Jaroslaw Marczuk1, Michal Pruc2, Zuzanna Wisniewska2, Wladyslaw Gawel3, Hubert Olszewski2, *Lukasz Szarpak2
The cost analysis and the assessment of intoxicated patients in the Emergency Unit of the Child Jesus Clinical Hospital in Warsaw in 2013
Analiza kosztów a ocena pacjentów w stanie nietrzeźwości w Szpitalnym Oddziale Ratunkowym Szpitala Klinicznego Dzieciątka Jezus w Warszawie w 2013 roku
1Polish Society of Disaster Medicine, Warsaw, Poland
2Lazarski University, Warsaw, Poland
3Student’s Scientific Association of Children’s Diabetology, Medical University of Silesia in Katowice, Poland
Streszczenie
Wstęp. Pacjent pod wpływem alkoholu stanowi duże wyzwanie diagnostyczne zarówno w warunkach przedszpitalnych, jak i szpitalnych. Jest również dużym obciążeniem dla systemu ochrony zdrowia z uwagi na konieczność wykonywania wysokospecjalistycznych procedur diagnozowania, w tym tomografii komputerowej.
Cel pracy. Celem pracy była ocena pacjentów pod wpływem alkoholu leczonych w Szpitalnym Oddziale Ratunkowym Szpitala Klinicznego Dzieciątka Jezus w Warszawie w 2013 roku.
Materiał i metody. Badanie przeprowadzono na podstawie analizy dokumentacji medycznej 519 pacjentów leczonych w ramach SOR-u, którzy byli pod wpływem alkoholu. W badaniu uwzględniono: dane socjodemograficzne, skalę GCS, doznane urazy oraz dokonano analizy kosztów leczenia pacjentów będących w stanie nietrzeźwości per capita.
Wyniki. Analiza statystyczna wykazała korelację pomiędzy stężeniem alkoholu a skalą świadomości Glasgow (R = -0.339, P < 0,001). 45,9% pacjentów pod wpływem alkoholu nie posiadało ubezpieczenia zdrowotnego. Osoby nieposiadające ubezpieczenia zdrowotnego miały istotnie statystycznie wyższe poziomy stężenia alkoholu aniżeli osoby posiadające ubezpieczenie (2,57 ± 1,07 vs. 2,97 ± 1,16 ‰; P < 0,001). Najczęstszymi rozpoznaniami u osób będących pod wpływem alkoholu leczonych w ramach SOR-u były: tępe urazy głowy (30,8%), zatrucie alkoholem (22,7%) oraz rany cięte głowy (17,2%).
Wnioski. Urazy głowy to najczęstsze rozpoznanie stwierdzane u pacjentów pod wpływem alkoholu leczonych w ramach SOR-u, wymagające kosztownych procedur diagnostycznych i generujące najwyższe koszty dla oddziału.
Summary
Introduction. Intoxicated patients are the major diagnostic challenge both in pre-hospital and in-hospital environment. They are also a serious cost burden for the healthcare system due to the necessity of performing the highly specialized diagnostic procedures, including computer tomography.
Aim. The aim of our study was the assessment of intoxicated patients who were treated in the Emergency Unit of Child Jesus Clinical Hospital in Warsaw in 2013.
Material and methods. The study was based on the medical records of 519 intoxicated patients who were treated in the Emergency Unit of the hospital. The study included: sociodemographic status, the Glasgow Coma Scale (GCS) score, sustained injuries and the per capita cost analysis for an intoxicated patients.
Results. Statistical analysis showed a correlation between blood alcohol content and GCS scoring (R = -.339, P < 0.001). 45.9% of intoxicated patients did not have health insurance. People who did not have health insurance had statistically significant higher levels of blood alcohol content than those who had insurance (2.57 ± 1.07 vs. 2.97 ± 1.16 ‰, P < 0.001). The most common diagnosis, among intoxicated people who were treated in the hospital’s Emergency Unit, included blunt head trauma (30.8%), alcohol poisoning (22.7%), and cut wounds of the head (17.2%).
Conclusions. Head trauma is the most common diagnosis found in intoxicated patients who are treated in the hospital’s Emergency Unit, requiring costly diagnostic procedures and therefore generating the highest costs for the ward.

