Małgorzata Badełek-Izdebska, *Lidia Zawadzka-Głos
Foreign bodies in the oesophagus on the example of patients of the Department of Paediatric Otolaryngology at the Medical University of Warsaw
Ciała obce w przełyku na przykładzie pacjentów Kliniki Otolaryngologii Dziecięcej WUM
Department of Pediatric Otolaryngology, Medical University of Warsaw, Poland
Head of Department: Lidia Zawadzka-Głos, MD, PhD
Streszczenie
Wstęp. Ciała obce w przełyku to jeden z częstszych nieinfekcyjnych powodów wizyty dziecka w szpitalnej izbie przyjęć. Dzieci zazwyczaj połykają przedmioty przypadkowo w trakcie zabawy, podczas poznawania świata za pomocą zmysłów, a także w czasie spożywania posiłków. Najczęściej połykane są monety, plastikowe lub metalowe fragmenty przedmiotów i baterie. W przełyku mogą także utkwić twarde kawałki jedzenia.
Cel pracy. Celem pracy była analiza objawów klinicznych oraz postępowania diagnostyczno-leczniczego u pacjentów z podejrzeniem obecności ciała obcego w przełyku.
Materiał i metody. Autorzy przeanalizowali kliniczne dane 49 pacjentów hospitalizowanych w Klinice Otolaryngologii Dziecięcej WUM z powodu podejrzenia lub obecności ciała obcego przełyku, a także proces diagnostyczno-leczniczy, podczas którego potwierdzono lub wykluczono rozpoznanie wstępne.
Wyniki. Przeanalizowano objawy, z którymi pacjenci zgłosili się do szpitala, zastosowane procedury diagnostyczne i lecznicze oraz rezultaty leczenia. Zwrócono uwagę na trudności diagnostyczne, jakie może napotkać lekarz w Izbie Przyjęć, a następnie otolaryngolog kwalifikujący pacjenta do leczenia zabiegowego lub decydujący o postępowaniu zachowawczym. Opisano możliwe powikłania mogące wystąpić podczas wykonywania ezofagoskopii.
Wnioski. Najczęstszymi ciałami obcymi są monety, metalowe lub plastikowe części przedmiotów lub pokarm. Najbardziej niebezpiecznymi ciałami obcymi są baterie dyskowe i ostre, duże przedmioty. Diagnostyka obrazowa obejmuje przeglądowe RTG klatki piersiowej i szyi, a w przypadku ciał niekontrastujących RTG z barytem lub watką nasączoną kontrastem.
Obecność objawów klinicznych i/lub wyników badań obrazowych sugerujących obecność ciała obcego w przełyku jest wskazaniem do endoskopii przełyku w znieczuleniu ogólnym.
Zarówno ezofagoskopia sztywna, jak i wykonywana za pomocą giętkiego fiberoskopu są obarczone pewnym stopniem ryzyka, o czym należy poinformować rodziców przed ich wykonaniem.
Summary
Introduction. Foreign bodies in the oesophagus are one of the more frequent non-infectious reasons for a child’s visit to the hospital emergency room. Most often, children swallow items accidentally while having fun, learning about the world with the help of their senses, as well as when eating meals. It is coins, plastic or metal fragments of objects that are usually swallowed. Also, hard pieces of food may stick to the oesophagus.
Aim. The aim of the study was to analyse clinical symptoms as well as diagnostic and therapeutic procedures in patients with suspicion of the presence of a foreign body in the oesophagus.
Material and methods. The authors analysed clinical data of 49 patients hospitalized in the Department of Paediatric Otolaryngology at the Medical University of Warsaw due to the suspicion or presence of a foreign body in the oesophagus. What was also analysed, was the diagnostic and therapeutic process during which the initial diagnosis was confirmed or excluded.
Results. The authors analysed the symptoms with which patients came to the hospital, the diagnostic and therapeutic procedures used and the results of treatment. Attention was paid to diagnostic difficulties that may be encountered by a physician in the Admission Room, and then an otolaryngologist qualifying the patient for interventional treatment or deciding on conservative procedures. Possible complications that may occur during ezophagoscopy are described.
