Michał Michalik, *Adrianna Podbielska-Kubera, Alfred Samet, Agnieszka Dmowska-Koroblewska, Marcin Broda
Corynebacterium pseudodiptheriticum – a dangerous respiratory pathogen. A case report
Corynebacterium pseudodiptheriticum – niebezpieczny patogen dróg oddechowych. Opis przypadku
Department of Otolaryngology, MML Medical Centre, Warsaw, Poland
Head of Department: Michał Michalik, MD, PhD
Streszczenie
Jesteśmy przekonani, że w patogenezie przewlekłego zapalenia zatok zbyt małą rolę przypisuje się bakteriom należącym do rodzaju Corynebacterium. W większości przypadków szczepy te traktowane są jako zanieczyszczenia. Tymczasem bakterie z rodzaju Corynebacterium mogą stanowić klinicznie istotny czynnik chorobotwórczy, zwłaszcza w przypadkach, gdy pobrane próbki materiału pochodzą z dolnych dróg oddechowych od chorych objawowych. Szczepy Corynebacterium cechują się zdolnością przetrwania w postaci biofilmów w środowisku szpitalnym, przyczyniając się do rozprzestrzeniania oporności na antybiotyki.
Przedstawiamy rzadki przypadek zakażenia Corynebacterium pseudodiptheriticum. Pacjentką była 10-letnia dziewczynka, która skarżyła się na nawracające katary i problemy z zatokami. Wykonano zabieg adenotomii i funkcjonalnej endoskopowej operacji zatok. Pacjentka zgłosiła się ponownie na konsultację pół roku po zabiegu z powodu utrzymującego się od 2 tygodni zaostrzenia objawów chorobowych (napływanie gęstej, trudnej do odkrztuszenia wydzieliny). Z pobranych wymazów wyhodowano C. pseudodiptheriticum i Staphylococcus epidermidis. Zastosowano leczenie cyprofloksacyną. Pacjentka zaobserwowała poprawę stanu zdrowia. Opisany przypadek zwraca uwagę na konieczność identyfikacji szczepów do gatunku oraz podkreśla rangę gatunków bakteryjnych uznawanych powszechnie za komensalne, które mogą u osób predysponowanych przyczynić się do wystąpienia poważnych powikłań.
Summary
We believe that an insufficient role is attributed to bacteria belonging to the genus Corynebacterium in the pathogenesis of chronic sinusitis. These strains are treated as contaminants in most cases. Meanwhile, Corynebacterium strains may be a clinically significant pathogenic agent, especially in cases where samples are collected from the lower respiratory tract in symptomatic patients. Corynebacterium strains can survive in the form of biofilms in hospitals and cause multi-resistant infections.
We present a rare case of Corynebacterium pseudodiptheriticum infection. The patient was a 10-year-old girl who complained of recurrent rhinitis and sinusitis. Adenoidectomy and functional endoscopic sinus surgery were performed. The patient returned for a consultation after six months due to exacerbation of the disease symptoms lasting for 2 weeks (inflow of thick secretions difficult to expectorate). Corynebacterium pseudodiptheriticum and Staphylococcus epidermidis were cultured from swabs. The patient was treated with ciprofloxacin, and her condition improved. The described case points to the need to identify strains of a given species and to pay attention to species commonly considered as commensals that may contribute to serious complications.
Introduction
Opportunistic microorganisms are etiological factors of many infectious diseases. Under normal conditions, they colonise the skin, oral cavity, upper respiratory tract and mucous membranes without causing any symptoms. However, commensals may induce infections in immunocompromised patients, patients after surgeries, as well as those with organ and systemic diseases. Such organisms include gram-positive club-shaped bacilli, i.e. Corynebacterium (1).
Of the 90 Corynebacterium species described in 2014, 16 were isolated from different environments, such as synthetic surfaces, food, water and soil; about 50 were isolated from humans or human clinical material; and 32 species were found in animals. Several species were detected both in humans and animals, which implies the possibility of transferring bacteria between animals and humans (2).
