Jolanta Majer1, Sandra Pyda2, Jerzy Robert Ladny3, Antonio Rodriguez-Nunez4, *Lukasz Szarpak5
The impact of the use of a footrest on the quality of chest compressions. A prospective, randomized, cross-sectional study
Wpływ zastosowania podnóżka na jakość uciskania klatki piersiowej. Badanie prospektywne, randomizowane, krzyżowe
1Emergency Unit, Holy Mary Memorial Provincial Specialist Hospital, Czestochowa, Poland
2Polish Society of Disaster Medicine, Warsaw, Poland
3Department of Emergency Medicine, Medical University of Bialystok, Poland
4Institute of Health Research of Santiago (IDIS), Spain; CLINURSID Research Group, Universidade de Santiago de Compostela, Santiago de Compostela, Spain; Paediatric Emergency and Critical Care Division, University Clinical Hospital of Santiago, Universidade de Santiago de Compostela, Santiago de Compostela, Spain; School of Nursing, Universidade de Santiago de Compostela, Santiago de Compostela, Spain
5Lazarski University, Warsaw, Poland
Streszczenie
Wstęp. Prowadzenie wysokiej jakości uciśnięć klatki piersiowej stanowi kluczowy element resuscytacji krążeniowo-oddechowej, przekładający się bezpośrednio na powrót spontanicznego krążenia.
Cel pracy. Celem pracy była ocena wpływu zastosowania podnóżka na jakość uciśnięć klatki piersiowej podczas symulowanej resuscytacji krążeniowo-oddechowej pacjenta na łóżku szpitalnym.
Materiał i metody. Badanie zostało zaprojektowane jako prospektywne, randomizowane, krzyżowe badanie symulacyjne, w którym udział wzięło 55 lekarzy. Uczestnicy badania mieli za zadanie wykonywanie 2-minutowej resuscytacji krążeniowo-oddechowej w oparciu o ciągłe uciśnięcia klatki piersiowej. Lekarze wykonywali uciśnięcia klatki piersiowej w dwóch scenariuszach: z podnóżkiem i bez stosowania podnóżka. Protokół badania został zaakceptowany przez Radę Programową Polskiego Towarzystwa Medycyny Katastrof (zgoda: 21.0.2018.IRB).
Wyniki. Częstotliwość uciśnięć klatki piersiowej w przypadku standardowej resuscytacji bez zastosowania podnóżka wynosiła 128 (IQR: 122-137) CPM, zaś w przypadku zastosowania podnóżka – 126 (IQR: 122-139) CPM. Mediana głębokości uciśnięć klatki piersiowej z podnóżkiem oraz bez podnóżka była zróżnicowana i wynosiła odpowiednio 48 mm (IQR: 43-48) vs. 43 mm (IQR: 37-46). Poprawność relaksacji klatki piersiowej w przypadku scenariusza z podnóżkiem i bez niego wykazywała istotnie statystyczne różnice (P < 0,001) i wynosiła odpowiednio 52% (IQR: 31-55) w przypadku zastosowania podnóżka oraz 30,5% (IQR: 26-35) podczas prowadzenia uciśnięć klatki piersiowej bez wykorzystania podnóżka. Poprawność ułożenia rąk na klace piersiowej podczas wykonywania uciśnięć klatki piersiowej w scenariuszu bez podnóżka wynosiła 72% (IQR: 68-83), zaś w scenariuszu z zastosowaniem podnóżka – 89% (IQR: 73-95; P = 0,015).
Wnioski. Zastosowanie podnóżka w statystycznie istotny sposób podnosi jakość uciśnięć klatki piersiowej w odniesieniu do głębokości uciśnięć klatki piersiowej, stopnia poprawności relaksacji klatki piersiowej oraz poprawności ułożenia rąk na klatce piersiowej.
Summary
Introduction. Conducting high-quality chest compressions is a key element of cardiopulmonary resuscitation that translates directly into the return of spontaneous circulation.
Aim. The aim of the study was to evaluate the impact of the use of the footrest on the quality of chest compressions during simulated cardiopulmonary resuscitation of a patient on a hospital bed.
Material and methods. The study was designed as a prospective, randomized, cross-sectional, simulated study in which 55 doctors participated. The participants of the study were tasked with performing two-minute cardiopulmonary resuscitation based on continuous compressions of the chest. Participants of the study performed chest compressions in two scenarios; with and without using a footrest. The study protocol was accepted by the Institutional Review Board of the Polish Society of Disaster Medicine (Approval No. 21.0.2018.IRB).
