*Helga Judit Feith1, Boróka Ábrám1, Andrea Szőke1, Erika Tóth2, István Vingender2
Oncological patients’ knowledge of patients’ rights and oncological health care organization
1Department of Social Sciences, Faculty of Health Sciences, Semmelweis University, Budapest, Hungary
Dean: Professor Zoltán Zsolt Nagy, MD, PhD
2Surgical and Molecular Tumour Pathology Centre, National Institute of Oncology, Budapest, Hungary
Director: Professor Miklós Kásler, MD
Summary
Introduction. Neoplastic diseases are the leading cause of death in Hungary nowadays. The number of oncological patients have been increasing for the last decades. In spite of that, the organization of oncological care is still a difficult subject.
Aim. The primary aim of our innovative study was to explore the scope of knowledge of oncological patients and their families about patients’ rights and health care organization. Additionally, our goal was to assess patient’s behaviors and attitudes towards the studied subjects.
Material and methods. 271 patients and family members from two big, outpatient oncology departments (one in Budapest, and another one in the town in the countryside) were enrolled in our study. The participants took part in verbal interview that was based on a pre-set questionnaire. The statistical analysis was conducted with SPSS Statistica 23 software.
Results. Patients with higher level of education tended to know more details concerning their disease and treatment, as well as their rights as patients. In general, the knowledge of health care organization of the participants was poor. Only 39.7% of the respondents indicated that pathologist played an important role in the diagnosis of type of cancer, whereas the same answer was chosen in 89.3% of cases in question inquiring about the role of the oncologist. These results were not influenced by the level of education of the participants. 44.2% of the participants thought that pathologists perform exclusively the postmortem examinations, while 16.8% of the participants could not indicate at all what role pathologists had in diagnosing a neoplasm.
Conclusions. Although all our respondents had active neoplastic disease or their family member was diagnosed with cancer, it has been revealed that: (1) a high percentage of them are not aware of patients’ rights, (2) they are not familiar with the oncological health care organization, which is independent of their level of education. Depending on the level of education, there is a group that does not want to learn patients’ rights at all. In our opinion, better education of patients in these fields would contribute to higher quality of oncological care, and consequently, to better quality of life and health status of oncological patients.
Introduction
According to the statistics by Eurostat from April 2015, the mortality of all malignant tumor reached 361,1 per 100 000 inhabitants in Hungary and 266,9 per 100 000 inhabitants in European Union (1). 28% of deaths in Hungary are caused by malignant tumors, and 28.3% of persons will be diagnosed with neoplasm by the age of 75 (2, 3). Hungary has relatively high morbidity and mortality of malignant tumors when compared with other EU countries (4).
Thanks to the development of new diagnostic and therapeutic tools, it has become possible for the patients to receive personalized oncological therapy. Pathologists are able to give a more detailed diagnosis, which is essential for the choice of an appropriate therapy (5). While the specialization in pathology is, thus, gaining more and more importance, the number of these specialists remains low, resulting in growing workload for the pathologists already working. This results in higher risk of incorrect diagnosis and longer waiting periods for the pathological results. This, in turn, can cause lower satisfaction level of the patients, which in turn can result in legal consequences for health care providers and health workers.
The patient’s rights in Hungary are regulated by the Act CLIV of 1997 on health. The institution advocating patients’ rights was officially launched in Hungary in July 2000 in Hungary, with 54 lawyers employed. Attorneys that defend patients’ laws play an important role in the processing of the complaints. Their role is to assist the patients and their families in formulating the complaints and in further legal proceedings. According to the report issued by patients’ advocates, the number of the patient’s complaints have been growing significantly from that time (6). In 2012, National Centre for Patients’ Rights and Documentation (OBDK) was created. Their annual report of 2015 revealed that 14 080 requests to the patient’s rights advocates arrived, 36% of which were complaints (7). Exact dates are not possible to obtain, because the central register is not able to detect all the violations of the patients’ rights.
After analyzing the patients’ advocates annual report, we conclude that the excessive workload of the health workers contributes to the number of complaints (6). It must be underlined that workload in oncology is unusually high, because of high number of patients (1-4).
Aim
The aim of our study was to explore the scope of knowledge of the patients’ rights (especially right to healthcare, right to refuse healthcare, right to be informed and right to access medical documentation) and health care organization. Additionally, our goal was to assess patient’s behavior and attitudes towards the studied subjects, as well as their past experiences. We analyzed the results to assess the correlation between knowledge of health care and sociodemographic status of the participants.
