© Borgis - New Medicine 4/2014, s. 142-145
*Konrad Wroński1,2
Medical error in gallbladder cancer treatment – case report, review of literature and legal analysis of the situation
1Department of Oncology, Faculty of Medicine, University of Warmia and Mazury, Olsztyn, Poland
Head of Department: prof. Sergiusz Nawrocki, MD, PhD
2Department of Surgical Oncology, Hospital Ministry of Internal Affairs with Warmia and Mazury Oncology Centre, Olsztyn, Poland
Head of Department: Andrzej Lachowski, MD
Summary
Gallbladder carcinoma is a highly aggressive malignancy. This neoplasm was first time described in 1777. More than 230 years later, the prognosis in gallbladder carcinoma is poor. Appropriate treatment of patients may help to improve the five year survival rate of patients.
Instruments recorded in national and international acts protect the patient against medical mistakes. National legislation requires the physician responsible for providing medical benefits corresponding to current medical knowledge and perform their work with due diligence. It is now one of the most important rights of the patient, which is often not observed by medical personnel.
The author of this article presented the case of a 73-year-old Caucasian woman who was admitted to the hospital because of recurrence of gallbladder carcinoma. Since 11-months of the diagnosis gallbladder cancer, the patient was referred to a specialist outpatient for further oncological treatment. Patient for 11 months were treated conservatively, contrary to current standards of conduct in this stage of the cancer, the implementation of imaging studies, instead of surgery. After 11 months there was observed icterus, weakness and malaise. In CT scan there was recurrence of neoplasm disease. In this article the author present the law consequences that may threaten a doctor who does not treat patient with current medical knowledge.
INTRODUCTION
Galbladder carcinoma is a highly aggressive malignancy (1). This neoplasm was first time described in 1777 (2). More than 230 years later, the prognosis in gallbladder carcinoma is poor (3). Appropriate treatment of patients may help to improve the five year survival rate of patients.
Instruments recorded in national and international acts protect the patient against medical mistakes (4-7). National legislation requires the physician responsible for providing medical benefits corresponding to current medical knowledge and perform their work with due diligence (5, 6). It is now one of the most important rights of the patient, which is often not observed by medical personnel.
CASE REPORT
A 73-year-old Caucasian woman was referred to the Department of Surgical Oncology due to icterus caused by recurrence of gallbladder carcinoma in computer tomography scan (fig. 1). Total bilirubin was 16,47 mg%. The patient suffered from weakness and malaise. The computed tomography scan revealed a significant degree of expansion of intrahepatic bile ducts. In the segment 5 and 6 of the liver in the vicinity of the lodge after the cut gallbladder, revealed poorly demarcated infiltration area measuring approximately 55 x 42 mm (fig. 1). In the 7th liver segment revealed a focal lesion of the characteristics of cysts with a diameter of 19 mm. The common bile duct was extended to 23 mm. Duodenal wall was thickened. Pancreas was without perceptible lesions and expand pancreatic duct. Spleen, adrenals and right kidney were without lesions. Left kidney was small and cirrhotic. Para-aortic lymph node size up to 16 mm.
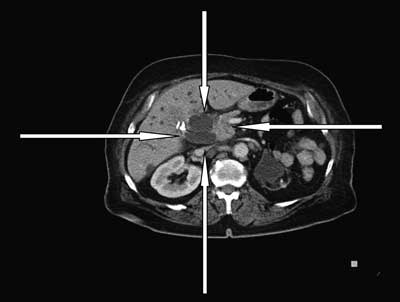
Figure 1. The computed tomography scan showing neoplasm tumor in the lodge after removed gallbladder.
The patient suffered from abdominal pain located in the right hypochondrium. Physical examination showed palpable tumor located in this area. There were no peritoneal symptoms. The external genitalia and uterine cervix were normal.