Results. The frequency of chest compressions for standard CPR without using the footrest was 128 (IQR: 122-137) CPM and with using the footrest, 126 (IQR: 122-139) CPM. The median depth of chest compressions with and without the footrest varied and was 48 mm (IQR: 43-48) and 43 mm (IQR: 37-46), respectively. The correctness of chest relaxation in the case of with and without a footstool showed statistically significant differences (P < 0.001) and was 52% (IQR: 31-55) when using the footrest, and 30.5% (IQR: 26-35) when performing chest compressions without using the footrest. Correct positioning of the hands on the chest during chest compressions in the scenario without the footrest was 72% (IQR: 68-83), and 89% (IQR: 73-95, P = 0.015) when using the footrest.
Conclusions. The use of a footstool in a statistically significant way increases the quality of chest compressions in relation to the depth of compressions of the chest, the degree of correctness of chest relaxation and the correctness of hand positioning on the chest.

INTRODUCTION
Sudden cardiac arrest constitutes as one of the major causes of mortality and morbidity worldwide. Atwood’s research indicates that the prevalence of out-of-hospital cardiac arrest in Europe is 275,000 cases per year (1). The survival rate of cardiac arrest is small, as indicated in studies by Nakanishi et al. (2), and Lindner et al. (3) the average survival rate for discharging people from non-hospital cardiac arrest is from 3 to 25%. In the case of in-hospital cardiac arrest, Girotra et al. (4), as well as Andrèasson et al. (5), indicate a survival rate of 20-40% with discharge from the hospital.
The history of cardiopulmonary resuscitation dates back to the middle of the 20th century, when mouth-to-mouth resuscitation was described by Dr. Peter Safar from the University of Pittsburgh in 1950’s, and when chest compressions were described at Johns Hopkins. Those methods were combined into the description of Cardiopulmonary Resuscitation in 1960 (6, 7). Currently, thanks to medical development, we have much more knowledge and guidelines for the management of cardiac arrest which are issued by the European Resuscitation Council (ERC) as well as the American Heart Association (AHA) every five years (8-11). The current guidelines for CPR were published in 2015. They indicate the rules of conducting cardiopulmonary resuscitation for both adult patients, children and newborns. However, it should be noted that numerous clinical and simulation studies indicate insufficient quality of chest compressions performed both by medical personnel (12-14), as well as casual witnesses of the event (15).
AIM
The aim of the study was to evaluate the impact of the use of a footrest on the quality of chest compressions during simulated cardiopulmonary resuscitation of a patient on a hospital bed.
MATERIAL AND METHODS
The study was designed as a prospective, randomized, cross-sectional, observational study. After the approval of the examination protocol by the Institutional Review Board of the Polish Society of Disaster Medicine (Approval No. 21.0.2018.IRB), the study was conducted based on medical simulation in the period from January to March 2018. After informing the study participants about the research goals, 56 doctors were recruited who had previously received training in basic resuscitation. Criteria of inclusion in the study contained parameters as such: a professionally active physician; clinical experience in the field of cardiopulmonary resuscitation. Exclusion criteria included pain in the wrist, back pain, pregnancy, and refusal to participate in the study. Voluntary written informed consent was taken from each participant.
In order to simulate a patient requiring cardiopulmonary resuscitation, an adult simulator, Resusci Anne Simulator (Laerdal, Stavanger, Norway), was used. The patient was placed on the Prodigy 3 hospital bed (Famed, Zywiec, Poland) set in resuscitation mode. In order to exclude the impact of breathing on the quality of cardiopulmonary resuscitation, the simulator was previously intubated and connected to the ventilator to allow for asynchronous resuscitation. The participants of the study were tasked with performing a two-minute cardiopulmonary resuscitation cycle with and without a footrest. For this purpose, a 25-cm tall footrest was selected, which was placed next to the hospital bed during cardiopulmonary resuscitation. Both the order of the participants and the methods of chest compressions were randomized. For this purpose, the Research Randomizer program (randomizer.org) was used. The subjects were divided into two groups. The first group began to perform continuous chest compressions without a footstool, and the second group with the use of a footstool. After the two-minute cycle, the participants had a 20-minute break and then performed compressions using a different method. A detailed randomization procedure for the study is shown on figure 1.