It was thought for many years that within clinically relevant bacteria only a very limited number of Corynebacterium species are potential human pathogens, e.g. C. diphtheriae, which is the etiological factor in diphtheria (2). However, literature data show that, based on the natural location in the oropharyngeal cavity, respiratory infections, such as acute and chronic bronchitis, acute exacerbations of bronchitis, pneumonia, and necrotising tracheitis, are also encountered (2).
Corynebacterium spp. infections usually affect patients receiving immunosuppressive therapy, long-term antibiotic therapy, or steroid treatment. Furthermore, these strains are isolated significantly more frequently from elderly patients (> 65 years), patients after surgeries, with ischemic heart disease, renal failure, respiratory failure, diabetes, cancer, multiorgan injuries, HIV, after amputations, transplantations and in patients receiving renal replacement therapy (1).
Corynebacterium spp. are characterised by significant virulence: they exhibit adhesive, haemolytic and haemagglutination activity. The most virulent strains include C. diphtheriae, C. pseudotuberculosis, C. urealyticum and C. ulcerans (3).
Together with C. striatum and C. propinquum, 2 closely related species, C. diphtheriticum forms a group of newly emerging respiratory pathogens, particularly in patients with chronic respiratory infections. Literature reports include patients with chronic obstructive pulmonary disease (COPD) and cystic fibrosis (CF). HIV-infected patients are also at a higher risk of C. pseudodiphtheriticum infections (2).
Corynebacterium pseudodiphtheriticum is a part of local bacterial microflora of the skin and mucus membranes in humans (4). Isolated in clinical trials, it is usually treated as contaminants (5). Nevertheless, these bacteria have emerged as opportunistic pathogens causing clinically significant infections in recent decades (4). The most important infections include endocarditis in patients with heart valves, respiratory infection (trachea, bronchi, lungs), and urinary tract infections (1).
Although the pathogenicity of C. pseudodiptheriticum is not an uncommon phenomenon, its role as an opportunistic pathogen is limited mainly to the lower respiratory tract, particularly in immunocompromised patients (6).
Corynebacterium pseudodiptheriticum plays an important role as an in-hospital pathogen. Unfortunately, so far little is known about its virulence factors (7). It is believed that the affinity for human fibrinogen and fibronectin, and the ability to form biofilms may contribute to the generation and spread of C. pseudodiptheriticum infections (8). Biofilm-related infections are considered to be the main cause of in-hospital morbidity and mortality. Bacteria living in a biofilm environment have the ability to exchange genetic material, and can also become permanent colonisers of a given body region (9). Souza et al. (8) described adhesive properties and the ability to form biofilm on hydrophilic (glass) and hydrophobic (plastic) surfaces by C. pseudodiptheriticum strains isolated from patients with local (pharyngitis) and systemic (bacteremia) infections.
Case report
A 10-year-old patient reported to Medical Center MML in Warsaw due to a 4-year history of rhinitis and sinusitis. Radiographic documentation showed opacity of the sinuses. The patient provided a report from sinus CT performed a month earlier, which confirmed chronic inflammation in the right maxillary sinus, obstructed ostiomeatal complexes and ethmoidal opacity. Changes were observed in the right sphenoid sinus. Physical examination revealed mucous secretion in the maxillary sinus ostium and a hypertrophic pharyngeal tonsil blocking the nasal passages. Chronic maxillary sinusitis was diagnosed, functional endoscopic sinus surgery (FESS) and adenoidectomy were performed. The patient reported with earlier results of bacteriological tests, which were positive for Haemophilus infuenzae, Neisseria, and S. epidermidis. CT was performed (fig. 1).
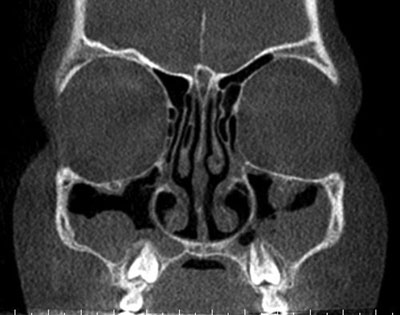
Fig. 1. Sinus CT before the procedure
Adenoidectomy and FESS were performed in 2016. Augmentin was included. The patient reported for a follow-up visit 2 days after procedure. She was feeling good and showed no signs of bleeding. The nose was healing without bleeding, the pharynx was pale.
