*Csaba Szekrenyesi1, Kata Rez1, Zoltán Z. Nagy1, 2
Surface temperature change of PMMA plates in refractive surgery performed with two types of modern excimer lasers
1Faculty of Health Sciences, Semmelweis University, Budapest, Hungary
Head of Faculty: Professor Zoltán Zsolt Nagy, MD, PhD
2Department of Ophthalmology, Semmelweis University, Budapest, Hungary
Head of Department: Professor Zoltán Zsolt Nagy, MD, PhD
Summary
Introduction. The conditions in the operating room can have an influence on the postoperative results of the refractive surgery performed with excimer lasers.
Aim. The aim of this study was to examine the relationship of the temperature of PMMA plates (polymethylmethacrylate), environmental conditions and the energy load caused by the laser impulses during refractive surgery procedure.
Material and methods. Wavelight Allegretto and Schwind Amaris excimer lasers were used for the study. Polymethylmethacrylate (PMMA) plates with parameters: -10 Dpt myopic ablation and 6.5 mm optical zone were used as a target for photoablation during the calibration of excimer lasers. Energy load and temperature rise were measured with high accuracy infrared thermometer.
Results. Logarithmically rising temperature was measured for both lasers. Maximal temperature measuredwas 48°C for the Allegretto laser and 43°C for the Amaris laser.
Conclusions. Higher energy load with smaller repetition rate causes higher thermal load. Thermal load of the PMMA plate during the ablation is dependent on the environmental conditions, such as temperature, humidity, air flow, smoke plume evacuation, etc.
Introduction
The accuracy of the excimer lasers used in refractive surgery is critical, considering the short- and long-term refractive results and wound healing. There is great demand to make the procedure faster and causing less discomfort for the patient, and, consequently, for the technical development of instruments used. On the other hand, the long-term results and the possible side-effect make it essential to precisely control the physical parameters (energy profile, repetition rate, airflow) of excimer laser during the whole refractive procedure (1, 2). The corneal temperature remains one of the most important parameters to control (3-6).
Before the refractive procedure, a speculum is applied onto the eye of the patient in to keep the eye open as well as to ensure constant temperature of the cornea. The removal of the superficial part of the corneal epithelium or isolation of the flap may change temperature in the eyeball (7).
During the procedure, laser impulses cause the ablation of corneal surface. According our preliminary study, part of the energy is transformed into heat and its amount is dependent on the frequency of the laser, its diameter and energy profile, as well as ablation strategy of the modern flying-spot devices (8). The cornea undergoes dynamic thermal changes during the procedure and exchanges heat with the surrounding tissues, as well as with the environment (9). Aqueous humor circulation causes thermal convection deeper into the eye, and the air flow enabled by laser smoke plume evacuators causes convection to the environment10. The cornea also radiates the heat (10).
In vivo studies examine the maximal temperature of the cornea during the treatment in clinical circumstances, the factors influencing corneal temperature, as well as the effect of corneal temperature on long-term results and wound healing, and the function of the heat-shock proteins (11-13).
In vitro studies frequently use PMMA (polymethylmethacrylate) plates and measure their surface temperature. The plates are also widely used for preoperative testing of the lasers – they serve for the calibration, the comparison of different lasers and their ablation profile, and the investigation of the relationship between the energy and temperature load (14-17).
This study examines the time factor of the temperature rise during excimer laser treatment equal to -10 D myopic refractive treatment on PMMA test plates on two different excimer lasers. Laser smoke plume evacuators were installed and the room conditions were equal to those used in the operating room.
Aim
The aim of this study was to examine the relationship of the temperature of PMMA plates, environmental conditions and the energy load caused by the laser impulses during refractive surgery procedure.
Material and Methods
Two models of excimer lasers were used for this study – Schwind Amaris 500E, operating on 500 Hz frequency, and Allegretto Wavelight, operating on 400 Hz frequency. Both of them were used on factory settings.
Environmental conditions of the room were stable. The temperature was set to 22 ± 1°C and humidity was 35 ± 5%.
Laboratory-calibrated, high accuracy infrared thermometer (EBRO TLC 730, WTW GmbH, Germany) was used to the measure the corneal surface temperature. Accuracy and resolution of the thermometer was 0.1°C. All measurements were obtained from 8 cm distance. The distance (D) and the measured spot size (S) were proportional, with D/S = 8/1. The spot size applied by 8 cm distance was 1 cm, therefore, equal to the size of the photoablation area. The thermometer was stored in the operating room in order to adjust it to the temperature of the environment.
The surface of the PMMA test plate was fitted to the working plane of the laser device. Spheric myopic -10 D surface profile and 6.5 mm optical zone plates were used. Continuous temperature measurement was taken. The results of the measurement were recorded with a video camera.
The output energies of both lasers were measured with calibrated Ophir thermoelectric UV energy meter, equipped with L30Ex measure head.
