© Borgis - New Medicine 3/2011, s. 93-98
*Mariann Csernus Raskovicsné1, László Papp2, Sándor Hollós3, Ildikó Szabó Kádárné4, Zoltán Balogh1
Examination of pressure ulcer prevalence and its application in creating quality indicators
1Semmelweis University Faculty of Health Sciences, Institute of Applied Health Sciences, Department of Nursing
Dean: Judit Mészáros CSc, professor
2University of Szeged, Faculty of Health Sciences and Social Studies, Department of Nursing
Head of department: Kornélia Helembai CSc, professor
3Semmelweis University Faculty of Health Sciences, Institute of Health Promotion and Clinical Methodology, Department of Clinical Studies
Dean: Judit Mészáros CSc, professor
4Pandy Kalman Hospital
Nursing director: Magdolna Mészáros Halmosné
Summary
Aim. The study aims to formulate a reliable, authentic prevalence marker, wherein the structural influences are not emerging and that can be used on annual basis, and opens the door to create a quality indicator to use among patients with high risk of pressure ulcer.
Material and methods. The study was conducted in 2006 in all inpatient wards of a 1500-bed county hospital. After quarterly retrospective duration prevalence (PD) and on predetermined dates, point-prevalence (PP) data collection, means were calculated to obtain yearly prevalence numbers, of which further examination was done with standard deviation (SD) measurment. An indicator was created among high-pressure ulcer risk patients using standard scale.
Results. Both examinations (longitudinal and cross-sectional) showed different prevalence among the hospital wards. High deviation was noticed between wards, but for the examination of the efficiency of pressure ulcer monitoring, results were prosperous (SDPD=0,699, SDPP=2,121). When creating quality indicators, we found significant difference between the examination methods.
Conclusions. Correlation was noticed between prevalence of pressure ulcers and the number of high-risk patients. The results also showed that quality indicator formulated from high-risk patient data could be applied to the clinical practice as a yearly examination method.
Introduction
Multimorbidity strongly contributes to the incidence of pressure ulcers. The incidence of decubitus is higher in patients over 60 years of age, who are incapable to suffice their own needs. Except of age, reduced moving ability, immobility, malnutrition, blood circulation problems, diabetes, fever, incontinence, obesity, dermatological problems and frostbite are also risk factors (14). Different studies also examined correlations between fecal incontinence, diarrhoea, fractures, dementia and hypalbuminaemia as risk factors and the occurence of decubitus (1, 3, 13, 16-18). Pressure ulcers, which evolve during healthcare are often associated with thrombophlebits, cellulitis, fascia necrosis, osteomyelitis and sepsis (4).
Pressure ulcers become a serious health problem, challenging both the community, the health care and health insurance systems. Its occurence is typical at all stages of healthcare (basic care, home care, hospital care). Because of the parellelism of the methods in health and social care, the social home care network also provides pressure ulcer care (10-12).
The health quality assurance systems consider both its prevention and treatment as important quality indicators of care. During configuration, use and evaluation of quality indicators, different questions emerged like: How could we evaluate, and with what markers should we compare the results? Are the conclusions valid and are they reliable for the representation of the care quality? (7).
Prevalence and incidence are common statistical markers for expressing frequencies of the illnesses, and they can be also used for the description of pressure ulcers (5, 6).
Both international and Hungarian health literature use these indicators to present the pressure ulcer care.
In Hungary, according to the Association for the Improvement of Care of Chronic Wounds and Incontinentia studies, the prevalence of pressure ulcers is between 40000-50000 cases per year (9) (table 1).
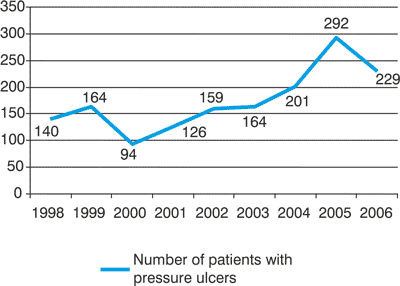
Table 1. Number of patients with pressure ulcers between 1998-2006.
