*Agnieszka Dmowska-Koroblewska, MichaŇā Michalik, Adrianna Podbielska-Kubera, WŇāodzimierz Jakub Siemianowski
Drug-induced sleep endoscopy in assessing airway patency – own experiences
Badanie endoskopowe droŇľnoŇõci dr√≥g oddechowych w czasie snu farmakologicznego – wstńôpne wyniki
Department of Otolaryngology, MML Medical Center, Warsaw
Head of Department: MichaŇā Michalik, MD, PhD
Streszczenie
Wstńôp. Zesp√≥Ňā obturacyjnego bezdechu sennego naleŇľy do zaburzeŇĄ oddychania w czasie snu. Brak poprawy stanu zdrowia po wczeŇõniej wykonanych zabiegach laryngologicznych stanowi wskazanie do badania endoskopowego w czasie snu indukowanego (DISE– ang. drug-induced sleep endoscopy). DISE dostarcza istotnych informacji na temat czynnoŇõciowej droŇľnoŇõci g√≥rnych dr√≥g oddechowych.
MateriaŇā i metody. Badania przeprowadzono na grupie pacjent√≥w, u kt√≥rych wczeŇõniejsze leczenie chrapania i bezdechu sennego byŇāo nieskuteczne. U pacjent√≥w przeprowadzono endoskopińô w czasie snu indukowanego DISE. Do znieczulenia zastosowano propofol podawany w cińÖgŇāym wlewie doŇľylnym, co zapewniŇāo bezpieczeŇĄstwo wykonywanej procedury.
Wyniki. Od 2007 do 2017 roku w Centrum Medycznym MML przeprowadzono 3911 zabieg√≥w leczńÖcych chrapanie i bezdechy podczas snu. W tym czasie wykonano 176 procedur DISE. Sposoby leczenia przyczynowego okreŇõlano na podstawie ankiety, tomografii komputerowej z promieniem stoŇľkowym (CBCT – ang. cone beam computed tomography), badania laryngologicznego i DISE. SubiektywnńÖ poprawńô z ustńÖpieniem objaw√≥w uzyskano u 80% pacjent√≥w. W 70% przypadk√≥w chrapanie zmniejszyŇāo sińô. U pozostaŇāej czńôŇõci pacjent√≥w wymagane byŇāo poszukiwanie przyczyn og√≥lnoustrojowych: kardiologicznych, neurologicznych gastrologicznych lub endokrynologicznych.
Wnioski. W grupie pacjent√≥w Centrum Medycznego MML zastosowanie techniki DISE przyczyniŇāo sińô do precyzyjnego okreŇõlenia miejsca wibrowania i zapadania sińô dr√≥g oddechowych.
Badanie DISE daje powtarzalne pomiary droŇľnoŇõci dr√≥g oddechowych na poziomie gardŇāa dolnego. DISE umoŇľliwia efektywnńÖ diagnostykńô przyczyn zaburzeŇĄ snu w sytuacji, gdy inne metody, takie jak tomografia stoŇľkowa czy cefalometria, nie sńÖ wystarczajńÖce.
Summary
Introduction. Obstructive sleep apnea is a disorder of breathing during sleep. Lack of clinical improvement after previously performed laryngological procedures is an indication for endoscopic examination during drug – induced sleep. Drug-induced sleep endoscopy (DISE) provides important information about functional upper airways patency.
Material and methods. The study was performed in patients in whom other treatment methods had not been effective. DISE was performed in these patients. Continuous intravenous propofol infusion was given as general anesthetic to ensure the safety of the procedure.
Results. From 2007 to 2017, 2897 procedures for snoring and sleep apnea were performed at the MML Medical Center. At this time, 176 DISE examinations were performed.
Causative treatment methods were determined by the means of questionnaire, CBCT, laryngological examination, and DISE examination. Subjective improvement of apnea symptoms was achieved in 80% of patients. In 70% of cases, snoring decreased. The rest of the patients are required to look for systemic causes of cardiological, neurological gastrological, or endocrine origin.
