*Artur Borowicz1, Klaudiusz Nadolny1, 2, Michal Kucap1, 3, Mariusz Gasior4, Bartosz Hudzik4, 5
The role and operation of emergency medical teams in patients with ST-segment elevation myocardial infarction
Rola i działanie zespołów ratownictwa medycznego u pacjentów z zawałem serca z uniesieniem odcinka ST
1Voivodeship Rescue Service in Katowice, Poland
2Department of Emergency Medicine and Disasters, Medical University of Bialystok, Voivodeship Rescue Service in Katowice, Poland
3College of Strategic Planning in Dabrowa Gornicza, Poland
43rd Department of Cardiology, School of Medicine with The Division of Dentistry in Zabrze, Medical University of Silesia, Katowice, Poland
5Department of Nutrition-Related Disease Prevention, School of Public Health in Bytom, Medical University of Silesia in Katowice, Poland
Streszczenie
Choroby sercowo-naczyniowe są główną przyczyną umieralności na świecie i stanowią 17,5 miliona zgonów rocznie lub 31% wszystkich zgonów na świecie rocznie. Wśród nich na pierwsze miejsce wysuwają się choroba wieńcowa oraz zawał mięśnia sercowego.
Częstość występowania zawału serca z uniesieniem odcinka ST (STEMI) w Europie waha się od 44 do 155/100 000 osób rocznie. W Polsce szacuje się, że STEMI występuje u około 80 000 osób rocznie. Niestety opóźnienia pacjenta w zakresie kontaktu ze służbą zdrowia są bardzo duże. Wynikają one z wielu czynników. Kampanie społeczne mogą przyczynić się do skrócenia tego czasu. Istotną rolę w leczeniu pacjentów ze STEMI oraz zmniejszeniu śmiertelności odgrywa system ratownictwa medycznego – począwszy od dyspozytora medycznego, który ma kontakt jako pierwsza osoba medyczna ze świadkiem zdarzenia albo z samym pacjentem, poprzez zespół ratownictwa medycznego. Już na etapie ambulansu zespół medyczny powinien rozpocząć leczenie. Podstawowym elementem jest system teletransmisji i telekonsultacji, który umożliwia szybkie i skuteczne leczenie reperfuzyjne pacjentów z ostrym zespołem wieńcowym.
Skrócenie czasu od bólu w klatce piersiowej do udrożnienia zamkniętego naczynia wieńcowego powoduje niższy wskaźnik śmiertelności z powodu zawału mięśnia sercowego z uniesieniem odcinka ST.
Summary
Cardiovascular diseases are the main cause of global mortality and constitute 30% of all deaths annually. The leading cardiovascular diseases are coronary disease and myocardial infarction.
The incidence of myocardial infarction with ST-segment elevation (STEMI) in Europe varies between 44 and 155/100,000 individuals per year. The annual number of STEMI cases in Poland amounts to about 80,000 individuals. Unfortunately, the values of patient-related delay in contacting medical services are significantly high and result from numerous factors. Social campaigns may lead to a minimization of this delay. The system of medical rescue plays an important role in the treatment of STEMI patients and in the decrease of mortality. Starting with a medical dispatcher, who is the first member of the medical personnel to have contact with the witness of the incident or the patient, and continuing with a medical rescue team. STEMI treatment should already be initiated in an ambulance. The basic procedure in prehospital STEMI patients is the system of teletransmission and teleconsultation, which ensure a prompt diagnosis and a direct transport to the center with the earliest reperfusion therapy available.
Minimizing the time from the occurrence of chest pain to coronary artery reperfusion leads to a decreased mortality caused by ST-segment elevation myocardial infarction.