Material and methods
271 patients and family members from two big, outpatient oncology departments (one in Budapest, and another town in the countryside) were enrolled in our study. The participants took part in verbal interview that was based on a pre-set questionnaire. The authors of the study were the interviewers. Before the beginning of the study, we obtained adequate permissions for the study of the hospitals’ ethical committee. Our research project was conducted in accordance with research ethics. The participants answered the questions voluntarily and their personal data was not recorded. Due to the need of standardization and comparison, as well as due to the fact that our study was a pilot study, we chose to use a structured interview. Our questionnaire contained 66 questions, most of them being close-ended questions, with six open-ended questions. Most of the interviews lasted 20-30 minutes. Most of the participants asked to take part in our study agreed to do so. Women tended to be more open in answering our questions. 271 interviews were performed in total, 121 of which in Budapest (44.6%) and 150 (55.4%) in another town – Miskolc. 66.4% of the participants visited the hospital as outpatients, and 33.6% as accompanying persons. Most of the patients were either in the hospital to get a treatment (41.9%) or on control (32.4%). The majority of the patients (59.4%) visited the hospital at least once a month at the time of the survey. To analyze obtained comparable data, SPSS 22 Statistica software was used. In addition to using distribution tests, the Pearson’s chi-squared test (χ2) was applied to measure bivariate relationships between categorical variables (with alpha < 0.05).
Results
Sociodemographic data
39.5% of the participants were male (N = 107), and 60.5% were female (N = 164). The mean age was 55.9 (SD = 14.1), with the youngest interviewee being 17 years old and the oldest one being 87 years old. The majority of the participants (73.8%) lived in urban areas (22.5% lived in Budapest; N = 61), 26.2% of the participants (N = 71) lived in a town or village. 34.3 of the participants had secondary education (N = 93), 29.2% graduated from vocational schools (N = 79), 23.6% had higher education (N = 64), and 12.9% had primary or incomplete primary education (N = 35). Surprisingly, the level of education did not correlate with the age of the participants (p = 0.290). Statistically, more persons with higher education lived in bigger cities (p < 0.001). 64.2% of all the responders (N = 170) had already had previous oncological patient experiences, 14.7% of the patients (N = 39) declared this was their first time as an oncological patient. Additionally, there were some relatives who had already visited the oncology department as a patient before (31.5% of all relatives, N = 28).
Attitudes towards health care and patients’ rights
84.9% of the responders (N = 225) usually obtained information about their current state of health from their therapists, and most of them thought it was the most reliable source of information (83.3%; N = 215). The second most used information source was the internet (53.4%; N = 141), despite the fact that only 1.9% of the responders (N = 5) declared they believed that the information they could find on the internet was reliable. 37.5% of the responders (N = 99) said that they usually got information about their oncological from physicians other than oncologist, as well as from their oncologist. Higher education and lower age correlated with using the internet as an information source (p < 0.001). 67.2% of persons with higher education (N = 43) and 17.6% of the participants (N = 6) who had primary or incomplete primary education declared to use the internet.
26.1% of the interviewees (N = 70) do not usually get more information about their potential illness neither before nor after the diagnosis. Statistically, higher education level predisposed to getting more information about illness (p < 0.001). A strong correlation was discovered between higher age of the respondent and lower amount of information they get about their health status (p = 0.002; fig. 1).
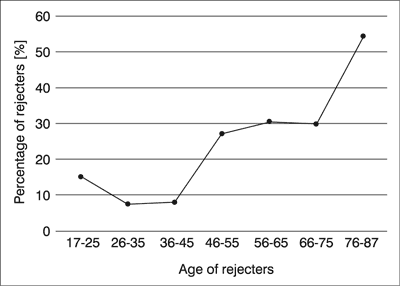
Fig. 1. Percentage of patients that refuse to have more information on their disease by patients’ age (N = 268)
The majority of the responders do not use their right to access medical records, as only 9.0% (N = 19) had asked to see the documentation about any of their previous medical treatment and 1.2% (N = 3) had had it copied for them. 34.7% of the responders (N = 86) were not aware of the fact that they could ask for a copy of their medical records and 18.4% of them did not know that they could access their medical records.
The majority of the interviewees (62.1%; N = 167) never asked for a second opinion on the diagnosis or treatment option. There was a statistically significant correlation between the education and asking for a second opinion (p = 0.004). 20.3% of the participants with higher education (N = 13) always or often asked for a second opinion, while the same was true for only 8.6% of the interviewees with primary or incomplete primary education (N = 3).
93.2% of the participants (N = 248) had never refused any treatment suggested to them, 17 people (6.4%) refused treatment once, and only one person refused pursuing suggested treatment more than once. The gender of the respondents, as well as their previous experiences with the oncology department, did not correlate with the answer to this question. However, persons between 46 and 65 years of age had refused suggested treatment more often than other patients (p = 0.005). It is also interesting to note that persons with primary or incomplete primary education tended to refuse suggested treatment more often (14.7%; N = 5), although the correlation was not statistically significant. The same was true for only 2.2% of the participants (N = 1) with secondary education and 4.7% of the participants with higher education (N = 3).