Conclusions. In our patients, the use of the DISE examination enabled to precisely determine the location of the vibration and of the collapse of the respiratory tract. DISE enables to effectively diagnose the cause of sleep disorders when other methods, such as cone beam computed tomography (CBCT) or cephalometry are not sufficient.
Introduction
Obstructive sleep apnea syndrome (OSAS) affects between 2% and 4% of the population, mostly adults (1). About 80-90% of cases of OSAS remain undiagnosed (2). OSAS also occurs in children, in particular children older than 3-6 years of age (1).
Obstructive sleep apnea is characterized by high morbidity and mortality and is considered a public health problem. Clinical signs of OSAS include snoring and restless sleep (2). OSAS can also be associated with poor concentration, morning headache, excessive sleepiness during the day, and reduced intellectual ability (3). OSAS leads to hypoxia and significantly reduces patient’s quality of life (4). Factors such as obesity, allergy, and facial deformities may aggravate the problem (4). One of the most common risk factor for OSAS is obesity (5). The accumulation of excessive amounts of adipose tissue around the neck is of particular importance (6).
Obstructive sleep apnea may result in complications in different systems: vascular (myocardial infarction), neurological (stroke), endocrine (growth disturbance in children), and pulmonary (pulmonary hypertension) (7). Therefore, it is important to diagnose this condition and treat it adequately.
Obstructive sleep apnea is a result of anatomical abnormalities of upper respiratory airways, such as nasal turbinate hypertrophy, nasal polyps, deviated nasal septum, adenoid hypertrophy, tonsillar hypertrophy, dropping of soft palate, especially of the uvula, hypertrophy of the base of the tongue, and a pathology of larynx (8). Apnea is defined as a complete blockage of the airflow through the airways lasting at least 10 seconds (4). The goal of treating obstructive sleep apnea is to maintain the patency of the upper respiratory tract.
The severity of OSAS symptoms varies and is dependent on many factors that are not fully known (9). It has been confirmed that sleeping position has an impact on the incidence and severity of symptoms of sleep apnea. Symptoms in patients with OSAS (frequency of apnea, its duration, and desaturation) are increased when the patient is supine. Changes in the upper respiratory tract that are dependent on position during sleep correspond to a different severity of apnea. The mechanism responsible for an increase in symptoms when lying on the back is not clear. Most likely, it is related to the influence of gravity on the arrangement of individual sections of the upper respiratory tract. In the supine position, the tendency of the airways to collapse is greater. After changing the sleeping position from supine to lateral, the obstruction in the structures such as tongue base and larynx is less common. The assessment of changes of the anatomical elements of the upper respiratory tract depending on the sleep position can be used to plan targeted treatment in patients (9).
The diagnostic of OSAS include laryngological examination, endoscopic examination, polysomnography (PSG), cone beam computed tomography (CBCT), rhinomanometry, and drug-induced sleep endoscopy (DISE).
Polysomnography, first described in 1965 by Gastaut, is used for the diagnosis and assessment of severity of OSAS. Continuous Positive Airway Pressure (CPAP) is considered a golden standard of treatment of OSAS (10).
Lack of improvement after previous laryngological surgical procedures (such as septoplasty, palatoplasty, tonsillotomy, and tonsillectomy) is an indication for DISE (11). This applies to both adult and pediatric patients. DISE should be performed in children who continue to snore and wake up during the night after adenotonsillotomy (11).
In 1991, Croft and Pringle first applied drug-induced sleep endoscopy to examine respiratory tract in sedation (12).
Surgical treatment of obstructive sleep apnea requires knowing the exact location of the obstacle. Only the examination of the upper respiratory tract during in a sleeping patient can provide complete information about the state of health (13). To date, there is no optimal method for determining the location of airway obstruction (3). Unfortunately, most of the techniques used to investigate the location of the obstruction are based on the examination in an awake patient and include static rather than dynamic observation. DISE is a unique examination for assessing the cause of apnea and/or snoring, thanks to the patient’s light sleep caused by a pharmacological agent (10).
The examination is completely safe for the patient and is conducted in the presence of an anesthesiologist in an operating room or in a suitably equipped treatment room. Vital parameters are constantly monitored, and if necessary, the patient can be intubated and connected to a life support machine (14).