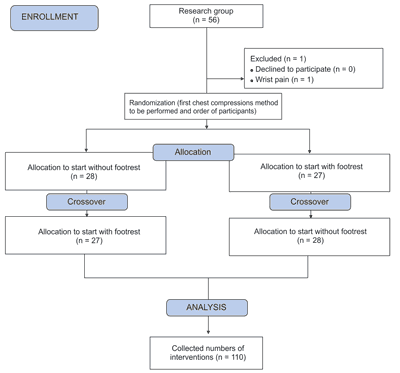
Fig. 1. Randomization flow chart
The study analyzed the quality parameters of chest compressions indicated by the software controlling the simulator. For this purpose, the following parameters were used: depth of chest compressions, frequency of chest compressions, degree of complete chest relaxation and proper positioning of hands during compressions. In addition, after completing the study, the participants filled out a questionnaire assessing the level of fatigue depending on the method of chest compressions. For this purpose, a 100-point scale was used (“1” – no fatigue, “100” – extreme fatigue).
All statistical analysis was performed using the statistical package, STATISTICA 13.0 EN (StatSoft, Tulusa, OK, USA). The results were presented as the median and the quarter interval (IQR), either as a number or percentage (%). The occurrence of normal distribution was confirmed by the Kolomogorov-Smirnov test. When the data was not characterized by normal distribution, non-parametric tests were used. Results were considered statistically significant at p < 0.05.
RESULTS
Participants
Powyżej zamieściliśmy fragment artykułu, do którego możesz uzyskać pełny dostęp.
Mam kod dostępu
- Aby uzyskać płatny dostęp do pełnej treści powyższego artykułu albo wszystkich artykułów (w zależności od wybranej opcji), należy wprowadzić kod.
- Wprowadzając kod, akceptują Państwo treść Regulaminu oraz potwierdzają zapoznanie się z nim.
- Aby kupić kod proszę skorzystać z jednej z poniższych opcji.
Opcja #1
29 zł
Wybieram
- dostęp do tego artykułu
- dostęp na 7 dni
uzyskany kod musi być wprowadzony na stronie artykułu, do którego został wykupiony
Opcja #2
69 zł
Wybieram
- dostęp do tego i pozostałych ponad 7000 artykułów
- dostęp na 30 dni
- najpopularniejsza opcja
Opcja #3
129 zł
Wybieram
- dostęp do tego i pozostałych ponad 7000 artykułów
- dostęp na 90 dni
- oszczędzasz 78 zł
Piśmiennictwo
1. Atwood C, Eisenberg MS, Herlitz J et al.: Incidence of EMS-treated out-of-hospital cardiac arrest in Europe. Resuscitation 2005; 67(1): 75-80.
2. Nakanishi N, Nishizawa S, Kitamura Y et al.: The increased mortality from witnessed out-of-hospital cardiac arrest in the home. Prehosp Emerg Care 2011; 15(2): 271-277.
3. Lindner TW, Søreide E, Nilsen OB et al.: Good outcome in every fourth resuscitation attempt is achievable – an Utstein template report from the Stavanger region. Resuscitation 2011; 82(12): 1508-1513.
4. Girotra S, Nallamothu BK, Spertus JA et al.; American Heart Association Get with the Guidelines-Resuscitation Investigators: Trends in survival after in-hospital cardiac arrest. N Engl J Med 2012; 367(20): 1912-1920.
5. Andrèasson AC, Herlitz J, Bång A et al.: Characteristics and outcome among patients with a suspected in-hospital cardiac arrest. Resuscitation 1998; 39(1-2): 23-31.
6. Aitchison R, Aitchison P, Wang E et al.: A review of cardiopulmonary resuscitation and its history. Dis Mon 2013; 59(5): 165-167.
7. Webb RT, Bacon D: History of Resuscitation. Int Anesthesiol Clin 2017; 55(3): 117-129.
8. Perkins GD, Handley AJ, Koster RW et al.; Adult basic life support and automated external defibrillation section Collaborators: European Resuscitation Council Guidelines for Resuscitation 2015: Section 2. Adult basic life support and automated external defibrillation. Resuscitation 2015; 95: 81-99.
