© Borgis - New Medicine 3/2006, s. 74-78
Małgorzata Malicka, Anna Zakrzewska, Danuta Gryczyńska
Homeopathic therapy in recurrent respiratory diseases in childhood
Medical University Department of Paediatric Otorhinolaryngology
Head of Department: Prof. Danuta Gryczyńska, MD, PhD
Summary
Summary
Recurrent respiratory infections are a serious health problem in childhood. The influence factors are: immaturity of immunological system, children spending time in day care centres, and environmental factors. In the case of recurrent infections many parents would like to treat their children with homeopathic medicines rather than antibiotics. The aim of the following study is to estimate the effectiveness of homeopathic therapy.
Introduction
Upper respiratory tract infections are among the most common respiratory system diseases in children. They must be considered not only as a health problem but also in a social context. The group most often affected is infants. As children grow older, infections become less frequent [1, 6]. In preschoolers more than 5 infections a year are referred to as a recurrent problem.
The most significant influence factor in younger children is that their mechanisms of general and local immunity are not fully developed. Another important cause is children spending time in day care centres (nurseries, kindergartens and schools). Finally, there are environmental agents such as living conditions, pollution and passive smoking [5].
The organism´s defence against infection is connected with activating mechanisms of local and general immunity. Mechanisms of systemic immunity lead to identifying antigens, cytokine synthesis and producing specific antibodies, which destroy microorganisms [4, 7, 9]. Local immunity mechanisms include mechanical barriers and peripheral lymphatic organs.
Upper respiratory tract proper function is associated with the defensive and purifying role of pseudostratified ciliated columnar epithelium and mucus produced by goblet cells and secreting cells. Most columnar epithelial cells are covered with cilia 5-7 mm long. On one cell there are about 50 to 200 cilia. At the temperature of the human body cilia move with a frequency of about 12-20 times per second in a two-phase cycle (fast and slow), shifting the thick outer layer of mucus. Movements of cilia on several neighbouring cells are coordinated metachromatically and this causes slight delays of movement phases in adjacent cells. This phenomenon, called mucociliary transport, is one of the most important respiratory tract defence mechanisms.
Mucus covering nasal cavities and sinuses is a liquid mixture of secretions from different cells. It consists of two layers: watery, low viscosity sol, which surrounds the cilia, and the upper viscous gel layer, which is transported along the tips of the cilia.
Sol contains fewer glycoproteins but more proteins and molecules. The more viscous gel contains acid and neutral glycoproteins, which trap and absorb particles and bacteria. In mucus there are found immunoglobulins, the most important of which is IgA, neutralizing pathogens. IgA blocks attachment of pathogens to mucosal surfaces and prevents them from entering the tissues. Immunoglobulin G, produced locally and transported from blood serum, is the major antibody fighting microorganisms. IgE, which increases in atopic reactions, is present in healthy humans in respiratory mucosal secretion in small quantities. Mucus also conveys enzymes such as lactoferin and lysozyme, which are antibacterially active, and albumin reacting with glycoproteins and thus regulating its rheological properties [10, 11, 12].
Systemic defensive mechanisms are divided into non-specific reactions (natural, innate) and specific reactions (acquired, adaptive). Non-specific reactions are a direct defence against infection – skin barrier, mucous membranes, complement protein system, natural antibodies IgM and fagocytic and cytotoxic cells. Their role is to reduce the number of pathogens immediately, which is significant for the course of infection [13, 16].
Acquired immunity is immunity acquired upon exposure to a specific pathogen, particularly in the course of an infection/disease or through successful vaccination. It depends on the presence and proper function of cells which identify and present the antigen to competent lymphocytes T and B [7, 9]. When the number of pathogens is large enough for induction of an adaptive response, specific immune reactions are activated (cellular and humoral).
Immediate humoral reaction is a process initiated at the first contact with the allergen, in which antibodies are produced and immunologic memory of the antigen is generated. Delayed humoral reaction, thanks to memory cells, is more dynamic – antibodies appear in the blood serum very quickly and in greater concentration.
Cellular immunity is connected with T lymphocytes, which produce intercellular inflammatory mediators. Like B cells, T lymphocytes have T cell receptors on their cell surfaces. They recognize antigens and through their clonal expansion trigger production of effector cells and creation of immunological memory. Helper T lymphocytes also activate cytotoxic T-cells, which play a vital role in virus infections [1, 2, 14].
Today it is known that derangements of the immune system cause many various diseases and that possibilities of their treatment are closely associated with modification of immune cell behaviour [3, 4].
Background
Recurrent upper respiratory tract infections are among the highest incident diseases in childhood. They mostly occur in preschool children and cause children´s absence in kindergartens and their parents´ sick leaves. Recurrent infections tend to prolong and often cause chronic rhinosinusitis in children and laryngopharyngitis in older children and adults.