Different classification systems, such as VOTE classification system (velum, oropharynx lateral walls, tongue base, epiglottis) and NOHL classification system (nose, oropharynx, hypopharynx, larynx) are used to determine the location and severity of the upper respiratory tract obturation. VOTE classification enables quantitative assessment (3). For every level, the severity of obturation is assessed in a three-level scale: 0 – no obstruction (no vibration); 1 – partial obstruction (vibration); 2 – complete obstruction – collapse of airways. Oropharyngeal obturation is classified as: ap – anteroposterior, l – lateral (fig. 1), or c – circular. Not all the obturation patterns can occur on all the assessed levels (11).
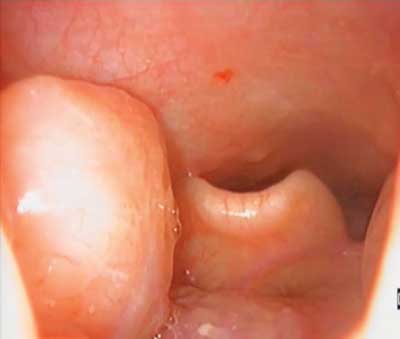
Fig. 1. Lower end of tonsil compressing epiglottis
In the NOHL classification system, obturation grade is assessed on a scale from 0 to 4. Oropharyngeal obturation is classified as: ap – anteroposterior, l – lateral, or c – circular. Laryngeal obstruction is also assessed: on an a (epiglottis) or b (glottis) level, as p – positive, or n – negative (fig. 2, 3) (15).
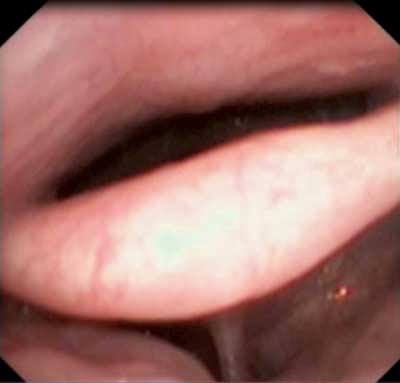
Fig. 2. Collapse of epiglottis
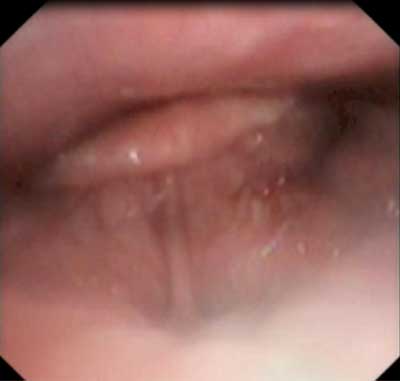
Fig. 3. Airway obstruction at the level of epiglottis
The majority of researchers use the VOTE system (3).
Material and Methods
The study was retrospective. DISE was performed on patients with obstructive sleep apnea. Before the procedure, patients were asked to complete the questionnaire, consisting of an original questionnaire for diagnosing breathing disorders during sleep (fig. 4), based on Berlin Questionnaire – enabling to assess the relationship between respiratory disturbances during sleep and cardiovascular and respiratory diseases – and Epworth Sleepiness Scale by the British Snoring and Sleep Apnoea Association (fig. 5) – enabling the assessment of daytime sleepiness and probability of falling asleep in everyday situations.



Fig. 4. Original questionnaire for diagnosing breathing disorders during sleep

Fig. 5. Epworth Sleepiness Scale
In some of the patients, as a part of extended diagnostic process, apnea/hypopnea index (AHI) was also determined. AHI describes the severity of sleep apnea and is expressed as a number of apnea and hypopnea episodes per hour of sleep (tab. 1).
Tab. 1. AHI score and severity level of OSAS
| AHI | Severity of OSAS |
| < 5 | normal |
| 5-14 | mild OSAS |
| 15-24 | moderate OSAS |
| > 24 | severe OSAS |
For each patient, body mass index (BMI) was also calculated and neck circumference was measured.
In laryngological examination, the following structures were assessed: external nose (symmetry and potential deformations), anterior nares, nasal septum, and inferior nasal conchae. Additionally, soft palate was assessed according to Mallampati classification (tab. 2), and tonsils were evaluated with Pirquet Tonsillar Hypertrophy Grading Scale (tab. 3).