She had no any other symptoms, there was no history of weight loss and loss of appetite. The patient was treated chronically due to arterial hypertension. She had cholecystectomy 11 months earlier in the Department of General Surgery one of the hospital in the Warmia and Mazury district. Histopathological examination showed adenocarcinoma cells in the wall of gallbladder. It was stage 2 neoplasm disease – perimuscular-tissue invasion (pT2N0M0). General surgeons sent the patient for further treatment to the oncological center. The patient was treated in the outpatient room by consultant of general and oncological surgery. Within 11 months the patient was performed two times ultrasound and once computer tomography. In the computer tomography 1 month after surgery there was no recurrence of neoplasm disease. The patient was not refer to surgery from outpatient room.
Blood test showed elevated levels of the alanine transaminase – 93 U/l (N: 2-33 U/l), the aspartate aminotransferase – 141 U/l (N: 2-32 U/l) and the alkalin phosphatase 418 U/l (N: 35-104 U/l). The rest blood tests were in the normal range.
After watching the CT scans, the case was inoperable. The patient underwent ERCP with incision Vaters papilla and the assumed of the prosthesis to the common bile duct. The patient felt good after treatment and the total bilirubin level gradually decrease. In the 7th day after the ERCP total bilirubin level was 4.95 mg%. The patient was discharged home in the 8th day after treatment in optimal general condition and directed to further palliative treatment to the Department of Chemotherapy.
DISCUSSION
Gallbladder carcinoma is the most frequent tumor of the extrahepatic biliary tract and the fourth commonest malignant neoplasm located in the upper gastrointestinal tract (8, 9). The most frequent histopathologic type of gallbladder carcinoma is adenocarcinoma – 80% of all cases (8, 9).
Patients who had diagnosed „incidental” gallbladder carcinoma on pathological examination of cholecystectomy specimen have significant better prognosis of 5-year survival than patients whose gallbladder cancer was diagnosed preoperatively or at the time of cholecystectomy (8). Patients who undergo radical re-resection after cholecystectomy („incidental” gallbladder carcinoma) have 5-year survival 35-38%, than those who did not undergo radical re-resection – median survival 5 months (10).
In the stage I and II neoplasm disease surgery play important role in treatment. Most cases of T2 gallbladder carcinoma is diagnosed in a routine after cholecystectomy specimen histopathological examination (11). After the histopathological diagnosis of gallbladder cancer in the preparation of routine operational after cholecystectomy patient should be referred to a reference center, where it will be possible radical surgery, preferably within two months (11). The goal of surgery is to perform a radical resection (R0), which are likely to only patients in the first and second stage - about 40% of them may survive 5 years. In the second stage, after cholecystectomy there should be performed surgery with partial resection of the right lobe of the liver (non-anatomical 2 cm resection of the liver - gallbladder bile or anatomic segmentectomy 4B and 5) plus dissection around the hepatoduodenal ligament, as well as histological verification of the cystic duct stump (11).
In the above case, the doctor made the mistake of not sending the patient to reoperation within two months after cholecystectomy. His medical behavior was not in accordance with current medical knowledge and recommendations for diagnostic and therapeutic treatment in malignant tumors published in 2013. Therefore the consultant of general and oncological surgery significant reduced the patient chances for a 5-year survival.
Under Article 8 of the Polish Code of Medical Ethics, every physician ought to perform all necessary diagnostic, therapeutic and prophylactic procedures while exercising due care and devoting an appropriate amount of time (12-14). A similarly information can be found in Article 4 of the Act the Professions of Doctor and Dentist, which states that every physician is obliged to exercise their profession according to current medical recommendations, available methods and means of preventing, diagnosing and treating diseases, in compliance with professional ethical principles and the duty of due care.
CRIMINAL LIABILITY OF PHYSICIANS
Criminal liability of a physician is related to committing a medical error/mistake. The term „medical error” is commonly understood as referring to a conduct (an act or an omission) which contradicts basic and widely recognized principles of contemporary (current) medical knowledge.
