*Natalia Fabisiak1, 2, Adam Fabisiak2, 3, Ewa Małecka-Panas3, Anita Gąsiorowska1
Acute pancreatitis – epidemiology, etiology, procedures and treatment: a retrospective cohort study
Ostre zapalenie trzustki – epidemiologia, etiologia, procedury medyczne i leczenie: retrospektywne badanie kohortowe
1Department of Gastroenterology, Medical University of Łódź
Head of Department: Professor Anita Gąsiorowska, MD, PhD
2Department of Biochemistry, Faculty of Medicine, Medical University of Łódź
Head of Department: Professor Jakub Fichna, MD, PhD
3Departament of Digestive Tract Diseases, Medical University of Łódź
Head of Department: Professor Ewa Małecka-Panas, MD, PhD
Streszczenie
Wstęp. Ostre zapalenie trzustki (OZT) jest procesem zapalnym trzustki spowodowanym najczęściej przez kamicę żółciową lub alkohol. Zachorowalność na OZT w zależności od głównego czynnika etiologicznego różni się w krajach Europy z przewagą OZT o etiologii alkoholowej w Europie Wschodniej.
Cel pracy. Celem badania była retrospektywna ocena etiologii OZT oraz określenie korelacji pomiędzy etiologią OZT a danymi demograficznymi, poziomem białka C-reaktywnego (CRP) i liczbą leukocytów (WBC) przy przyjęciu, długością trwania hospitalizacji oraz ciężkością i śmiertelnością OZT.
Materiał i metody. Poddano ocenie retrospektywnej historie choroby pacjentów hospitalizowanych od 1 września 2014 do 31 sierpnia 2016 roku w Klinice Chorób Przewodu Pokarmowego w Łodzi z powodu OZT. Dwie zmienne zostały porównane przy użyciu testu t-studenta z 95% przedziałem ufności. Trzy zmienne porównano przy pomocy testu ANOVA z testem Tuckeya jako analizą post-hoc. Korelację oceniono przy użyciu korelacji r-Pearsona z regresją liniową. Testu Chi2 używano, porównując grupy, a test dokładnego prawdopodobieństwa Fishera – w przypadku, gdy liczność grupy była mniejsza od 5. Wartość P mniejsza od 0,05 była uznawana za istotną statystycznie.
Wyniki. Spożycie alkoholu było głównym czynnikiem etiologicznym OZT i wystąpiło u 149 pacjentów (52,3%), kolejno przed przyczyną żółciową (27%), rakiem (2,5%), OZT wywołanym hipertriglicerydemią, jatrogennym OZT oraz OZT wywołanym lekami (po 0,7%). Dokładna przyczyna nie została wyjaśniona u 46 pacjentów (16,1%). Średnia wieku dla chorych z OZT o alkoholowej etiologii była istotnie statystycznie niższa niż u pacjentów z żółciopochodnym OZT (42,7 ± 0,98 vs 60,23 ± 1,95; p < 0,001). Spośród wszystkich pacjentów, kobiety były istotnie statystycznie starsze w porównaniu z mężczyznami (p < 0,001). OZT o etiologii alkoholowej występowało istotnie statystycznie częściej u mężczyzn niż kobiet (p < 0,001). Nie znaleziono związku między etiologią a ciężkością choroby (p = 0,61). Znaleziono istotną statystycznie korelację pomiędzy poziomem CRP przy przyjęciu a długością hospitalizacji (p < 0,001, r = 0,2433). Ponadto, poziom CRP przy przyjęciu był istotnie statystycznie wyższy u pacjentów z umiarkowaną i ciężką postacią choroby w porównaniu do łagodnej postaci OZT (odpowiednio: p < 0,01 oraz p < 0,001).
Wnioski. Wykazaliśmy, iż alkohol jest głównym czynnikiem etiologicznym OZT u pacjentów przyjętych na nasz Oddział i dotyczy głównie mężczyzn poniżej 65. roku życia. Kobiety powyżej 40. roku życia częściej przebyły żółciopochodne OZT. CRP może być uznany za marker klinicznej ciężkości choroby i może potencjalnie zostać wykorzystany do szybkiego przewidywania konieczności dłuższej hospitalizacji u pacjentów przy przyjęciu do szpitala.
