Iwona Łapińska1, *Lidia Zawadzka-Głos2
Does tonsillar hypertrophy contribute to speech disorders in children?
Czy przerost migdałków ma wpływ na zaburzenia mowy u dzieci?
1Department of Otolaryngology with Maxillofacial Surgery Subdivision, Provincial Integrated Hospital in Elbląg, Poland
Head of Department: Mirosław Denisiuk, MD
2Department of Pediatric Otolaryngology, Medical University of Warsaw, Poland
Head of Department: Lidia Zawadzka-Głos, MD, PhD
Streszczenie
Wstęp. Przerost migdałka gardłowego i/lub migdałków podniebiennych oraz wysiękowe zapalenie uszu to najczęstsze jednostki chorobowe wieku dziecięcego, z którymi zgłaszają się do laryngologa mali pacjenci. Adenotomia to najczęściej wykonywana operacja chirurgiczna wśród pacjentów pediatrycznych. Wskazania do adenotomii to najczęściej bezdech senny, częste infekcje górnych dróg oddechowych oraz zapalenie ucha środkowego z wysiękiem. Wysiękowe zapalenie ucha jest definiowane jako obecność płynu w uchu środkowym bez współistniejących objawów zakażenia ucha.
Cel pracy. Celem pracy była analiza kliniczna pacjentów poddanych zabiegom wykonywanym w obrębie migdałków oraz ocena wpływu przerostu migdałków na zaburzenia mowy.
Materiał i metody. Badanie było badaniem prospektywnym, w którym wzięło udział 92 pacjentów poddanych zabiegom: adenotomii, adenotonsillotomii i adenotonsillektomii.
Wyniki. Badaniu poddano grupę 92 osób w wieku 4,5-18 lat z dwóch ośrodków, u których zastosowano leczenie operacyjne migdałków. W ośrodku warszawskim udział w badaniu wzięło 63 pacjentów, a w ośrodku elbląskim 29 dzieci. Zdecydowaną większość grupy badanej stanowiły dzieci w wieku od 5 do 9 lat. Pogorszenie słuchu oraz zwiększanie głośności telewizora przed zabiegiem zgłosiło 42 (45,7%) ankietowanych. 37 (40,2%) pacjentów pytało kilka razy o tę samą rzecz. Wśród osób, które prezentowały problemy ze słuchem, 28 (30,4%) pacjentów zgłaszało zaburzenia mowy, a 4 (4,3%) dzieci miało bełkotliwą mowę.
Wnioski. Konieczna jest prawidłowa i wczesna diagnoza oraz odpowiednie leczenie OME u dzieci. Poprawa słuchu u dzieci przyczynia się do poprawy wymowy.
Summary
Introduction. Hypertrophy of the pharyngeal and/or palatine tonsils as well as otitis media with effusion are the most prevalent childhood diseases leading to the referral of children to the ENT specialist. Adenoidectomy is the most commonly performed surgical procedure among paediatric patients. The main indications to adenoidectomy include sleep apnoea, frequent infections of the upper respiratory tract, and otitis media with effusion (OME). OME is defined as the presence of fluid in the middle ear without coexisting symptoms of ear infection.
Aim. The aims of the study were to perform a clinical analysis of patients undergoing surgery on tonsils, and to evaluate the effect of tonsillar hypertrophy on speech disorders.
Material and methods. The prospective study involved a group of 92 patients subjected to surgical procedures including adenoidectomy, adenotonsillotomy and adenotonsillectomy.
Results. The study was carried out in a group of 92 patients aged 4.5-18 years who underwent tonsil surgery in two of Poland’s specialist medical centres. A total of 63 patients treated in the Warsaw centre, and 29 patients receiving treatment in the Elbląg centre, were included. The vast majority of the study group comprised children aged 5 to 9 years. Hearing impairment and the need to turn up the volume of the TV before the procedure were reported by 42 (45.7%) of the respondents. A total of 37 (40.2%) patients reported having to ask about the same thing several times. Among the patients who presented with hearing problems, 28 (30.4%) reported speech disorders, and 4 (4.3%) had slurred speech.
