Jacek Smereka1, Marek Dabrowski2, Mateusz Puslecki3, Mateusz Szarek4, Damian Gorczyca4, Zuzanna Popielarska4, Dominika Dunder4, Jerzy Robert Ladny5, Karol Bielski4, Szymon Bialka6, Kurt Ruetzler7, *Lukasz Szarpak4
Should we use a guide during endotracheal intubation in normal and difficult airways? A randomized, cross-over, simulation study. Pilot data
Czy powinniśmy stosować prowadnicę podczas intubacji dotchawiczej w warunkach normalnych i trudnych drogach oddechowych? Randomizowane krzyżowe badanie symulacyjne – badania pilotażowe
1Department of Emergency Medical Service, Wroclaw Medical University, Poland
2Chair and Department of Medical Education, Poznan University of Medical Sciences, Poland
3Department of Rescue Medicine, Poznan University of Medical Sciences, Poland
4Lazarski University, Warsaw, Poland
5Department of Emergency Medicine, Medical University of Bialystok, Poland
6Department of Anaesthesiology and Intensive Care, Medical University of Silesia, Katowice, Poland
7Departments of Outcomes Research and General Anesthesiology, Anesthesiology Institute, Cleveland Clinic, Cleveland, Ohio, USA
Streszczenie
Wstęp. Zabezpieczenie drożności dróg oddechowych w warunkach medycyny ratunkowej stanowi jedną z podstawowych czynności wykonywanych względem osoby w stanie bezpośredniego zagrożenia życia. Pomimo wprowadzenia do użytku nadgłośniowych urządzeń do wentylacji, intubacja dotchawicza stanowi nadal złoty standard zabezpieczenia dróg oddechowych.
Cel pracy. Celem pracy jest ocena efektywności intubacji dotchawiczej z prowadnicą intubacyjną i bez prowadnicy intubacyjnej wykonywanej przez studentów ostatniego roku studiów medycznych.
Materiał i metody. W badaniu zaprojektowanym jako badanie randomizowane, krzyżowe udział wzięło 47 studentów ostatniego roku studiów medycznych. Uczestnicy wykonywali intubację dotchawiczą osoby dorosłej za pomocą standardowego laryngoskopu z łopatką Macintosha w dwóch technikach: z prowadnicą intubacyjną i bez prowadnicy intubacyjnej. Intubacja odbywała się w dwóch scenariuszach badawczych: scenariusz A – normalne drogi oddechowe, scenariusz B – trudne drogi oddechowe. Analizie poddano skuteczność intubacji, czas trwania procedury, stopień uwidocznienia głośni czy też łatwość wykonania procedury.
Protokół badania został zaakceptowany przez Radę Programową Polskiego Towarzystwa Medycyny Katastrof (protokół: 30.02.2018.IRB).
Wyniki. Mediana czasu intubacji z prowadnicą intubacyjną i bez prowadnicy dla poszczególnych scenariuszy badawczych była zróżnicowana. Dla scenariusza A czas do pierwszej próby wentylacji był krótszy przy zastosowaniu prowadnicy – 24,9 s (IQR: 21-32,5), w porównaniu z intubacją bez prowadnicy – 29,5 s (IQR: 24-35) (p = 0,013). W scenariuszu B czas intubacji ze sztyletem i bez sztyletu wynosił odpowiednio 43,5 s (IQR: 29,5-52) vs. 52 s (IQR: 43-57,5) (p = 0,001). Podczas scenariusza A skuteczność pierwszej próby intubacji z wykorzystaniem sztyletu w porównaniu z intubacją bez sztyletu wynosiła 44,7 vs. 27,6%, zaś całkowita skuteczność wynosiła w obu przypadkach 100%. W przypadku scenariusza B skuteczność pierwszej próby intubacji ze sztyletem i bez sztyletu wynosiła 27,6 vs. 17%, zaś całkowita skuteczność intubacji 78,7 vs. 42,6%.