Conclusions. Foreign bodies in the oesophagus are a common problem in the paediatric population. The most common foreign objects are coins, metal or plastic items or food. The most dangerous foreign objects are disc batteries and sharp, large objects.
Diagnostic imaging includes chest and neck X-ray, and in the case of non-contrasting bodies – X-ray with barium or a cotton ball soaked in contrast.
The presence of clinical symptoms and/or imaging results suggesting the presence of a foreign body in the oesophagus is an indication for oesophageal endoscopy under general anaesthesia. Both rigid esophagoscopy and the use of a flexible fiberscope are burdened with a certain degree of risk, of which the parents should be informed before those are performer.
Introduction
Foreign bodies in the oesophagus are one of the more frequent causes of hospitalization of patients in laryngology units. Most often, foreign objects are swallowed by children accidentally during play, while learning about the outside world with the help of the senses of touch and taste, as well as when eating meals. The youngest children, including infants, are not always able to signal the swallowing of objects; however, vigilant observation by their parents or their presence during an accidental ingestion of the item, is the reason for the carers to contact the doctor and implement appropriate diagnostics. Symptoms may vary in severity, depending on the type of the foreign body, its location, and the time of presence of the body in the oesophagus. Depending on these circumstances, appropriate measures are implemented.
Aim
The aim of the study was to analyse clinical symptoms as well as diagnostic and therapeutic procedures in patients with suspicion of the presence of a foreign body in the oesophagus.
Material and methods
The research material was the history of diseases of 49 patients hospitalized in the Department of Paediatric Otolaryngology of the Paediatric Hospital of the Medical University of Warsaw from the end of December 2015 to the beginning of April 2018. A retrospective analysis of the medical data of children admitted to our department due to the suspicion of presence of a foreign body in the oesophagus was conducted. The data from the interview was analysed, as well as the symptoms that the patient reported to the hospital, the results of imaging tests, indications for the performance of esophagoscopy or the reasons for resignation from the treatment, and factors determining the possibility of ending treatment in the hospital ward.
Results
In the analysed period, 49 patients were registered and admitted to the Department of Paediatric Otolaryngology. There were 21 girls and 28 boys in the studied group of patients. The youngest patient at the time of admission to the ward was 6 months old, the oldest – 17 years and 7 months old. The division into age groups was as follows: children up to 12 years old accounted for 14.3%, children from 13 years of age up to 2 years old accounted for 16.3%, patients aged 2-3 years accounted for 24.5%, the remaining 44.9% were patients over 3 years of age. Only one patient was admitted as planned for esophagoscopy due to symptoms lasting for many months, which could suggest, inter alia, the presence of an obstacle in the oesophagus. The remaining 48 patients were admitted to hospital urgently; in 45 children symptoms had appeared within 24 hours before hospitalization, three children had had symptoms for a few days before entering the hospital. In a large part of patients, the interview for the possibility of swallowing a foreign body was positive. This applied to children who reported problems after swallowing an item they were playing with for a short time before the symptoms occurred, as well as situations in which parents or caregivers were convinced that the missing objects or fragments were likely to be in the child’s mouth. These were mostly coins or plastic tokens, as well as plastic elements of toys or decorations. Other situations that caused the parents to report to the hospital were problems with swallowing, directly or shortly after eating a meat meal, fish, pieces of fruit or vegetables and sweets. The aliments presented by the patients were mainly related to problems with swallowing of solid food, but also fluids. Some patients complained about the feeling of an obstacle in the throat or neck, as well as neck pain in the projection of the oesophagus, and the pain was not always associated with the act of swallowing. Other symptoms observed in children included salivation, vomiting, retching or refusal of food intake. One patient had pain in the back. In four patients, a cough was observed, but these children did not present breathing disorders in the form of dyspnoea or stridor.