Conventional treatment does not always prevent recurrence of the problem. That is why patients willingly use homeopathic and herbal medicines. These medicines increase phagocytic abilities of neutrophilic granulocytes and trigger an immunomodulative effect. This may support anti-inflammatory treatment, improve the body´s self-defence and consequently reduce the risk of rhinosinusitis.
Objective
The objective of this study was to test the homeopathic medicine Sinuspax in children with recurrent upper respiratory tract infections with following complications in the form of rhinosinusitis.
Materials
The study was conducted on 80 children, aged 3-14 years (divided into 2 groups: 3-7 years, 7.1-14 years), who reported to the Laryngological Outpatient Clinic with acute rhinitis and headaches lasting longer than 10 days. Patients fulfilling the criterion of more than 5 upper respiratory tract infections a year, followed by rhinitis lasting 2-3 weeks after recovery, were qualified to the studied group.
Rhinosinusitis was diagnosed if at least 3 of the following symptoms lasted longer than 10 days:
– runny nose
– nasal mucosal congestion
– cough
– headache
– fatigue
Criteria excluding patients from the study:
– allergies of upper respiratory tract
– ongoing oral or nasal steroid therapy
– immunomodulative treatment
– drug intolerance.
Trial Group.
| | Group I (3-7 y.) | Group II (7.1-14 y.) |
| Girls | 14 | 19 |
| Boys | 26 | 21 |
| Total | 40 | 40 |
Control Group.
| | Group III (3-7 y.) | Group IV (7.1-14 y.) |
| Girls | 7 | 7 |
| Boys | 8 | 8 |
| Total | 15 | 15 |
Children with allergies, children treated with immunomodulative medicines within the 6 weeks before the study and children with abnormalities of the nasal septum and wing of the nostril (revealed by laryngological examination) were excluded from the study.
Two study groups were created. The first group received Sinuspax orally for 3 months: 3 x 1 pill for younger children and 3 x 2 pills for older children. The second, control group, comprised 30 children of comparable ages, who were treated with antibiotics and adjuvant drugs.
Method
The children qualified as adequate were included in the studied group. The control group consisted of children at the comparable age who were treated in accordance with the standard methods of treatment in case of prolonged rhinosinusitis.
The children with prolonged rhinosinusitis were included in the study group. In those children there were intensifying headaches which required diagnostic radiology examination in order to exclude the presence of inflammatory fluid in the maxillary sinus. Occipito-mental roentgenogram with Water´s method was carried out. In the group of the examined children there were 2 children from the older group in whom the fluid was found. Sinus puncture was carried out and antibiotic therapy was included.
All children enrolled in the study were carefully interviewed regarding their medical history and current problems. General paediatric and laryngological examinations were carried out. Changes of nasal cavities were assessed in anterior and posteriori rhinoscopy. Where necessary, an X-ray picture of the nasal sinuses was made.
The study was performed according to the schedule: a preliminary visit, 2 control visits at 1-month intervals and 1 visit after 6 months, including laryngological and laboratory examination.
Immunological parameters, total IgE and interferon-gamma were measured during the preliminary visit and after 3 months of treatment.
In the case of acute infection with fever a child was treated with adjuvant homeopathic medicines: L.-52 (drops) and Voxpax (pills). If there was no improvement, antibiotic treatment was administered.
Results
2 children from the younger group revealed medicine intolerance. It was manifested in profuse nasal secretion running down the throat, irritating it and making eating and breathing difficult. These children were excluded from the study.
In 3 children from the younger group and 2 children from the older group high level of IgE, on both first and second examination, was recorded. These children were excluded from further study and recommended deeper diagnostics.
Further study was carried out in the remaining children, their age and sex groups being shown below:
In all children from the study and control group mucopurulent secretion was present, and in 4 children from group I and 18 children from group II profuse purulent secretion in nose cavities. 6 children from the older group had radiograms of nasal sinuses done before the visit. 4 of these children prior to the study had sinus puncture or Proetz sinus irrigation done.
In 8 children from group I parents observed excessive sleepiness and lack of previous activity during the day. 24 children from the older group reported fatigue and exhaustion and 20 children reported frontal headaches.
