© Borgis - New Medicine 4/2013, s. 114-119
Magdalena Frąckiewicz1, *Lidia Zawadzka-Głos1, Elżbieta Podsiadły2, Lechosław P. Chmielik1, Joanna Rogulska2
Bacteriological aetiology of chronic rhinosinusitis in children; a study from the pediatric otolaryngology clinic of the warsaw medical university
1Department of Pediatric Otolaryngology, Medical University of Warsaw, Poland
Head of Department: Lidia Zawadzka-Głos, MD, PhD
2Department of Laboratory Diagnostics and Clinical Immunology of Development Age, Poland
Head of Department: prof. Urszula Demkow, MD, PhD
Summary
Introduction. Chronic rhinosinusitis (CRS) is a long-lasting inflammation whose aetiology is multifactorial. In the majority of patients, the disease develops from an existing impaired patency of the nose or ostia of paranasal sinuses. Such patients require surgical treatment, however almost always the disease is accompanied by bacterial infection of this region.
Aim. To identify and estimate the sensitivity of pathogens to drugs through bacteriological testing of samples from children surgically treated for chronic rhinosinusitis or those where preliminary treatment of such diseases has been proposed.
Material and methods. The study was performed on children who had undergone the initial stage of conservative treatment at the Department of Paediatric Otolaryngology, Warsaw Medical University between 2007 and 2010. Samples for bacteriological examination were collected during the endoscopic sinus surgery from under the middle nasal turbinates and maxillary sinuses.
Results. Pathogens that either most frequently caused or co-existed with chronic rhinosinusitis were determined in samples taken from the maxillary sinuses and from under the middle nasal turbinates. Staphylococcus aureus was found to be the most frequently cultured.
Discussion. Chronic rhinosinusitis develops as a result of composite and multistage inflammatory process. At least one component of the CRS pathogenesis is through chronic or recurrent bacterial infection. Our study demonstrated in many cases a lack of correlation between the results from under the nasal turbinates and maxillary sinuses.
Conclusions. 1. Our screening tests have a different bacterial aetiology for rhinosinusitis than those patients seen by their family doctor. 2. In most cases results from under the middle nasal turbinate differ from the lumen of maxillary sinuses. 3. Examining samples taken from under the middle nasal turbinates and maxillary sinuses plays a vital role in establishing the aetiology of rhinosinusitis and in choosing the appropriate treatment if a recurrence of rhinosinusitis occurs. 4. On basis of this study, the authors suggest amoxicillin and amoxicillin with clavulanate acid be used as first line treatment agents in cases of exacerbated chronic rhinosinusitis.
INTRODUCTION
In essence, chronic rhinosinusitis is a long-lasting mucosal inflammation of the nose and paranasal sinuses that cannot be cured by pharmacological treatment (1, 3, 4). Its most frequent cause in children is an impaired patency of the nose or of the ostia of paranasal sinuses together with local immunological disorders. Factors that predispose children to chronic rhinosinusitis are adenoids, nasal septum deviation, tumor of the nasopharynx, retained foreign bodies in the nose, unilateral or bilateral choanal atresia. Its main symptoms are: a dense muco-purulent discharge retained in the nasal cavities, impaired nasal patency and others including a productive cough, (mainly in the morning), a clearing one’s throat, halitosis, loss of appetite and smell, morning vomiting and in older children recurrent headaches.
Regardless of the cause, bacterial infection almost always plays role in the pathomechanism of chronic rhinosinusitis (1-3). Antibiotic therapy is seen to be vital regarding the frequency in which of chronic rhinosinusitis occurs. Family doctors usually do not make a bacteriological examination because the plain nasal culture, available in a surgery, has little diagnostic value. However, bacteriological testing of samples taken from under the middle nasal turbinates and lumen of maxillary sinuses can be important although this is basically inaccessible for family doctors, paediatricians or even otorhinolaryngologists from out-patient clinic. For these doctors, whose role is to administer antibiotic therapy, a knowledge of the most frequent pathogens in this disease is thereby important. The compositions of pathogens changes over time and will depend on local living conditions of the population. Therefore, adequately equipped clinical centers should monitor on their region for the most frequent bacteriologic agents in cases of chronic rhinosinusitis.
