Jolanta Majer1, Jacek Smereka2, Jerzy R. Ladny3, Marek Dabrowski4, Mateusz Puslecki4, Agata Dabrowska4, Michael Czekajlo5, Dominika Dunder6, *Lukasz Szarpak5, 6
Quality of chest compressions during cardiopulmonary resuscitation performed by physicians: do we need to use mechanical chest compression devices? A multicenter, randomized, crossover study
JakoŇõńá kompresji klatki piersiowej podczas resuscytacji krńÖŇľeniowo-oddechowej prowadzonej przez lekarzy: czy potrzebujemy mechanicznej kompresji klatki piersiowej? Badanie wielooŇõrodkowe, randomizowane, krzyŇľowe
1Polish Society of Disaster Medicine, Warsaw, Poland
2Department of Emergency Medical Service, Wroclaw Medical University, Poland
3Department of Emergency Medicine, Medical University of Bialystok, Poland
4Department of Rescue Medicine, Poznan University of Medical Sciences, Poland
5Hunter Holmes MCGuire VAMC, Center for Simulation and Healthcare Innovation, Richmond, Virginia, USA
6Lazarski University, Warsaw, Poland
Streszczenie
Wstńôp. Prowadzenie wysokiej jakoŇõci resuscytacji krńÖŇľeniowo-oddechowej stanowi istotny element wpŇāywajńÖcy na powr√≥t spontanicznego krńÖŇľenia. Wytyczne resuscytacji krńÖŇľeniowo-oddechowej kŇāadńÖ duŇľy nacisk na wysokiej jakoŇõci kompresjńô klatki piersiowej.
Cel pracy. Celem pracy byŇāo okreŇõlenie jakoŇõci kompresji klatki piersiowej wykonywanej z systemem i bez systemu kompresji klatki piersiowej LifeLine ARM podczas symulowanej resuscytacji krńÖŇľeniowo-oddechowej wykonywanej przez lekarzy.
MateriaŇā i metody. W randomizowanym, krzyŇľowym badaniu symulacyjnym udziaŇā wzińôŇāo 75 lekarzy. Uczestnicy wykonywali 2-min cykl resuscytacji, z systemem i bez systemu mechanicznej kompresji klatki piersiowej LifeLine ARM. Cykle wykonywane byŇāy w 4 scenariuszach: (A) manualna kompresja w standardowym cyklu 30 uciŇõnińôńá klatki piersiowej do 2 oddech√≥w ratowniczych, (B) manualna cińÖgŇāa kompresja klatki piersiowej, (C) resuscytacja z wykorzystaniem LifeLine ARM w cyklu 30 uciŇõnińôńá klatki piersiowej do 2 oddech√≥w ratowniczych, (D) resuscytacja z wykorzystaniem LifeLine ARM w cyklu kompresji cińÖgŇāej. Protok√≥Ňā randomizowany, krzyŇľowy badania zostaŇā zaakceptowany przez Radńô ProgramowńÖ Polskiego Towarzystwa Medycyny Katastrof.
Wyniki. GŇāńôbokoŇõńá kompresji klatki piersiowej w przypadku badanych scenariuszy byŇāa zr√≥Ňľnicowana i wynosiŇāa odpowiednio: 44 mm (IQR: 38-46) dla scenariusza A, 47 mm (IQR: 43-48) dla scenariusza B, 51 mm (IQR: 50-52) dla scenariusza C oraz 51 mm (IQR: 50-53) dla scenariusza D. CzńôstotliwoŇõńá uciŇõnińôńá klatki piersiowej w poszczeg√≥lnych scenariuszach wynosiŇāa odpowiednio: 129 (124-133), 125 (119-128), 101 (100-101), 101 (100-101), odpowiednio dla scenariuszy A, B, C i D. Odsetek niepeŇānej relaksacji klatki piersiowej wynosiŇā 71% (IQR: 55-79) dla scenariusza A, 63% (IQR: 51-69) dla scenariusza B, 0% (IQT: 0-1) dla scenariuszy C i D.