Tab. 2. Mallampati score
| Grade | Description |
| 1. | soft palate, uvula, fauces, pillars visible |
| 2. | soft palate, uvula, fauces visible |
| 3. | soft palate, base of uvula visible |
| 4. | soft palate not visible |
Tab. 3. Pirquet score
| Grade | Description |
| 1. | Tonsils hidden behind tonsillar pillars |
| 2. | Tonsils extend to pillars |
| 3. | Tonsils visible beyond pillars |
| 4. | Tonsils covering 50% of space between pillars |
| 5. | Tonsils extend to midline |
Patients underwent endoscopic examination and CBCT (fig. 6). The indications for surgical treatment included deviated nasal septum, turbinate hypertrophy, and dropping of the soft palate.

Fig. 6. Airway obstruction at the level of velum and tongue root
The patients qualified for surgery underwent different procedures, including palatoplasty, coblation inferior turbinate reduction, septoplasty, tonsillotomy, or tonsillectomy. Different surgical techniques were applied, including Shaver method, Celon-coblation turbinate reduction, and contact diode laser.
Patients had control visits one and four weeks after the procedure. Treatment outcomes were evaluated 3 months after surgery. Patients re-filled in the questionnaires, laryngological examination was also performed. Moreover, CBCT and rhinomanometry were performed in every patient. If nasal patency was maintained and soft palate was lifted, but the symptoms persisted, it was attempted to find a cause of obstruction in lower pharynx and larynx.
Lack of improvement after previous laryngological procedures had been considered to be an indication for DISE.
During DISE, the following equipment was used: video processor Olympus CV-170; video rhinolaryngoscope Olympus ENF-V3, diameter: 2.6 mm, length: 30 cm; video rhinolaryngoscope Olympus ENF-VH, diameter: 3.9 mm, length: 30 cm.
On the examination day, patients were admitted on a day-case basis.
A standard procedure for preparation for surgical procedure with general anesthesia was implemented.
The patients were asked to refrain from eating and drinking before the procedure. No additional blood tests before the anesthesia were required, but medical interview concerning chronic diseases was collected.
During the examination, patients were lying supine on the operating table. Standard life parameters monitoring included ECG, heart rate, blood pressure, and oxygen saturation monitoring. Nasal cannulas were introduced into the nasal cavity. During the examination, the cannulas were subsequently transferred and introduced into the oral cavity in order to avoid the interference with the introduction of the soft endoscope. During the examination, oxygen was administered in the amount of 2-3 l/min. Ineach patient, intravenous access to a vein of the forearm was obtained. After premedication with 3 mg midanium intravenously, anesthesia was induced with 1-1.5 mg/kg body weight propofol. Subsequently, anesthesia was maintained with propofol infusion at the rate of 3-6 mg/kg body weight/hour for the entire time of the procedure. The administration of propofol ensured that the sedation was safe and stable (9).
The patients of the MML Medical Center usually did not require the supply of narcotic analgesics. After the end of the examination, intravenous propofol was discontinued. After about 5 to 10 minutes, the patients awoke from the induced sleep and were transported to the recovery room. After 2 to 3 hours, they were released from the hospital.
VOTE classification system was used for the assessment of the obturation (7).
Treatment methods used in the MML Medical Center depend on the location of the underlying cause. Techniques described earlier are used.
The results presented in this article include the analysis of patients’ responses to the first 10 questions of the original questionnaire. Comprehensive results, currently undergoing analysis, will include remaining answers to the original questionnaire, Epworth Sleepiness Scale, rhinomanometry, and computed tomography.
Results
Between 2007 and 2017, 2,897 surgical procedures for snoring and sleep apnea were performed at the MML Medical Center. The study included 1053 women and 2844 men. Mean age was 46 years for men and 35 years for women. Mean disease duration was 4 years. One hundred seventy-six DISE procedures were performed. Methods of causative treatment were determined based on the questionnaire, CBCT, laryngological and endoscopic examination. Subjective improvement of apnea symptoms was achieved in 80% of patients. In 70% of cases, snoring decreased. The rest of the patients are required to look for systemic causes of cardiological, neurological gastrological, or endocrine origin.