INTRODUCTION
Each year, intoxicated patients are admitted to the emergency units (EU) in Poland. For most of them this is a one-time situation, however there is also a group of patients for whom it is an established part of life (1, 2). These patients most often are brought in by Medical Rescue Teams, who are dispatched to a patient under the influence of alcohol or other drugs (3, 4). In Poland, there is still a lack of clear legal regulations that would comprehensively describe the rules of hospitalization of intoxicated people. The hospital and mostly all of the Emergency Department personnel (mainly an admitting doctor) cannot refuse hospitalization of an intoxicated person, who is brought in by the police or the Medical Rescue Team, until they carry out a basic diagnosis which will allow for ruling out the immediate life threatening condition of said person. Personnel and people who work in the hospitals are more and more often becoming victims of aggression while performing examination of this kind of special patient (5). Knowing that the patient is drunk with alcohol does not release the personnel from the proper examination of the patient, carrying out the tests or the necessary diagnosis and obliges to pay special attention, because especially in mental disorders, it is difficult to unambiguously assess whether there is an underlying mental illness requiring hospitalization or the behavior is the result of excessive alcohol consumption (6, 7). It should also be noted that, when a patient is admitted in the EU, the doctor or the coordinator of the triage may decide on the use of so-called “use of force”, which means that such patients might be hospitalized without their consent. This regulation applies to the people who: pose a threat to themselves, others or public safety, violently damage objects in their surroundings or interrupt with the functioning of the hospital (8, 9). When an intoxicated person shows such symptoms, the doctor should not only decide to not refuse the admission, but first and foremost should determine whether these symptoms are the result of a mental illness or abuse of alcohol alone (6, 10). Acting according to the rules of examination and diagnosis of the patient will ensure his safety, however we cannot forget about ensuring the safety of the personnel who works in the hospital (11). The number of intoxicated patients who are admitted to EU is growing and changes depending on the place and days of the week. The majority of alcohol intoxicated patients are treated within EU around the weekend days and in the large cities. Intoxicated patients account for over 10% of all patients admitted to the EU.
AIM
The aim of our study was the assessment of intoxicated patients who were treated in the Emergency Unit of Child Jesus Clinical Hospital in Warsaw in 2013.
MATERIAL AND METHODS
This study was based on the retrospective analysis of medical records of the patients who were admitted to the EU of the Child Jesus Clinical Hospital in Warsaw. After gaining the approval of ethics board of Warsaw Medical University and the approval of the Hospital Management the analysis of intoxicated patients, who were admitted to the EU of this hospital from 1st January 2013 until 31st December 2013, was performed.
We assessed the following variables: sex, age, hour and day of the admission to the EU, reason for hospitalization, degree and level of injuries, mechanism of injury, comparison of Glasgow Coma Scale based on the records from Medical Rescue Teams as well as further procedures with the patient. Additionally, an analysis of the costs of treatment of intoxicated patients per capita was performed.
RESULTS
The characteristics of the study group
The study included 624 intoxicated patients who received treatment in the EU. Among women the largest group was aged 17-30, which amounted for 48.51%. For men the largest group was in the age of 31-51, which amounted for 49.16%.
There was a statistically significant correlation between the amount of alcohol in the body and the GCS score (R = -0.339; P < 0.001) (fig. 1). There were no statistically significant differences between amount of alcohol and occurrence of injuries (2.77 ± 1.28 vs. 2.75 ± 1.03‰; P = 0.768) (fig. 2). The study revealed a high statistical significance between a probability of traumatic patient and blood alcohol content. Among the traumatic men, 36.94% were people whose blood alcohol content was between two and three promil. The non-traumatic patients with the same amount blood alcohol content accounted for 25.81%. The blood alcohol content ranging from three and four promil accounted for 32.8% of non-traumatic patients and 23.83% of traumatic patients. The total number of trauma patients is 333 and not-traumatic is 186. Among women, the results are evenly distributed and do not show statistically significant variability. Among the most common diagnoses within analyzed patients were: blunt head trauma (30.8%), alcohol poisoning (22.7%), cut wounds of the head (17.2%). A detailed list of diagnoses within the analyzed group is shown in figure 3.