Dry cough becoming a nuisance was reported by 24 children from the older group. Parents of all 35 children from the younger group observed a cough described as either dry or moist. Despite Sinuspax treatment 10 children from the younger group and 14 children from the older group were diagnosed with acute upper respiratory tract infection and/or laryngitis. These children were prescribed L-52 and Vox-pax, according to the procedure of the study. Blood serum level of interferon-gamma before and after treatment is shown below:
The level of total serum IgE in examined children is shown in Table 2.
| | Group I (3-7 years) | Group II (7,1-14 years) |
| Girls | 12 | 18 |
| Boys | 23 | 20 |
| Total | 35 | 38 |
Table 1. Interferon-gamma level.
| | Up to 7 years | More than 7 years | Compared |
| B | K | B | K | < 7 years | > 7 years |
| Before treatment | 0,06 | 1,00 | 1,60 | 0,19 | | |
| ? 0.06 | ? 2.16 | ? 3.38 | ? 0.17 | p > 0.05 | p > 0.05 |
| 0.06 | 0.3 | 0.36 | 0.25 | | |
| After treatment | 0.71 | 0.36 | 0.15 | 0.31 | | |
| ? 1.64 | ? 0.45 | ? 0.09 | ? 0.09 | p > 0.05 | p < 0.05 |
| 0.28 | 0.21 | 0.15 | 0.36 | | |
| compared | p < 0.05 | p > 0.05 | p > 0.05 | p > 0.05 | - | - |
Table 2. IgE level.
| | Up to 7 years | More than 7 years | Compared |
| B | K | B | K | < 7 years | > 7 years |
| Before treatment | 35.64 | 36.79 | 35.09 | 24.27 | | |
| ? 28.67 | ? 33.96 | ? 28.07 | ? 10.79 | p > 0.05 | p > 0.05 |
| 25.44 | 24.50 | 28.57 | 22.33 | | |
| After treatment | 17.78 | 44.00 | 32.60 | 37.50 | | |
| ? 12.96 | ? 21.59 | ? 31.88 | ? 17.47 | p < 0.05 | p > 0.05 |
| 14.88 | 42.70 | 22.60 | 39.30 | | |
| compared | p < 0.05 | p > 0.05 | p > 0.05 | p = 0.05 | - | - |
Disscussion
In all children treated for 3 months with compound homeopathic medicines clinical picture improved, which was manifested in lower frequency of upper respiratory tract infections in parents´ opinion.
Within the first 10 days of treatment slight intensification of symptoms (more secretion in nasal cavities) was recorded, which may be connected with so-called initial exacerbation in homeopathic medicine use. These symptoms disappeared in further treatment. In 2 patients medicine intolerance occurred and medicine was discontinued after a few days.
Immunological parameters analysed before and after 3 months of treatment revealed a statistically significant (p<0.05) fall in IgE concentration in the study group of younger children 4-7 years. No statistically significant changes in the study group of older children or in either control group (p>0.05, p=0.05) were recorded. Statistically significant lower IgE concentration (p <0.05) in the group of younger children before and after Sinuspax treatment was stated. The result was also significant when compared with children in the control group after treatment. In remaining groups there were no statistically remarkable differences.
Serum immunoglobulin IgE, generally connected with atopy, elevates in parasitic diseases and virus or atopic infections with symptoms in the upper respiratory tract. Decreased serum immunoglobulin after 3-month Sinuspax treatment, with allergies and parasitic diseases excluded prior to the study, indicates beneficial effects of this medicine, also in the case of virus infections. They mostly occur in the group of younger children and the relatively short period of the study showed positive differences in this particular group.
Further monitoring led to excluding from the study 3 children from the younger group and 2 from the older group due to elevated IgE on both first examination and after 3 months. Raised IgE level could be the effect of virus infection, but it remained unchanged without infection, so these children were referred to an outpatient Allergology Clinic for further diagnostics.
In the group of younger children after 3-month Sinuspax treatment a statistically significant rise (p <0.05) in interferon-gamma was recorded.
A statistically significant difference was recorded in the group of older children after Sinuspax treatment when compared to children from the control group undergoing traditional treatment, in whom interferon-gamma level was higher.
No statistically significant differences were recorded in the remaining age groups.
Interferon gamma level elevation in children up to 7 years of age, with improvement of health condition (fewer infections, disappearing ailments and symptoms signifying rhinosinusitis) shows the effectiveness of this method. Not only did frequency of recurrent infections decrease, but chronic symptoms of rhinosinusitis were removed and development of acute infections following rhinosinusitis was prevented. Time of treatment shortened to 3-4 days of using symptomatic medicine.
Sinuspax is a compound medicine. It contains such preparations as: Thuya, Calcarea carbonica and Calcarea fluorica, which stimulate lymphoid tissue and may be responsible for immunity stimulation. Other ingredients play mainly a purification role: Kalium sulf., Silicea, Kalium bichromicum [8, 16]. Perhaps the ingredient called Sabadilla – decidedly intensifying mucous membranes´ secretion – caused increased secretion and intolerance in 2 children from the younger group.
Clinical analysis and published laboratory trials suggest that antihomotoxic treatment may be beneficial for the course of virus infection and reduce probability of rhinosinusitis in their course. Lower frequency of respiratory tract infections was recorded as well. These results may indicate improvement of local immune mechanisms function [15].
Patients tolerated treatment well and parents willingly used tested medicines. Other scientific studies confirm the high clinical effectiveness of this treatment and researchers do not find differences in therapy effectiveness between homeopathic and traditional methods [18].
