© Borgis - Postępy Nauk Medycznych 7/2017, s. 392-396
*Robert Kijanka1, 2, Michał Ćwiertnia1, 2, Piotr Białoń1, 3, Tomasz Ilczak1, 2, Arkadiusz Stasicki1, 2, Beata Kudłacik1, Monika Chorąży4, Marzena Wojewódzka-Żelezniakowicz5, Adam Jakubowski5, Robert Gałązkowski6, Klaudiusz Nadolny7, 8, Jerzy Robert Ładny5, Łukasz Szarpak9, Rafał Bobiński1
Non-invasive methods of measuring the carboxyhemoglobin level in pre-hospital procedure
Nieinwazyjne metody pomiaru karboksyhemoglobiny w postępowaniu przedszpitalnym
1Institute of Emergency Medicine, Department of Nursing and Emergency Medicine, Faculty of Health Sciences, University of Bielsko-Biała
Head of Institute: Associate Professor Rafał Bobiński, MD, PhD
2Emergency Medical Services in Bielsko-Biała
Head of Services: Wojciech Waligóra
3Department of Emergency Medical Aid, Health Care Center in Żywiec
Head of Department: Antoni Juraszek
4Department of Neurology, Medical University of Białystok
Head of Department: Jan Kochanowicz, MD, PhD
5Department of Emergency Medicine and Disasters, Medical University of Białystok
Head of Department: Professor Jerzy Robert Ładny, MD, PhD
6Department of Emergency Medical Service, Medical University of Warsaw
Head of Department: Grzegorz Michalak, MD, PhD
7Voivodeship Rescue Service in Katowice
Head of Services: Artur Borowicz
8College of Strategic Planning in Dąbrowa Górnicza
Head of College: Anna Rej-Kietla, MD, PhD, LLM
9Department of Emergency Medicine, Medical Univeristy of Warsaw
Head of Department: Zenon Truszewski, MD, PhD
Streszczenie
Tlenek węgla powstaje w wyniku procesów niepełnego spalania węgla, drewna i wielu substancji organicznych przy niedostatecznym dopływie tlenu. Ze względu na właściwości fizyczne wykrycie jego obecności w atmosferze bez zastosowania profesjonalnych urządzeń nie jest możliwe. Czujniki pozwalające potwierdzić obecność CO oparte są na trzech głównych technologiach. Zaliczamy do nich technologię chemooptyczną z zastosowaniem m.in. ogniw Gell, urządzenia wykorzystujące półprzewodniki metalu oraz detektory elektrochemiczne. Podstawowymi metodami pomiaru stężenia karboksyhemoglobiny we krwi są badania laboratoryjne. Alternatywą są urządzenia służące do nieinwazyjnego stwierdzania zatrucia tlenkiem węgla u pacjenta. Metody te polegają na zbadaniu powietrza wydychanego lub na umieszczeniu czujnika na palcu osoby badanej. Wykorzystanie urządzeń służących do bezinwazyjnego stwierdzania zatrucia tlenkiem węgla może być szczególnie korzystne w opiece przedszpitalnej. Wiarygodne przedszpitalne pomiary mogą umożliwić m.in. bezpośredni transport pacjenta do ośrodka zajmującego się leczeniem przy wykorzystaniu komory hiperbarycznej czy segregację medyczną w przypadku zatrucia u większej liczby poszkodowanych. W literaturze dotyczącej bezinwazyjnego pomiaru COHb toczy się dyskusja na temat wiarygodności tego typu pomiarów.
Summary
Carbon monoxide is produced as a result of processes of incomplete combustion of coal, wood and many organic substances with the insufficient supply of oxygen. Due to its physical characteristics detecting the presence of carbon monoxide in atmosphere without applying professional devices is impossible. Detectors allowing for confirming the presence of CO are based on three main technologies. These include the chemo-optical technology applying i.a. Gell cells, devices applying metal semiconductors as well as electrochemical detectors. The basic methods of measuring the concentration of carboxyhemoglobin in the blood are laboratory examinations. An alternative are devices used for non-invasive diagnosing of carbon monoxide intoxication of the patient. These methods consist in examining the exhaled air or in placing a sensor on the examined person’s finger. Applying devices used for non-invasive determining of carbon monoxide intoxication may be particularly beneficial in pre-hospital care. Reliable pre-hospital measurements may allow for i.a. the direct transportation of a patient to a facility enabling treatment applying a hyperbaric chamber or medical segregation in case of the intoxication of a higher number of patients. The literature on the non-invasive measurements of COHb discusses the reliability of this type of measurements.