Summary
Introduction. Acute pancreatitis (AP) is an inflammation of the pancreas which is the most frequently caused by cholelithiasis and alcohol abuse. The morbidity of AP in regard with certain etiological factor differs between the European countries with alcoholic AP to be most prevalent in Eastern Europe.
Aim. The aims of the study were to retrospectively assess the etiology of AP and to evaluate correlation between the etiology of AP and demographic data, CRP (C-reactive protein), WBC (white blood cells) count on admission, duration of hospitalization, severity and mortality of AP.
Material and methods. The history of patients hospitalized from September 1st 2014 to August 31st 2016 in the Department of Digestive Tract Diseases in Lodz, Poland due to acute pancreatitis of any etiology was retrospectively assessed. Two means were compared using Student’s t-test with 95% confidence interval. Three means were compared using ANOVA with Tukey’s test as a post-hoc test. Correlations were assessed using r-Pearson correlation with linear regression. Chi-square test was used when comparing groups or Fisher’s exact probability test when the sample size was lower than 5. P value less than 0.05 was considered.
Results. Alcoholic abuse was the major etiological factor of AP which occurred in 149 patients (52.3%), followed by: biliary (27%), cancer (2.5%), hypertriglyceridemia-induced, iatrogenic, drug-related (0.7% for all). The exact cause was not clarified in 46 patients (16.1%). Mean age of patients with alcoholic AP was significantly lower than patients with biliary AP (42.7 ± 0.98 vs 60.23 ± 1.95; p < 0.001). Among all patients, females were significantly older compared to males (p < 0.001). Alcoholic AP was significantly more common in males than females (p < 0.001). There was no relationship between etiology and severity of AP (p = 0.61). There was a statistically significant correlation between the CRP on admission and length of hospitalization (p < 0.001, r = 0.2433). Also, concentration of CRP on admission was significantly higher in patients with moderate and severe compared with mild disease (p < 0.01 and p < 0.001, respectively).
Conclusions. We demonstrated that alcohol is a major etiological factor of AP in patients admitted to our Department and affects mostly males below 65 years old. Female above 40 years old more frequently suffers from biliary AP. CRP can be regarded a marker of clinical severity and it could potentially be used to rapidly predict the necessity of longer hospitalization in these patients on admission.

Introduction
Acute pancreatitis (AP) is an inflammation of the pancreas characterized by an acute epigastric pain radiating to the back, a concomitant elevated activity of serum pancreatic enzymes (amylase and lipase) and/or characteristic abnormalities demonstrated on computed tomography (CT) scan, magnetic resonance imaging (MRI), or transabdominal ultrasonography (USG). Generally, two types of AP are observed: interstitial edematous pancreatitis and necrotizing pancreatitis. The revised Atlanta Classification of AP distinguished three grades of severity: (i) a mild form which is characterized by absence of organ failure and local or systemic complication; (ii) a moderate form in which transient (< 48 h) organ dysfunction and/or local or systemic complication occurs and (iii) a severe form characterized by a persistent organ failure (> 48 h) (1). In Poland incidence rate of AP is estimated on 72.1/100 000 patients per year and is one of the highest in European countries (2). A mild course of the disease is observed in 80.7% of patients. The incidence of severe AP is noted in roughly 7% of patients and has been increasing over the past years (2, 3). Noteworthy, cholelithiasis and alcohol abuse are two major etiological factors of AP (4-7). The third most common cause of AP is hypertriglyceridemia (8).
AP is associated with increased mortality rate reaching up to 60% in severe disease (2). Treatment of AP depends on severity of the disease. However, the therapeutic options are few with intensive hydration and pain reduction as a basic management. Antibiotic therapy is recommended only if concomitant extra-pancreatic infection or infected necrosis are present. To date, detailed data concerning epidemiology and etiology of acute pancreatitis in Poland are not known.