Introduction
Cardiovascular diseases are the main cause of global mortality and constitute 17.5 mln deaths annually or 30% of all deaths worldwide per year (1). The leading cardiovascular diseases are coronary disease and myocardial infarction. Acute coronary syndromes are diagnosed in 1.5 mln patients worldwide (2), and in 140,000 patients in Poland (3). Over the past three decades in Europe, there has been a tendency towards a decreasing coronary disease-related mortality. However, over 4 mln European patients die due to cardiovascular diseases every year, which constitutes 45% of the total number of deaths in Europe (4). Coronary disease is the cause of about 20% of all deaths in Europe. The coronary disease-related mortality rate in Poland amounts to 191 deaths in 100,000 inhabitants. It is worth noticing that the rate has decreased by 39% throughout the past decade. Nevertheless, this rate remains higher than the European rate amounting to 132 deaths in 100,000 inhabitants (5). The incidence of ST-segment elevation myocardial infarction (STEMI) in Europe varies between 44 and 155/100,000 individuals annually. It has been estimated that in Poland, STEMI is diagnosed in 80,000 individuals per year (6, 7). STEMI-related mortality depends on numerous factors such as age, Killip class assigned to patients at admission, delayed treatment, the emergency medical system (EMS)-based STEMI networks, the selected therapy, diabetes, renal failure, and multi-vessel coronary artery disease. In spite of the implementation of new drugs in the antithrombotic therapy and the improvement of percutaneous coronary intervention (PCI) techniques, the in-hospital STEMI-related mortality varies between 4 and 12%, and amounts to 10% in the next 12 months after myocardial infarction (8, 9).
Review
STEMI-related procedures (including both diagnosis and treatment) is initiated at the moment of first medical contact, FMC (10). European experts suggest that local strategies of reperfusion therapy should be created to maximize the effectiveness of treatment (5). Delays in the treatment of STEMI are the most easily audited indicators of the quality of care. There are two types of delays related to the treatment of STEMI (fig. 1):
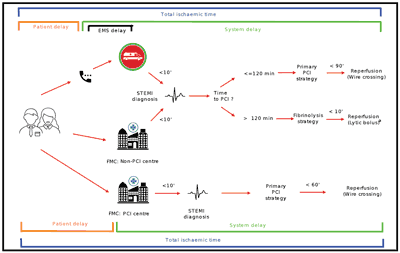
Fig. 1. Delays related to the treatment of STEMI
– patient-related delays,
– system delays.
In order to minimize patient-related delays, it is recommended to raise social awareness as far as the ability to identify myocardial infarction symptoms and reporting these symptoms to rescue services are concerned. Regarding the aspects of system delays, they all indicate the quality level of medical care (11).
The system of Emergency Medical Services (EMS) is crucial in dealing with STEMI patients, and is not only responsible for transport but also contributes to a prompt diagnosis of myocardial infarction, an appropriate patient triage, and implementation of preliminary treatment (12). Emergency medical units are divided into:
– specialized emergency medical teams with a minimum of three individuals qualified to perform emergency medical procedures, including a doctor and a nurse or a paramedic of the EMS system,
– basic emergency medical teams with at least two individuals qualified to perform emergency medical procedures, including a nurse or a paramedic of the EMS system – Article 36 (1) Law on State Emergency Medical Services (13).
Percutaneous coronary intervention (PCI) is the best way of STEMI treatment and leads to a decreased mortality and prevalence when contrasted with conservative therapy and thrombolytic treatment. The longer the time from the first medical contact (FMC) to the reperfusion of the artery responsible for myocardial infarction, the lower the implied outcome (14). There was a clear relationship between the delay in primary PCI and mortality in an annual observation. Every 30 minutes of delay in an invasive treatment was related to an increase of the relative annual ratio of mortality by 7.5%. The above-mentioned results have been considered in the recommendations of the European Society of Cardiology that focus on the time between the moment the patient reports to the doctor and the initiation of reperfusion therapy (15, 16).
Powyżej zamieściliśmy fragment artykułu, do którego możesz uzyskać pełny dostęp.
Mam kod dostępu
- Aby uzyskać płatny dostęp do pełnej treści powyższego artykułu albo wszystkich artykułów (w zależności od wybranej opcji), należy wprowadzić kod.
- Wprowadzając kod, akceptują Państwo treść Regulaminu oraz potwierdzają zapoznanie się z nim.
- Aby kupić kod proszę skorzystać z jednej z poniższych opcji.