Carbon monoxide (CO) which is the by-product of the incomplete combustion of coal has accompanied humanity since they learned to use fire. It may be assumed that in the first homes where fireplaces were situated in the central point and smoke used to vent out through an opening in the roof there was a possibility of generating high concentrations of carbon monoxide which could negatively affect the health and life of the inhabitants (1). The first historical mention of the harmful effect of carbon monoxide is attributed to Aristotle who noticed that coal fumes lead to “a heavy head and death” (2).
Carbon monoxide is produced as a result of processes of incomplete combustion of coal, wood and many organic substances with the insufficient supply of oxygen. During proper combustion coal generates combustion gases containing ca. 1% of carbon monoxide while even 30% of CO may be produced in improper combustion conditions (3). Carbon monoxide is an odorless and colorless gas which does not cause the irritation of respiratory tracts, its molecular weight is 28.01 and its density in reference to that of air is 0.967 (4). In the regulation of the Minister of Health dated 28.09.2005 (Journal of Laws No. 201, item 1674) on hazardous substances it has been classified as an extremely flammable gas and a toxic substance which poses a serious threat to human health. In regulations specifying the acceptable limits of CO concentration the occupational exposure limit has been defined as 23 mg/m3 and the short-term exposure limit (STEL) has been defined as 117 mg/m3. Healthcare room standards define the maximum volume in indoor air as 30 mg/m3 within 24 hours and 100 mg/m3 within 30 minutes (4, 5).
A natural source of carbon monoxide in nature is mainly the oxidation of methane in the atmosphere and the releasing of CO from oceans. Other natural sources are fires of forests and of grasses, volcanoes and storms. A contemporary source of human exposure to the harmful effect of carbon monoxide is primarily industrial activity. The most frequent sources of carbon monoxide in industrial conditions are mines and steelworks. Significant concentrations of CO may occur in boiler rooms, especially those with furnaces fired with culm, in car workshops and garages as well as during using various types of burners. Another source of exposure are heating systems. It is estimated that in Poland over a half of the 6 million households using the gas network possesses gas heaters of flow water. Improper use of heating installations, too tight windows and blocking vent grilles results in the lack of airflow into the rooms and thus incomplete combustion of gas and the production of toxic carbon monoxide concentrations (6). The reason for the occurrence of high carbon monoxide concentrations may also be the meteorological situation when during the formation of the so-called inversions the air movement may favor the injecting of combustion gases into flats. The combustion gases which enter the rooms this way contain not only carbon monoxide but also carbon dioxide and other combustion products possessing a specific smell (7).
Carbon monoxide poses a threat in every concentration and due to the difficulty of identifying it, it is often referred to as a “silent murderer”. According to the statistics of the National Fire Service in the years 2010-2015 in Poland there were over 24 000 carbon monoxide incidents as a result of which over 12 000 people were injured and 477 died (fig. 1).
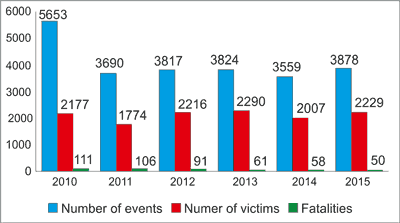
Fig. 1. Carbon monoxide intoxications in the years 2010-2015. Elaborated on the basis of data obtained at http://www.straz.gov.pl
Due to the physical properties of carbon monoxide detecting its presence in atmosphere without applying professional devices isn’t possible. The aim of preventive actions based mainly on conducting informative campaigns is applying home CO detectors. They allow for the early detection of the increased concentration of carbon monoxide. Despite of the widespread availability of home detectors their application still isn’t common, that is why in the heating season there are many cases of exposure to the toxicity of CO which generate the need for the interventions of emergency services. Currently detectors allowing for detecting carbon monoxide in atmosphere constitute standard equipment of units of State Fire Service and of Voluntary Fire Departments. They allow for measuring the concentration level of the gas in the inspected room.