Aim of the study
During the research process, we aimed to find a prevalence marker, which:
– when applicated, measures reliable, authentic incidence and prevalence on annual level, wherein the structural influences are not emerging, and
– opens the door to create a quality indicator when used among patients with high risk of pressure ulcer.
Materials and methods
The study was done in 2006 in all inpatient wards of a 1500-bed county hospital. When selecting the sample wards, we considered the occurence of pressure ulcers from previous years. In the recent study, internal medicine (both acute and chronic), surgical and intensive care wards were chosen to participate. All patients treated in these units, including all patients suffering from pressure ulcers, participated in the research. Before commencing the study, we gained ethical approval for this study from the hospital′s general director (table 2).
Table 2. Sample distribution by wards and examination methods (nr of persons).
| Ward | Internal medicine (chronic) | Internal medicine (acute) | ICU | General surgery | Sum |
| By duration | I. | 20 | 4 | 7 | 3 | 34 |
| II. | 16 | 6 | 5 | 5 | 32 |
| III. | 6 | 0 | 10 | 1 | 17 |
| IV. | 17 | 4 | 9 | 8 | 38 |
| Sum (Nd) | 59 | 14 | 31 | 17 | 121 |
| By timeframe | I. | 4 | 1 | 1 | 0 | 6 |
| II. | 4 | 1 | 0 | 0 | 5 |
| III. | 1 | 0 | 0 | 1 | 2 |
| IV. | 3 | 0 | 3 | 2 | 8 |
| Sum (Np) | 12 | 2 | 4 | 3 | 21 |
When creating data pool for the analysis, we made quarterly retrospective Pd and in predetermined, random dates – a Pp data collection in each wards. After all data was collected, statistical means were calculated for the formulation of prevalence markers (PD, PP) of the year 2006.
Pd, Pp = number of all patients with pressure ulcers/number of all patients (N) * 100
PD = (Pd1 + Pd2 + Pd3 + Pd4) / N
PP = (Pp1 + Pp2 + Pp3 + Pp4) / N
Using the quarterly numbers, standard deviation (SD) was calculated to measure the data deviation from statistical mean.
SDPD = Σ (Pd(1-4) – Pd)2 / N
SDPP = Σ (Pp(1-4) – Pp)2 / N
Patients with high risk of pressure ulcers were filtered using the criteria of the expanded version of Norton Scale (level of cooperation/motivation, skin status, accompanying illnesses, physical condition, mental condition, activity, mobility, incontinence, age), which was used in the sample hospital. Patients with 20 or less points in the Norton scale were assigned to this subgroup.
The ratio of patients with high risk of pressure ulcers and all patients with decubitus were also examined referring to year 2006. The examination was done with two different methods.
1. Both patient numbers (high risk vs. all pressure ulcer patients) were followed throughout the year, and the ration was calculated at the end of the year (Id);
2. Both numbers were collected in predetermined quarterly dates throughout the year, and the data was summarized at the end of the year to formulate the ratio (Ip).
Id = no. of all patients with decubitus / no. of high risk patients * 100
Id = Nd / Nhr * 100
Ip = no. of all patients with decubitus at a quarterly date / no. of high risk patients at a quarterly date * 100
Ip = Σnd(1-4) / Σnhr(1-4) * 100
Results
Our survey was performed quarterly in every sample ward. As study data, we measured duration-prevalence at each study stage, and point-prevalence in predetermined, random dates during the research process. From these data, we calculated statistical means, in order to formulate prevalence markers of the whole year (diagram 1, 2).
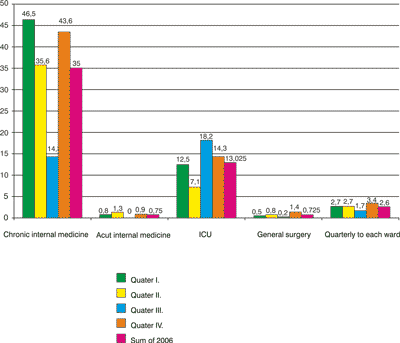
Diagram 1. Duration-prevalence by sample wards (%); Nd=121.