Aim
To identify and estimate the sensitivity of pathogens to drugs through bacteriological testing of samples taken from under the middle turbinates and lumen of maxillary sinuses from children surgically treated for chronic rhinosinusitis or those where preliminary treatment of such diseases has been proposed.
MATERIAL AND METHODS
The study was performed on 230 patients with chronic rhinosinusitis (107 females, 123 males) aged 5 to 17, where conservative treatment had been ineffective and who underwent endoscopic surgery at the Clinical Department of Pediatric Otolaryngology, of Warsaw Medical University in the period between January 2007 and May 2010. Before surgery, patients were treated with antibiotics and 36 (15.65%) of patients received antibiotics during the surgery. Samples for bacteriological examination were collected during the surgical procedure from under both middle nasal turbinates using a swab and from maxillary sinuses using a suction assembly. The material was cultured on TSA medium containing 5% defibrinated mutton-blood, chocolate agar with bacitracin (HAEM, Biomerieux), Chapman’s medium (MSA2, Biomerieux), MacConkey’s medium (MCK, Biomerieux), whereas sample material from the sinuses was additionally cultured on a medium for the isolation of anaerobic bacteria (SCS, Biomerieux). The cultures were incubated at a temperature 37°C and in the case of the chocolate medium in an atmosphere of 5% CO2, whereas anaerobic cultures were contained within an atmosphere of 10% CO2, 85% N2, 5% H2. Identification of pathogens was performed by ATB Expression System (Biomerieux). The sensitivity to drugs of bacteriological strains was determined using the diffuse-discoid method or E-tests. Determinations and interpretation were carried out according to recommendations of National Drug-sensitiveness Centre and Clinical Laboratory Standards Institute (CLSI). In all cases where results of microbiological examination were positive, antibiograms were performed. Results with antibiograms were attached to the patient’s records in the out-patient clinic for cases exhibiting aggravated of symptoms of CRS.
RESULTS
From the 230 examined children, real pathogens were cultivated in 100 cases from material taken from one or both sinuses. Bacterial aetiology of chronic rhinosinusitis was confirmed in 43.5% of the children examined.
In material taken from the maxillary sinuses there was no growth of pathogens in 66% from the left side and 63.5% from the right side. Among pathogens most frequently observed, Staphylococcus aureus, Haemophilus influenza, Moraxella catarrhalis, Streptococcus pneumoniae, Klebsiella pneumonia were cultured. On the left side in the group under ‘others’ the following were detected: Acinetobacterlwoffii (1), Escherichia coli (1), Pseudomonas aeruginosa (1), Enterobacter cloacae ESBL (-) (1), Pantoea spp. (1), C. guillermondi (1), Staphylococcus mitis (1), Staphylococcus agalactiae (1). Mixed bacterial cultures were seen in 12 cases (fig. 1).
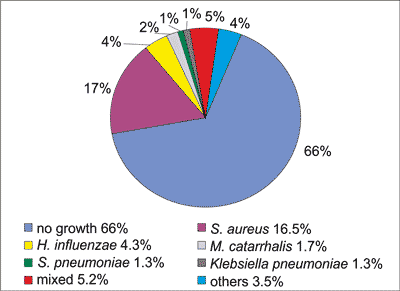
Fig. 1. Results of bacterial cultures from the left maxillary sinus.
On the right side in the group under ‘others’ the following were detected: Acinetobacterlwoffii (1), Escherichia coli (1), Pseudomonas aeruginosa (1), Klebsiella planticolha (1), Staphylococcus mitis (1), Staphylococcus agalactiae (1), Propionibacterium acnes (1), Haemophilus parainfluenzae (1), Proteus mirabilis (1), E. faecalis (1), Candida albicans (1), Actinomyces naeslundii (1). Mixed bacterial cultures were seen in 9 cases (fig. 2).

Fig. 2. Results of bacterial cultures from the right maxillary sinus.
In the material from under the middle nasal turbinates there was no growth of pathogens in 74% on the left side and in 74.3% on the right side. Among pathogens most frequently observed Staphylococcus aureus, Haemophilus influenza, Moraxella catarrhalis, were cultured. On the left side in the group under ‘others’ the following were detected: Pseudomonas aeruginosa (1), Escherichia coli (1), Staphylococcus mitis (1). Mixed bacterial cultures were seen in 6 cases (fig. 3).