Discussion
OSAS is a widespread, but largely undiagnosed illness (1). Obstructive sleep apnea has been underestimated as a risk factor for cardiovascular diseases for many years (6). Therefore, thorough examination is needed in order to assess the risk of sleep apnea, as well as to develop strategies to prevent and treat OSAS (12).
OSAS diagnosis is based on medical history and polysomnographic examination, which assesses the type and severity of sleep disturbances.
Patients that belong to OSAS risk groups are asked to complete the Berlin Questionnaire and Epworth Daily Sleepiness Scale questionnaire. In patients with confirmed sleep apnea, laryngological consultation is also advised to assess the obstruction of upper respiratory airways. In case of anatomical abnormalities, surgical treatment should be considered.
Patients of the MML Medical Center who had not experienced improvement after previous laryngological procedures were qualified for DISE.
In more than 80% of the patients in the study, a decrease in the severity of symptoms – lower daytime sleepiness and less problems in falling asleep, as well as a lower degree of snoring – was observed, which is consistent with the literature (17). In a non-randomized, prospective trail, in which patients underwent DISE, the authors were able to determine the percentage of airway obstruction in patients based on digital photos made during the examination (18). The highest degree of stenosis was observed at the velum (84.1 ± 18.7%), as well as at the tongue base (39.3 ± 37.5%), and at the epiglottis (44.6 ± 42.8%).
Literature data shows that DISE is a safe, effective, repeatable and easy to use technique for locating obstruction sites in the upper respiratory tract. Preliminary studies have shown that the therapeutic success of OSAS in patients in whom DISE was used is more common (75%) than in other patients (40%) (3). Hessel et al. (13) confirm the efficacy of DISE in OSAS patients in 69% of cases.
Drug-induced sleep endoscopy proved to be an important technique for identifying multilevel collapse, especially at the base of the tongue and on the epiglottis level. DISE examinations also have also demonstrated the important role of laryngopharyngeal obstruction in OSAS (2).
CPAP is still the most important method of treatment of OSAS. Despite the proven efficacy of CPAP, a significant amount of patient may not be able to tolerate this method and seeks for alternative treatment methods, such as surgery and/or functional oral mechanisms (19). CPAP turns out to be ineffective in patients in which there is epiglottis collapse, as it may result in moving the epiglottis towards the larynx (19).
Chisholm et al. (13) report that patients in which CPAP was ineffective, DISE can be used. It is then possible to perform an effective laser surgery of the soft palate and reduce the AHI index below 20 in 90% of cases (13).
Invasive treatment method – epiglottis resection – is the preferred solution in cases when the epiglottis collapses and block the respiratory tract during sleep. In OSAS patients, the removal of epiglottis in combination with other procedures may lead to a significant improvement in the patient’s health (19).
DISE is not performed during physiological sleep. During natural sleep, a reduction of the tone of the genioglossus muscle occurs during NREM sleep phase (non-rapid eye movement) and REM phase (rapid eye movement). This phenomenon is intensified in patients with OSAS when compared with healthy persons. After the induction of pharmacological sleep, the reduction of the tone of the genioglossus muscle may contribute to the collapse of the tongue base. In order to confirm the efficacy of DISE, it is necessary to conduct randomized studies on large groups of patients (20). At the same time, the results of the reviews show a lot of discrepancies between the location of obstacles in patients remaining awake and examined with DISE (13).
DISE is considered to be an integral part of the diagnostic process in patients with suspected OSAS in many countries, including the Netherlands. The opponents of this method argue that pharmacological sleep is not equivalent to physiological sleep. An ideal solution would be to perform DISE during physiological sleep, however, this procedure is very demanding and therefore, very rarely used (10).