Upon admission, 7 patients had the results of a chest X-ray carried out in another hospital, of which 6 patients had a review examination, and one X-ray examination with barium pulp. In 40 patients, radiological examination in the form of a chest X-ray was performed in the local hospital emergency ward, in 2 patients the examination was repeated in the ward because of the time that elapsed from the previous imaging examination to the planned esophagoscopy. In 2 patients, radiological examination was aborted upon admission and during further hospitalization. Two patients had a radiological examination with barium pulp carried out upon admission. Imaging studies revealed the presence of a foreign body in the oesophagus projection in 32 cases (31 metallic objects and 1 with bone density); in 5 patients indirect symptoms indicating the possibility of swallowing a foreign body were observed (in 2 examinations, there was an oblong contracting loss (fig. 1) in 1 examination tracheal modelling was described, in one patient the X-ray revealed the stoppage of the barium pulp in the oesophagus, 1 study showed the presence of a unilateral air trap in the pulmonary field). No irregularities were found in 9 X-ray examinations.
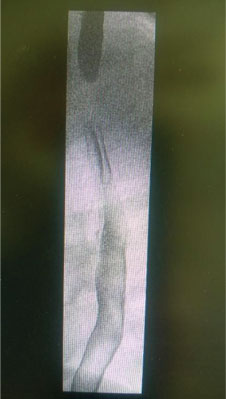
Fig. 1. Longitudinal loss of contrasting (a plastic token)
Rigid esophagoscopy under general anaesthesia was performed in 38 patients, 36 of whom were intubated before the procedure, while in the other two cases, the foreign body was first removed from the pharyngeal laryngoscope using Magilla forceps, and then after intubation, the oesophagus was inspected with a rigid esophagoscope. During esophagoscopy, foreign bodies in the oesophagus were seen and removed in 33 patients; in 5 cases the foreign body in the oesophagus was not found. Among the removed foreign bodies there were: 19 coins, 11 metal objects, 6 plastic elements, 1 bone and 1 seed of green peas. Most foreign bodies were removed from the area of the first or second oesophageal stricture. Items removed from the lower throat were: a metal wire (fig. 2) and a plastic star.
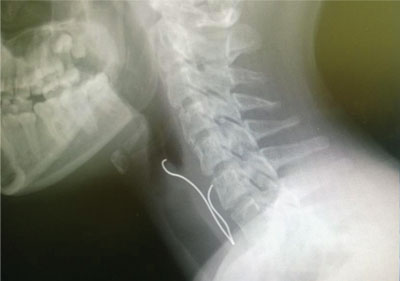
Fig. 2. Wire on the border of the lower throat and esophagus
In four patients, due to coughing in the past and a persistent cough, as well as results of imaging examinations indicating the possibility of aspiration of a foreign body to the respiratory tract, simultaneous bronchoscopy was performed. In three cases, there was a thick mucopurulent secretion in the airways, in the fourth patient – the airways were free.
Four patients underwent gastrofiberoscopy: in two patients, foreign bodies dislocated to the gastric cardia, the next patient was suspected of carrying fragments of a glass bauble in the oesophagus or stomach, one patient reported symptoms after eating a tangerine particle. Coins and a piece of tangerine were removed, while fragments of the bauble were not found.
None of the 38 patients was diagnosed with oesophagus perforation during esophagoscopy; in one case (of an ingested open safety pin) – a slight oesophageal wall injury was found (fig. 3); two children showed slight flushing of the oesophagus wall at the foreign body adhesion site; in two patients a red, stained wall of the oesophagus along its entire length was observed and eosinophilic esophagitis was suspected, which was confirmed in the results of a further histopathological examination.
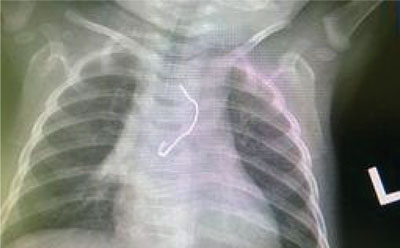
Fig. 3. Safety pin in the esophagus of a 6-month-old child
Seven hospitalized patients were treated conservatively. In three of them the symptoms occurred after eating food (sweets, meat), in two children, the symptoms disappeared quite quickly after admission to the ward, and the X-ray showed no abnormalities, in two patients – metal objects moved to further parts of the gastrointestinal tract, which was confirmed in imaging studies.