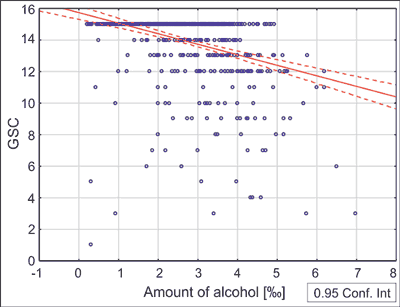
Fig. 1. Simple linear regression analysis (Pearson) between GCS and amount of alcohol
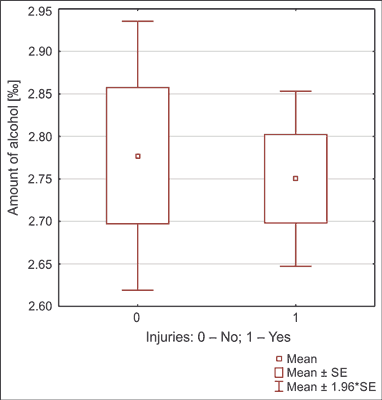
Fig. 2. Univariate comparison of amount of alcohol and the occurrence of injuries
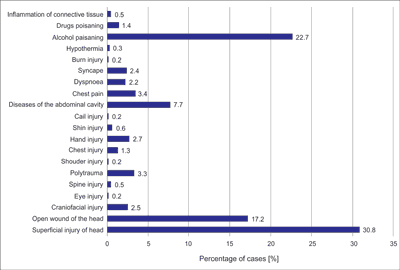
Fig. 3. Characteristics of diagnoses
In the analyzed group of patients, no statistically significant differences were found between a GCS score and occurrence of injuries (14 ± 2 vs. 14 ± 2; P = 0.939) (fig. 4). A vast majority of patients without insurance are found in the age group of 31-55. 52.36% of all uninsured patients are found in this age group. Among men the age group 31-55 was the largest and amounted for around 50% of all men.
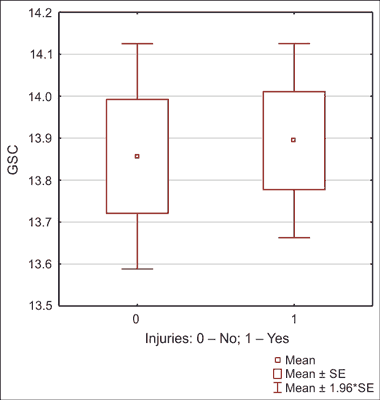
Fig. 4. Univariate comparison of GCS and the occurrence of injuries
There were statistically significant differences between amount of alcohol in the body and having insurance (2.57 ± 1.07 vs. 2.97 ± 1.16‰; P < 0.001) (fig. 5).
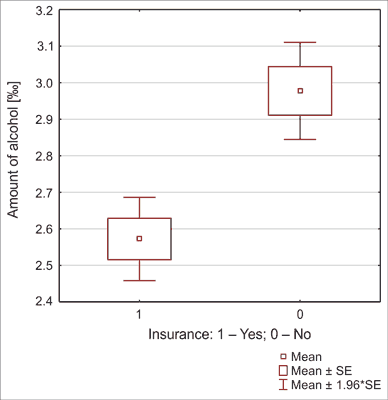
Fig. 5. Univariate comparison of amount of alcohol and the insurance
Powyżej zamieściliśmy fragment artykułu, do którego możesz uzyskać pełny dostęp.
Mam kod dostępu
- Aby uzyskać płatny dostęp do pełnej treści powyższego artykułu albo wszystkich artykułów (w zależności od wybranej opcji), należy wprowadzić kod.
- Wprowadzając kod, akceptują Państwo treść Regulaminu oraz potwierdzają zapoznanie się z nim.
- Aby kupić kod proszę skorzystać z jednej z poniższych opcji.
Opcja #1
29 zł
Wybieram
- dostęp do tego artykułu
- dostęp na 7 dni
uzyskany kod musi być wprowadzony na stronie artykułu, do którego został wykupiony
Opcja #2
69 zł
Wybieram
- dostęp do tego i pozostałych ponad 7000 artykułów
- dostęp na 30 dni
- najpopularniejsza opcja
Opcja #3
129 zł
Wybieram
- dostęp do tego i pozostałych ponad 7000 artykułów
- dostęp na 90 dni
- oszczędzasz 78 zł
Piśmiennictwo
1. Boyle AA, Martin MS, Ahmed H et al.: Changing epidemiology of assault victims in an emergency department participating in information sharing with police: a time series analysis. Emerg Med J 2018; pii: emermed-2017-207087. DOI: 10.1136/emermed-2017-207087.
2. Kool B, Buller S, Kuriyan R et al.: Alcohol and injury among attendees at a busy inner city New Zealand emergency department. Injury 2018; 49(4): 798-805.
3. Vanschoenbeek GM, Hautekiet T, Calle S et al.: Alcohol-related emergency department admissions in an elderly population. Acta Clin Belg 2018 Jun 19: 1-6. DOI: 10.1080/17843286.2018.1482039.