Aim
The aim of this study was to estimate the etiology of AP and to evaluate correlation between the etiology of AP and demographic data, C-reactive protein (CRP), white blood cells (WBC), duration of hospitalization, severity and mortality of AP in Department of Digestive Tract Diseases Norbert Barlicki Memorial Teaching Hospital No. 1 in Łódź.
Material and methods
The history of patients hospitalized over the period of 2 years, from September 1st 2014 to August 31st 2016 due to acute pancreatitis of any etiology was retrospectively assessed. Medical histories were collected by searching the hospital records with the database search of ICD-10 code &dsquo;K85” as a main diagnosis. Patients were re-evaluated towards AP prior to the inclusion based on Atlanta Recommendations defined as a presence of two of the three following criteria: (i) typical abdominal pain; (ii) activity of amylase and/or lipase increased above threefold of normal range; (iii) characteristic abnormalities in abdominal imaging. Necrotic pancreatitis was recognized when areas of necrosis, affecting the pancreas and/or peripancreatic tissues was observed in abdominal CT scan. Patient was excluded if the criteria were not fulfilled or the data was incomplete. Following items were collected whenever it was possible: sex, age, duration of hospitalization, day of the week of admission, etiology, level of CRP on admission, level of WBC on admission, imaging results, type (edematous or necrotic), severity, the need of antibiotics, the need of medical nutrition therapy, comorbidities, local and systemic complications, mortality. Alcoholic AP was defined when patients had a history of alcohol consumption within 48 h before symptom onset or patient had a history of alcohol abuse with no signs of other possible causes. Biliary pancreatitis was defined when there was a gallstone or biliary sludge on USG or CT. The etiology was considered to be idiopathic when causative factors could not be identified from a detailed clinical and drug history or after initial investigations. We relied on the Revised Atlanta Classification (1) and American College of Gastroenterology (ACG) Guidelines (9).
Statistical analysis
Statistical analysis was performed using software Statistica 12.5 (Statistica, Tulsa, Oklahoma) and GraphPad Prism 5.0 (GraphPad Software, Inc, La Jolla, CA). Two means were compared using Student’s t-test with 95% confidence interval. Three means were compared using ANOVA with Tukey’s test as a post-hoc test. Correlations were assessed using r-Pearson correlation with linear regression. Chi-square test was used when comparing groups or Fisher’s exact probability test when the sample size was lower than 5. Compared values were evaluated for outliers using Grubbs’ Test and excluded if found to be significant outliers. P value less than 0.05 was considered as significant.
Results
Our study included 285 patients with AP hospitalized in Department of Digestive Tract Diseases. Thirty four patients (11.9%) were hospitalized more than once. Twenty two patients discharged from hospital on request before completing the treatment. Thirteen patients was transferred to intensive care unit (4.6%) and seven patients died (2.5%). Median age of death was 65.3 (range: 38-95). Sudden cardiac arrest was the cause of death in all patients what was accompanied by total respiratory failure in 3 of them.
Epidemiology
The majority of our cohort was male – 65.6% (tab. 1).