Attention was also drawn to the need for establishing a single sedation method (10). The influence of the sedation method (propofol and midazolam in a bolus, and then titrated during the procedure) on the results of the examination of the airway obstruction may vary. Rabelo et al. report that using propofol shortens REM sleep phase, which slightly changes the architecture of sleep, and does not have significant influence on the respiratory system and AHI index (10). The same conclusions were drawn from a study including diazepam (10). A study conducted by Sadaok et al. indicated that pharmacological sleep after diazepam administration does not differ from physiological sleep in aspects other than REM duration (10). Up to date, there is no standard protocol for sedation during DISE, as dosage and duration of the anesthesia depend on many factors, including individual differences, and susceptibility to the sedative effect of the drug. Further studies are needed in order to avoid false positive results (10).
In literature, there are reports of use of DISE-TCI (Target Controlled Infusion) in order to replicate the conditions that the airways are subjected to during snoring and sleep apnea in DISE (21). In target controlled infusion, after programing the target anesthetic level in serum or in effector organ (brain), the infusion pump determines the rate of infusion of the drug, based on an algorithm taking into account, among others, sex, age, body weight and height of the patient. This way of anesthetic administration ensures fast induction of analgesia, as well as its adequate depth (22). However, according to the literature, better sedation control is achieved with the use of bispectral index to monitor consciousness level (23). Bispectral index minimizes the risk of restoring patient’s consciousness during the procedure. Moreover, it enables proper dosage of propofol during surgery (24).
A randomized, prospective, single-center study comparing the efficacy of DISE and DISE-TCI was performed (13). The study included 40 patients randomly assigned to either DISE or DISE-TCI group. There was a statistically significant difference in the percentage of patients that had been considered treated from sleep apnea (4 patients – 20% – in DISE group vs. 17 patients – 85% – in DISE-TCI group; p < 0.0001). Two patients in DISE group required oxygen administration after the first dose of propofol. Unstable vital signs were observed in 13 patients in DISE group (65%) and in 1 patient in DISE-TCI group (5%) (p = 0.0001). The results suggest that DISE-TCI should be the first choice for drug-induced sleep endoscopy due to its increased accuracy, stability, and safety (21). At the same time, Witkowska et al. (18) reported that there were no clinically significant differences in hemodynamic parameters, sleep depth, time of recovery form anesthesia, and consumption of anesthetics between groups with target controlled infusion and manual infusion of the drugs.
Data obtained during the DISE examination should be interpreted with due care. In some cases, finding additional location of obstruction may lead to unnecessary procedures. High doses of drugs and a long examination time are disadvantages of the DISE method. Moreover, the treatment of all obstruction locations found in DISE is not a guarantee of success (13). DISE examination may help to explain the pathophysiology of sleep apnea associated with different sleeping positions (25).
Abdullah et al. observed that patients with higher BMI are characterized by a higher number of obstruction sites when compared with other patients, in whom typically only single obstruction sites are identified (10).
Literature data show that the surgical success is significantly less common in patients with increased BMI. In these patients, mainly circular obstruction occurs. Iwanaga et al. confirmed the more common occurrence of obstruction at the level of the palate and at the tongue base in patients with BMI > 30 and higher AHI scores. At higher AHI values, the collapse of airways at many levels is also observed (10).
The literature presents how DISE examination, in comparison with a classic laryngological examination, influences the qualification for individual procedures or a mandibular protruding device. After DISE examination, a change of treatment method was recommended. Surgery of soft palate was recommended in 93,8% of cases after DISE (and in 77,3% of cases without DISE). Modification of treatment was also recommended in 23 out of 38 patients in a study by Gillespie et al (14). The planning of treatment with the use of DISE allowed to achieve improvement in 72% of patients in a large group including 2,485 patients analyzed by Kotecha et al. (14).
Epiglottis collapse in patients with OSAS occurs more frequently than reported in the previous studies. Before introducing DISE, 12% of patients with OSAS were diagnosed with epiglottis collapse based on the laryngological examination on an awake patient. Epiglottis collapse may be observed during DISE, even if previous laryngological examination had not revealed the problem (19).
In the group of patients of MML Medical Center, the main goal of the examination was to precisely identify the location of vibration and airway obturation. DISE has fully enabled us to achieve this goal. It should be emphasized that DISE as a diagnostic procedure has its drawbacks, which include, above all, high costs and risk of complications (e.g. allergic reaction, airway obstruction) (26). In addition, this method is dependent on the experience of the operators, the route of administration of anesthesia, and the dose of an anesthetic. The multiplicity and complexity of classification systems in diagnosis of OSAS is a major drawback that makes it difficult to compare results between centers (27).