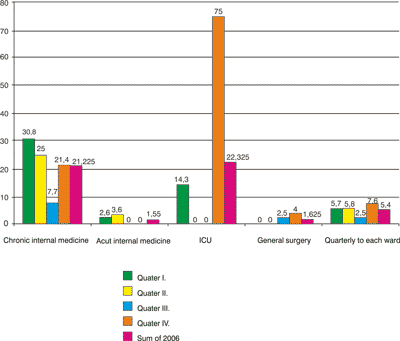
Diagram 2. Point-prevalence by sample wards (%); Np=21.
As quarterly duration-prevalence data shows, the pressure ulcer is most frequent at the Chronic Internal Medicine ward (PD = 14,3-46,5%). The occurence of pressure ulcer is between 7,1-18,2% in ICU, 0-1,3% in acute Internal Medicine and 0,2-1,4% in the Surgery.
Examining the wards separately, we observed high standard deviation (SDPD) (diagram 3), but the efficacy of the analysis could be seen in the summarized prevalence data (PD), which is 1,7-3,4 %, with low deviation (SDPD = 0,699).
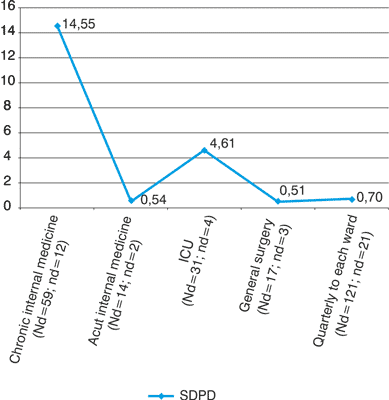
Diagram 3. Standard deviation of duration-prevalence, year 2006.
In the quarterly point-prevalence data (PP1-4), we also noticed high numbers at Chronic Internal Medicine (7,7--30,8 %). At ICU, we measured very high deviation since in some data collecting sessions, there was no patient with pressure ulcer in the ward. This also raised the SD value of the whole data (SDPP = 2,12) (diagram 4).
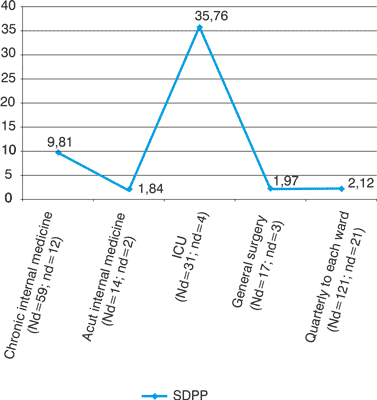
Diagram 4. Standard deviation of point-prevalence, year 2006.
The patient data was labeled using the criteria of expanded Norton scale, which was used at the hospital and qualitative indicators were created using methods explained earlier. Diagram 5 shows the results both by wards and summarized.

Diagram 5. Ábra: Minőségi indikátorok, 2006 (%).
As the wardly separated data shows, at Chronic Internal Medicine, each measurement resulted in high numbers. At ICU, the quality indicator based on the data collected at specific dates is higher. These results ensued from the large number of high-risk patients.
Quality indicator based on duration data, according to summarized data, is almost twice as high as the one created with point-prevalence.
Conclusions
If we interpret our results as longitudinal survey, our analysis demonstrates continuously high prevalence of pressure ulcers in Chronic Internal Medicine ward (PD1-4=14,3-46,5, PD=35). The cross-sectional data collection showed high occurence of pressure ulcers at Chronic Internal Medicine (PP1-4=7,7-30,8, PP=21,2), but also at ICU (PP=22,3). We noticed high deviation in two sample wards (Chronic Internal Medicine, ICU) during both longitudinal and cross-sectional data analysis, but for the examination of the efficiency of pressure ulcer monitoring, results were prosperous (SDPD=0,699, SDPP=2,121). The sample size also influences the validity of the prevalence data. There were wards during both longitudinal and cross-sectional data collection, where no pressure ulcers were detected.