4. McNicholl B, Goggin D, O’Donovan D: Alcohol-related presentations to emergency departments in Ireland: a descriptive prevalence study. BMJ Open 2018; 8(5): e021932.
5. Egerton-Warburton D, Gosbell A, Moore K et al.: Alcohol-related harm in emergency departments: a prospective, multi-centre study. Addiction 2018; 113(4): 623-632.
6. Andrews CM, Westlake M, Wooten N: Availability of Outpatient Addiction Treatment and Use of Emergency Department Services Among Medicaid Enrollees. Psychiatr Serv 2018; 69(6): 729-732.
7. Rodrigues M, Pontes T, Almeida J et al.: Alcohol use in adolescence: 5 years admissions at a pediatric emergency department. Int J Adolesc Med Health 2018 Apr 13. pii: /j/ijamh.ahead-of-print/ijamh-2017-0166/ijamh-2017-0166.xml. DOI: 10.1515/ijamh-2017-0166.
8. Park JH, Park JO, Ro YS et al.: Effect of alcohol use on emergency department length of stay among minimally injured patients based on mechanism of injury: multicenter observational study. Clin Exp Emerg Med 2018; 5(1): 7-13.
9. Klein LR, Martel ML, Driver BE et al.: Emergency Department Frequent Users for Acute Alcohol Intoxication. West J Emerg Med 2018; 19(2): 398-402.
10. Weber CD, Schmitz JK, Garving C et al.: The alcohol-intoxicated trauma patient: impact on imaging and radiation exposure. Eur J Trauma Emerg Surg 2018 Mar 22. DOI: 10.1007/s00068-018-0945-4.
11. Li K, Ochoa E, Vaca FE et al.: Emerging Adults Riding With Marijuana-, Alcohol-, or Illicit Drug-Impaired Peer and Older Drivers. J Stud Alcohol Drugs 2018; 79(2): 277-285.
12. Ngo QM, Eisman AB, Walton MA et al.: Emergency Department Alcohol Intervention: Effects on Dating Violence and Depression. Pediatrics 2018 Jun 5. pii: e20173525. DOI: 10.1542/peds.2017-3525.
13. Di Castelnuovo A, Costanzo S, Bagnardi V et al.: Alcohol dosing and total mortality in men and women: an updated meta-analysis of 34 prospective studies. Arch Intern Med 2006; 166(22): 2437-2445.
14. Martel ML, Klein LR, Lichtenheld AJ et al.: Etiologies of altered mental status in patients with presumed ethanol intoxication. Am J Emerg Med 2018; 36(6): 1057-1059.
15. Noel GN, Roch AR, Michelet PM et al.: Impact of the EURO-2016 football cup on emergency department visits related to alcohol and injury. Eur J Public Health 2018; 28(3): 434-436.
16. United States Centers for Disease Control and Prevention Excessive drinking is draining the U.S. economy; https://www.cdc.gov/features/costsofdrinking/. Atlanta, GA 2017.
17. Teasdale G, Maas A, Lecky F et al.: The Glasgow Coma Scale at 40 years: standing the test of time. Lancet Neurol 2014; 13(8): 844-854.
18. Rundhaug NP, Moen KG, Skandsen T et al.: Moderate and severe traumatic brain injury: effect of blood alcohol concentration on Glasgow Coma Scale score and relation to computed tomography findings. J Neurosurg 2015; 122(1): 211-218.
19. Sperry JL, Gentilello LM, Minei JP et al.: Waiting for the patient to “sober up”: Effect of alcohol intoxication on glasgow coma scale score of brain injured patients. J Trauma 2006; 61(6): 1305-1311.
20. Szarpak L, Madziala M: Epidemiology of cranio-cerebral injuries in emergency medical services practice. Pol Przegl Chir 2011; 83(12): 646-651.
21. Gómez-Restrepo C, Gómez-García MJ, Naranjo S et al.: Alcohol consumption as an incremental factor in health care costs for traffic accident victims: evidence in a medium sized Colombian city. Accid Anal Prev 2014; 73: 269-273.
22. Gómez-Restrepo C, Naranjo-Lujan S, Rondón M et al.: Latin American Clinical Epidemiology Network Series – Paper 6: The influence of alcohol in traffic accidents and health care costs of it in Bogotá-Colombia. J Clin Epidemiol 2017; 86: 106-110.