Control examination after 3 months of treatment revealed that symptoms disappeared in all children. Examination after 6 months showed recurrence of infection in 15 children from the younger group and 10 from the older group.
Recurrent respiratory tract infections often imply the necessity of repeated antibiotic treatment. This evokes parents´ reluctance and concern. There are also known incidents of antibiotic discontinuity immediately after acute symptoms disappear.
Homeopathy is an alternative method of treatment and the discussed conditions led the authors to carry out the study in order to prove its effectiveness.
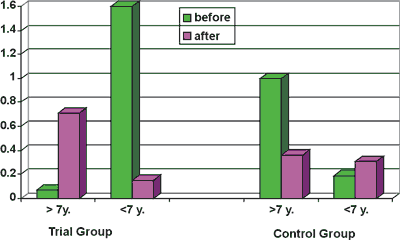
Fig. 1. Different serum level of interferon-gamma in examined children.
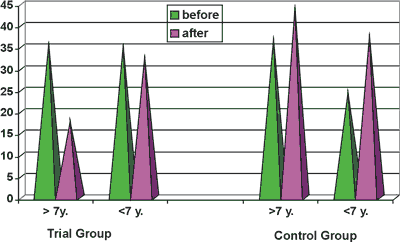
Fig. 2. Different concentrations of serum total IgE in examined children.
CONCLUSIONS
1. Homeopathic treatment causes less symptoms of infections of upper respiratory tracts.
2. Using a homeopathic medicine such as Sinuspax was a well-tolerated method of treatment.
3. Clinical improvement was connected with higher level of interferon-gamma, but only in the group of younger children.
Piśmiennictwo
1. Chmielewska-Szewczyk D.: Choroby infekcyjne układu oddechowego u dzieci. Via Medica, Gdańsk 2001. 2. Dzierżanowska D., Jurkiewicz D., Zielnik-Jurkiewicz B.: Zakażenia w otolaryngologii. Alfa Medica Press, Bielsko Biała 2002. 3.Eriksson K., Holmgern J.: Recent advances in mucosal vaccines and adiuvants. Curr Opin Immunol, 2002, 14, 666-72. 4. Goldschmidt O., Kahn L., Klimek L., et al.: Specific Anti-Infective Immune Therapy. An Effective Way to Treat Reccurent Tonsilltis in Childhood. Drugs. 1977, 1, 38-43. 5.Gryczyńska D., Kobos J., Zakrzewska A.: Relationship between passive smoking, recurrent respiratory tract infections and otitis media in children. Int. J. of Ped. Otorhinolaryng. 1999, suppl. 49, 275-278. 6.Gryczyńska D.: Wybrane zagadnienia z otolaryngologii dziecięcej. Repetytorium z pediatrii, red. Kawalec W., Kubicka K., PZWL, Warszawa 2004. 7. Jędrzejczak W.: Podstawowe zasady immunoterapii Immunoterapia, 1995, 7-8, 391-396. 8.Jouanny Jacques Materia-Medica. Leki homeopatyczne w praktyce medycznej. Editions Boiron, Daimonion, Instytut Wyd., Lublin 1994. 9.Kowalski M.L.: Immunologia Kliniczna. Mediton, Łódź 2000. 10.Kraehenbuhl J.P., Neutra M.P.: Molecular and cellular basis of immune protection of mucosal surfeces. Physiol.Rev. 1992, 72, 853-873. 11.Krzeski A., Janczewski G.: Choroby nosa i zatok przynosowych. Sanmedia, Warszawa 1997. 12.Ligęzińki A.: Postępy w diagnostyce i leczeniu chorób nosa i zatok przynosowych. Medycyna Praktyczna, Kraków 1998. 13.Marchant A., Duchow J., Goldman M.: Adhesion molecules in antibacterial defenses: effects of bacterial extracts. Respiration 1992, 59, 24-27. 14.Osur S.L., Viral: respiratory infection in association with asthma and sinusitis. Ann Allergy Asthma Immunol 2002, 89, 553-60. 15.Pawińska A., Jarosz K.: Immunoprofilaktyka nieswoista w zakażeniach układu oddechowego, Szkoła Interny Kliniki Nowej, 10, 13, 13078-13083. 16.Repetytorium homeopatii, Pryw. Oficyna Wyd. "Planeta", Poznań 1992. 17.Rogues C., Frayret M.N., Luc J., et al.: Immunostimulant effects on granulocyte function during an acute respiratory 8infection. Dev ,Biol, Stand. 1992, 77, 183-187. 18.Wiesenauer . I in Virksamkeitsprüfung von homöopathischen. Kombinations spräparaten bei Sinusitis, Arzneim-Forsch./Drug Res. 39, (I), 5, 1989, 620-25.