In patients who had esophagoscopy with foreign body removal performed, and a scratch or an injury of the oesophageal mucosa was found during the procedure, a control X-ray imaging was carried out, which showed no abnormalities in the form of perforation of the oesophagus or any features of pneumothorax. The girl who had the oesophageal mucosa injured after the removal of the safety pin was hydrated intravenously for 12 hours, then the child was allowed to drink the physiological saline, gradually introducing other fluids to drink, and then food. The remaining patients were able to take oral fluids 2 hours after the procedure, and then their diet was gradually extended.
In all patients, the ailments present at the hospital admission disappeared. Patients without esophagoscopy lesions in the oesophagus mucosa were discharged from the hospital after two days.
Discussion
Foreign bodies in the oesophagus are a common problem in the paediatric period. Most often they enter the gastrointestinal tract accidentally during play, much less often – when eating meals. Items found most frequently in the oesophagus in children are coins, fasteners, metal parts of utility items, tacks, wires, metal or plastic fragments of toys, plastic tokens and buttons. Among the foods that stop in the oesophagus are bones, large and hard pieces of meat, fruit or vegetables. The statistics presented in international publications also confirm the data about our patients published in the previous parts of this paper.
Most foreign bodies pass freely through the gastrointestinal tract without any complications (1). Due to their shape or size, however, they may stop within the oesophagus at various levels. The most common place of entrapment of a foreign body in the oesophagus is its first physiological stenosis just below the ring-throat muscle. Subsequently, foreign bodies stop at the level of the second stenosis and are most rarely found in the oesophagus near the hiatus of the oesophageal diaphragm. The problem of entrapment of a foreign body in the oesophagus or the feeling of an obstacle in the neck may affect patients who suffer from eosinophilic esophagitis (2, 3). Among the patients examined by us, this diagnosis was made in two cases, and was confirmed in histopathological examination of the extracted fragments of the oesophageal mucosa.
Ailments reported by the patient or – in the case of the youngest children – symptoms described by the parents, are most often related to difficulty in swallowing solid or liquid food, refusal of food, salivation in the mouth or throat, vomiting, retching, pain or feeling of an obstacle in the throat or neck (4). Most of our patients presented these symptoms to a greater or lesser extent. Swallowed foreign bodies of considerable size may cause respiratory problems in the form of dyspnoea or cough, less frequently – stridor (5). Cough was one of the symptoms in four of our patients, but as it turned out during bronchoscopy, it resulted from a simultaneous infection within the respiratory tract. Symptoms usually occur shortly after ingestion of a foreign body, but especially in very young children or patients with delayed psychomotor development may be overlooked or noticed after a long time. Only four of the children we examined presented symptoms lasting over 24 hours at the time of admission to the hospital. This is an important fact because foreign bodies may be the cause of complications in the form of perforation of the oesophagus leading to mediastinitis, mediastinum, esophago-tracheal fistula, esophago-oesophageal fistula as well as esophago-aortic fistula (6-8). These complications, especially mediastinitis, are still characterized by a high percentage of mortality, therefore the severity of pain especially when swallowing or breathing, dyspnoea, tachycardia, subcutaneous emphysema should be a stimulus to accelerate the diagnosis and implement proper treatment (9).