Wnioski. Intubacja dotchawicza z wykorzystaniem prowadnicy intubacyjnej wiązała się wyższą skutecznością pierwszej próby intubacji, krótszym czasem trwania procedury, jak również niższym stopniem trudności wykonania procedury.
Summary
Introduction. Protecting airway patency in emergency medicine situations is one of the basic activities performed in relation to a person in a state of immediate life threat. Despite the introduction of supraglottic ventilation devices for use, endotracheal intubation is still the gold standard for respiratory protection.
Aim. The aim of the study is to evaluate the effectiveness of endotracheal intubation performed with and without an intubation guide carried out by students in their final year of medical studies.
Material and methods. In a study designed as a randomized trial, 47 students in their final year of medical studies took part. Participants in the study performed endotracheal intubation on an adult using a standard laryngoscope with a Macintosh blade in two techniques: with and without an intubation guide. Intubation was carried out in two scenarios: Scenario A – normal airways; Scenario B – difficult airways. We analyzed the effectiveness of intubation, the duration of the procedure, the degree of visualization of the glottis or the ease of performing the procedure.
The study protocol was approved by the Program Board of the Polish Society for Disaster Medicine (Approval No. 34.02.2018.IRB).
Results. The median time to intubation with and without stylet was compared for each of the aforementioned scenarios. For scenario A, time to first ventilation was achieved fastest for tube with stylet, 24.9 s (IQR: 21-32.5), when compared to that of tube without stylet at 29.5 s (IQR: 24-35) (p = 0.013). In scenario B, the time for intubation with and without stylet varied and amounted to 43.5 s (IQR: 29.5-52) vs. 52 s (IQR: 43-57.5) (p = 0.001). During Scenario A, the effectiveness of the first intubation trial using stylet compared to intubation without stylet was 44.7 vs. 27.6%, while the total efficiency was 100% in both cases. In the case of scenario B, the effectiveness of the first attempt to intubate with and without stylet was 27.6 vs. 17%, and total intubation efficiency 78.7 vs. 42.6%.
Conclusions. Endotracheal intubation using an intubation guide was associated with a higher efficacy of the first intubation trial, a shorter duration of the procedure, as well as a lower degree of difficulty in the procedure.

INTRODUCTION
The protection of upper airway patency plays a fundamental role in resuscitation procedures regardless of the cause of sudden cardiac arrest. It is one of the basic skills that should be demonstrated by medical personnel working in the healthcare system (1, 2).
Endotracheal intubation is still one of the medical activities that pose quite a challenge even for the most experienced people in this skill, which classifies it in the forefront of procedures performed in emergency medicine with the highest risk of iatrogenic diseases (3). At the same time, it is also one of the most effective methods of instrumental airway protection because it provides the possibility of asynchronous ventilation in relation to compression, prevents regurgitation, and provides the possibility of positive end-expiratory pressure (PEEP) ventilation in respiratory therapy (4, 5). The decision to intubate a patient consists of many factors, i.e. the patient’s respiratory capacity, hypoventilation and hypercapnia as well as the number of points in GCS (Glasgow Coma Scale). Due to the diversity of individual conditions and numerous indirect factors (lighting, patient position, body structure, etc.) affecting the correct positioning of the endotracheal tube in direct laryngoscopy, instruments supporting this medical procedure were developed (6-10).
AIM
The aim of the study is to evaluate the effectiveness of endotracheal intubation performed with and without an intubation guide performed by final year medical students under normal and difficult airways conditions.
MATERIAL AND METHODS
The research is a continuation of research carried out by authors whose aim is to search for the most effective method of intubation (9, 11-14). The study was designed as a randomized, cross-over study and was performed based on medical simulation. The study protocol was approved by the Program Board of the Polish Society for Disaster Medicine (Approval No. 34.02.2018.IRB). The study involved 47 final year medical students participating in Advanced Cardiovascular Life Support training (ACLS) conducted by accredited American Heart Association instructors. Written voluntary informed consent was taken from each participant.