Wnioski. JakoŇõńá manualnej kompresji klatki piersiowej wykonywanej przez lekarzy podczas symulowanej resuscytacji osoby dorosŇāej jest mniejsza aniŇľeli w przypadku zastosowania systemu kompresji klatki piersiowej LifeLine ARM, odpowiednio w odniesieniu do mediany czńôstoŇõci kompresji klatki piersiowej, gŇāńôbokoŇõci kompresji oraz stopnia relaksacji klatki piersiowej.
Summary
Introduction. The quality of cardiopulmonary resuscitation is an important element influencing the return of spontaneous circulation. Guidelines for cardiopulmonary resuscitation put a great emphasis on high quality chest compression.
Aim. The aim of the study was to assess the quality of chest compressions performed with and without the Lifeline ARM mechanical chest compression device during simulated cardiopulmonary resuscitation performed by physicians.
Material and methods. The randomized cross-over simulation study involved 75 physicians. They performed 2-min cardiopulmonary resuscitation cycles, with and without the use of the Lifeline ARM mechanical chest compression system, in 4 scenarios: (A) manual chest compressions with a standard cycle of 30 compressions: 2 rescue breaths; (B) continuous chest compressions; (C) resuscitation with the Lifeline ARM in cycles of 30 chest compressions: 2 rescue breaths; (D) resuscitation with the Lifeline ARM with continuous chest compressions.
A randomized cross-over controlled simulation study was performed, whose protocol was approved by the Institutional Review Board of the Polish Society of Disaster Medicine (approval No.: 23/09/2017.IRB).
Results. The depth of chest compressions with different test scenarios varied and amounted to 44 mm (IQR: 38-46) for scenario A, 47 mm (IQR: 43-48) for scenario B, 51 mm (IQR: 50-52) for scenario C, and 51 mm (IQR: 50-53) for scenario D. The frequency of chest compressions during research scenarios varied and amounted to 129 (124-133) vs. 125 (119-128) vs. 101 (100-101) vs. 101 (100-101) CPM (Scenario A, B, C, D, respectively). The percent of chest compressions with incomplete release varied and amounted to 71% (IQR: 55-79) for scenario A, 63% (IQR: 51-69) for scenario B, 0% (IQR: 0-1) for scenarios C and D.
Conclusions. The quality of manual chest compressions performed by physicians during simulated adult resuscitation is lower than that of chest compressions with the Lifeline ARM device with reference to the median chest compression rate, median chest compression depth, and percent of chest compressions with incomplete release.

INTRODUCTION
Sudden cardiac arrest is among the most serious health problems in both Europe and the United States and remains associated with very high mortality and morbidity (1, 2). As indicated by Atwood et al. (3), as well as by Luc et al. (4), there are approximately 420,000 out-of-hospital cardiac arrests occurring in the United States and 275,000 in Europe each year. The survival rate of patients with sudden cardiac arrest is low and varies with regard to whether the cardiac arrest occurred in the pre-hospital or hospital setting. A study by Luc et al. (5) included 84,625 hospitalized patients with cardiac arrest; a short-term patient survival to discharge from hospital was only 22.3%. Ofoma et al. (5) indicated the survival rate of patients with in-hospital cardiac arrest of 18.6%, and also demonstrated that the survival was significantly lower in those who arrested during off-hours compared with on-hours (16.8 vs. 20.6%).
In pre-hospital cardiac arrest, the patients’ survival rate is lower, and, as indicated in studies performed by Nakanishi et al. (6) and Lindner et al. (7), the average survival rate for discharging people from pre-hospital cardiac arrest equals 3-25%. This is related to the fact that pre-hospital cardiac arrest often leads to a delay in the initiation of basic life support procedures, and advanced life support procedures are usually implemented only after the arrival of the emergency medical team, in contrast to in-hospital settings, where they are started nearly immediately after cardiac arrest occurrence (8).