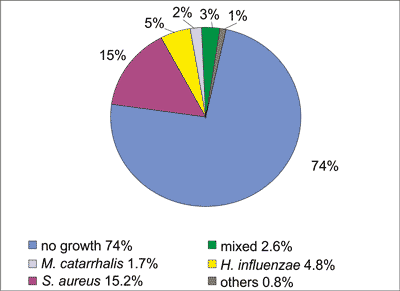
Fig. 3. Results of bacterial cultures from under the left middle nasal turbinate.
On the right side in the group under ‘others’ the following were detected: Streptococcus pyogenes (1), Escherichia coli (1), Staphylococcus mitis (1), Alcaligenes spp. (1), Klebsiellaoxytoca (1) were stated. Mixed bacterial cultures were stated in 8 cases (fig. 4).

Fig. 4. Results of bacterial cultures from under the right middle nasal turbinate.
A more detailed analysis of the infection was performed for separate and mixed pathogens for the following: Staphylococcus aureus, Haemophilusinfluenzae, Streptococcus pneumoniae and Moraxella catarrhalis.
A single aetiological factor from one or both sinuses was cultivated with regard to Staphylococcus aureus in 53 cases (tab. 1), Haemophilusinfluenzaein 16 cases (tab. 2), Streptococcus pneumoniaein 3 cases (tab. 3), Moraxella catarrhalis in 6 cases (tab. 4).
Table 1. Incidence frequency in isolating Staphylococcus aureus from the maxillary sinuses and underthe middle nasal turbinates.
| No | LMS | RMS | Swab from LMNT | Swab from RMNT | Number of patients |
| 1 | S. aureus | S. aureus | S. aureus | S. aureus | 19 |
| 2 | S. aureus | S. aureus | | | 11 |
| 3 | | | S. aureus | S. aureus | 4 |
| 4 | S. aureus | S. aureus | | S. aureus | 1 |
| 5 | | S. aureus | S. aureus | S. aureus | 1 |
| 6 | S. aureus | | S. aureus | S. aureus | 1 |
| 7 | S. aureus | | S. aureus | | 2 |
| 8 | | S. aureus | | S. aureus | 2 |
| 9 | S. aureus | | | | 3 |
| 10 | | S. aureus | | | 7 |
| 11 | | | S. aureus | | 1 |
| 12 | | | | S. aureus | 1 |
| TOTAL | 53 |
LMS – left maxillary sinus, RMS – right maxillary sinus, LMNT – left middle nasal turbinate, RMNT – right middle nasal turbinate
Table 2. Incidence frequency in isolating H. influenzae from the maxillary sinuses and under the middle nasal turbinates.
| No | LMS | RMS | Swab from LMNT | Swab from RMNT | Number of patients |
| 1 | H. influenzae | H. influenzae | H. influenzae | H. influenzae | 4 |
| 2 | H. influenzae | H. influenzae | | | 4 |
| 3 | | | H. influenzae | | 3 |
| 4 | | H. influenzae | | | 2 |
| 5 | | | H. influenzae | H. influenzae | 1 |
| 6 | | | | H. influenzae | 1 |
| 7 | H. influenzae | H. influenzae | | H. influenzae | 1 |
| TOTAL | 16 |
Table 3. Incidence frequency in isolating S. pneumoniae from the maxillary sinuses and under the middle nasal turbinates.
| No | LMS | RMS | Swab from LMNT | Swab from RMNT | Number of patients |
| 1 | S. pneumoniae | S. pneumoniae | | | 1 |
| 2 | | S. pneumoniae | | | 1 |
| 3 | S. pneumoniae | | | | 1 |
| TOTAL | 3 |
Table 4. Incidence frequency in isolating M. catarrhalis from the maxillary sinuses and under the middle nasal turbinates.
| No | LMS | RMS | Swab from LMNT | Swab from RMNT | Number of patients |
| 1 | M. catarrhalis | M. catarrhalis | M. catarrhalis | M. catarrhalis | 3 |
| 2 | M. catarrhalis | M. catarrhalis | | | 1 |
| 3 | | | M. catarrhalis | M. catarrhalis | 1 |
| 4 | | | | M. catarrhalis | 1 |
| TOTAL | 6 |
Mixed infections, the presence of 2 or more pathogens from sinuses or from under the middle nasal turbinates are shown in table 5.