Data from an interview with a young patient or their caregivers indicating the presence of a foreign body in the oesophagus are an indication for diagnostic imaging in the form of chest X-ray examinations, both AP and lateral ones (10). X-ray, however, reveals only metallic or strongly calcified structures such as bones. In the case of other foreign bodies, X-ray imaging may be taken after giving the patient barium pulp to drink or after having them ingest a cotton ball soaked in contrast, which is particularly helpful when suspecting swallowing bones or longitudinal sharp objects such as hairpins, toothpicks, etc. This may be conducted on the condition that the child cooperates during the examination and has desire to drink barium or swallow the cotton ball. This study cannot be performed in people with intellectual disability due to the risk of aspiration. An X-ray image assesses the presence of a foreign body in the oesophagus, the level of retention, and the presence of perforation of the oesophageal wall. In the latter case, the barium test is contraindicated; an aqueous contrast medium may be administered, if necessary. Computed tomography is recommended by some authors in the case of suspected presence of small, non-diminutive foreign bodies such as bones, or foreign bodies that have been inside for a long period of time (11). In our group of patients, there were no indications for computed tomography.
In the case of finding a shading foreign body in the oesophagus, the patient is qualified for rigid esophagoscopy under general anaesthesia. In patients with no visible foreign bodies in imaging, but presenting undiminished symptoms and symptoms mentioned above, oesophagus endoscopy is also indicated. Consent for esophagoscopy is provided in writing by parents or legal guardians, and in the case of 16-year-old patients or older – also by themselves. The duration of the procedure depends on the severity of the symptoms and the type of a foreign body. We usually use a 6-hour grace period for food and 2-hour grace period for liquids, yet the information that the foreign body is a disk battery shown in the X-ray obliges us to perform the esophagoscopy as soon as possible due to the risk of electrolyte leakage and the formation of liquefactive necrosis of oesophageal walls in the place where the batteries adhere (12). In the case of our patients, in the considered period, there were no batteries among swallowed items. Esophagoscopy is performed in an operating room, under general anaesthesia and after intubation. After the removal of the foreign body, we always re-check the oesophagus in order to exclude the presence of additional foreign bodies and in order not to miss the possible damage caused by the foreign body or during the manoeuvring with the esophagoscope. Depending on the size and shape of the object, different degrees of damage to the mucous membrane of the oesophagus can be found, which affects further treatment of the patient. Among the children we examined, in the vast majority, changes such as tearing or perforation of the mucosa were not observed, and the most serious one was the cut of the wall made by the sharp end of the open safety pin.
In cases when there is a high probability of the foreign body moving into the stomach, esophagoscopy can be performed with a flexible fiberscope or gastroscope; it took place in three of our patients. In addition, one patient whose symptoms appeared while eating fruit had gastrofibroscopy performed, which allowed to remove the foreign body, as well as visualize mucosal inflammation changes in the oesophagus and stomach, and implement appropriate treatment.
Removal of the foreign body during esophagoscopy resulted in the resolution of aliments with which the patients had reported to the hospital. We did not report any complications after the surgery, but it should be realized that – as with any procedure – the esophagoscopy is burdened with the risk of iatrogenic complications resulting from the presence of a foreign body.
Conservative proceedings, postponement of esophagoscopy or complete resignation in patients who have reported to the hospital due to suspicion of the presence of a foreign body in the oesophagus may take place when the symptoms have significantly decreased over time or have completely disappeared, and a foreign body has not been found in the X-ray examination or has displaced to further parts of the digestive tract. We recommend starting the oral irrigation of the patient, and in the absence of dysphagia symptoms, gradually introducing the mashed diet and further observation of the patient. Parents are advised to thoroughly check the patient’s faeces so that they do not miss the expulsion of the foreign body. If, however, the foreign body is in the stomach for more than 2 weeks, it is advisable to apply to the Department of Gastrology for endoscopic removal. Very rarely, (in fewer than 1% of the cases) it happens that the presence of a foreign body in the oesophagus requires surgical procedure – esophagectomy, usually performed in the thoracic surgery department. They are usually trapped or long-trapped foreign bodies (13). The age of the child below 1.5 years of age is one of the predisposing factors. In the period under consideration, none of our patients required esophagectomy.
Foreign bodies, which due to their size or shape should not be the cause of dysphagia in healthy children, may however become a problem in patients with multiple stresses and oesophageal strictures. One of our patients experienced symptoms in the form of salivation, retching and problems with food intake. In this 13-year-old boy with Arnold-Chiari syndrome, with tracheostomy due to paralysis of the vocal folds and massive deformation of the chest and spine, dysphagia was resolved after the removal of the green pea grains in the esophagoscope (fig. 4). The anatomic structure was the causative factor in the occurrence of problems during food intake.