Conclusions. Correct and early diagnosis and appropriate treatment of OME in children is necessary. An improvement of hearing in children contributes to an improvement in pronunciation.
Introduction
Hypertrophy of the pharyngeal and/or palatine tonsils as well as otitis media with effusion are the most prevalent childhood diseases leading to the referral of children to the ENT specialist. Adenoidectomy is the most commonly performed surgical procedure among paediatric patients. The main indications to adenoidectomy include sleep apnoea, frequent infections of the upper respiratory tract, and otitis media with effusion (OME). OME is defined as the presence of fluid in the middle ear without coexisting symptoms of ear infection. Manifestations observed in children with OME include primarily hearing loss and the sensation of ”full ear” (ear obstruction). It should be noted, however, that the symptoms of OME are often latent. Consequently, they are rarely seen in the initial stage of the disease, and can be easily missed. Otoscopy is a commonly performed laryngological examination and, at the same time, one of the primary tools for the diagnosis of OME. The main difficulties associated with otoscopy include narrow ear canals or the child’s crying during the examination (1, 2). Consequently, symptoms of OME may be missed by otoscopic examination, especially in children presenting with no signs of hearing impairment (1). Undiagnosed and untreated OME may have serious consequences including poor speech and delay in intellectual development or permanent anatomical deformities in the middle ear cavity. Therefore, correct and early diagnosis followed by appropriate treatment of OME in children play a very significant role (3).
Aim
The aim of the study was to perform a clinical analysis of patients undergoing tonsil surgery who were diagnosed with speech disorders and conductive hearing loss.
Material and methods
The study group consisted of 92 patients aged 4.5 to 18 years who underwent surgical treatment (adenoidectomy, adenotonsillotomy and adenotonsillectomy) in the Department of Paediatric Otolaryngology, Medical University of Warsaw (63), and the Provincial Integrated Hospital in Elbląg (29). The surgical procedures were performed between 1 February and 30 November 2016. The study had a prospective design. As part of the assessment of eligibility for surgery all patients had their history taken and underwent physical examination. Eligible patients were subjected to surgery and a follow-up examination six months after the procedure. The examination allowed a comparison and evaluation of the outcome of operative treatment of tonsillar hypertrophy in children in a prospectively designed study.
Results
The study was carried out in a group of 92 patients aged 4.5-18 years who underwent tonsil surgery in two of Poland’s specialist medical centres (in Warsaw and Elbląg). A total of 63 patients were treated in the Warsaw centre, and 29 patients received treatment in the Elbląg centre. A vast majority of the study group comprised children aged 5 to 9 years.
In the group of 29 children treated in Elbląg, 18 patients (62.1%) were of the male sex, and 11 patients (37.9%) of the female sex. The group of 63 children treated in the Warsaw centre comprised 38 boys (60.3%) and 25 girls (39.7%) (fig. 1).
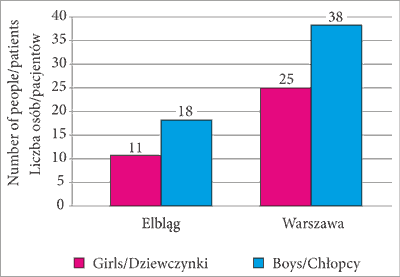
Fig. 1. Distribution of the study group by gender
The procedures performed in the patients were also analyzed, with results presented in figure 2. The main surgical procedure was adenotonsillotomy, performed in a total of 55 patients.
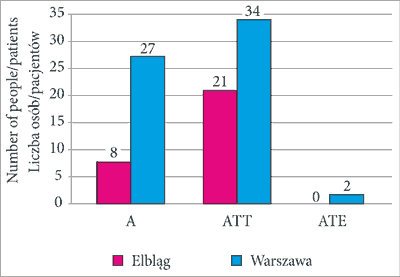
Fig. 2. Type of surgical procedure
Attention was also given to the adjunct surgical procedures performed in the paediatric patients. Tympanostomy was performed in 6 children (20.7%) in Elbląg and 8 children (12.7%) in Warsaw. Tympanocentesis was performed in 3 children (10.3%) in Elbląg and 10 children (15.9%) in Warsaw.