Detectors allowing for confirming the presence of CO are based on three main technologies. These include the chemo-optical technology applying i.a. Gell cells, devices applying metal semiconductors as well as electrochemical detectors (8). Regardless of the technology detecting the presence of carbon monoxide is highly significant due to the toxic effect generated in the human organism even by small concentrations of carbon monoxide. The concentration of the gas in atmospheric air causes the occurrence of symptoms which depend on the time which the intoxicated person spent in the toxic environment. A light headache occurs as a result of a 2-3 hour exposure to the concentration ranging from 100 to 200 ppm (0.01-0.02%). With the concentration 400 ppm (0.04%), a strong headache occurs after 60 minutes of inhalation. The gas concentration at the level of 800 ppm (0.08%) causes dizziness, vomiting and convulsions after 45 minutes, and after two hours it leads to a lasting coma. The concentration which is twice as high – 1600 ppm (0.16%) causes a strong headache, vomiting and convulsions within 20 minutes and within 2 hours it leads to death. Higher concentrations cause the occurrence of worrying symptoms already after a few minutes and death occurs within 3-30 minutes of remaining in an atmosphere containing from 3200 ppm (0.32%) to 12 800 ppm (1.28%) of the toxic gas (tab. 1) (9, 10).
Tab. 1. Symptoms of carbon monoxide intoxication
| Volumetric concentration of CO in the air | Intoxication symptoms |
| 100-200 ppm (0.01-0.02%) | light headache with the exposure for 2-3 hours |
| 400 ppm (0.04%) | a strong headache beginning after ca. 1 hour of inhaling this concentration |
| 800 ppm (0.08%) | dizziness, vomiting and convulsions after 45 minutes of inhalation; after two hours – a lasting coma |
| 1600 ppm (0.16%) | a strong headache, vomiting, convulsions after 20 minutes, death after 2 h |
| 3200 ppm (0.32%) | an intensive headache and vomiting after 5-10 minutes; death after 30 minutes |
| 6400 ppm (0.64%) | a headache and vomiting after 1-2 minutes; death within less than 20 minutes |
| 12 800 ppm (1.28%) | loss of consciousness after 2-3 inhalations; death after 3 minutes |
Source: http://www.straz.gov.pl/data/other/czujniki_tlenku_wegla.pdf (accessed on 14.03.2017)
Powyżej zamieściliśmy fragment artykułu, do którego możesz uzyskać pełny dostęp.
Mam kod dostępu
- Aby uzyskać płatny dostęp do pełnej treści powyższego artykułu albo wszystkich artykułów (w zależności od wybranej opcji), należy wprowadzić kod.
- Wprowadzając kod, akceptują Państwo treść Regulaminu oraz potwierdzają zapoznanie się z nim.
- Aby kupić kod proszę skorzystać z jednej z poniższych opcji.
Opcja #1
29 zł
Wybieram
- dostęp do tego artykułu
- dostęp na 7 dni
uzyskany kod musi być wprowadzony na stronie artykułu, do którego został wykupiony
Opcja #2
69 zł
Wybieram
- dostęp do tego i pozostałych ponad 7000 artykułów
- dostęp na 30 dni
- najpopularniejsza opcja
Opcja #3
129 zł
Wybieram
- dostęp do tego i pozostałych ponad 7000 artykułów
- dostęp na 90 dni
- oszczędzasz 78 zł
Piśmiennictwo
1. Kryteria zdrowotne środowiska: Tlenek węgla. Ministerstwo Zdrowia i Opieki Społecznej. Tom 13. Wydawnictwo Lekarskie PZWL, Warszawa 1987: 24-27.
2. Penney G: The Toxic Twins: Hydrogen Cyanide and Carbon Monoxide, Educational Supplement Sposored by the Cyanide Poisoning Treatment Coalition, March 2009: 1-9.
3. Seńczuk W: Toksykologia. Wydawnictwo Lekarskie PZWL, Warszawa 2002: 520-526.
4. Jakubowski M: Tlenek węgla. Dokumentacja dopuszczalnych wielkości narażenia zawodowego. PiMOŚP 2006; 4(50): 69-92.
5. Kaiser K: Tlenek i dwutlenek węgla w pomieszczeniach. Rynek Instalacyjny 2010; 9; http://www.rynekinstalacyjny.pl/ (dostęp: 15.03.2017).