Scenario simulation
Prior to the study, all participants successfully completed ACLS training. Next, the instructor demonstrated the correctness of intubation using the Macintosh laryngoscope. Subsequently, the participants had a 10-minute training session during which they performed endotracheal intubation using a Macintosh laryngoscope and a standard endotracheal tube without a guide using AT Kelly Torso (Laerdal, Stavanger, Norway).
During the target study, a SimMan 3G adult simulator (Laerdal, Stavanger, Norway) was used to simulate a patient in need of endotracheal intubation, which was placed on the floor in a brightly lit room. The study participants performed endotracheal intubation with and without intubation stylet (fig. 1). Endotracheal intubation was performed based on two research scenarios:
• Scenario A – normal airway,
• Scenario B – difficult airway. Difficult airways were obtained by inflation of the tongue using software that controlled the simulator, so as to obtain the visibility of the glottis at level 3 by Cormack-Lehane scale (15).
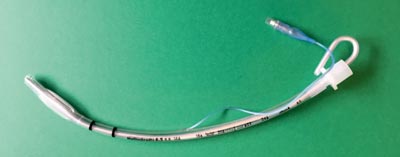
Fig. 1. Endotracheal tube with semirigid stylet
Both the order of the participants and the research methods were random. For this purpose, the ResearchRadomizer program was used. A detailed procedure for randomization of the study is presented on figure 2.
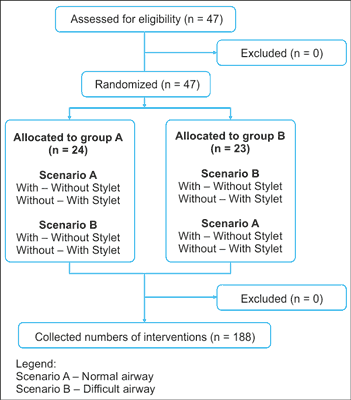
Fig. 2. Randomization flow chart
Measurements
The basic parameter measured in the study was the assessment of the effectiveness of the first intubation attempt, assessed by the correctness of chest elevation in the case of ventilation with the use of endotracheal tube and self-expanding bag, additional confirmation was obtained thanks to the readings of the parameters indicated by the software controlling the simulator. In addition, the total intubation efficacy assessed against a maximum of three intubation tests performed by study participants was measured. The next parameter measured in the study was intubation time, defined as the time from hand-in-hand by performing laryngoscope intubation until an effective ventilation test using a self-expanding bag. In addition, both the percentage of glottic opening and the ease of intubation was assessed. The percentage of glottic opening (POGO) score was defined as the glottic visual highlighting rate based on direct laryngoscopy. Ease of technical use was defined as a scale from 1 to 100, where “1” – meant an easy procedure, and “100” – as a very difficult procedure to perform.
Statistical analysis
Powyżej zamieściliśmy fragment artykułu, do którego możesz uzyskać pełny dostęp.
Mam kod dostępu
- Aby uzyskać płatny dostęp do pełnej treści powyższego artykułu albo wszystkich artykułów (w zależności od wybranej opcji), należy wprowadzić kod.
- Wprowadzając kod, akceptują Państwo treść Regulaminu oraz potwierdzają zapoznanie się z nim.
- Aby kupić kod proszę skorzystać z jednej z poniższych opcji.
Opcja #1
29 zł
Wybieram
- dostęp do tego artykułu
- dostęp na 7 dni
uzyskany kod musi być wprowadzony na stronie artykułu, do którego został wykupiony
Opcja #2
69 zł
Wybieram
- dostęp do tego i pozostałych ponad 7000 artykułów
- dostęp na 30 dni
- najpopularniejsza opcja
Opcja #3
129 zł
Wybieram
- dostęp do tego i pozostałych ponad 7000 artykułów
- dostęp na 90 dni
- oszczędzasz 78 zł
Piśmiennictwo
1. Szarpak L: Laryngoscopes for difficult airway scenarios: a comparison of the available devices. Expert Rev Med Devices 2018; 15(9): 631-643.