The key to the therapeutic success is an individual approach to every patient, and paying attention to the sleep position and individual characteristics of the patient (10).
Literature reports confirm that experience in DISE examination is necessary for reliable results (28).
These issues remain the subject of research.
Conclusions
In the group of patients of MML Medical Center, the use of DISE has enabled to precisely determine the location of vibration and airway obturation.
DISE permits to obtain repeatable measurements of airway patency of the hypopharynx.
DISE enables effective diagnosis of sleep disturbances in cases in which different diagnostic methods, such as CBCT or cephalometry, are not sufficient.
Despite the lack of standardization of clinical trials, drugs used for sedation and applied classification system, results of the studies suggest including DISE technique for the diagnosis of the obstruction sites in patients with OSAS. The use of a universal DISE assessment system could facilitate the comparison of test results between centers.
During DISE, the way in which airways are obstructed, as well as the site of the obstruction, can be visualized. It is also possible to assess several obstruction sites, which is advantageous when compared with classical endoscopy. Classical endoscopy, unlike DISE, may irritate the upper respiratory tract and disrupt the patient’s sleep.
Adequate assessment of all the obstruction sites using both DISE and VOTE system aims to improve the effectiveness of treatment of patients with OSAS. Only surgical ablation of all the obstacles identified during DISE can answer the question whether the identified obstacles were the reason for the sleep apnea syndrome.
DISE examination is safe and easy to perform, and it enables to create an individual treatment plan. Endoscopy during pharmacological sleep is a valuable supplement to the diagnostic process of breathing disorders during sleep. Modern anesthetic drugs decrease the risk of the examination. Available classification systems are subjective and need to be objectified.
PiŇõmiennictwo
1. Young T, Finn L: Epidemiological insights into the public health burden of sleep disordered breathing: sex differences in survival among sleep clinical patients. Thorax 1998; 53 suppl. 3: 516-519.
2. Viana Ada C Jr, Thuler LC, Ara√ļjo-Melo MH: Drug-induced sleep endoscopy in the identification of obstruction sites in patients with obstructive sleep apnea: a systematic review. Braz J Otorhinolaryngol. 2015; 81: 439-446.
3. Altintaş A, Olgun B, Yegin Y et al.: Interobserver Consistency of Drug-Induced Sleep Endoscopy in Diagnosing Obstructive Sleep Apnea Using a VOTE Classification System. J Craniofac Surg. 2017; 1: 1-10.
4. Hasiec A, Szumowski ŇĀ, Walcza F: Obturacyjny bezdech – senny zab√≥jca. For Med Rodz 2012; 6 (3), 103-114.
5. Schwartz AR, Patil SP, Laffan AM et al.: Obesity and obstructive sleep apnea: pathogenic mechanisms and therapeutic approaches. Proc Am Thor Soc 2008; 5(2); 185-192.
6. Ciuba I: Obturacyjny bezdech senny. Zam St Mat; 2011; 13(1): 109-115.
7. Jagannathan R, Seixas A, St-Jules D et al.: Systems Biology Genetic Approach Identifies Serotonin Pathway as a Possible Target for Obstructive Sleep Apnea: Results from a Literature Search Review. Sleep Disord 2017; 2017: 6768323.
8. Atulkumar Shah J, George A, Chauhan N, Francis S: Obstructive Sleep Apnea.Role of an Otorhinolaryngologist; Indian J Otolaryngol Head Neck Surg 2016; 68(1): 71-74.
9. Lee CH, Kim DK, Kim SY et al.: Changes in Site of Obstruction in Obstructive Sleep Apnea Patients According to Sleep Position: A DISE Study. Laryngoscope 2015; 125: 248-254.
10. Ravesloot MJ, de Vries N: One hundred consecutive patients undergoing drug-induced sleep endoscopy: results and evaluation. Laryngoscope 2011; 121(12): 2710-2716.