Hearing impairment and the need to turn up the volume of the TV before the procedure were reported by 42 (45.7%) of the respondents. A total of 37 (40.2%) patients reported having to ask about the same thing several times. Six months after the procedure hearing impairment was reported by 2 patients (2.2%), the need to turn up TV volume – by 1 patient (1.1%), and asking about the same thing several times – also by 1 patient (1.1%). Prior to the procedure, otitis was reported by 40 (43.5%) patients, and after the procedure the number dropped to just 1 (1.1%) patient. Among the patients who presented with hearing problems, 28 (30.4%) reported speech disorders, and 4 (4.3%) had slurred speech. A follow-up examination performed 6 months after the procedure showed that none of the patients had a speech disorder or slurred speech (tab. 1).
Tab. 1. Symptoms presented by children with tonsillar hypertrophy
| Symptom | Elbląg | Warsaw | Total |
| I | II | I | II | I | II |
| Turning up TV volume | 18 | 0 | 24 | 1 | 42 | 1 |
| Asking about the same thing several times | 15 | 0 | 22 | 1 | 37 | 1 |
| Slurred speech | 2 | 0 | 2 | 0 | 4 | 0 |
| Otitis | 13 | 0 | 27 | 1 | 40 | 1 |
| Speech disorder | 3 | 0 | 25 | 0 | 28 | 0 |
| Hearing impairment | 12 | 0 | 30 | 2 | 42 | 2 |
Discussion
Complaints experienced by patients with pharyngeal tonsillar hypertrophy depend on the obstruction of the nasopharynx. Hypertrophy of pharyngeal lymphatic tissue may partially or completely block the posterior nostrils, leading to a change in the breathing pattern. The result is closed rhinolalia, which adversely affects the pronunciation of sounds and words. Severe palatine tonsillar hypertrophy has an effect on pharyngeal patency and mobility of the soft palate and palatal arches. Pharyngeal tonsillar hypertrophy may also result in the obstruction of the pharyngeal opening of the Eustachian tube, leading to hearing loss and, consequently, exacerbating the speech disorder.
The main function of the Eustachian tube is ventilation of the middle ear in order to equalize air pressure in the middle ear (4). Mechanical obstruction of the Eustachian tube due to pharyngeal tonsillar hypertrophy can be an important factor contributing to OME (5, 6). Symptoms of OME are often latent. As a result, they initially go unnoticed by the paediatric patients themselves and people around them. Manifestations of otitis media with effusion in children which may alert parents or caregivers include turning up the TV volume, asking several times about the same thing or a decline in school performance. Some children with tonsillar hypertrophy are diagnosed with OME despite reporting no complaints associated with impaired hearing (1). Sometimes parents are not aware of the symptoms of hearing impairment in their children. Untreated OME may have serious consequences including poor speech and impaired intellectual development as well as permanent anatomical deformities in the middle ear cavity. In our study, as many as one-third of the study population presented with speech disorders, and four patients had slurred speech. All the children with slurred speech underwent adenotonsillectomy (ATE). After the surgical procedures on the tonsils the number of patients with speech disorders and slurred speech dropped to zero. These positive outcomes demonstrate the benefit of a surgical procedure involving a reduction in volume or complete removal of pharyngeal lymphatic tissue in patients with hearing impairment and speech disorder.