Opcja #1
29 zł
Wybieram
- dostęp do tego artykułu
- dostęp na 7 dni
uzyskany kod musi być wprowadzony na stronie artykułu, do którego został wykupiony
Opcja #2
69 zł
Wybieram
- dostęp do tego i pozostałych ponad 7000 artykułów
- dostęp na 30 dni
- najpopularniejsza opcja
Opcja #3
129 zł
Wybieram
- dostęp do tego i pozostałych ponad 7000 artykułów
- dostęp na 90 dni
- oszczędzasz 78 zł
Piśmiennictwo
1. Cardiovascular diseases; http://www.who.int/mediacen-tre/factsheets/fs317/en/ (data dostępu: 16.10.2017).
2. Polonski L, Gasior M, Gierlotka M et al.: Polish Registry of Acute Coronary Syndromes (PL-ACS). Characteristics, treatments and outcomes of patients with acute coronary syndromes in Poland. Kardiol Pol 2007; 65(8): 861-872.
3. Steg PG, James SK, Atar D et al.: ESC Guidelines for the management of acute myocardial infarction in patients presenting with ST-segment elevation. Task Force on the management of ST-segment elevation acute myocardial infarction of the European Society of Cardiology (ESC). Eur Heart J 2012; 33(20): 2569-2619.
4. Townsend N, Nichols M, Scarborough P et al.: Cardiovascular disease in Europe – epidemiological update 2015. Eur Heart J 2015; 36(40): 2696-2705.
5. Kubica J, Adamski P, Paciorek P et al.: Anti-aggregation therapy in patients with acute coronary syndrome – recommendations for medical emergency teams. Experts standpoints. Kardiologia Pol 2017; 4: 399-408.
6. Obloj D, Zalewski J, Wroblewska I: Medical rescue team activities with patients diagnosed with acute coronary syndrome. Anest Ratow 2017; 11: 273-281.
7. Zurowska-Wolak M, Ilczak T: ECG teletransmission – perspective of emergency medical service. Anest Ratow 2016; 10: 358-362.
8. Kristensen SD, Laut KG, Fajadet J et al.: European Association for Percutaneous Cardiovascular Interventions. Reperfusion therapy for ST elevation acute myocardial infarction 2010/2011: current status in 37 ESC countries. Eur Heart J 2014; 35(29): 1957-1970.
9. Pedersen F, Butrymovich V, Kelbæk H et al.: Short- and long-term cause of death in patients treated with primary PCI for STEMI. J Am Coll Cardiol 2014; 64(20): 2101-2108.
10. Kubica J, Adamski P, Paciorek P et al.: Anti-aggregation therapy in patients with acute coronary syndrome – recommendations for medical emergency teams. Experts standpoint. Kardiologia Pol 2017; 75, 4: 399-408.
11. Terkelsen CJ, Sørensen JT, Maeng M et al.: System delay and mortality among patients with STEMI treated with primary percutaneous coronary intervention. JAMA 2010; 304(7): 763-771.
12. Kubica J, Adamski P, Paciorek P: Treatment of patients with acute coronary syndrome: recommendations for medical emergency teams: Focus on antiplatelet therapies. Updated experts standpoint. Cardiol J 2018. DOI: 10.5603/CJ.a2018.0042.
13. Ustawa o Państwowym Ratownictwie Medycznym z dnia 8 września 2006 roku. Dz. U. 2006 nr 191 poz. 1410.
14. Bagai A, Jollis JG, Dauerman HL et al.: Emergency department bypass for ST-segment-elevation myocardial infarction patients identified with a prehospital electrocardiogram: a report from the American Heart Association Mission: Lifeline program. Circulation 2013; 128(4): 352-359.
15. Wang TY, Nallamothu BK, Krumholz HM et al.: Association of door-in to door-out time with reperfusion delays and outcomes among patients transferred for primary percutaneous coronary intervention. JAMA 2011; 305(24): 2540-2547.
16. Ibanez B, James T, Agewall S et al.: Wytyczne ESC dotyczące postępowania w ostrym zawale serca z uniesieniem odcinka ST w 2017 roku. Kardiologia Pol 2018; 76(2): 229-313.
17. Bonnefoy E, Steg PG, Boutitie F et al.; CAPTIM Investigators: Comparison of primary angioplasty and pre-hospital fibrinolysis in acute myocardial infarction (CAPTIM) trial: a 5-year follow-up. Eur Heart J 2009; 30(13): 1598-1606.