Table 5. Incidence frequency of mixed infections.
| No | LMS | RMS | Swab from LMNT | Swab from RMNT | Number of patients |
| 1. | H. influenzae
S. pneumoniae | H. influenzae
S. pneumoniae | H. influenzae
S. pneumoniae | H. influenzae
S. pneumoniae | 2 |
| 2. | H. influenzae
S. pneumoniae | H. influenzae
S. pneumoniae | S. aureus | S. aureus | 1 |
| 3. | | | H. influenzae
S. aureus | H. influenzae
S. aureus | 1 |
| 4. | H. influenzae
S. pneumoniae | H. influenzae
S. pneumoniae | H. influenzae
| H. influenzae
| 1 |
| 5. | H. influenzae
S. aureus | H. influenzae
S. aureus | H. influenzae | H. influenzae | 1 |
| 6. | E. coli | | H. influenzae | H. influenzae | 1 |
| 7. | S. aureus | S. aureus | S. aureus
H. influenzae
S. pneumoniae | S. aureus | 1 |
| 8. | | | S. pneumoniae
M. catarrhalis | S. pneumoniae
M. catarrhalis | 1 |
| 9. | H. influenzae
S. aureus | H. influenzae
S. aureus | S. aureus | H. influenzae
S. aureus | 1 |
| 10. | S. pneumoniae | S. pneumoniae | | S. pneumoniae
H. influenzae | 1 |
| 11. | S. aureus
H. influenzae | S. aureus | S. aureus | S. aureus
S. pneumoniae | 1 |
| 12. | S. pneumoniae
M. catarrhalis | | | | 1 |
| 13. | H. influenzae | H. influenzae | S. aureus | S. aureus | 1 |
| 14. | H. influenzae
S. pneumoniae | H. influenzae
S. pneumoniae | | | 1 |
| 15. | H. influenzae
M. catarrhalis | H. influenzae
M. catarrhalis | H. influenzae
M. catarrhalis | H. influenzae
M. catarrhalis | 1 |
| 16. | S. aureus | S. pneumoniae | S. aureus | S. aureus | 1 |
| 17. | | S. pneumoniae | S. aureus | S. aureus | 1 |
| 18. | | | S. aureus | K. oxytoca | 1 |
| 19. | | E. faecalis | E. coli | E.coli | 1 |
| TOTAL | 20 |
No correlation observed between results of bacterial cultures from maxillary sinuses and from those under the middle nasal turbinates (p = 0.1573).
The sensitivity to drugs of bacterial strains cultivated from maxillary sinuses or from the middle nasal turbinates of children with chronic rhinosinusitis was as follows:
– in 3 patients there were strains of Streptococcus pneumoniae cultured where all strains were sensitive to penicilin; in one case there was resistance to macrolides, lincosamins and streptogramins b (MLSb),
– among 16 bacterial strains of Haemophilus influenzae, all were sensitive to ampicilin; in 7 cases resistance to trimetoprim/sulfametoxasol was seen,
– among 53 bacterial strains of Staphylococcus aureus, all were sensitive to meticilin and thereby also sensitive to penicilinsisoxasolin, penicilins with inhibitors, cefalosporins and carbapenems; 7 bacterial strains had a MLSb resistance-mechanism (i.e. resistance to macrolides, lincosamins and streptogramins b); in 2 bacterial strains of Staphylococcus aureus there was resistance to 14- and 15-carbonic macrolides and streptogramins b.
Because of cefuroxim and amoxicilin being oversubscribedby family doctors the following bacterial resistance mechanism would be expected to occur in the bacterial cultures: MRSA (Staphylococcus aureus), PRSP (Streptococcus pneumoniae), BLNAR/BLPACR (Haemophilus influenzae). Results actually obtained did not indicate the above-mentioned resistance mechanism. Among bacterial cultures of Staphylococcus aureus and Streptococcus pneumoniae resistance to macrolides, lincosamins and streptogramins b (MLSb) was observed that can be linked to oversubscription of Clindamicin and abuse of selection criteria. Bacterial strains of Streptococcus pneumoniae with resistance to macrolides were cultured sporadically. Obtained preparations of Haemophilus influenzae demonstrated resistance to trimetoprim/sulfametoxasol.