Tab. 1. Characteristics of patients with acute pancreatitis
| Acute pancreatitis (N = 285), n (%) |
Sex
female
male |
98 (34.4%)
187 (65.6%) |
Age, years
≤ 39
40-64
≥ 65 |
90 (31.6%)
137 (48.1%)
58 (20.3%) |
Mean age
female
male | 50.01 ± 1.02
56.77 ± 1.86
46.47 ± 1.12 |
Etiology
alcohol abuse
cholelithiasis
idiopathic
cancer (pancreatic or of major duodenal papilla)
hypertriglyceridemia
post-ERCP
drug-related |
149 (52.3%)
77 (27.0%)
49 (17.2%)
6 (2.1%)
2 (0.7%)
2 (0.7%)
2 (0.7%) |
Mean level of CRP on admission p = 0.75
female
male | 63.47 ± 5.76
63.22 ± 9.65
59.55 ± 6.66 |
Mean level of WBC on admission p = 0.83
female
male | 12.41 ± 0.28
12.32 ± 0.33
12.20 ± 0.45 |
Mean duration of hospitalization p=0.92
female
male | 10.54 ± 0.47
10.49 ± 0.74
10.59 ± 0.61 |
Day of the week on admission
monday
tuesday
wednesday
thursday
friday
saturday
sunday |
36 (12.6%)
44 (15.4%)
49 (17.2%)
40 (14.0%)
50 (17.6%)
37 (13.0%)
29 (10.2%) |
Deaths
female
male | 7 (2.5%)
3
4 |
ERCP – endoscopic retrograde cholangiopancreatography; CRP – C-reactive protein; WBC – white blood cells
The ratio of male to female was 1.91:1. Mean age of patients was 50.01 ± 1.02. In our cohort 137 patients (48.1%) were between 40-64 years. The youngest patient was 20, the oldest was 95 years old. Overall, females were significantly older compared to males (p < 0.001) (fig. 1). Mean duration of hospitalization was 10.54 ± 0.47 days with no statistically significant gender differences (p = 0.92). We found no correlation between the age of patients and the duration of hospitalization in our cohort (p = 0.015) (fig. 2). Friday was the most common day of admission to hospital among our patients (17.6%).
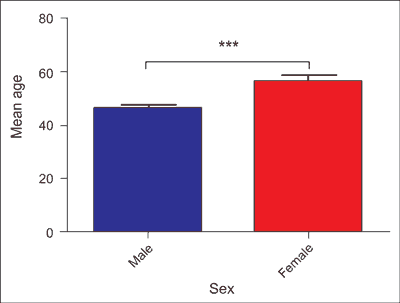
Fig. 1. Overall females were significantly older compared to males in our cohort (p < 0.001). Data represent mean ± SEM. Groups compared using Student’s t-test
***p < 0.001, as compared with male group
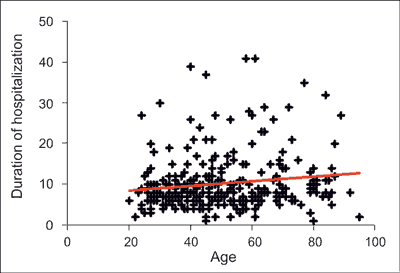
Fig. 2. Correlation between the age of patients and the duration of hospitalization in our cohort followed by a linear regression analysis
Laboratory results
Mean level of CRP on admission to the hospital was 63.47 ± 5.76 (range: 0.2-441.2) and there was no significant difference between male and female (p = 0.75). There was weak significant correlation between the level of CRP and the duration of hospitalization (p < 0.001) (fig. 3). Higher mean levels of CRP on admission was significantly associated with more severe course of AP compared with mild (p < 0.001) and moderate (p < 0.01) course of disease (fig. 4). Mean level of WBC on admission to the hospital was 12.41 ± 0.28 (range: 2.71-33.55). No statistically significant difference between man and female was observed (p = 0.83). No correlation between the level of WBC and duration of hospitalization was demonstrated (p = 0.0273)
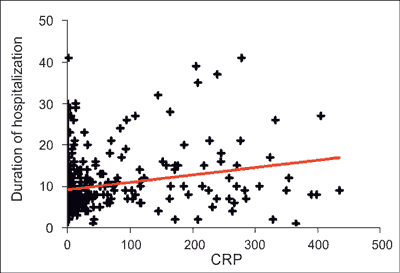
Fig. 3. Correlation between the level of CRP and the duration of hospitalization in our cohort followed by a linear regression analysis
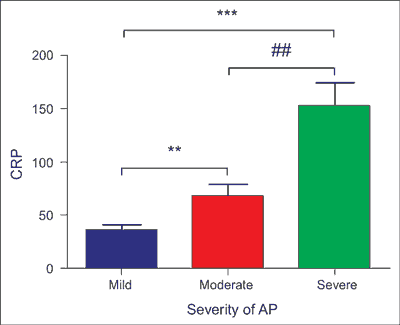
Fig. 4. Mean level of CRP was significantly higher in patients with severe course of AP compared with patients with mild (p < 0.001) and moderate (p < 0.01) course of the disease. Data represent mean ± SEM. Groups compared using ANOVA with Tukey’s test as a post-hoc test
***p < 0.001, as compared with mild group
##p < 0.001, as compared with moderate group
**p < 0.01
Etiology
Alcoholic AP was the most common etiological factor in our cohort and occurred in 149 patients (52.3%). Biliary AP was diagnosed in 77 cases (27%). Pancreatic or major duodenal papilla cancer was detected as a cause of AP in 6 patients (2.1%). Hypertriglyceridemia-induced, iatrogenic and drug-related AP occurred in every 2 patients (0.7% for all). Despite the full examination the cause was not elucidated in 49 patients (17.2%).