The patient reported again for consultation 6 months after the surgery due to symptom exacerbation (lasting for 2 weeks): an inflow of thick secretion difficult to expectorate. Bacteriological swabs were collected. All samples were secured on Amies transportation medium with activated charcoal. Microbes were cultured under aerobic conditions. Gram staining was positive for multiple Gram-positive club-shaped rods. The catalase test was positive. The microbes were then identified using the API-Coryne test (bioMerieux, France). An automatic method (Vitek 2, bioMerieux) and commercially available manual tests were used to assess drug resistance. Corynebacterium pseudodiptheriticum and Staphylococcus epidermidis were grown. Cipronex was included. Patient’s condition improved. CT was performed (fig. 2). Also, treatment with silver nanoparticles and intestinal flora analysis were recommended.
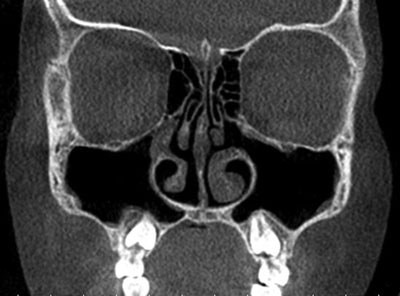
Fig. 2. Sinus CT after the procedure
Discussion
Diseases caused by Corynebacterium strains are a serious medical and veterinary problem. These are opportunistic microorganisms, which are aetiological factors of multiple human and animal diseases. They should never be underestimated as they may contribute to therapeutic failures, prolonged treatment time and increased costs (1).
Van Roeden et al. confirmed that C. pseudodiptheriticum should be considered a clinically relevant pathogen when cultured from the lower respiratory tract in symptomatic patients (7). The authors attempted to clarify the clinical significance of C. pseudodiptheriticum as a lower respiratory pathogen and to identify patients at a risk of infection caused by this microbe. The majority of patients (86%) were diagnosed with comorbidities (heart and lung diseases). All isolates were sensitive to amoxicillin (7).
Camello et al. (10) isolated C. pseudodiptheriticum from patients in various age groups. The microbes were mainly related to infections in the urinary tract (29.2%), respiratory tract (27.45%) and injection sites (18.6%). Strains were obtained only from 32.7% of patients. These patients had at least one comorbidity: end-stage renal disease, renal transplant, AIDS, tuberculosis, cancer, hepatic cirrhosis, haemodialysis and catheter use. Antimicrobial susceptibility tests confirmed multiresistant strains. Most of these strains (> 50%) were resistant to oxacillin, erythromycin and clindamycin (10).
The authors emphasised that despite significant differences in age and health status of patients, C. pseudodiptheriticum may be the cause of various infections. It is extremely important to identify the species of the pathogen and to select an appropriate antibiotic therapy (10).
In their study in 1,589 patients, Kraev et al. (3) showed that aside from C. diphtheriae, 11% of acute upper respiratory tract infections were caused by other Corynebacterium species. C. pseudodiphtheriticum and C. xerosis were isolated most frequently. Furthermore, Kraeva et al. (3) showed that Corynebacterium (except for C. diphtheriae) were most often isolated from clinical samples in combination with Staphylococcus and Streptococcus strains.
Chandran et al. (5) obtained various Corynebacterium species: C. pseudotuberculosis, C. ulcerans, C. striatum, C. minutissimum, C. haemolyticum. The strains were isolated from catheter tips, sputum, tracheostomy secretions and wound infections. They were highly resistant to many antibiotics as opposed to isolates from blood (C. pseudotuberculosis, C. minutissimum, C. ulcerans and C. renale), which were sensitive to most antibiotics. Furthermore, the isolates were able to produce a biofilm. This ability allows for bacterial survival in hospitals, which may lead to the development of multiresistant strains (5). Literature data indicate that some Corynebacterium species show mechanisms of erm (X)-associated acrolide-lincosamide-streptogramin B (MLSB) resistance (8). According to Olender et al., a large proportion of strains (89.7%) isolated from nasal mucosa in patients with upper respiratory symptoms showed constitutive MLSb resistance (9).