11. Kezirian EJ, Hohenhorst W, de Vries N: Drug-induced sleep endoscopy: the VOTE classification. Eur Arch Otorhinolaryngol 2011; 268(8): 1233-1236.
12. Croft CB, Pringle M: Sleep nasendoscopy: a technique of assessment in snoring and obstructive sleep apnoea. Clin Otolaryngol Allied Sci 1991; 16: 504-509.
13. Blumen MB, Latournerie V, Bequignon E et al.: Are the obstruction sites visualized on drug-induced sleep endoscopy reliable? Sleep Breath 2015; 19: 1021-1026.
14. Grochowski T, Kukwa W, Krzeski A et al.: Badanie endoskopowe gardŇāa dolnego we Ňõnie farmakologicznym. Mag Otolar 2014; 50(13): 57-61.
15. Vicini C, De Vito A, Benazzo M et al.: The nose oropharynx hypopharynx and larynx (NOHL) classification: A new system of diagnostic standardized examination for OSAHS patients. Eur Arch Otorhinolaryngol 2012; 269(4): 1297-1300.
16. Roblin G, Williams AR, Whittet H: Target-controlled infusion in sleep endoscopy. Laryngoscope 2001; 111: 175-176.
17. Kotecha BT, Hannan SA, Khalil HM et al.: Sleep nasendoscopy: A 10-year retrospective audit study. Eur Arch Otorhinolaryngol 2007; 264(11): 1361-1367.
18. Ryan C, Borek BS, Erica R at al.: Quantitative Airway Analysis During Drug-Induced Sleep Endoscopy for Evaluation of Sleep Apnea. Laryngoscope 2012; 122(11): 2592-2599.
19. Torre C, Camacho M, Liu SY et al.: Epiglottis collapse in adult obstructive sleep apnea: a systematic review. Laryngoscope 2016; 126(2): 515-523.
20. Yegïn Y, √áelik M, Kaya KH et al.: Comparison of drug-induced sleep endoscopy and M√ľller’s maneuver in diagnosing obstructive sleep apnea using the VOTE classification system. Braz J Otorhinolaryngol. 2017; 83(4): 445-450.
21. De Vito A, Agnoletti V, Berrettini S et al.: Drug-induced sleep endoscopy: conventional versus target controlled infusion techniques – a randomized controlled study. Eur Arch Otorhinolaryngol 2011; 268: 457-462.
22. Witkowska M, Karwacki Z, Rzaska M et al.: Por√≥wnanie docelowej infuzji kontrolowanej i anestezji caŇākowicie doŇľylnej z uŇľyciem propofolu i remifentanylu do operacji mikrodyskoidektomii w odcinku lńôdŇļwiowym krńôgosŇāupa; Anest Int Ter 2012, 44:(3), 156-163.
23. Lo YL, Ni YL, Wang TY et al.: Bispectral Index in Evaluating Effects of Sedation Depth on Drug-Induced Sleep Endoscopy. JCSM 2015; 11(9): 1011-1020.
24. Myles PS, Leslie K, McNeil J et al.: Bispectral index monitoring to prevent awareness during anaesthesia: the B-Aware randomised controlled trial. Lancet 2004; 363(9423): 1757-1763.
25. Safiruddin F, Koutsourelakis I, de Vries N: Analysis of the influence of head rotation during drug-induced sleep endoscopy in obstructive sleep apnea. Laryngoscope 2014; 124: 2195-2199.
26. Carrasco-Llatas M, Agostini-Porras G, Cuesta-Gonz√°lez MT, Rodrigo-Sanbartolomè A et al.: Drug-induced sleep endoscopy: a two drug comparison and simultaneous polysomnography. Eur Arch Otorhinolaryngol 2014; 271(1): 181-187.
27. Dijemeni E, Kotecha B: Drug-Induced Sedation Endoscopy (DISE) DATA FUSION system: clinical feasibility study. Eur Arch Otorhinolaryngol 2017; 1: 1-14.
28. Vroegop AV, Vanderveken OM, Wouters K et al.: Observer variation in drug-induced sleep endoscopy: experienced versus nonexperienced ear, nose, and throat surgeons. Sleep 2013; 36(6): 947-953.