The prevalence of pressure ulcers and high-risk patient number correlate: among highly endangered patients, there is higher chance of pressure ulcers. When creating quality indicators from high-risk patient data, we noticed significant difference between longitudinal and cross-sectional results (Id=15,75; Ip=8,01). The results also showed that quality indicator formulated from high-risk patient data could be applied to the clinical practice as a yearly examination method.
Piśmiennictwo
1. Allman RM, Laprade CA, Noel LB et al.: Pressure sores among hospitalized patients. Annals of Internal Medicine 1986 Sep; 105 (3): 337-42. 2. Belica É: A kórházi ellátás minőségének indikátorai IV. Az 1996-os betegforgalmi adatokra vonatkozó elemzések, EMIKK füzetek, 16. szám, Debrecen, 1998 (Indicators of the hospital care quality IV. Data analysis from year 1996. – in hungarian). 3. Berlowitz DR, Wilking SV: Risk factors for pressure sores. A comparison of cross-sectional and cohort-derived data. Journal of the American Geriatrics Society 1989 Nov; 37 (11): 1043-50. 4. National Center for Epidemiology, Ajánlások az intézményi decubitus-fertőzések monitorozásának kialakításához, Epinfo 2009; 16: 14-15 (Recommendations for development of an institutional-level monitoring system for pressure ulcers. – in hungarian). 5. EPUAP vázlatos állásfoglalása a prevalencia és incidencia nyomonkövetésre vonatkozóan. Sebinko 2003; 1: 11-14. (EPUAP statement of prevalence and incidence follow-up. – in hungarian). 6. Forgács I, Paksy A, Pauka T: Népegészségtan, HIETE, Budapest 1995; 61-63. (Public Health – in hungarian). 7. Frantz RA: Measuring prevalence and incidence of pressure ulcers. Advanced Wound Care 1997 Jan-Febr; 10 (1): 21-24. 8. Gulácsi L: Association for the Improvement of Care of Chronic Wounds and Incontinentia, Sebinko 1998; 6: 1-6. 9. Gulácsi L: Minőségfejlesztés az egészségügyben. Medicina Könyvkiadó Rt., Budapest; 2000: 468-470. (Quality improvement in health care – in hungarian). 10. Hoppe C, Kottner J, Dassen T, Lahmann N: Pressure ulcer risk and pressure ulcer prevalence in German hospitals and nursing homes. Pflege Z 2009 Jul; 62 (2): 424-8. 11. Hoppe C, Pöhler A, Kottner J, Dassen T: Pressure ulcers: new data about risk, prevalence and places of development. Results of a study in German nursing homes and hospitals. Pflege Z 2008 Feb; 61 (2): 90-3. 12. Lahmann N, Halfens RJ, Dassen T: Effect of non-response bias in pressure ulcer prevalence studies. Journal of Advanced Nursing 2006 Jul; 55 (2): 230-6. 13. Mecocci P, von Strauss E, Sherubini A et al.: Cognitive impairment is the major risk factor for development of geriatric syndromes during hospitalization: results from the GIFA study. Dementia and Geriatric Cognitive Disorders 2005; 20(4): 262-9. 14. Pearson A, Francis K, Hodgkinson B, Curry G: Prevalence and treatment of pressure ulcers in Northern New South Wales. Australian Journal of Rural Health 2000; Vol. 8, Pt. 2: 103-110. 15. Raskovics-Csernus M, Papp L: Nurse′s roles in chronic wounds care, Nővér – Hungarian Journal of Nursing Theory and Practice 2007; 20(6): 14-21 (in hungarian). 16. Shahin ES, Dassen T, Halfens RJ: Pressure ulcer prevalence and incidence in intensive care patients: a literature review. Nursing in Critical Care 2008 Mar-Apr; 13 (2): 71-9. 17. Tannen A, Dassen T, Halfens R: Differences in prevalence of pressure ulcers between the Netherlands and Germany – associations between risk, prevention and occurrence of pressure ulcers in hospitals and nursing homes. Journal of Clinical Nursing 2008 May; 17(9): 1237-44. 18. Theaker C, Mannan M, Ives N, Soni N: Risk factors for pressure sores in the critically ill. Anaesthesia 2000 Mar; 55 (3): 221-4.