9. Monsieurs KG, Nolan JP, Bossaert LL et al.; ERC Guidelines 2015 Writing Group: European Resuscitation Council Guidelines for Resuscitation 2015: Section 1. Executive summary. Resuscitation 2015; 95: 1-80.
10. Kleinman ME, Brennan EE, Goldberger ZD et al.: Part 5: Adult Basic Life Support and Cardiopulmonary Resuscitation Quality: 2015 American Heart Association Guidelines Update for Cardiopulmonary Resuscitation and Emergency Cardiovascular Care. Circulation 2015; 132 (18 suppl. 2): S414-435.
11. Neumar RW, Shuster M, Callaway CW et al.: Part 1: Executive Summary: 2015 American Heart Association Guidelines Update for Cardiopulmonary Resuscitation and Emergency Cardiovascular Care. Circulation 2015; 132 (18 suppl. 2): S315-367.
12. Smereka J, Szarpak L, Rodríguez-Núñez A et al.: A randomized comparison of three chest compression techniques and associated hemodynamic effect during infant CPR: A randomized manikin study. Am J Emerg Med 2017; 35(10): 1420-1425.
13. Truszewski Z, Szarpak L, Kurowski A et al.: Randomized trial of the chest compressions effectiveness comparing 3 feedback CPR devices and standard basic life support by nurses. Am J Emerg Med 2016; 34(3): 381-385.
14. Kaminska H, Wieczorek W, Matusik P et al.: Factors influencing high-quality chest compressions during cardiopulmonary resuscitation scenario, according to 2015 American Heart Association Guidelines. Kardiol Pol 2018; 76(3): 642-647.
15. Iskrzycki L, Smereka J, Rodriguez-Nunez A et al.: The impact of the use of a CPRMeter monitor on quality of chest compressions: a prospective randomised trial, cross-simulation. Kardiol Pol 2018; 76(3): 574-579.
16. Zou Y, Shi W, Zhu Y et al.: Rate at 120/min provides qualified chest compression during cardiopulmonary resuscitation. Am J Emerg Med 2015; 33(4): 535-538.
17. Lee SH, Kim K, Lee JH et al.: Does the quality of chest compressions deteriorate when the chest compression rate is above 120/min? Emerg Med J 2014; 31(8): 645-648.
18. Bae J, Chung TN, Je SM: Effect of the rate of chest compression familiarised in previous training on the depth of chest compression during metronome-guided cardiopulmonary resuscitation: a randomised crossover trial. BMJ Open 2016; 6(2): e010873.
19. Stiell IG, Brown SP, Christenson J et al.; Resuscitation Outcomes Consortium (ROC) Investigators: What is the role of chest compression depth during out-of-hospital cardiac arrest resuscitation? Crit Care Med 2012; 40(4): 1192-1198.
20. Vadeboncoeur T, Stolz U, Panchal A et al.: Chest compression depth and survival in out-of- hospital cardiac arrest. Resuscitation 2014; 85(2): 182-188.
21. Zhan L, Yang LJ, Huang Y et al.: Continuous chest compression versus interrupted chest compression for cardiopulmonary resuscitation of non-asphyxial out-of hospital cardiac arrest. Cochrane Database Syst Rev 2017; 3: CD010134.
22. Ewy GA, Zuercher M, Hilwig RW et al.: Improved neurological outcome with continuous chest compressions compared with 30:2 compressions-to-ventilations cardiopulmonary resuscitation in a realistic swine model of out-of-hospital cardiac arrest. Circulation 2007; 116(22): 2525-2530.
23. Xanthos T, Karatzas T, Stroumpoulis K et al.: Continuous chest compressions improve survival and neurologic outcome in a swine model of prolonged ventricular fibrillation. Am J Emerg Med 2012; 30(8): 1389-1394.
24. Szarpak L, Truszewski Z, Smereka J et al.: Are paramedics able to perform endotracheal intubation with access to the patient through the back seat of the car? Randomized crossover manikin study. Am J Emerg Med 2016; 34(6): 1161-1163.
25. Szarpak L, Truszewski Z, Smereka J et al.: Does the use of a chest compression system in children improve the effectiveness of chest compressions? A randomized crossover simulation pilot study. Kardiol Pol 2016; 74(12): 1499-1504.
26. Smereka J, Bielski K, Ladny JR et al.: Evaluation of a newly developed infant chest compression technique: A randomized crossover manikin trial. Medicine (Baltimore) 2017; 96(14): e5915.