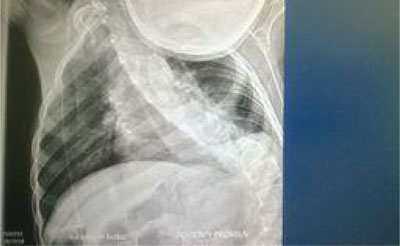
Fig. 4. Distortion of the spine and chest
Conclusions
Foreign bodies in the oesophagus are a common problem in the paediatric population. The most common foreign objects are coins, metal or plastic items or food.
Diagnostic imaging includes chest and neck X-ray, and in the case of non-contrasting bodies – X-ray with barium or a cotton ball soaked in contrast.
The presence of clinical symptoms and/or imaging results suggesting the presence of a foreign body in the oesophagus is an indication for oesophageal endoscopy under general anaesthesia. The most dangerous foreign objects are disc batteries and sharp, large objects.
Both rigid esophagoscopy and the use of a flexible fiberscope are burdened with a certain degree of risk, of which the parents should be informed before those are performer.
Piśmiennictwo
1. Lee JH: Foreign body ingestion in children. Clin Endosc 2018; 51(2): 129-136.
2. El-Matary W, El-Hakim H, Popel J: Eosinophili cesophagitis in children needing emergency endoscopy for foreign body and food bolus impaction. Pediatr Emerg Care 2012; 28(7): 611-613.
3. Hudson S, Sampson C, Muntz HR et al.: Foreign body impaction as presentation of eosinophili cesophagitis. Otolaryngol Head Neck Surg 2013; 149(5): 679-681.
4. Sink JR, Kitsko DJ, Mehta DK et al.: Diagnosis of Pediatric Foreign Body Ingestion: Clinical Presentation, Physical Examination, and Radiologic Findings. Ann Otol Rhinol Laryngol 2016; 125(4): 342-350.
5. Baddouh N, Arjdal L, Raji A, Bourrous M: Unsuspected Cause of Respiratory Distress: Unrecognized Esophageal Foreign Body. Case Rep Pediatr 2018; 2018: 6283053.
6. Wei Y, Chen L, Wang Y et al.: Proposed management protocol for in gested esophageal foreign body and aortoesophageal fistula: a single center experience. Int J Clin Exp Med 2015; 8(1): 607-615.
7. Liming BJ, Fischer A, Pitcher G: Bronchial Compression and Tracheosophageal Fistula Secondary to Prolonged Esophageal Foreign Body. Ann Otol Rhinol Laryngol 2016; 125(12): 1030-1033.
8. Cole S, Kearns D, Magit A: Chronic esophageal foreign bodies and secondary mediastinitis in children. Ann Otol Rhinol Laryngol 2011; 120(8): 542-545.
9. Liu J, Zhang X, Xie D et al.: Acute mediastinitis associated with foreign body erosion from the hypopharynx and esophagus. Otolaryngol Head Neck Surg 2012; 146(1): 58-62.
10. Iwama I: Overlooked radiographic finding results in delayed diagnosis of a retained oesophageal foreign body. BMJ Case Rep 2014; 2014. pii: bcr2014204856.
11. Park S, Choi DS, Shin HS et al.: Fish bone foreign bodies in the pharynx and upper esophagus: evaluation with 64-slice MDCT. Acta Radiol 2014; 55(1): 8-13.
12. Krom H, Visser M, Hulst JM et al.: Serious complications after button battery ingestion in children. Eur J Pediatr 2018; 177(7): 1063-1070.
13. Schramm JC, Sewell RK, Azarow KS et al.: Chronic cervical esophageal foreign bodies in children: surgical approach after unsuccessful endoscopic management. Ann Otol Rhinol Laryngol 2014; 123(1): 19-24.