Criminal liability for a medical error relies on general principles of liability for offences against life and health. It essentially represents liability for unintentional offences with ensuing criminal consequences (financial effects).
The situation discussed here involves a diagnostic and treatment error. Conservative treatment of the patient in the policlinic was medical mistake. These measures will undoubtedly help to shorten the life of the patient and only palliative treatment. In stage 2 of gallbladder carcinoma, in which the patient was described above, it was a chance to cure or at least a significant degree of prolongation her life time.
Past judicial decisions demonstrate that cases of medical mistake, depending on their effects, are usually classified under the following provisions of the Penal Code:
– Article 155 of the Penal Cod:
„Whoever unintentionally kills a human being shall be subject to the penalty of the deprivation of liberty for a term of between 3 months and 5 years”;
– Article 156 § 2 of the Penal Code:
„Whoever (acting unintentionally) causes grievous bodily harm in a form which:
1) deprives a human being of sight, hearing, speech or the ability to procreate, or
2) causes another serious disability, a severe incurable or prolonged illness, a disease posing a serious threat to life, a permanent mental illness, a permanent total or substantial incapacity to work in an occupation, or a permanent severe bodily disfigurement or deformation shall be subject to the penalty of the deprivation of liberty for a term of up to three years”;
– Article 157 § 3 of the Penal Code:
„Whoever (acting unintentionally) causes an impairment of functioning of a bodily organ or a disturbance of health other than specified in Article 156 § 1, or Whoever (acting unintentionally) causes an impairment of functioning of a bodily organ or a disturbance of health lasting not longer than seven days, shall be subject to a fine, the penalty of restriction of liberty or the penalty of deprivation of liberty for a term of up to one year”.
CIVIL LIABILITY OF PHYSICIANS
In the Article 415 of the Civil Code is written: „Whoever by his fault causes an injury to another person shall be obliged to redress it”.
A physician can be held civilly liable only when the following three prerequisites are cumulatively satisfied:
– a medical error, i.e. an injury-causing event,
– a (material or non-material) injury understood as a detriment to legally protected interests whose occurrence is attributable to the physician,
– a causal relationship between the injury-causing event and the injury.
An important article in the Civil Code is the Article 444, where is written:
㤠1.In the case of a bodily harm or a disturbance of health, the redress of injury shall include all costs arising there from. Upon the request of the injured person, the person obliged to redress the injury shall pay in advance the sum required to cover the costs of medical treatment and, if the injured person becomes disabled, also the sum required to cover the costs of training for an alternative occupation.
§ 2. If the injured person loses, either wholly or partially, the ability to do paid work or if the injured person’s needs increase or their prospects for future success diminish, the injured person may demand from the obliged person an appropriate pension as a means of redressing the injury.
§ 3. If at the time of pronouncing judgment the injury suffered by the injured person cannot be assessed precisely, they can be granted a temporary pension”.
A legal basis for demanding a compensation can be found in Article 445 § 1 of the Civil Code: „In cases provided for in the preceding article (Article 444 of the Civil Code – cited above), the court may grant the injured party an appropriate amount of money as a pecuniary compensation for the suffered injury”.
The court may grant a compensation for a non-material injury or any other type of physical and mental suffering – such as caused by wrong treatment.
PROFESSIONAL LIABILITY OF PHYSICIANS
Pursuant to Articles 53 and 83 of the Act on Chambers of Physicians, physicians are subject to professional liability for breaching the principles of medical ethics and provisions related to practising the profession of a physician. Proceedings concerning the professional liability of physicians are held regardless of criminal or disciplinary proceedings pertaining to the same act. Article 53 provides that: „Chamber members are subject to the medical professional liability for violation of the rules of medical ethics and the provisions relating to the exercise of the medical profession, hereinafter referred to as professional offense”.