Pèrez-Parra et al. (12) described a case of infective endocarditis by Corynebacterium pseudodiphtheriticum in an 8-year-old child with an aortic valve. The infection caused a severe neurological embolism and death. The authors emphasised that cases of endocarditis, which are usually diagnosed in immunocompromised patients, are often associated with poor prognosis.
Indumathi et al. (6) reported a case of a 6-year-old previously healthy boy with diphtheria-like illness caused by C. pseudodiptheriticum. In countries with very low incidence of diphtheria, C. pseudodiphtheriticum should be included in the differential diagnosis for a child presenting with diphtheria-like illness. Simple, rapid screening tests should be used to differentiate the pathogen from C. diphtheriae (6).
Johnson et al. (13) described a case of endocarditis in a 14-year-old boy with tetralogy of Fallot. Blood cultures grew C. pseudodiphtheriticum. There have also been reports of septic arthritis caused by C. pseudodiphtheriticum. The literature review implies that the pathogen is rare, which may result in late diagnosis and inappropriate treatment.
Cantarelli et al. (14) reported a rare case of cutaneous infection caused by C. pseudodiphtheriticum. The patient presented to a clinical laboratory with a skin ulcer on his left lower limb. C. pseudodiphtheriticum was identified. The infection was successfully treated with ciprofloxacin.
Cases of C. pseudodiphtheriticum infection related to other conditions, such as hyperamonaemia, are also encountered. It should be remembered that urinary tract infections caused by urease-producing bacteria may increase serum ammonia, which leads to consequences (11).
As part of natural pharyngeal microflora, C. pseudodiphtheriticum is likely to prevent colonisation by more pathogenic microbes. C. pseudodiptheriticum may be used as nasal and pharyngeal probiotic, e.g. after eradication of nasal S. aureus (15). Kiryukhina et al. (15) suggested that a saline suspension of C. pseudodiphtheriticummay may be used to eliminate S. aureus from the nasal cavity. However, further investigations are needed.
Only a limited number of cases of C. pseudodiphtheriticum infections in sinusitis may be found in literature. There were few reports on the presence of Corynebacterium, but without specifying the species of these strains.
Merino et al. (16) investigated aspirates from patients with chronic maxillary sinusitis. The most prevalent aerobic bacteria included Streptococcus viridans (27.6%), Streptococcus pneumoniae (11.7%), Corynebacterium species (11.5%), Staphylococcus aureus (9.4%), Moraxella catarrhalis (6.6%), Hemophilus parainfluenzae (5.8%), group C beta haemolytic streptococci (4.5%) (17).
Biel et al. (18) presented their study in 174 patients diagnosed with chronic maxillary sinusitis requiring endoscopic surgical intervention. Aseptic aspirates were collected during the procedure. A total of 217 isolates were recovered from 174 patients. Coagulase-negative staphylococci prevailed (36%). Furthermore, Staphylococcus aureus (25%), Streptococcus viridans (8.3%), Corynebacterium (4.6%) and anaerobic bacteria (6.4%) were isolated.
Conclusions
Corynebacterium pseudodiptheriticum is considered a clinically relevant pathogen when cultured from the lower respiratory tract in symptomatic patients. Compared to the available literature data, our findings indicate that only a minor role is attributed to Corynebacterium bacteria in the pathogenesis of chronic sinusitis. Corynebacterium strains are usually treated as contaminants. However, these are opportunistic pathogens, which may contribute to clinically relevant infections. Corynebacterium strains are able to survive in the form of biofilms in hospitals, and thus contribute to multi-resistance. Therefore, proper and complete identification of strains as well as determination of their resistance to antibiotics are crucial. This will allow for implementing appropriate epidemiological procedures in patients from whom such strains were isolated.
Piśmiennictwo
1. Banaszkiewicz T, Krukowski H: Corynebacterium – występowanie i chorobotwórczość dla ludzi i zwierzą. Medycyna Wet 2011; 67(4): 229-232.