6. Żurański J: Wentylacja naturalna mieszkań z paleniskiem gazowym a śmiertelne zatrucia tlenkiem węgla. Forum Wentylacyjne 2003. Materiały seminaryjne. Stowarzyszenie Polska Wentylacja, Warszawa 2003: 50-60.
7. Raszeja S: Medycyna sądowa. Wydawnictwo Lekarskie PZWL, Warszawa 1993: 241-245.
8. Wright J: Chronic and occult carbon monoxide poisoning: we don’t know what we’re missing. Emerg Med J 2002; 19: 386-390.
9. Grobelska K, Królikowska A, Zieliński E et al.: Zatrucie tlenkiem węgla – zadania ratownika na miejscu zdarzenia. BiTP 2014; 34(2): 123-132.
10. www.straż.gov.pl (dostęp 14.03.2017).
11. Sieroń A, Cieślar G: Zarys medycyny hiperbaryczncznej. Alfa Medica Press, Bielsko-Biała 2006: 285-287.
12. Kot J, Sićko Z, Michałkiewicz M: Wartość oznaczania karboksyhemoglobiny na podstawie pomiaru stężenia tlenku węgla w powietrzu wydechowym pacjentów z zatruciem tlenkiem węgla w porównaniu z bezpośrednim pomiarem karboksyhemoglobiny we krwi. Med Intens Ratunk 2007; 1(10): 129-134.
13. Hampson N, Piantadosi C, Thom L et al.: Weaver Practice Recommendations in the Diagnosis, Management, and Prevention of Carbon Monoxide Poisoning. Am J Resp Crit Care Med 2012; 11: 1096-1101.
14. Suner S, Partridge R, Sucov A et al.: Non-Invasive Pulse Co-Oximetry Screening in the Emergency Department Identifies Occult Carbon Monoxide Toxicity. J Emerg Med 2008; 34 (4): 441-450.
15. Touger M, Birnbaum A, Wang J et al.: Performance of RAD-57 Pulse Co-Oximeter. Ann Emerg Med 2010; 56(4): 382-388.
16. Physio-Control, Inc.: Instrukcja użytkowania LIFEPAK 15; http://www.physio-control.com (dostęp: 14.03.2017).
17. Hampson NB: Noninvasive Pulse CO-Oximetry Expedites Evaluation and Management of Patients with Carbon Monoxide Poisoning. Am J Emerg Med 2012; 30(9): 2021-2024.
18. Gałązkowski R, Wejnarski A, Baumberg I et al.: Wpływ przedszpitalnego zastosowania nieinwazyjnego pomiaru karboksyhemoglobiny na działania ratunkowe w zdarzeniach mnogich i masowych – opis przypadku. Medycyna Pracy 2014; 65(2): 289-295.
19. Stasicki A, Biela W, Debudaj A et al.: Zatrucie tlenkiem węgla jako zdarzenie o charakterze potencjalnie mnogim lub masowym. Na Ratunek 2016; 6: 12-15.
20. Busch M: Carbon Monoxide Exposure in Norwegian Rescue Helicopters. Air Med J 2015; 34(6): 328-332.
21. Feiner JR, Rollins MD, Sall JW et al.: Accuracy of Carboxyhemoglobin Detection by Pulse CO-Oximetry during Hypoxemia. Anesth Analg 2013; 117(4): 847-858.
22. Van Ginderdeuren F, Van Cauwelaert K, Malfroot A: Influence of digital clubbing on oxygen saturation measurements by pulse-oximetry in cystic fibrosis patients. J Cyst Fibros 2006; 5(2): 125-128.
23. Harlan N, Weaver LK, Deru K: Inaccurate pulse CO-oximetry of carboxyhemoglobin due to digital clubbing: case report. Undersea Hyperb Med 2016; 43(1): 59-61.
24. Roth D, Herkner H, Schreiber W et al.: Accuracy of Noninvasive Multiwave Pulse Oximetry Compared With Carboxyhemoglobin From Blood Gas Analysis in Unselected Emergency Department Patients. Ann Emerg Med 2011; 58(1): 74-79.