Powyżej zamieściliśmy fragment artykułu, do którego możesz uzyskać pełny dostęp.
Mam kod dostępu
- Aby uzyskać płatny dostęp do pełnej treści powyższego artykułu albo wszystkich artykułów (w zależności od wybranej opcji), należy wprowadzić kod.
- Wprowadzając kod, akceptują Państwo treść Regulaminu oraz potwierdzają zapoznanie się z nim.
- Aby kupić kod proszę skorzystać z jednej z poniższych opcji.
Opcja #1
29 zł
Wybieram
- dostęp do tego artykułu
- dostęp na 7 dni
uzyskany kod musi być wprowadzony na stronie artykułu, do którego został wykupiony
Opcja #2
69 zł
Wybieram
- dostęp do tego i pozostałych ponad 7000 artykułów
- dostęp na 30 dni
- najpopularniejsza opcja
Opcja #3
129 zł
Wybieram
- dostęp do tego i pozostałych ponad 7000 artykułów
- dostęp na 90 dni
- oszczędzasz 78 zł
Piśmiennictwo
1. Banks P, Bollen TL, Dervenis C et al.: Classification of acute pancreatitis – 2012: revision of the Atlanta classification and definitions by international consensus. Gut 2012; 62: 102-111.
2. Kozieł D, Głuszek S: Epidemiology of acute pancreatitis in Poland – selected problems. Med Stud 2016; 1: 1-3.
3. Głuszek S, Kozieł D: Prevalence and progression of acute pancreatitis in the Swietokrzyskie Voivodeship population. Pol Przegl Chir 2012; 84: 618-625.
4. Bogdan J, Elsaftawy A, Kaczmarzyk J, Jabłecki J: Epidemiological characteristic of acute pancreatitis in Trzebnica district. Pol Przegl Chir 2012; 84: 70-75.
5. Nesvaderani M, Eslick GD, Vagg D et al.: Epidemiology, aetiology and outcomes of acute pancreatitis: A retrospective cohort study. Int J Surg 2015; 23: 68-74.
6. Vidarsdottir H, Möller PH, Vidarsdottir H et al.: Acute pancreatitis. Eur J Gastroenterol Hepatol 2013; 25: 1068-1075.
7. Yadav D, Lowenfels AB: The epidemiology of pancreatitis and pancreatic cancer. Gastroenterology 2013; 144: 1252-1261.
8. Negoi I, Paun S, Sartelli M et al.: Hypertriglyceridemia-induced acute pancreatitis: a systematic review of the literature. J Acute Dis 2017; 6: 1-5.
9. Tenner S, Baillie J, DeWitt J, Vege SS: American College of Gastroenterology guideline: management of acute pancreatitis. Am J Gastroenterol 2013; 108: 1400-1415.
10. Farthing M, Roberts SE, Samuel DG et al.: Survey of digestive health across Europe: Final report. Part 1: The burden of gastrointestinal diseases and the organisation and delivery of gastroenterology services across Europe. United Eur Gastroenterol J 2014; 2: 539-543.