2. Vivek B, Sripriya R, Mishra G et al.: Comparison of success of tracheal intubation using Macintosh laryngoscope-assisted Bonfils fiberscope and Truview video laryngoscope in simulated difficult airway. J Anaesthesiol Clin Pharmacol 2017; 33(1): 107-111.
3. Kurowski A, Szarpak L, Zasko P et al.: Comparison of direct intubation and Supraglottic Airway Laryngopharyngeal Tube (S.A.L.T.) for endotracheal intubation during cardiopulmonary resuscitation. Randomized manikin study. Anaesthesiol Intensive Ther 2015; 47(3): 195-199.
4. Szarpak L, Kurowski A, Truszewski Z et al.: Comparison of 3 video laryngoscopes against the Miller laryngoscope for tracheal intubation during infant resuscitation. Am J Emerg Med 2015; 33(3): 460-461.
5. Szarpak L: Videolaryngoscopy or direct laryngoscopy for child tracheal intubation during cardiopulmonary resuscitation. Am J Emerg Med 2016; 34(12): 2453.
6. Kurowski A, Szarpak L, Truszewski Z et al.: Can the ETView VivaSight SL Rival Conventional Intubation Using the Macintosh Laryngoscope During Adult Resuscitation by Novice Physicians? A Randomized Crossover Manikin Study. Medicine (Baltimore) 2015; 94(21): e850.
7. Yildirim A, Kiraz HA, Ağaoğlu ? et al.: Comparison of Macintosh, McCoy and C-MAC D-Blade video laryngoscope intubation by prehospital emergency health workers: a simulation study. Intern Emerg Med 2017; 12(1): 91-97.
8. Moustafa MA, Arida EA, Zanaty OM et al.: Endotracheal intubation: ultrasound-guided versus fiberscope in patients with cervical spine immobilization. J Anesth 2017; 31(6): 846-851.
9. Gawlowski P, Smereka J, Madziala M et al.: Comparison of the ETView Single Lumen and Macintosh laryngoscopes for endotracheal intubation in an airway manikin with immobilized cervical spine by novice paramedics: A randomized crossover manikin trial. Medicine (Baltimore) 2017; 96(16): e5873.
10. Kim DH, Yoo JY, Ha SY et al.: Comparison of the paediatric blade of the Pentax-AWS and Ovassapian airway in fibreoptic tracheal intubation in patients with limited mouth opening and cervical spine immobilization by a semi-rigid neck collar: a randomized controlled trial. Br J Anaesth 2017; 119(5): 993-999.
11. Kaminska H, Wieczorek W, Dabrowski M et al.: Comparison of four laryngoscopes in cervical immobilization scenario. Pilot data. Am J Emerg Med 2018; 36(5): 890-891.
12. Szarpak L, Karczewska K, Czyzewski L et al.: Airtraq Laryngoscope Versus the Conventional Macintosh Laryngoscope During Pediatric Intubation Performed by Nurses: A Randomized Crossover Manikin Study With Three Airway Scenarios. Pediatr Emerg Care 2017; 33(11): 735-739.
13. Szarpak L, Truszewski Z, Vitale J et al.: Exchange of supraglottic airways for endotracheal tube using the Eschmann Introducer during simulated child resuscitation: A randomized study comparing 4 devices. Medicine (Baltimore) 2017; 96(26): e7177.
14. Ladny JR, Sierzantowicz R, Kedziora J et al.: Comparison of direct and optical laryngoscopy during simulated cardiopulmonary resuscitation. Am J Emerg Med 2017; 35(3): 518-519.
15. Glosser L: Assessment of endotracheal tube intubation. Review of existing scales. Disaster Emerg Med J 2017; 2(2): 91-93.