The ability to perform cardiopulmonary resuscitation is among the basic skills that should be possessed by medical personnel, including physicians, nurses, and paramedics (9). The process of developing and implementing recommendations for resuscitation dates back to the 1950s (10); however, during the latest decades, guidelines for cardiopulmonary resuscitation are issued every 5 years by the European Resuscitation Council (ERC) and the American Heart Association (AHA) (11, 12). The current resuscitation guidelines for both children and adults emphasize minimizing interruptions in chest compressions as a key factor affecting resuscitation effectiveness and thus the return of spontaneous circulation (11, 12). According to the current guidelines, high-quality chest compressions are characterized by an appropriate frequency of 100-120 compressions per minute (CPM), a corresponding compression depth of 50-60 mm, as well as complete chest relaxation after each compression. Performing chest compressions in this way determines the most effective perfusion pressure and increases the chances for the return of spontaneous circulation.
According to many studies, though, the quality of resuscitation – even performed by medical personnel – is often insufficient (13). Paramedics perform chest compressions exceeding the recommended maximum rate and not reaching the recommendation for chest compression depth.
There are several types of medical equipment supporting cardiopulmonary resuscitation quality, starting from resuscitation feedback devices (14), to mechanical chest compression devices (15). Although the current guidelines do not recommend the routine use of mechanical chest compression systems during cardiopulmonary resuscitation, the systems application is allowed in situations of prolonged cardiopulmonary resuscitation, inability to perform high quality chest compressions, or patient transport.
An example of such a device is the Lifeline ARM (ARM; Defibtech, Guilford, CT, USA) mechanical chest compression device. It has been designed to perform chest compressions owing to the movements of the piston that compress the chest, so it is possible to standardize the compressions parameters in accordance with the current guidelines for adult resuscitation (12, 16). The device is equipped with an intuitive control panel, enabling to carry out cardiopulmonary resuscitation in two modes: standard 30 chest compressions: 2 rescue breaths, or continuous chest compressions without interruptions for rescue breaths (fig. 1a, b).

Fig. 1a, b. Lifeline ARM: (a) the mechanical chest compression device; (b) the control panel
AIM
The aim of the study was to assess the quality of chest compressions performed with and without the Lifeline ARM mechanical chest compression device during simulated cardiopulmonary resuscitation performed by physicians.
MATERIAL AND METHODS
Study design and selection of participants
A randomized cross-over controlled simulation study was performed, whose protocol was approved by the Institutional Review Board of the Polish Society of Disaster Medicine (approval No.: 23/09/2017.IRB). The study was carried out in Warsaw, Poznan, and Wroclaw, between October 2017 and May 2018, among physicians participating in basic life support courses based on the AHA 2015 resuscitation guidelines.
After obtaining a voluntary written informed consent from each participant, 77 physicians were qualified for the study. Among the inclusion criteria, there was practicing the medical profession and voluntary participation in the study. The exclusion criteria consisted of specialization in anesthesiology or emergency medicine, as well as pain in the wrist or back. The total of 75 participants completed the survey; 2 withdrew during the study course because of wrist pain.
Cardiopulmonary resuscitation training
Before the start of the study, all participants successfully completed training in basic life support procedures conducted by accredited AHA instructors. After the training, physicians were instructed on the use of the Lifeline ARM mechanical chest compression system. Then, they had 5 minutes to familiarize with the device.
Simulation scenarios
In order to simulate a patient with cardiac arrest requiring cardiopulmonary resuscitation, an adult SimMan 3G simulator (Laerdal, Stavanger, Norway) was used. During the study, the participants performed cardiopulmonary resuscitation in teams consisting of 2 persons. One was responsible for replacement breaths and the other applied chest compressions; after the end of a 2-minute cycle, the roles changed. Then, each participant had a 20-minute break before performing resuscitation based on a different scenario.
The study participants performed cardiopulmonary resuscitation based on 4 scenarios:
a) Scenario A – cardiopulmonary resuscitation with manual chest compressions with a standard cycle of 30 compressions: 2 rescue breaths.
b) Scenario B – cardiopulmonary resuscitation with continuous chest compressions. For this purpose, an independent instructor performed endotracheal intubation allowing for asynchronous resuscitation.
c) Scenario C – cardiopulmonary resuscitation performed with the Lifeline ARM chest compression system in cycles of 30 chest compressions: 2 rescue breaths.
d) Scenario D – cardiopulmonary resuscitation performed with the Lifeline ARM mechanical chest compression system for continuous chest compressions. For this purpose, as in scenario B, the simulator was intubated, allowing continuous chest compressions without interruptions for rescue breaths.