2. Burkovski A: Corynebacterium pseudodiphtheriticum: Putative probiotic, opportunistic infector, emerging pathogen. Virulence 2015; 6(7): 673-674.
3. Kraeva LA, Manina ZN, Tseneva GI, Radchenko AG: Etiologic role of Corynebacterium non diphtheriae in patients with different pathology. Zh Mikrobiol Epidemiol Immunobiol 2007; (5): 3-7.
4. Furiasse D, Gasparotto AM, Monterisi A et al.: Pneumonia caused by Corynebacterium pseudodiphtheriticum. Rev Argent Microbiol 2016; 48(4): 290-292.
5. Chandran R, Puthukkichal DR, Suman E, Mangalore SK: Diphtheroids-Important Nosocomial Pathogens. J Clin Diagn Res 2016; 10(12): DC28-DC31.
6. Indumathi VA, Shikha R, Suryaprakash DR: Diphtheria-like illness in a fully immunised child caused by Corynebacterium pseudodiphtheriticum. Indian J Med Microbiol 2014; 32(4): 443-445.
7. Van Roeden SE, Thijsen SF, Sankatsing SU, Limonard GJ: Clinical relevance of Corynebacterium pseudodiphtheriticum in lower respiratory tract specimens. Infect Dis (Lond) 2015; 47(12): 862-868.
8. Souza MC, dos Santos LS, Sousa LP et al.: Biofilm formation and fibrinogen and fibronectin binding activities by Corynebacterium pseudodiphtheriticum invasive strains. Antonie Van Leeuwenhoek 2015; 107(6): 1387-1399.
9. Olender A, Niemcewicz M: Macrolide, lincosamide, and streptogramin B-constitutive-type resistance in Corynebacterium pseudodiphtheriticum isolated from upper respiratory tract specimens. Microb Drug Resist 2010; 16(2): 119-122.
10. Camello TC, Souza MC, Martins CA et al.: Corynebacterium pseudodiphtheriticum isolated from relevant clinical sites of infection: a human pathogen overlooked in emerging countries. Lett Appl Microbiol 2009; 48(4): 458-464.
11. Goda T, Watanabe K, Kobayashi J et al.: A case of hyperammonemia with obstructive urinary tract infection by urease-producing bacteria. Rinsho Shinkeigaku 2017; 57(3): 130-133.
12. Pèrez-Parra S, Peña A, Blanca E, García F: Letal endocarditis due to Corynebacterium pseudodiphtheriticum. Rev Chilena Infectol 2016; 33(2): 229-231.
13. Johnson JN, Miller SG, Lodge AJ: Corynebacterium endocarditis of a percutaneously placed transcatheter pulmonary valve. Cardiol Young 2014; 24(5): 932-934.
14. Cantarelli V, Brodt TC, Secchi C et al.: Cutaneous infection caused by Corynebacterium pseudodiphtheriticum: a microbiological report. Rev Inst Med Trop Sao Paulo 2008; 50(1): 51-52.
15. Kiryukhina NV, Melnikov VG, Suvorov AV et al.: Use of Corynebacterium pseudodiphtheriticum for elimination of Staphylococcus aureus from the nasal cavity in volunteers exposed to abnormal microclimate and altered gaseous environment. Probiotics Antimicrob Proteins 2013; 5(4): 233-238.
16. Merino LA, Ronconi MC, Hreñuk GE, de Pepe MG: Bacteriologic findings in patients with chronic sinusitis. Ear Nose Throat J 2003; 82(10): 798-800, 803-804, 806.
17. Erturan G, Holme H, Iyer S: Corynebacterium pseudodiphtheriticum septic arthritis secondary to intra-articular injection-a case report and literature review. J Med Microbiol 2012; 61(Pt 6): 860-863.
18. Biel MA, Brown CA, Levinson RM et al.: Evaluation of the microbiology of chronic maxillary sinusitis. Ann Otol Rhinol Laryngol 1998; 107(11 Pt 1): 942-945.