Results
The energy measured during the procedure with the Wavelight Allegretto laser are shown in figure 1, and with the Schwind Amaris – in figure 2. The repetition rate of the Schwind Amaris laser is 125% higher (500 vs 400 Hz), but the output power of the Wavelight Allegretto is about 180% higher (620 vs 350 mW). Therefore, the procedure time is 140% longer with the Amaris laser (40 vs 29 s).
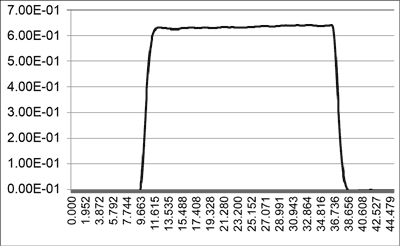
Fig. 1. The energy during the -10 Dpt treatment of the Wavelight Allegretto
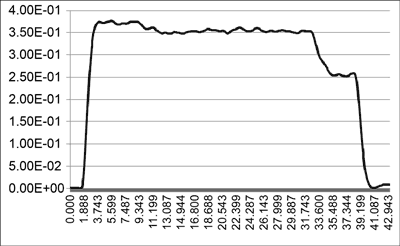
Fig. 2. The energy during the -10 Dpt treatment of the Schwind Amaris
Corneal temperatures measured for both lasers are shown in figure 3. Maximal temperature for both lasers was reached at the end of the procedure and measured 48°C for the Allegretto laser and 43°C for the Amaris laser. The temperature increased faster and higher in the procedure with the Allegretto laser, as it causes bigger thermal load to the material. In spite of this, it must be underlined that the maximum temperature of the PMMA remains under 49-50°C.
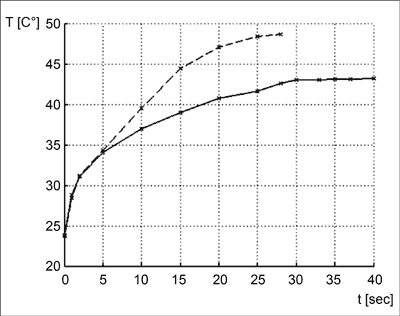
Fig. 3. Temperature changes during -10 Dpt treatment by the Allegretto (dashed line) and the Amaris (solid line)
After performing the one-way ANOVA variance analysis, a statistically significant difference was found regarding the temperature changes among the two laser systems (p < 0.005).
Discussion
An excessively high temperature of the cornea may cause thermal activation and inactivation of different corneal proteins, which may lead to unwanted stromal wound healing, regression of the refractive results and risk of increase of higher order aberrations in the treated eyes (18). Therefore, studying temperature changes is of high practical importance.
According to our preliminary study (8), thanks to the convection of the aqueous humor and the smoke removal system, corneal surface temperature during the procedure did not exceed +40°C. What is important, by this temperature, no heat damage of the corneal collagen and other protein structures is done. On the other hand, other factors (e.g. ultraviolet-B exposure by the sun or solarium after the procedure, genes, etc.) may influence the corneal surface temperature. The metabolic activity of the keratocytes induced by high temperature may cause abnormal wound healing and preventing it is a subject of multiple clinical trials.
PMMA plates are widely used for calibration and comparison of excimer lasers. Earlier studies compared the ablation profile of different excimer lasers during the photoablation of PMMA plates. It was concluded that in spite of a different ablation pattern and a different amount of ablated tissue, same refractive outcomes were achieved (19). In another study, the smoothness of the ablated surface of PMMA plates was examined (20). It has been shown that the smoothness of the treated surface by the modern, flying-spot lasers is satisfying, in contrast to the significantly worse refractive outcomes of the older lasers. Other studies investigate the energy load and thermal load of the PMMA plate in the myopic ablative procedure (21). The importance of the stability of the environmental conditions in the room is proven, and a linear correlation between the ablation depth and the temperature of the surgical environment is indicated. Our study investigated the temperature change of two different modern, flying-spot lasers. In relationship with the environmental conditions, with the airflow and the thermal load caused by the ablation energy, and with the heat conduction in the PMMA plates, the surface temperature rose logarithmically for both lasers. In the same environmental conditions, different energy profiles, local airflow relations and repetition rate determined the PMMA temperature changes. Higher energy caused higher stable temperature level. The impulse energy of the the Schwind Amaris laser is lower than this by the the Wavelight Allegretto laser, which translated to a longer treatment time despite a higher repetition rate.
It must be underlined that the measured temperatures result in the dynamic balance between many factors, but basically depend on the thermal properties of the PMMA material, which is different than thermal properties of the cornea. Therefore, temperature changes of human cornea have different characteristics and must be studied separately (8).
Conclusions
The importance of our results is not the absolute temperature values of the PMMA surfaces, because it can be much higher than the corneal surface, depending on the thermal properties of the material of the PMMA, the ablation profile, the ablation depth, the repetition rate of the laser, and the environmental factors of the room. The continuous (steady) temperature load caused by the stable energy absorption of the laser impulses results in a logarithmically increasing surface temperature. This provides an equilibrium state between the continuous temperature load, the properties of the PMMA plate and the different environmental factors, including the room temperature, humidity and smoke plume evacuation system. These factors might have a significant effect regarding the evolved temperature conditions. Our results suggest the sensitivity of this equilibrium state, which means, that any change of the above mentioned factors may have effect to the evolving surface temperature of the PMMA plate or the cornea.