During all scenarios, the simulator was placed on a flat floor in a well-lit room.
The order of the study participants and the research scenarios was random. The physicians were divided into 4 groups with the use of the Research Randomizer program (randomizer.org). The randomization procedure is shown in detail in figure 2.
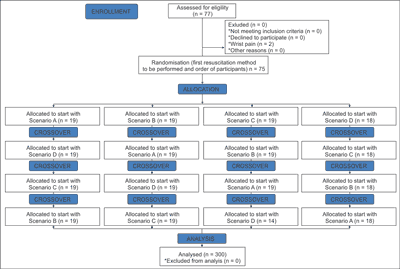
Fig. 2. Randomization flow chart
Data collection and measure quality of chest compression
During the study, only the data concerning the quality of chest compressions automatically recorded by the software controlling the simulator were analyzed.
The primary outcome of the trial was chest compression depth. The appropriate depth was defined as 50-60 mm, and the appropriate chest compression rate as 100-120 CPM, in accordance with the AHA guidelines (16). We also evaluated the no-flow time. In addition, after performing the resuscitation scenarios, the study participants were asked for their self-assessment of the rescuer’s fatigue. The assessment was provided in a 100-point visual analog scale (VAS), where 1 meant no fatigue, and 100 stood for extreme fatigue. The participants were also asked to indicate their attitudes towards the use of mechanical chest compression systems during real resuscitation activities.
Statistical analysis
On the basis of previous studies, we calculated the necessary sample size as at least 54 participants using G*Power 3.1 (two-tailed t-test; Cohen’s d – 0.8; alpha error – 0.05; power – 0.95). In order to increase the power of the study, we decided to qualify 75 participants.
PowyŇľej zamieŇõciliŇõmy fragment artykuŇāu, do kt√≥rego moŇľesz uzyskańá peŇāny dostńôp.
Mam kod dostńôpu
- Aby uzyskańá pŇāatny dostńôp do peŇānej treŇõci powyŇľszego artykuŇāu albo wszystkich artykuŇā√≥w (w zaleŇľnoŇõci od wybranej opcji), naleŇľy wprowadzińá kod.
- WprowadzajńÖc kod, akceptujńÖ PaŇĄstwo treŇõńá Regulaminu oraz potwierdzajńÖ zapoznanie sińô z nim.
- Aby kupińá kod proszńô skorzystańá z jednej z poniŇľszych opcji.
Opcja #1
29 zŇā
Wybieram
- dostńôp do tego artykuŇāu
- dostńôp na 7 dni
uzyskany kod musi byńá wprowadzony na stronie artykuŇāu, do kt√≥rego zostaŇā wykupiony
Opcja #2
69 zŇā
Wybieram
- dostńôp do tego i pozostaŇāych ponad 7000 artykuŇā√≥w
- dostńôp na 30 dni
- najpopularniejsza opcja
Opcja #3
129 zŇā
Wybieram
- dostńôp do tego i pozostaŇāych ponad 7000 artykuŇā√≥w
- dostńôp na 90 dni
- oszczńôdzasz 78 zŇā
PiŇõmiennictwo
1. Berdowski J, Berg RA, Tijssen JG et al.: Global incidences of out-of-hospital cardiac arrest and survival rates: systematic review of 67 prospective studies. Resuscitation 2010; 81(11): 1479-1487.
2. Freund B, Kaplan PW: A review of the utility of a hypothermia protocol in cardiac arrests due to non-shockable rhythms. Cardiol J 2017; 24(3): 324-333.
3. Atwood C, Eisenberg MS, Herlitz J et al.: Incidence of EMS-treated out-of-hospital cardiac arrest in Europe. Resuscitation 2005; 67(1): 75-80.
4. Luc G, Baert V, Escutnaire J et al.: Epidemiology of out-of-hospital cardiac arrest: a French national incidence and mid-term survival rate study. Anaesth Crit Care Pain Med 2018; pii: S2352-5568(18)30068-7.