18. Danchin N, Coste P, Ferrières J et al.; FAST-MI Investigators: Comparison of thrombolysis followed by broad use of percutaneous coronary intervention with primary percutaneous coronary intervention for ST-segment-elevation acute myocardial infarction: data from the French registry on acute ST-elevation myocardial infarction (FAST-MI). Circulation 2008; 118(3): 268-276.
19. Thiemann DR, Coresh J, Oetgen WJ et al.: The association between hospital volume and survival after acute myocardial infarction in elderly patients. N Engl J Med 1999; 340(21): 1640-1648.
20. Huber K, De Caterina R, Kristensen SD et al.: Task Force on Pre-hospital Reperfusion Therapy of the Working Group on Thrombosis of the ESC. Pre-hospital reperfusion therapy: a strategy to improve therapeutic outcome in patients with ST-elevation myocardial infarction. Eur Heart J 2005; 26(19): 2063-2074.
21. Rekosz J, Kasznicka M, Kwiatkowska D et al.: Electrocardiogram tele-transmission: Support in diagnosing cardiovascular diseases in operations undertaken by Warsaw-area basic medical rescue teams between 2009 and 2013. Cardiol J 2015; 22(6): 675-682.
22. Steg PG, James SK, Atar D et al.: ESC Guidelines for the management of acute myocardial infarction in patients presenting with ST-segment elevation. Task Force on the management of ST-segment elevation acute myocardial infarction of the European Society of Cardiology (ESC). Eur Heart J 2012; 33: 2569-2619.
23. Authors/Task Force members, Windecker S, Kolh P et al.: 2014 ESC/EACTS Guidelines on myocardial revascularization: The Task Force on Myocardial Revascularization of the European Society of Cardiology (ESC) and the European Association for Cardio-Thoracic Surgery (EACTS). Eur Heart J 2014; 35: 2541-2619.
24. Roffi M, Patrono C, Collet JP et al.: 2015 ESC Guidelines for the management of acute coronary syndromes in patients presenting without persistent ST-segment elevation: Task Force for the Management of Acute Coronary Syndromes in Patients Presenting without Persistent ST-Segment Elevation of the European Society of Cardiology (ESC). Eur Heart J 2016; 37: 267-315.
25. Wiviott SD, Braunwald E, McCabe CH et al.: Prasugrel vs. clopidogrel in patients with acute coronary syndromes. N Engl J Med 2007; 357: 2001-2015.
26. Wallentin L, Becker RC, Budaj A et al.: Ticagrelor vs. clopidogrel in patients with acute coronary syndromes. N Engl J Med 2009; 361: 1045-1057.
27. Montalescot G, van’t Hof AW, Lapostolle F et al.; ATLANTIC Investigators: Prehospital ticagrelor in ST-segment elevation myocardial infarction. N Engl J Med 2014; 371(11): 1016-1027.
28. Rozporządzenie Ministra Zdrowia z dnia 20 kwietnia 2016 r. w sprawie medycznych czynnos?ci ratunkowych i s?wiadczen? zdrowotnych innych niż medyczne czynnos?ci ratunkowe, które mogą byc? udzielane przez ratownika medycznego.
29. Kubica J, Kubica A, Jilma B et al.: Impact of morphine on antiplatelet effects of oral P2Y12 receptor inhibitors. Int J Cardiol 2016; 215: 201-208.
30. Kubica J, Adamski P, Ostrowska M et al.: Morphine delays and attenuates ticagrelor exposure and action in patients with myocardial infarction: the randomized, double-blind, placebo-controlled IMPRESSION trial. Eur Heart J 2016; 37: 245-252.
31. Puymirat E, Lamhaut L, Bonnet N et al.: Correlates of pre-hospital morphine use in ST-elevation myocardial infarction patients and its association with in-hospital outcomes and long-term mortality: the FAST-MI (French Registry of Acute ST-elevation and non-ST-elevation Myocardial Infarction) programme. Eur Heart J 2016; 37: 1063-1071.
32. Meine TJ, Roe MT, Chen AY et al.: Association of intravenous morphine use and outcomes in acute coronary syndromes: results from the CRUSADE Quality Improvement Initiative. Am Heart J 2005; 149: 1043-1049.