Patients’ medical knowledge, desire for information and knowledge on health care organization
64.7% of the participants (N = 174) were satisfied with the length and frequency of the medical information given to them and 57.1% (N = 153) were satisfied with how fast the therapy was started and with the choice of the therapy itself (in the light of the results). Women were generally more satisfied with their health care (p = 0.036) and institutional information given to them (p = 0.039). The patients’ reason for discontent was mostly long waiting period (49.4%; N = 133). Patients from Budapest were more likely to be satisfied with the waiting period – 45.3% of them (N = 54) were satisfied with it, while only 17.3% of the respondents (N = 26) from Miskolc were (p < 0.001).
75.0% of the respondents (N = 195) felt they had received adequate information about their health status from their physician. 17.3% of the respondents (N = 45) did not pose their physicians any questions and only 5% of the participants (N = 13) declared they had had no opportunity to do so. While not statistically significant (p = 0.052), a correlation between the answers for this questions and age of the patients was found – young adults were more likely to ask questions, as well as to receive answers. The likelihood of asking questions or receive answers was not influenced by respondents’ gender, level of education or being a patient or patient’s relative.
65.4% of the respondents (N = 174) declared they wanted to learn about their treatment process, whereas 26.7% of the respondents (N = 71) were not interested in it. Respondents from Budapest and with higher education were more likely to be eager to know more about their treatment process (p < 0.001). The age of the participants did not correlate with the answer to this question, however, the respondents aged between 26 and 45 years wanted to have more information more often.
Only 5.2% of the participants (N = 14) requested a second opinion on their histopathological examination. 46.5% of the interviewees (N = 125) were not aware that they could ask for a second opinion. We have examined, why many interviewees have never asked the second opinion. Our hypothesis was that the majority of respondents do not know that it is possible. A clear correlation was found (p = 0.003) between the two variables. Only 25.6% of the respondents (N = 65), who have never asked for a secondary medical diagnosis replied that, they think it is possible to request a second opinion.
Most of the respondents were not familiar with the term ”targeted therapy”. 33.8% of them (N = 90) did not know what it meant, 18.4% (N = 49) believed that it was another name for cancer treatment, such as radiotherapy or chemotherapy. All in all, more than half of the interviewees did not have adequate knowledge in this area. The answers were influenced by the level of education (p = 0.027), those who answered correctly tended to have higher level of education. The answers were not influenced by the gender, age, previous oncological experience or being patient or patient’s relative.
The whole process of cancer treatment depends on the correct diagnosis, therefore, many of our questions focused on this field of oncological care. Most of our interviewees (60.3%; N = 158) thought that pathologist did not participate in the oncological diagnostic process, and 89.3% (N = 234) indicated the oncologist as the physician who made the diagnosis. Answers to other questions seem to confirm this lack of knowledge about pathologist’s responsibilities. When asked about a specialization that is most important in the diagnostic process, 57.5% of the participants (N = 150) indicated the oncologist, 18.4% – other specialists (N = 48), and only 16.5% (N = 43) – the pathologist. In both of the questions discussed above, the answers were not influenced by gender, level of education, previous oncological experience or being a patient or patient’s relative.
More than four out of five interviewees (84.3%; N = 226) were not able to or only partly able to describe the scope of pathologists’ responsibilities. Only 15.7% (N = 42) could give an accurate answer, which consisted of two elements: disease diagnosis, histopathological diagnosis and performing post-mortem examination. Less than half of the respondents (41.0%; N = 110) knew that histopathological diagnosis was made by a pathologist (fig. 2). The answers depended on the age of the interviewees (p = 0.005). Middle-aged interviewees (36-55 years old) tended to answer the question more correctly than younger (35 years old and youngers) and older participants (56 years old or older). The answer to this question was not influenced by the level of education or previous oncological experience.
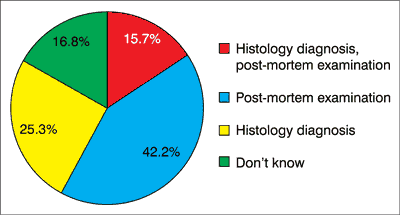
Fig. 2. Responsibilities of the pathologist, answers given by the participants (%) (N=268)
Our last question concerned the willingness of the patient to cooperate (tab. 1). 64.8% of the participants (N = 116) declared they always cooperate with their physician in all the aspects of the treatment. Women were more likely to cooperate than men (p = 0.001), but were also more open to alternative therapies.