5. Ofoma UR, Basnet S, Berger A et al. for the American Heart Association Get with the Guidelines – Resuscitation Investigators: Trends in survival after in-hospital cardiac arrest during nights and weekends. J Am Coll Cardiol 2018; 71(4): 402-411.
6. Nakanishi N, Nishizawa S, Kitamura Y et al.: The increased mortality from witnessed out-of-hospital cardiac arrest in the home. Prehosp Emerg Care 2011; 15(2): 271-277.
7. Lindner TW, Søreide E, Nilsen OB et al.: Good outcome in every fourth resuscitation attempt is achievable – an Utstein template report from the Stavanger region. Resuscitation 2011; 82(12): 1508-1513.
8. Treptau J, Ebnet J, Akin M et al.: Angiographic detection of fatal acute aortic dissection Stanford type A under resuscitation. Cardiol J 2016; 23(6): 620-622.
9. Telec W, Klosiewicz T, Zalewski R et al.: Chain of survival used for a victim of sudden cardiac arrest in a public place. Disaster Emerg Med J 2017; 2(3): 135-136.
10. Aitchison R, Aitchison P, Wang E et al.: A review of cardiopulmonary resuscitation and its history. Dis Mon 2013; 59(5): 165-167.
11. Monsieurs KG, Nolan JP, Bossaert LL et al.: European Resuscitation Council Guidelines for Resuscitation 2015: Section 1. Executive summary. Resuscitation 2015; 95: 1-80.
12. Neumar RW, Shuster M, Callaway CW et al.: Part 1: Executive Summary: 2015 American Heart Association Guidelines Update for Cardiopulmonary Resuscitation and Emergency Cardiovascular Care. Circulation 2015; 132(18 suppl. 2): 315-367.
13. Abelairas-Gómez C, Barcala-Furelos R, Szarpak L et al.: The effect of strength training on quality of prolonged basic cardiopulmonary resuscitation. Kardiol Pol 2017; 75(1): 21-27.
14. Kurowski A, Szarpak L, Bogdanski L et al.: Comparison of the effectiveness of cardiopulmonary resuscitation with standard manual chest compressions and the use of TrueCPR and PocketCPR feedback devices. Kardiol Pol 2015; 73(10): 924-930.
15. Szarpak L, Filipiak KJ, Ladny JR et al.: Should nurses use mechanical chest compression devices during CPR? Am J Emerg Med 2016; 34(10): 2044-2045.
16. Kleinman ME, Brennan EE, Goldberger ZD et al.: Part 5: Adult Basic Life Support and Cardiopulmonary Resuscitation Quality: 2015 American Heart Association Guidelines Update for Cardiopulmonary Resuscitation and Emergency Cardiovascular Care. Circulation 2015; 132(18 suppl. 2): S414-435.
17. Pakula RJ, Wanat S: CPR in terms of maritime search and rescue service working conditions. Disaster Emerg Med J 2017; 2(2):104-105.
18. Ewy GA, Zuercher M: Role of manual and mechanical chest compressions during resuscitation efforts throughout cardiac arrest. Future Cardiol. 2013; 9(6): 863-873.
19. Chen J, Lu KZ, Yi B et al.: Chest compression with personal protective equipment during cardiopulmonary resuscitation: a randomized crossover simulation study. Medicine (Baltimore) 2016; 95(14): 1-6.
20. Smereka J, Szarpak L, Smereka A et al.: Evaluation of new two-thumb chest compression technique for infant CPR performed by novice physicians. A randomized, crossover, manikin trial. Am J Emerg Med 2017; 35(4): 604-609.
21. Mayrand KP, Fischer EJ, Ten Eyck RP: A simulation-based randomized controlled study of factors influencing chest compression depth. West J Emerg Med 2015; 16(7): 1135-1140.
22. Lampe JW, Tai Y, Bratinov G et al.: Developing a kinematic understanding of chest compressions: the impact of depth and release time on blood flow during cardiopulmonary resuscitation. Biomed Eng Online 2015; 14: 102.
23. Fox J, Fiechter R, Gerstl P et al.: Mechanical versus manual chest compression CPR under ground ambulance transport conditions. Acute Card Care 2013; 15(1): 1-6.