16. Tosh P, Rajan S, Kumar L: Ease of Intubation with C-MAC Videolaryngoscope: Use of 60° Angled Styletted Endotracheal Tube versus Intubation over Bougie. Anesth Essays Res 2018; 12(1): 194-198.
17. Driver BE, Prekker ME, Klein LR et al.: Effect of Use of a Bougie vs Endotracheal Tube and Stylet on First-Attempt Intubation Success Among Patients With Difficult Airways Undergoing Emergency Intubation: A Randomized Clinical Trial. JAMA 2018; 319(21): 2179-2189.
18. Lee YC, Lee J, Son JD et al.: Stylet angulation of 70 degrees reduces the time to intubation with the GlideScope®: A prospective randomised trial. J Int Med Res 2018; 46(4): 1428-1438.
19. Komasawa N, Nishihara I, Minami T: Effects of stylet use during tracheal intubation on postoperative pharyngeal pain in anesthetized patients: A prospective randomized controlled trial. J Clin Anesth 2017; 38: 68-70.
20. Biro P, Bättig U, Henderson J et al.: First clinical experience of tracheal intubation with the SensaScope, a novel steerable semirigid video stylet. Br J Anaesth 2006; 97(2): 255-261.
21. Buis ML, Maissan IM, Hoeks SE et al.: Defining the learning curve for endotracheal intubation using direct laryngoscopy: A systematic review. Resuscitation 2016; 99: 63-71.
22. Aghamohammadi H, Massoudi N, Fathi M et al.: Intubation learning curve: comparison between video and direct laryngoscopy by inexperienced students. J Med Life 2015; 8(spec. iss. 4): 150-153.
23. Sakles JC, Mosier J, Patanwala AE et al.: Learning curves for direct laryngoscopy and GlideScope® video laryngoscopy in an emergency medicine residency. West J Emerg Med 2014; 15(7): 930-937.
24. Szarpak L, Madziala A, Czekajlo M et al.: Comparison of the UEScope videolaryngoscope with the Macintosh laryngoscope during simulated cardiopulmonary resuscitation: A randomized, cross-over, multi-center manikin study. Medicine (Baltimore) 2018; 97(36): e12085.
25. Szarpak L, Smereka J, Ladny JR: Comparison of Macintosh and Intubrite laryngoscopes for intubation performed by novice physicians in a difficult airway scenario. Am J Emerg Med 2017; 35(5): 796-797.
26. Hippard HK, Kalyani G, Olutoye OA et al.: A comparison of the Truview PCD and the GlideScope Cobalt AVL video-laryngoscopes to the Miller blade for successfully intubating manikins simulating normal and difficult pediatric airways. Paediatr Anaesth 2016; 26(6): 613-620.
27. Rendeki S, Keresztes D, Woth G et al.: Comparison of VividTrac®, Airtraq®, King Vision®, Macintosh Laryngoscope and a Custom-Made Videolaryngoscope for difficult and normal airways in mannequins by novices. BMC Anesthesiol 2017; 17(1): 68.
28. Szarpak L, Czyzewski L, Truszewski Z et al.: Comparison of Coopdech®, CoPilot®, Intubrite®, and Macintosh laryngoscopes for tracheal intubation during pediatric cardiopulmonary resuscitation: a randomized, controlled crossover simulation trial. Eur J Pediatr 2015; 174(11): 1517-1523.
29. Madziala M, Smereka J, Dabrowski M et al.: A comparison of McGrath MAC® and standard direct laryngoscopy in simulated immobilized cervical spine pediatric intubation: a manikin study. Eur J Pediatr 2017; 176(6): 779-786.
30. Karczewska K, Szarpak L, Smereka J et al.: ET-View compared to direct laryngoscopy in patients with immobilized cervical spine by unexperienced physicians: A randomized crossover manikin trial. Anaesthesiol Intensive Ther 2017; 49(4): 274-282.