DISCUSSION
Chronic rhinosinusitis develops as a result of composite and multistage inflammation. At least one component of CRS pathogenesis is chronic or recurrent bacterial infection which as a consequence results in a disorder in the normal function of the mucosa (3, 7-9). In this study, samples were taken during surgery from under the middle nasal turbinates and from inner parts of the maxillary sinuses. Among pathogens most frequently observed were: Staphylococcus aureus, Haemophilus influenzae, Streptococcus pneumonia. However, the most frequently occurring agent in the studied group was non-pathogenic Staphylococcus spp. coagulase (-). The results obtained are similar to those described in the literature (7, 10), were likewise the most frequent occurrences were of the non-pathogenic Staphylococcus spp. coagulase (-) and of pathogenic bacteria Staphylococcus aureus.
Except in a few cases, the cultured pathogens were sensitive to commonly administered antibiotics which in Poland are amoxicilin, cefuroxim and clindamicin. In recent years an excessive use of antibiotics can be observed in our country, however not to such a degree as in different regions of the world (5, 6).
Results actually obtained did not indicate the high percentage of resistance mechanism among bacterial strains. The alarm can be engender by Staphylococcus aureus and Streptococcus pneumoniae with resistance to macrolides, lincosamins and streptogramins B (MLSb), that can be linked to oversubscription of macrolides and Clindamicinin treating rhinosinusitis and abuse of selection criteria.
This study also demonstrated that in many cases there was a lack of correlation between the results obtained from under the nasal turbinates and maxillary sinuses.
CONCLUSIONS
1. Results of bacteriological testing in the studied group differ from the aetiology that causes rhinosinusitis in patients seen by the family doctor.
2. Results obtained from the middle nasal turbinate in most cases differ from those taken from the lumen of the maxillary sinuses.
3. Examination of samples taken from the middle nasal turbinates and maxillary sinuses play a vital role in establishing the aetiology of rhinosinusitis and in choosing the precise treatment in cases when rhinosinusitis recurs.
4. On the basis of our study results, authors suggest amoxicillin and amoxicillin with clavulanateacid as a first line treatment agent in the exacerbation of chronic rhinosinusitis.
Piśmiennictwo
1. Frąckiewicz M: Pediatric Otorhinol aryngology, ed. Chmielik M, Medical University of Warsaw, 2010: 9-29. 2. Wu AW, Shapiro NL, Bhattacharyya N: Chronic rhinosinusitis in children: What are the treatment options? Immunol Allergy Clin N Am 2009; 29: 705-717. 3. Mendoza de Morales T: VIII IAPO Manual of Pediatric Otorhinolaryngology, ed. Sih T et al.: São Paulo 2009: 187-193. 4. Bluestone CD et al.: Pediatric Otolaryngology, Fourth Edition, 2003; 2: 998-1009. 5. Bhattacharyya N, Kepnes LJ: The risk of development of antimicrobial resistance in individual patients with chronic rhinosinusitis. Arch Otolaryngol Head Neck Surg 2004; 130: 1201-1204. 6. File TM, Hadley JA: Rational use of antibiotics to treat respiratory tract infections. Am J Manag Care 2002; 8: 713-727. 7. Sandler NA, Johns FR, Braun TW: Advances in the management of acute and chronic sinusitis. J Oral Maxillofac Surg 1996; 54(8): 1005-1013. 8. Vaidya AM et al.: Correlation of middle meatal and maxillary sinus cultures in acute maxillary sinusitis. Am J Rhinol 1997; 11(2): 139-143. 9. Axelsson A, Brorson JE: The correlation between bacteriological findings in the nose and maxillary sinus in acute maxillary sinusitis. Laryngoscope 1973; 83(12): 2003-2011. 10. Kremer B et al.: Clinical value of bacteriological examinations of nasal and paranasal mucosa in patients with chronic sinusitis. Eur Arch Otorhinolaryngol 2001; 258(5): 220-225.