24. Wang PL, Brooks SC: Mechanical versus manual chest compressions for cardiac arrest. Cochrane Database Syst Rev 2018; 8: CD007260.
25. Iskrzycki L, Smereka J, Rodriguez-Nunez A et al.: The impact of the use of a CPRMeter monitor on quality of chest compressions: a prospective randomised trial, cross-simulation. Kardiol Pol 2018; 76(3): 574-579.
26. Ladny JR, Smereka J, Rodr√≠guez-N√ļñez A et al.: Is there any alternative to standard chest compression techniques in infants? A randomized manikin trial of the new “2-thumb-fist” option. Medicine (Baltimore) 2018; 97(5): 1-6.
27. Truszewski Z, Szarpak L, Kurowski A et al.: Randomized trial of the chest compressions effectiveness comparing 3 feedback CPR devices and standard basic life support by nurses. Am J Emerg Med 2016; 34(3): 381-385.
28. Smereka J, Kaminska H, Wieczorek W et al.: Which position should we take during newborn resuscitation? A prospective, randomised, multicentre simulation trial. Kardiol Pol 2018; 76(6): 980-986.
29. Field RA, Yeung J, O’Carroll D et al.: Chest compressions in the emergency department: rate does not have to compromise compression depth. Resuscitation 2013; 84(1): e13-14.
30. Truszewski Z, Szarpak L, Kurowski A et al.: Mechanical chest compression with the LifeLine ARM device during simulated CPR. Am J Emerg Med 2016; 34(5): 917.
31. Wieczorek W, Kaminska H: Impact of a corpuls CPR Mechanical Chest Compression Device on chest compression quality during extended pediatric manikin resuscitation: a randomized crossover pilot study. Disaster Emerg Med J 2017; 2(2): 58-63.
32. Aufderheide TP, Pirrallo RG, Yannopoulos D et al.: Incomplete chest wall decompression: a clinical evaluation of CPR performance by EMS personnel and assessment of alternative manual chest compression-decompression techniques. Resuscitation 2005; 64(3): 353-362.
33. Gohier F, Dellimore KH, Scheffer C: Development of a real-time feedback algorithm for chest compression during CPR without assuming full chest decompression. Resuscitation 2014; 85(6): 820-825.
34. Smereka J, Szarpak L, Rodr√≠guez-N√ļñez A et al.: A randomized comparison of three chest compression techniques and associated hemodynamic effect during infant CPR: a randomized manikin study. Am J Emerg Med 2017; 35(10): 1420-1425.
35. Yannopoulos D, McKnite S, Aufderheide TP et al.: Effects of incomplete chest wall decompression during cardiopulmonary resuscitation on coronary and cerebral perfusion pressures in a porcine model of cardiac arrest. Resuscitation 2005; 64(3): 363-372.
36. Kurowski A, Hryniewicki T, Czyzewski L et al.: Simulation of blind tracheal intubation during pediatric cardiopulmonary resuscitation. Am J Respir Crit Care Med 2014; 190(11): 1315.
37. Tranberg T, Lassen JF, Kaltoft AK et al.: Quality of cardiopulmonary resuscitation in out-of-hospital cardiac arrest before and after introduction of a mechanical chest compression device, LUCAS-2; a prospective, observational study. Scand J Trauma Resusc Emerg Med 2015; 23: 37.
38. Putzer G, Braun P, Zimmermann A et al.: LUCAS compared to manual cardiopulmonary resuscitation is more effective during helicopter rescue – a prospective, randomized, cross-over manikin study. Am J Emerg Med 2013; 31(2): 384-389.
39. Czekajlo M, Dabrowska A: In situ simulation of cardiac arrest. Disaster Emerg Med J 2017; 2(3): 116-119.
40. Majer J, Jaguszewski MJ, Frass M et al.: Does the use of cardiopulmonary resuscitation feedback devices improve the quality of chest compressions performed by doctors? A prospective, randomized, cross-over simulation study. Cardiol J 2018 Aug 29. DOI: 10.5603/CJ.a2018.0091.