11. O’Farrell A, Allwright S, Toomey D et al.: Hospital admission for acute pancreatitis in the Irish population, 1997 2004: could the increase be due to an increase in alcohol-related pancreatitis? J Public Health 2007; 29: 398-404.
12. Huang K, Lin P, Nie S et al.: The epidemiological and clinical characteristics of 1316 cases of acute pancreatitis in Guangdong region. Zhonghua nei ke za zhi 2007; 46: 831-834.
13. Sand J, Valikoski A, Nordback I: Alcohol Consumption in the Country and Hospitalizations for Acute Alcohol Pancreatitis and Liver Cirrhosis during a 20-Year Period. Alcohol Alcohol 2009; 44(3): 321-325.
14. Razvodovsky YE: Alcohol consumption and pancreatitis mortality in Russia. JOP 2014; 15(4): 365-370.
15. Roberts SE, Thorne K, Evans PA et al.: Mortality following acute pancreatitis: social deprivation, hospital size and time of admission: record linkage study. BMC Gastroenterol 2014; 14: 153.
16. Roberts SE, Morrison-Rees S, John A et al.: The incidence and aetiology of acute pancreatitis across Europe. Pancreatology 2017; 17: 155-165.
17. Lee JK, Enns R: Review of idiopathic pancreatitis. World J Gastroenterol 2007; 13: 6296-6313.
18. Lankisch PG, Karimi M, Bruns A et al.: Temporal Trends in Incidence and Severity of Acute Pancreatitis in Lüneburg County, Germany: A Population-Based Study. Pancreatology 2009; 9: 420-426.
19. Frey CF, Zhou H, Harvey DJ, White RH: The Incidence and Case-fatality Rates of Acute Biliary, Alcoholic, and Idiopathic Pancreatitis in California, 1994-2001. Pancreas 2006; 33: 336-344.
20. Zhu Y, Pan X, Zeng H et al.: A Study on the Etiology, Severity, and Mortality of 3260 Patients With Acute Pancreatitis According to the Revised Atlanta Classification in Jiangxi, China Over an 8-Year Period. Pancreas 2017; 46: 504-509.
21. Einarsson K, Nilsell K, Leijd B, Angelin B: Influence of Age on Secretion of Cholesterol and Synthesis of Bile Acids by the Liver. N Engl J Med 1985; 313: 277-282.
22. Novacek G: Gender and Gallstone Disease. Wiener Medizinische Wochenschrift 2006; 156: 527-533.
23. Cho JH, Kim TN, Kim SB: Comparison of clinical course and outcome of acute pancreatitis according to the two main etiologies: alcohol and gallstone. BMC Gastroenterol 2015; 15: 87.
24. Kotán R, Pósán J, Sápy P et al.: Analysis of clinical course of severe acute biliary and non biliary pancreatitis: a comparative study. Orv Hetil 2010; 151: 265-268.
25. Andersen AM, Novovic S, Ersbøll AK, Hansen MB: Mortality in Alcohol and Biliary Acute Pancreatitis. Pancreas 2008; 36: 432-434.
26. Losurdo G, Iannone A, Principi M et al.: Acute pancreatitis in elderly patients: A retrospective evaluation at hospital admission. Eur J Intern Med 2016; 30: 88-93.
27. Gardner TB, Vege SS, Chari ST et al.: The Effect of Age on Hospital Outcomes in Severe Acute Pancreatitis. Pancreatology 2008; 8: 265-270.
28. Yadav D, Lowenfels AB: Trends in the Epidemiology of the First Attack of Acute Pancreatitis. Pancreas 2006; 33: 323-330.
29. Párniczky A, Kui B, Szentesi A et al.: Prospective, Multicentre, Nationwide Clinical Data from 600 Cases of Acute Pancreatitis. PLoS One 2016; 11: e0165309.
30. Dervenis C, Johnson CD, Bassi C et al.: Diagnosis, objective assessment of severity, and management of acute pancreatitis. Santorini consensus conference. Int J Pancreatol 1999; 25: 195-210.