Tab. 1. Patients compliance with physician’s recommendations (N = 179)
| Statement | Answers | Results |
| Total | Male | Female |
| I comply with physician’s suggestions concerning lifestyle, diet, medication, etc. | Yes, in all cases | 64.8% | 55.7% | 70.7% |
| Usually | 24.6% | 35.7% | 17.4% |
| Yes, but sometimes I prefer alternative therapies | 8.3% | 2.9% | 11.9% |
| Not really | 1.7% | 4.3% | 0.0% |
| No, I do not want to make changes in my life because of my illness | 0.6% | 1.4% | 0.0% |
Conclusions
Our most important conclusion is that many patients do not exercise their patient’s right provided by the Hungarian Act on Health, despite the fact that the patients’ rights regulation is well known to the Hungarian patients (8, 9).
According to our analysis, most of the patients do not pose questions concerning their condition or try to look for information about it on their own, as they prefer to rely on their physician instead. They tend not to ask for a second opinion on the diagnosis, are not familiar with the targeted therapy, as well as with the process of oncological diagnosis itself. According to another research conducted in Hungary (8), one third of patients feel that they have been adequately informed, and one quarter of the respondents could not name a single patient’s right. From our study, it can be concluded that the lack of knowledge (e.g. a significant number of our participants were not aware that they could access their medical documentation) is only part of the problem, as patients are also not interested in exercising their rights (e.g. significant number of our participants did not want to learn more about their treatment process).
Most of the results described above correlate with patients’ level of education. It can be concluded that participants with higher education were more aware of their rights. Several papers examined the relationship between low social status and less favorable health status (10, 11). The results of our study show that lack of knowledge on patients’ right granted by the Act on Health can make establishing the diagnosis difficult. Lower social status and lack of knowledge put many patients at a particular disadvantage in the field of health care.
Despite the fact that all of the respondents had been directly exposed to neoplastic disease, either as a patient or as a relative, there is clear evidence that many of them do not exercise patients’ rights, and, regardless of their education, they are not familiar with the organization of oncological health care. Depending on their education, some of the participants did not want to learn about it at all. Only a small percentage of respondents requested second opinion on their histopathological examination despite the importance of second opinion in preventing diagnostical errors. Most of the interviewees thought the pathologist had no role in establishing the cancer diagnosis. Although the educational level was a predictive factor in most questions (second opinion, getting information, etc.), it was not the case for questions concerning the responsibilities of the pathologist.
In our opinion, better education of patients in these fields would contribute to higher quality of oncological care, and consequently, to better quality of life and health status of oncological patients. After this pilot study, further studies in related subjects are planned.
Piśmiennictwo
1. Eurostat: Causes of death – standardized death rate, 2012 (per 100 000 inhabitants); http://ec.europa.eu/eurostat/statistics-explained/index.php/File:Causes_of_death_%E2%80%94_standardised_death_rate,_2012_%28per_100_000_inhabitants%29_YB15.png (accessed: 2.09.2016). 2. A haláloki struktúra változása Magyarországon, 2000-2012; https://www.ksh.hu/docs/hun/xftp/idoszaki/pdf/halalokistruk.pdf. 3. Cancer Index: Hungary Cancer Statistics 2012; http://www.cancerindex.org/Hungary (accessed: 2.09.2016). 4. World Cancer Research Fund International: Data on specific cancers; http://www.wcrf.org/int/cancer-facts-figures/data-specific-cancers (accessed: 2.09.2016). 5. Tímár J: A patológiai diagnosztika jelentősège a daganatos betegsègek szemèlyre szabott orvoslásában. Magyar Onkológia 2013; 57: 26-32. 6. Betegjogi, Ellátottjogi ès Gyermekjogi Közalapítvány Tíz èves a betegjogi kèpviselet. 2010; http://www.jogvedok.hu/www/kozalapitvany/10evesabetegjogikepviselet/lay/articles/show/107/10_eves_ a_betegjogi_kepviselet (accessed: 2.09.2016). 7. National Center for Patients’ Rights and Documentation: Report 2015. [Országos Betegjogi, Ellátottjogi, Gyermekjogi ès Dokumentációs Központ Beszámoló 2015]. http://www.obdk.hu/UserFiles/obdk_2015__evi_beszamolo.pdf (accessed: 2.09.2016). 8. Páthy-Dencső B: Betegjogi kutatás 2009. TÁRKI; http://www.tarki.hu/adatbank-h/kutjel/pdf/b280.pdf (accessed: 2.09.2016). 9. Betegjogi, ellátottjogi ès gyermekjogi kutatás 2013. http://www.obdk.hu/UserFiles/betegjogi__ellatottjogi__gyermekjogi_kutatas_2013.pdf. 10. Parikh S, Brennan P, Boffetta P: Meta-analysis of social inequality and the risk of cervical cancer. Int J Cancer 2003; 105: 687-691. 11. Woods LM, Rachet B, Coleman MP: Origins of socio-economic inequalities in cancer survival: a review. Ann Oncol 2006; 17: 5-19.