One of the recent studies has shown that the mean values of middle ear pressure are significantly higher in patients with pharyngeal tonsillar hypertrophy (7-9). The airflow passing through the relatively narrower lumen creates negative pressure leading to the dysfunction of the auditory tubes (1). Studies by Alhady i Sharnoubi (7) show that the most severe auditory tube dysfunction occurs in patients with tonsillar hypertrophy, while less severe Eustachian tube disorders are seen in patients with chronic sinusitis, and the least severe complaints are associated with chronic tonsillitis. Kindermann et al. (10) in their study found that obstruction of the pharyngeal orifice of the Eustachian tube caused by hypertrophy of pharyngeal lymphatic tissue was associated with tympanograms suggestive of abnormal pressure in the middle ear. A study conducted by Günel et al. (11) showed that the mean negative pressure in the middle ear before adenoidectomy was significantly higher than after adenoidectomy, which correlates with the study by Kindermann et al. Our study has demonstrated a clear improvement in hearing after tonsil surgery. The findings are consistent with the results of the survey showing a significant reduction in the number of children with hearing impairment (42:2), increasing the TV volume (42: 1) or asking about the same thing (37:1).
In our study, in addition to adenoidectomy (A) or adenotonsillotomy (ATT), the children concurrently underwent adjunctive surgical procedures: tympanostomy (14) and tympanocentesis (13). A total of 27 procedures were performed. This number is smaller than the number of people who reported impaired hearing or increasing the TV volume before the main procedure (A/ATT) (42 patients). Based on the findings, it may be concluded that tympanostomy or tympanocentesis can only be an auxiliary procedure improving hearing in children after adenoidectomy or adenotonsillotomy.
Conclusions
1. Children with tonsillar hypertrophy may develop speech disorders.
2. An improvement of hearing promotes correct pronunciation and increases the child’s lexicon, as well as improving school performance.
3. Surgical treatment of hypertrophic tonsils produces a positive effect, contributing to the elimination of speech disorders in children.
4. The basic procedure to improve the patency of the auditory tube in children with tonsillar hypertrophy is adenoidectomy.
Piśmiennictwo
1. Ren DD, Wang WQ: Assessment of middle ear effusion and audiological characteristics in young children with adenoid hypertrophy. Chin Med J (Engl) 2012; 125: 1276-1281.
2. Engel J, Anteunis L, Chenault M, Marres E: Otoscopic findings in relation to tympanometry during infancy. Eur Arch Otorhinolaryngol 2000; 257: 366-371.
3. Müderris T, Yazıcı A, Bercin S et al.: Consumer acoustic reflectometry: accuracy in diagnosis of otitis media with effusion in children. Int J Pediatr Otorhinolaryngol 2013; 77: 1771-1774.
4. Chauhan B, Chauhan K: A comparative study of eustachian tube functions in normal and diseased ears with tympanometry and videonasopharyngoscopy. Indian J Otolaryngol Head Neck Surg 2013; 65: 468-476.
5. Di Francesco R, Paulucci B, Nery C, Bento RF: Craniofacial morphology and otitis media with fusion in children. Int J Pediatr Otorhinolaryngol 2008; 72: 1151-1158.
6. Maw AR, Parker A: Surgery of the tonsils and adenoids in relation to secretory otitis media in children. Acta Otolaryngol Suppl 1988; 454: 202-207.
7. Alhady RA, Sharnoubi ME: Tympanometric findings in patients with adenoid hyperplasia, chronic sinusitis and tonsillitis. J Laryngol Otol 1984; 98: 671-676.
8. Egeli E, Oghan F, Ozturk O et al.: Measuring the correlation between adenoidal-nasopharyngeal ratio (AN ratio) and tympanogram in children. Int J Pediatr Otorhinolaryngol 2005; 69: 229-233.
9. Tuohimaa P, Palva T: The effect of tonsillectomy and adenoidectomy on the intra-tympanic pressure. J Laryngol Otol 1987; 101: 892-896.
10. Kindermann CA, Roithmann R, Lubianca Neto JF: Obstruction of the eustachian tube orifice and pressure changes in the middle ear: are they correlated? Ann Otol Rhinol Laryngol 2008; 117: 425-429.
11. Günel C, Ermişler B, Başak HS: The effect of adenoid hypertrophy on tympanometric findings in children without hearing loss. Kulak Burun Bogaz Ihtis Derg 2014; 24(6): 334-338.