According to our results, the energy properties of all models of excimer lasers should be tested daily on a proper and identical way to ensure the suggested manufactural settings and to avoid unwanted possible diopter changes (under- or overcorrection) and side effects during the avascular corneal healing phase.
Piśmiennictwo
1. Müller B, Boeck T, Hartmann C: Effect of excimer laser beam delivery and beam shaping on corneal sphericity in photorefractive keratectomy. J Cataract Refract Surg 2004 Feb; 30(2): 464-470. 2. Khoramnia R, Lohmann CP, Wuellner C et al.: Effect of 3 excimer laser ablation frequencies (200 Hz, 500 Hz, 1000 Hz) on the cornea using a 1000 Hz scanning-spot excimer laser. J Cataract Refract Surg 2010 Aug; 36(8): 1385-1391. 3. Arba-Mosquera S, Shraiki M: Analysis of the PMMA and cornea temperature rise during excimer laser ablation. J Mod Opt 2010; 57(5): 400-407. 4. Ishihara M, Arai T, Sato S et al.: Measurement of the surface temperature of the cornea during ArF excimer laser ablation by thermal radiometry with a 15-nanosecond time response. Lasers Surg Med 2002; 30(1): 54-59. 5. Langenbucher A, Seitz B, Kus MM, Naumann GOH: Thermal effects in excimer laser trephination of the cornea. Graefes Arch for Clin Exp Ophthalmol 1996; 234 (suppl.): 142-148. 6. Maldonado-Codina C, Morgan PB, Efron N: Thermal consequences of photorefractive keratoectomy. Cornea 2001; 20: 509-515. 7. Kim MJ, Kim JC, Park WC et al.: Effect of thermal preconditioning before excimer laser photoablation. J Korean Med Sci 2004; 19: 437-446. 8. Szekrenyesi Cs, Sandor G, Gyenes A et al.: Change of corneal surface temperature using different excimer lasers with different repetitive frequency in surface refractive procedures. New Med 2016; 3: 79-83. 9. Dantas PE, Martins CL, de Souza LB, Dantas MC: Do environmental factors influence excimer laser pulse fluence and efficacy? J Refract Surg 2007 Mar; 23(3): 307-309. 10. Bende T, Seiler T, Wollansack J: Corneal thermal gradients. Graefes Arch for Clin Exp Ophthalmol 1988; 226: 277-280. 11. de Ortueta D, Magnago T, Triefenbach N et al.: In vivo measurements of thermal load during ablation in high-speed laser corneal refractive surgery. J Refract Surg 2012 Jan; 28(1): 53-58. 12. Tsubota K, Toda I, Itoh S: Reduction of subepithelial haze after photorefractive keratectomy by cooling the cornea. Am J Ophthalmol 1993; 115: 820-821. 13. Nagy ZZ, Toth J, Nagymihaly A, Suveges I: The role of ultraviolet-B in corneal healing following excimer laser in situ keratomileusis. Pathol Oncol Res 2002; 8(1): 41-46. 14. Gottsch JD, Rencs EV, Cambier JL et al.: Excimer laser calibration system. J Refract Surg 1996 Mar-Apr; 12(3): 401-411. 15. Dorronsoro C, Siegel J, Remon L, Marcos S: Suitability of Filofocon A and PMMA for experimental models in excimer laser ablation refractive surgery. Opt Express 2008 Dec 8; 16(25): 20955-20967. 16. Naroo SA, Charman WN: Surface roughness after excimer laser ablation using a PMMA model: profilometry and effects on vision. J Refract Surg 2005 May-Jun; 21(3): 260-268. 17. O’Neill W, Kapadia P, Thomas T: A study of laser-based removal of polymethylmethacrylate bone cement. J Laser Appl 1996 Jun; 8(3): 149-154. 18. Kasagi Y, Yamashita H: HSP47 expression in cornea after excimer laser photoablation. Jpn J Ophthalmol 2002 Mar-Apr; 46(2): 123-129. 19. Canals M, Elies D, Costa-Vila J, Coret A: Comparative study of ablation profiles of six different excimer lasers. J Refract Surg 2004 Mar-Apr; 20(2): 106-109. 20. Doga AV, Shpak AA, Sugrobov VA: Smoothness of ablation on polymethylmethacrylate plates with four scanning excimer lasers. J Refract Surg 2004 Sep-Oct; 20 (5 suppl.): 730-733. 21. Wernli J, Schumacher S, Wuellner C et al.: Initial surface temperature of PMMA plates used for daily laser calibration to control the predictability of corneal refractive surgery. J Refract Surg 2012 Sep; 28(9): 639-644.


