0155997.
24. Smereka J, Ladny JR, Naylor A et al.: C-MAC compared with direct laryngoscopy for intubation in patients with cervical spine immobilization: a manikin trial. Am J Emerg Med 2017; 35(8): 1142-1146.
25. Kaplan A, Göksu E, Yıldız G, Kılıç T: Comparison of the C-MAC Videolaryngoscope and Rigid Fiberscope with Direct Laryngoscopy in Easy and Difficult Airway Scenarios: A Manikin Study. J Emerg Med 2016; 50(3): e107-114.
26. Konrad C, Schüpfer G, Wietlisbach M, Gerber H: Learning manual skills in anesthesiology: Is there a recommended number of cases for anesthetic procedures? Anesth Analg 1998; 86(3): 635-639.
27. Nouruzi-Sedeh P, Schumann M, Groeben H: Laryngoscopy via Macintosh blade versus GlideScope: success rate and time for endotracheal intubation in untrained medical personnel. Anesthesiology 2009; 110(1): 32-37.
28. Ladny JR, Sierzantowicz R, Kedziora J, Szarpak L: Comparison of direct and optical laryngoscopy during simulated cardiopulmonary resuscitation. Am J Emerg Med 2017; 35(3): 518-519.
29. Gawlowski P, Smereka J, Madziala M et al.: Comparison of the Macintosh laryngoscope and blind intubation via the iGEL for intubation with C-spine immobilization: a randomized, crossover, manikin trial. Am J Emerg Med 2017; 35(3): 484-487.
30. Cho J, Chung HS, Chung SP et al.: Airway scope vs Macintosh laryngoscope during chest compressions on a fresh cadaver model. Am J Emerg Med 2010; 28(6): 741-744.