Article 83 provides that „a medical court may adjudicate the following penalties:
1. admonition;
2. reprimand;
3. financial penalty;
4. ban on holding managerial positions in healthcare organizational units for a period from one to five years;
5. limitation of the scope of activities in practising the profession of a physician for a period from six months to two years;
6. suspension of the right to practise the profession for a period from one to five years;
7. deprivation of the right to practise the profession.
Adjudicating the penalty provided for in section 5 or 6, a medical court may additionally adjudicate the penalty provided for in section 4”.
CONCLUSIONS
1. Gallbladder carcinoma is a highly aggressive malignancy.
2. The prognosis and 5 year survival rate in gallbladder carcinoma is poor.
3. The chosen treatment should be individualized for every patient.
4. Patients suffered from gallbladder carcinoma should be treated in high specialized cancer centers.
5. Patients must be treated with current medical knowledge.
Piśmiennictwo
1. Kondo S, Nimura Y, Hayakawa N et al.: regional and para-aortic lymphadenectomy in radical surgery for advanced gallbladder carcinoma. Br J Surg 2000; 87: 418-422. 2. Nevin JE: Carcinoma of the gallbladder. Cancer 1976; 37: 141-148. 3. Paimela H, Karppinen A, Hockerstedt K et al.: Poor prognosis of gallbladder cancer persists regardless of improved diagnostics methods. Ann Chir Gynecol 1997; 86: 13-17. 4. Wroński K: Prawa pacjenta. Nowotwory. J Oncol 2007; 3: 326-332. 5. Wroński K: Znajomość praw pacjenta przez osoby chore leczone w Klinice Chirurgii Onkologicznej Uniwersytetu Medycznego w Łodzi. Onkol Pol 2007; 2: 75-83. 6. Wroński K, Okraszewski J, Bocian R: Prawne konsekwencje ujawnienia tajemnicy lekarskiej. Nowotwory 2008; 58(2): 186-189. 7. Wroński K, Bocian R, Cywiński J, Dziki A: Prawne konsekwencje związane z ujawnieniem dokumentacji medycznej osobom nieuprawnionym. Kardiochir Torakochir Pol 2008; 5(4): 463-465. 8. Smith GCS, Parks RW, Madhavan KK et al.: A 10-year experience in the management of gallbladder cancer. HPB 2003; 5: 159-166. 9. Kaneoka Y, Yamaguchi A, Isogai M et al.: Hepatoduodenal ligemant invasion by gallbladder carcinoma: histologic patterns and surgical recommendation. World J Surg 2003; 27: 260-265. 10. Ito H, Matros E, brooks DC et al.: Treatment outcomes associated with surgery for gallbladder cancer: a 20-year experience. J Gastrointest Surg 2004; 8:183-190. 11. Potemski P, Polkowski W: Nowotwory układu pokarmowego. W: Zalecenia postępowania diagnostyczno-terapeutycznego nowotworach złośliwych 2013. VM Media Sp z o.o. VM Group sp. k. 12. Safjan D: Prawo pacjenta do informacji o rozpoznaniu i prognozowanych metodach leczenia. Antidotum 1993; 1: 26-8. 13. Nestorowicz M: Prawo medyczne. TNOiK, Toruń 2000. 14. Gubiński A: Komentarz do kodeksu Etyki Lekarskiej. Zakład Informacyjno-Wydawniczo-Kolportażowy Okręgowej Izby Lekarskiej, Warszawa 1995.
List of used legal acts:
1. Kodeks Etyki Lekarskiej z 14 grudnia 1991 roku ze zmianami.
2. Ustawa z dnia 23 kwietnia 1964 r. – Kodeks cywilny ze zmianami.
3. Ustawa z dnia 6 czerwca 1997 r. – Kodeks karny ze zmianami.
4. Ustawa z dnia 5 grudnia 1996 r. o zawodzie lekarza i lekarza dentysty ze zmianami.
5. Ustawa z dnia 2 grudnia 2009 r. o izbach lekarskich ze zmianami.
